Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is a comparison between Version 2 by Vivi Li and Version 1 by Natalia A. Shnayder.
Regular physical activity in cyclic sports can influence the so-called “angiogenic switch”, which is considered as an imbalance between proangiogenic and anti-angiogenic molecules. Disruption of the synthesis of angiogenic molecules can be caused by local changes in tissues under the influence of excessive physical exertion and its consequences, such as chronic oxidative stress and associated hypoxia, metabolic acidosis, sports injuries, etc.
- angiogenic switch
- angiogenesis
- vascular endothelial growth factor (VEGF)
- fibroblast growth factor (FGF)
- angiopoietin
- platelet growth factor (EDGF)
- epidermal growth factor (EGF)
- receptor
- skeletal muscle
- myocardium
- lung tissue
- nervous tissue
- pathology
- physi
1. Introduction
In the modern world, sports are considered as one of the components of a healthy lifestyle, including prevention of cerebral ischemia, coronary heart disease, diabetes mellitus, atherosclerosis, and many other diseases. However, angiogenesis, as a dynamic and complex process regulated by various growth factors, can change under the influence of active physical activity. Changes can occur both in the positive direction and in the direction of the development of the pathological process. Against this background, it is promising and important to study the so-called “angiogenic switch” as an imbalance between proangiogenic and anti-angiogenic molecules (inhibitors and activators of angiogenesis) [1]. The “angiogenic switch”, through which new capillaries grow in the vasculature, includes the prevascular phase and the vascular phase. In the prevascular phase, germinating cells proliferate (sometimes as quickly as in the vascular phase), but the rate of these cells’ death (apoptosis) balances proliferation and maintains the germinating mass in a stable state. In the vascular phase, exponential cell growth begins [2]. The change in the activity of the synthesis of angiogenic molecules depends on an increase in the production of one or several angiogenesis activators such as endothelial vascular growth factor (VEGF), fibroblast growth factor (FGF), platelet growth factor (PDGF), epidermal growth factor (EGF), and others. They can be mobilized from the extracellular matrix or released from host cells (for example, macrophages). The expression of endogenous angiogenesis inhibitors such as thrombospondin-1 (TSP-1) or interferon beta can be suppressed. Thus, the “angiogenic switch” includes something more than a simple activation of angiogenic activity and is considered to be the result of a balance of positive and negative regulators [2]. Integrin signaling also contributes to this regulatory balance. Resting vessels express one class of integrins, while germinating capillaries express another. Interference with signaling from the latter class of integrins can inhibit angiogenesis. Proteases control the bioavailability of angiogenic activators and inhibitors. Some release FGF-2 stored in the extracellular matrix, while plasmin, a proangiogenic component of the blood coagulation system, is degraded to form an angiogenesis inhibitor, angiostatin [3]. Activation of the angiogenic process can be caused by local changes in tissues under the influence of excessive physical exertion and their consequences, such as hypoxia, metabolic acidosis, trauma, inflammation, and impaired homeostasis of metal ions. The study of angiogenesis and the “angiogenic switch” in athletes and the translation of the results of these studies into the training process is important for maintaining the physical health of athletes as well as increasing the functional resources of the nervous, musculoskeletal, cardiovascular, and respiratory systems of athletes and their sports performance.
2. Current Resesearches and Results
2.1. Vascular Endothelial Growth Factor (VEGF)
2.1.1. Role of VEGF in Angiogenesis in Athletes
An important aspect of adaptation to training loads in cyclic sports is an increase in the number of capillaries in muscle fibers, which improves the metabolism of skeletal muscles and myocardium, as well as in the brain and lung tissue. Primarily, the “angiogenic switch” is important in aerobic sports (i.e., long distance running). The high capillarization of the working muscles increases the peripheral circulation and thus influences the maximum oxygen consumption. This is the key to the high athletic performance of long distance runners (endurance training). Vasculogenesis (the first stage is the primitive formation of vessels inside the embryo and in the surrounding membranes, as well as the circulation of the yolk sac) and angiogenesis (second stage is responsible for the remodeling and expansion of this network) the formation of new blood vessels) play an important homeostatic role, as blood vessels carry nutrients to tissues and organs and remove catabolic products. However, uncontrolled growth of blood vessels can contribute to the development of many pathological processes, including vascular disorders [4]. From this point of view, an important aspect of adaptation to sports loads is the establishment of a balance in the synthesis of proangiogenic and anti-angiogenic molecules (activators and inhibitors of angiogenesis), or the “angiogenic switch”. Identification of genetic markers associated with the regulation of blood vessel growth is an important aspect in sports practice. One of the key factors affecting vascular growth is the VEGF-A protein. It is a heparin-binding protein that exists as a disulfide-linked homodimer. This growth factor causes proliferation and migration of vascular endothelial cells and is involved in the regulation of both physiological and pathological angiogenesis. VEGF-A expression is significantly increased in endurance athletes (for example, in long distance runners) [5].
VEGF and the “Angiogenic Switch” in Skeletal Muscle
Muscle injuries are one of the most common pathologies in orthopedic practice. Most muscle injuries (10% to 55% of all injuries) occur during sports activities. Muscle injuries are a serious problem due to slow recovery, during which athletes are unable to participate in training and competition, as well as due to the frequent consequences and recurrence of injuries [6]. Muscle regeneration is a complex biological process. Once damaged, satellite cells proliferate, thus providing enough cells for repair. The proliferation phase ends with the appearance of the first small regenerating muscle tubes approximately 3 days after injury [7]. At the same time, some of the proliferated cells become immobile again, while the rest begin to merge with the formation of multinucleated muscular tubes (terminal differentiation). Subsequently, there is a biochemical differentiation of muscle tubes into muscle fibers. This process is accompanied by an increase in macrophages and the destruction of damaged fibers. The results obtained when studying the effect of VEGF-A on the formation of myotubes show that this process is associated with the stimulation of differentiation by increasing the maturation of multinucleated myofibrils [8]. To identify the receptor that mediates these effects of VEGF-A on myogenic cells, it must be kept in mind that both VEGFR-1 and VEGFR-2 are activated in differentiating myogenic cells, in myotubes, and in satellite cells after muscle injury. In cultured myoblasts and cells, inhibition of the VEGFR-2 protein kinase reverses the protective effect of VEGF-A on cell apoptosis, suggesting the involvement of VEGFR-2 in mediating VEGF-A signal. The effect of VEGF-A on muscle recovery after injury is likely to be mediated by various mechanisms. The factor has a well-known proangiogenic activity; research results show [9,10][9][10] that it prevents apoptosis and promotes muscle fiber growth. According to the authors, the restoration of muscle tissue is realized through the interaction of all the listed effects of VEGF-A. An additional possibility is that mobilizing bone marrow progenitor cells, VEGF-A promotes muscle regeneration through transdifferentiation or fusion of these cells, although there is evidence to refute this mechanism. For a long time, VEGF-A was considered an endothelial-specific growth factor that promotes a strong angiogenic response. However, current studies demonstrate the ability of VEGF-A to induce myofibril regeneration in skeletal muscle. In addition to angiogenesis, the interaction of VEGF-A with its receptors is important for the survival and stimulation of cell differentiation in a wide range of different tissues, including skeletal muscle [8].
VEGF and “Angiogenic Switch” in the Myocardium
Studies by many authors have shown that physical activity has a positive effect on the coronary vasculature, including myocardial oxygen demand, endothelial function, autonomic tone, markers of inflammation, and the development of collateral coronary vessels [11,12][11][12]. However, the direct effect of exercise on myocardial angiogenesis remains poorly understood. Physical activity is accompanied by functional, electrical, and structural remodeling of the heart. Myocardial hypertrophy is accompanied by an increase in the left atrium diameter, the left ventricle wall thickness, and myocardial mass. Vascular changes in the myocardium are reported to be associated with neoangiogenesis and capillary density in the heart muscle [13]. Angiogenesis in the myocardium is a complex process mediated by the interaction of proangiogenic and anti-angiogenic factors. Cardiomyocytes express VEGFR-1 and VEGFR-2, which are rapidly activated in response to hypoxia [14]. It is believed that the role of VEGF-A in myocardial remodeling is related to the balance of its actions on VEGFR-1, which inhibits the development of hypertrophy, and VEGFR-2, which has prohypertrophic effects. A transgenic murine model of VEGFR-1 deletion of endothelial cells led to angiogenesis and the development of cardiomyocyte hypertrophy through signaling of erb-B tyrosine kinase [15]. These processes can be further influenced by microRNAs (miRNAs) such as miR-374, which is known to positively regulate cardiomyocyte hypertrophy in murine models. Vascular endothelial growth factor-B (VEGF-B) and angiopoietin 1 (ANGPT-1) are the main angiogenic factors that enhance endothelial cell proliferation and accelerate vascular growth in the infarction zone [13]. Among the various types of mechanisms that regulate gene expression, epigenetic changes associated with the acetylation–deacetylation of histones by various isoforms of histone deacetylase (HDAC) are also important [16]. Recent research indicates that changes in oxidant/antioxidant balance can affect angiogenic activity in tissues [17]. These oxidative changes are the result of reactive oxygen species (ROS). ROS can change the structure of proteins, lipids, carbohydrates, and nucleic acids. According to the authors, damage to the mitochondrial membrane is realized through ROS radicals derived from xanthine oxidase of inflammatory cells [ibid.]. Alternatively, during oxidation, the high rate of destruction of red blood cells from intense endurance exercise can increase the amount of free iron, which will help protect highly reactive hydroxyl radicals through iron-catalyzed Haber–Weiss reactions. Ardakanizade et al. [13] studied short-term and long-term adaptive changes occurring in the myocardium as a result of physical exertion on endurance to elucidate the molecular picture of tissue remodeling. In addition, the authors tried to reveal the effect of an exercise regimen on oxidative changes and angiogenesis in the heart muscle. Experimental studies conducted in animals showed high myocardial plasticity as a result of endurance exercises, which was expressed by changes in the signaling cascade at the level of transcription and translation. These changes increased the contractile ability of the myocardium, and consequently, the cardiovascular system potential [18]. A significant increase in myocardial contractility was accompanied by a significant increase in its mass and left ventricle wall thickness. The study reported the presence of the heart muscles impairment, which was accompanied by oxidative changes. The results showed that oxidative stress was dependent on the duration of endurance exercise. The decrease in antioxidant capacity was more pronounced with prolonged exercise, indicating an increase in oxidative changes caused by the duration of the exercise program. Oxidative changes have been expressed as an increase in oxidative markers (nitric oxide (NO)) and the end product of lipid peroxidation (MDA). With prolonged endurance exercise, vasodilation occurs due to the need for blood supply to the heart muscle. Therefore, NO is involved in blood supply, helping coronary arteries through endothelial nitric oxide synthase (eNOS) [19]. This blood supply is always accompanied by an increase in NO and the expression of the gene for vascular endothelial growth factor beta (VEGF-B) in the molecular structure.
VEGF-B becomes active due to the interaction between a hypoxia-inducible factor-1 (HIF-1) and a hypoxia reactive element (HRE) in response to hypoxia induced by prolonged endurance exercise [20,21][20][21]. VEGF-B stimulates endothelial cell proliferation as well as migration and new vessel formation through transmission signal carried out by tyrosine kinase receptors [22]. Thus, the need for blood supply to the coronary muscles is satisfied by the process of angiogenesis and expression of VEGF-B. As the expression of VEGF-B increased in the experimental group (performing endurance exercises for a long time), the same group demonstrated a higher level of angiogenesis. Thus, the higher production of ROS, which occurs concurrently with the higher expression of VEGF-B, confirms the relationship between angiogenesis and oxidative stress. Exercise induces muscle tissue calcineurin signaling pathways to enable muscle tissue contraction. It has been shown in the literature that the regulation of calcineurin-dependent genes is mediated by the MEF2 transcription factors [23]. Moreover, it was indicated that the expression of the MEF-2c gene can be increased in endothelial cells via VEGF-B, which, in turn, regulates the process of vasculogenesis [24]. Therefore, a significantly higher expression of the VEGF-B gene and the VEGF-B gene induced by endurance exercise is associated with an increase in cardiac muscle contractility and vascularization. Angiopoietin 1 (ANGPT-1) is a protein that supports the survival of endothelial cells during angiogenesis. VEGF-B-induced vascular permeability can be blocked and regulated by overexpression of ANGPT-1 [24]. Thus, the density of new vessels can be adjusted. Accordingly, a higher expression of ANGPT-1 in the experimental group (where endurance exercises were performed for a short period of time) contributed to the angiogenesis regulation. However, this was not observed in another study group with a longer period of endurance exercises [13]. This suggests that with prolonged aerobic loads, regulation of angiogenesis is impaired and new blood vessels are formed. These data are consistent with the results of other studies, which reported that concomitant expression of VEGF-B and angiopoietin-2 can increase and regulate the density and permeability of microvessels [25].
After birth, mammalian cardiomyocytes become differentiated and generally lose their ability to proliferate. However, a certain level of their renewal occurs throughout life [26]. Note that in adulthood, the growth of the heart occurs more due to hypertrophy of cardiomyocytes than due to hyperplasia. Myocardial hypertrophy can be either physiological or pathological. Physiological hypertrophy is the result of a response to exercise or other stimuli. Normally, a hypertrophied heart exhibits improved vascular perfusion and metabolism, and the growth process is initiated by molecular pathways specific for physiological hypertrophy [27]. Cardiac perfusion is largely controlled by the microvessel through a dense capillary network with approximately one capillary per muscle fiber. Consequently, being critical for neoangiogenesis, VEGF plays a central role in cardiomyocyte hypertrophy.
VEGF and “Angiogenic Switch” in Cerebrovascular and Cardiovascular Systems
The role of VEGF-A in maintaining the “angiogenic switch” balance in the cardiovascular and cerebrovascular systems is beyond doubt. The positive effects of VEGF-A are associated with the protection of endothelial cells by increasing the expression level of antiapoptotic proteins and NO synthesis [28]. VEGF causes severe endothelium-dependent vasodilation, primarily through nitric oxide (NO) and prostacyclin (PGI2). In cultured human endothelial cells, binding of VEGF-A to VEGFR-2 activates the PI3K/Akt pathway, followed by activation of endothelial NO synthase (eNOS) and NO release. However, VEGF-induced vasodilation is not reversed by inhibition of NO and PGI2, suggesting that an endothelial-derived hyperpolarizing factor (EDHF) is also involved in VEGF-mediated vasodilation [29]. The negative effects of VEGF-A have been reported in several studies. The ability of VEGF-A to induce atherogenesis and its effect on endothelial cells as a mitogen through re-endothelialization were reviewed by Braile et al. [30]. The mitogenic effect of VEGF-A on endothelial cells is mediated through VEGFR-2 and the activation of kinase is regulated by extracellular signals (ERK1/2). Phosphorylation of VEGFR-2 leads to the activation of phospholipase C (PLC-γ), which in turn stimulates the Raf-MAPK/ERK (MEK)-ERK1/2 kinase cascade in cultured endothelial cells [29]. VEGF-A plays a role in cell migration, including vascular smooth muscle cells, monocytes, and polymorphonuclear cells. In endothelial cells, cell migration is induced by activation of focal adhesion kinase (FAK) and paxillin, as well as via the phosphatidylinositol kinase (PI3K)/Akt and MAPK pathways [29]. The ability of VEGF-A to induce adhesion of monocytes through transendothelial migration and activation [31], improving endothelial permeability and increasing expression of the adhesion protein and chemoattractant protein-1 of monocytes has also been described [32]. VEGF-A was previously known as a vascular permeability factor. Its interaction with VEGFR-2 on cultured endothelial cells triggers the activation of several pathways that regulate the adhesive properties of the transmembrane protein, vascular endothelial cadherin (VE-cadherin). These pathways include the protooncogene tyrosine kinase src and culminate in phosphorylation and internalization of VE-cadherin, separating it from the cytoskeleton. This subsequent loss of adhesive bond results in a marked increase in vascular permeability.
Ylä-Herttuala et al. found no VEGF-A or its receptors in intact segments of human coronary vessels. However, their expression increases in endothelial microcapillaries, in macrophages, and in partially differentiated smooth muscle cells of atherosclerotic lesions [33]. In their research on animal model of rabbits exposed to 8 weeks of chronic stress, Yu et al. revealed instability of atherosclerotic plaques and activation of angiogenesis caused by the release of VEGF-A which was found in large amounts in blood serum [34].
VEGF and “Angiogenic Switch” in Lung Tissue
Sports loads in cyclic sports are associated with an increase in oxygen consumption. That is why the pulmonary system becomes the main system subject to functional changes during exercise. Numerous studies of the sports physiology have demonstrated a clear relationship between heart rate, oxygen consumption, respiratory rate and minute ventilation, energy metabolism, and lactate production [35]. Although the lungs are one of the limiting systems of the body in cyclic sports, their response to high-intensity loads and other environmental stresses is often overlooked. Vigorous exercise can contribute to capillary leakage, especially when left atrial pressure rises due to left ventricular (LV) systolic or diastolic insufficiency. LV diastolic dysfunction, which causes an increased pressure in the left atrium during exercise, often results in pulmonary edema and capillary hemorrhage. Studies suggest that the lungs can respond to exercise and immersion stress with pulmonary edema and pulmonary hemorrhage [36].
There are many controversial questions about the role of VEGF-A in the physiology and pathology of the lungs. Lung tissue contains the highest level of transcripts among the wide range of organs expressing VEGF-A. The lung is one of the main organs in which VEGF-A controls several important physiological functions [37]. Lung morphogenesis requires constant physical and molecular interactions between the mesenchymal stroma and epithelial elements. Airway epithelial cells are the predominant source of VEGF-A throughout lung organogenesis and appear to be critical for normal alveolarization, rapid alveolar proliferation during lung maturation, and normal vascular development. It is believed that VEGF-B, VEGF-C, VEGF-D, and PlGF also play a role in the physiological development of the lungs [38], but they are not extensively studied in this context or not so extensively as VEGF-A. There exists much research on these other growth factors. During exercise and airway activation, the lungs gradually receive a rich blood supply through the growth of endothelial cells and vascular cells in the pulmonary mesenchyme. This growth is accompanied by the expression of VEGF-A and its receptors, which play central morphogenetic functions in the lung tissue [39]. Pulmonary VEGF-A is synthesized by alveolar epithelial cells, bronchial epithelial cells, smooth muscle cells, and alveolar macrophages. This topographic compartmentalization allows VEGF-A to interact with components of the extracellular matrix, thereby creating concentration gradients that regulate the physiological functions of VEGF-A in the lungs [39]. Overexpression of pulmonary VEGF-A results in markedly dysmorphic lung structure. In contrast, neutralization of VEGF-A throughout fetal development by the extracellular domain Fc-VEGFR1 promotes a clearly simplified lung in neonatal mice [40,41][40][41]. Inhibition of VEGF-A leads to regression of tracheal capillaries and death of endothelial cells in the lungs of adult mice, while most vessels become resistant to VEGF-A cleavage after embryonic development [41]. It has recently been shown that this VEGF-A is an isoform of both VEGF-A xxx a and VEGF-A xxx b [42]. Similarly, VEGF-A receptors and coreceptors are also expressed by several types of cells in the normal lung on either side of the alveolar capillary membrane (ACM), including ATII cells. The classical processes associated with VEGF-A activity (permeability, angiogenesis, and mitogenesis) are extremely limited in the mature lung. Thus, although the exact role of VEGF-A in the lungs is not fully defined, it has been suggested that compartmentalization of VEGF-A in the alveolar space of intact lung tissue is essential to maintain normal lung structure and function.
In addition to its well-known functions as a trophic factor and growth factor, VEGF-A may play a new biological role in maintaining lung homeostasis. Cellular homeostasis of the lung tissue requires the rapid removal of apoptotic cells in order for their total number to remain constant. Effective removal of damaged cells reduces the risk of necrosis and inflammation, and by binding of apoptotic cells to the phosphatidylserine receptor, many immunosuppressive cytokines (TGF-β, PGE2, PGI2, and IL10) are released to suppress inflammation and reduce the risk of autoimmune diseases [43]. VEGF can promote efferocytosis, which, in turn, leads to further VEGF-A production and cell repair during lung tissue damage [44].
Chin-Kuo Lin et al. studied the expression patterns of inflammatory cytokines and growth factors after pulmonary hyperventilation (VILI) and determined the phenotypes of monocytes recruited to the lungs during recovery to elucidate how monocytes recruited to the lungs and pulmonary VEGF-A promote epithelial proliferation [45]. The increased expression of VEGF-A and TGF-β found by the authors in injured lungs underlines the role that VEGF-A and TGF-β play in lung recovery after VILI. Proteins belonging to the families of epidermal growth factor and fibroblast growth factor are involved in the restoration of damaged lung epithelium [46]. In addition to its well-known angiogenetic properties, VEGF-A acts as a powerful epithelial lung mitogen involved in repairing lung damage [47,48,49][47][48][49]. Studies have shown that the effects of VEGF-A vary depending on the damaged cells in the lung tissue and the recovery time [38,50,51][38][50][51]. VEGF-A receptor signaling is required for the maintenance of alveolar structures in normal rat lungs, as well as for the regulation of proliferation and apoptosis of damaged alveolar epithelial cells in an autocrine or paracrine manner [52]. Acute respiratory distress syndrome (ARDS) is the most severe form of lung disease. Medford et al. found that VEGF-A expression was significantly increased in late ARDS cases after day 7 compared with controls (without lung tissue damage) and early ARDS cases within 48 h [53]. Chin-Kuo Lin et al. [45] analyzed VEGF-A expression and the number of Ki67-positive cells in the alveolar epithelium of lung slices and found a strong positive correlation between VEGF-A expression and alveolar epithelial cell proliferation during VILI recovery. Their results demonstrated that VEGF-A can help repair alveoli in damaged lungs during healing [45]. Taken together, these findings suggest a dual role for VEGF-A in lung tissue repair: Increased serum VEGF-A concentration promotes progressive lung damage early in the disease, while increased VEGF-A expression in lung tissue promotes lung recovery during the late recovery phase. Thus, the revealed information about positive and negative effects of VEGF-A indicates that while considering the therapeutic effect of VEGF-A on lung tissue under intense physical activity the biology of VEGF-A in the lungs should be taken into account.
2.1.2. Association of the VEGF Gene SNVs with Changes in the “Angiogenic Switch” Stroke and Functional Resources in Athletes
The VEGF gene encoding the homonymic protein plays a key role in the regulation of vasculogenesis and angiogenesis. It was identified, isolated, and cloned more than 25 years ago [54]. It is localized on chromosome 6p21.1 (Figure 1).
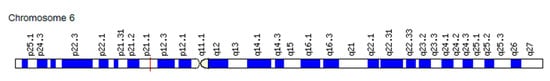

Figure 1. Localization of the VEGF gene on chromosome 6p21.1.
There are several related genes, including VEGF-B and VEGF-C, but the greatest attention is paid to VEGF-A because of its key role in the regulation of angiogenesis, in both physiological and pathological homeostasis. All isoforms of the VEGF protein have specific receptors. They have different affinities for the different receptors and can bind to them. VEGF-B overrides the activity of VEGF-A by activating VEGFR-1. VEGF-C and VEGF-D can be angiogenic factors. In this case, they are activated via the VEGFR-2 and VEGFR-3 receptors. Furthermore, these factors can be lymphangiogenic (mainly VEGF-D) and are activated through the VEGFR-3 receptor. The absolute and relative levels of expression of VEGFR-2 and VEGFR-3 in the endothelium can influence the nature of the effect of growth factors VEGF-C/D—angiogenic or lymphangiogenic effects. VEGF expression is stimulated by a variety of proangiogenic factors, including hypoxia-induced factor (HIF), epidermal (EGF), and fibroblast (FGF) growth factors. In addition, the blood pH, the partial pressure, and the O2 concentration in the inhaled air affect the VEGF level. Although VEGF primarily targets endothelial cells, it has been shown to have multiple effects on additional cell types. Primarily, VEGF-mediated pathogenic effects are caused by its effect on vascular permeability and neoangiogenesis (neovascularization) [54].
The severity of expression of genes encoding the process of angiogenesis is reported to be associated with the intensity of physical activity [55]. This confirms the point of view, according to which the change in the “angiogenic switch” stroke is a marker of athletes’ physical performance. Among the studied single nucleotide variants (SNVs) of VEGF, SNVs in the promoter (regulatory) region are of particular interest. For example, the replacement of cytosine with guanine at position −634 (−634 G/C; rs2010963) increases the activity of the gene and, accordingly, determines individual differences in the level of its expression [56].
Akhmetov et al. [5] investigated the frequency distribution of VEGF-A alleles in athletes involved in cyclic sports and in a control group of subjects not involved in sports. The authors also evaluated the association of the studied SNV rs2010963 (−634 G/C) genotypes of VEGF with the aerobic performance of athletes and the control group. The frequency of the C allele in the control group was 25.3% in women and 23.6% in men (p ≤ 0.05). The distribution of genotypes in the control group was as follows: GG—57.6%; GC—35.8%; CC—6.6%. The frequency of the C allele was statistically significantly higher in the group of athletes than in the control group (29.2% versus 24.5%, respectively; p = 0.0026). The distribution of genotypes among athletes was as follows: GG—50.6%; GC—40.4%; CC—9%. Analysis of the distribution of alleles in men and women did not reveal statistically significant differences in both groups (p ≥ 0.05). A higher frequency of the C allele was found in long-distance runners compared to athletes in other sports. This indicates that the C allele can be a genetic predictor of the development and endurance manifestation in athletes.
Considering that SNVs of the VEGF gene promoter can alter the expression of the VEGF gene and the level of the VEGF-A protein in tissues, Prior et al. [57] suggested that SNVs −2578/−1154/−634 in the promoter region of the VEGF gene are associated with the expression of VEGF in human myoblasts and maximal oxygen consumption (MOC) before and after aerobic exercise. The authors analyzed the effect of the VEGF promoter region haplotype −2578/−1154/−634 on the VEGF expression using the luciferase reporter assay in cultured human myoblasts. In a study with exposure to hypoxia, it was found that haplotypes CGG and AGG showed the lowest hypoxic induction (1.5 and 2.0 times, respectively), while haplotypes AAG and CGC showed the highest hypoxic induction of the VEGF gene expression (3.1 and 3.2 times, respectively). According to the authors, the results obtained demonstrated the potential functional effect of SNVs −2578, −1154, and −634 as follows: the combination of G-alleles (AGG and CGG haplotypes) leads to a decrease in the VEGF gene expression in cultured human myoblasts compared to the AAG and CGC haplotypes; the presence of A or C alleles in −2578 SNV (the first position in the haplotype) did not statistically significantly affect the expression of the VEGF gene. The data obtained showed that the influence of these haplotypes corresponded to the dominant/recessive genetic model, given that only subjects with two copies of AGG or CGG haplotypes showed low BMD. Subjects with ≥1 copy of AAG or CGC haplotypes showed higher BMD values. As none of these three SNVs has been found at any particular transcription factor binding site identified to date, the exact mechanism of the effects of the VEGF −2578/−1154/−634 haplotype on the VEGF gene expression remains unknown. It is possible that these SNVs disrupt binding sites for transcription factors that are not yet identified or affect interactions between transcription factors. For example, the hypoxia response element (HRE) in the promoter region of the VEGF gene (5′-position from −2012 to −2005) requires interaction with the upstream protein activator−1 (5′-position from −2166 to −2160) and the downstream protein activator −2α (5′-position from −1117 to −1110), which lie within the test sequence in the promoter region. The authors suggested that SNVs −1154 and/or −634 might somehow influence these interactions [57].
Studies conducted by Arsic et al. [8] used immunohistochemical analysis to show that in intact muscle fibers neither VEGFR-1 nor VEGFR-2 is expressed. In contrast, damage to muscle fibers led to a marked increase in the presence of these receptors. In particular, both receptors were strongly expressed by elongated cells surrounding the newly formed fibers, which could be identified by the presence of a central nucleus resembling the appearance of activated satellite cells at the edge of regenerating fibers. Expression was detected early after injury and persisted until later stages of the regenerative process. In addition, highly expressed VEGFR-2 was found on the surface of mature muscle fibers in the early recovery period after injury. Most strikingly, overexpression of PlGF, a VEGFR-1 agonist, did not promote muscle regeneration after injury, even at very high doses of the vector. These results clearly indicate that VEGFR-2 is a major mediator of VEGF action on myogenic cells.
Currently, at least two signaling pathways are known that are important for muscle regeneration. The first pathway is the activation of VEGFR-2 in endothelial cells, namely, PI3K/Akt. The second is kinase pathways that lead to increased expression and activity of the MyoD protein. Activation of Akt signaling in muscle cells is important for the suppression of apoptosis during differentiation and growth of myofibrils [58]. Interestingly, insulin growth factor-1, a powerful promoter of muscle regeneration that stimulates muscle differentiation through Akt, also increases VEGF synthesis in cells, indirectly suggesting the involvement of VEGF in the regeneration process [59]. Accordingly, muscle fibers transduced with active Akt also produce increased levels of VEGF and show signs of muscle hypertrophy. Thus, the SNV rs2010963 (−634 G/C) of the VEGF gene is associated with the physical performance of athletes and plays a key role in sports selection. The role of other studied SNVs needs to be clarified. The results of these studies are of both fundamental and applied importance as they contribute to a better understanding of the molecular adaptation mechanisms of the cerebrovascular and cardiovascular systems to aerobic loads as well as facilitate the choice of optimal sports specialization and type of professional training of athletes.
2.2. Fibroblast Growth Factor (FGF)
2.2.1. The Role of FGF in Angiogenesis in Athletes
Fibroblast growth factor (FGF) was originally identified as a protein capable of stimulating fibroblast proliferation. It is currently known to have 22 isoforms, although there are only 18 receptors for them (FGFR). Four FGF isoforms (FGF11, FGF12, FGF13, and FGF14) do not bind to FGFR [60]. FGFs perform multiple functions through FGFR binding and activation. Activated FGFRs mediate signaling by recruiting specific molecules that bind to phosphorylated tyrosine in the cytosolic portion of the receptor, triggering a number of signaling pathways leading to specific cellular responses. They then serve as docking sites, docking proteins, or signaling enzymes. Signaling complexes are formed and recruited to active receptors, leading to a cascade of phosphorylation events [61]. The main signaling pathway for stimulating FGFRs is the RAS/MAP kinase pathway, and the PI3/AKT kinase pathway and the PLCγ pathway have also been studied. Unlike other growth factors, FGF works with heparin or heparan sulfate proteoglycan (HSPG) to activate FGFR and induce pleiotropic responses that lead to a variety of cellular responses [62]. Expression of FGF-binding proteins (FGFBP) can modulate FGF-dependent vascular permeability and is considered to be an “angiogenic switch” in the regeneration of many tissues, including skeletal muscle, tendons, myocardium, blood vessels, lung, and nervous tissue [60]. The physiological role of FGFs as an “angiogenic switch” depends on the FGF signaling pathway. This interaction results in new sites for a set of proteins that are responsible for the activation or weakening of signaling [30]. Four isoforms of FGF (FGF1, FGF2, FGF4, and FGF6) are the most studied as proangiogenic factors.
FGF and the “Angiogenic Switch” in Skeletal Muscle
Skeletal muscle regeneration is largely controlled by FGFs, which are abundant in the regenerating muscle regions. Of greatest interest is the FGF6 isoform, as it is most specific for muscles and is strongly activated upon injury [63].
Yablonka-Reuveni et al. studied the role of FGF in recruiting skeletal muscle satellite cells. They demonstrated the high efficiency of the FGF2 isoform in stimulating the proliferation of satellite cells [64]. Doukas et al. investigated the activity of FGF isoforms in skeletal muscle recovery. In particular, plasmid and adenoviral vectors were immobilized in a collagen–gelatin mixture, which was then delivered to damaged muscle tissue. The results demonstrated an angiogenic response in muscles (microvascular development) in the early stages of injury. Subsequently, the authors discovered arteriogenesis or the development of higher-order vessels, which contained medial layers of smooth muscle cells, as well as increased muscle tube regeneration after delivery of FGF2 or FGF6 isoforms to damaged muscle tissue [65,66][65][66].
Richardson R.S. studied the expression of angiogenic growth factors in skeletal muscles in response to a single physical exercise (in particular, b-FGF and a-FGF in the gastrocnemius muscles) [67]. Animal models were injected with b-FGF and a-FGF intramuscularly into the right gastrocnemius muscle. Exercise significantly reduced vascularization in both the right and left calf muscles compared to control (without exercise), probably because of changes in muscle mass. Intramuscular injection of b-FGF significantly increased vascularization locally in the right muscle into which it was injected, while intramuscular injection of a-FGF did not lead to vascularization of the right muscle. With the simultaneous administration of angiogenic factors and physical activity, only b-FGF caused a significant local increase in vascular growth in the muscle under study. Neither b-FGF nor a-FGF elicited any angiogenic action on the left side. This can be explained by the one-sided effect of exercise.
FGF and “Angiogenic Switch” in the Myocardium
Left ventricular hypertrophy is an adaptive response of the heart to exercise, but it is also a risk factor for cardiovascular mortality. Among the factors contributing to the transition from adaptive to pathological remodeling of the heart, an imbalance of the “angiogenic switch”, leading to the development of defects in cardiac angiogenesis and vascularization, plays a significant role [14]. Changes in hemodynamic and mechanical factors, as well as hypoxia, leading to a mismatch between the oxygen demand of the heart and its blood supply, stimulate the release of angiogenic growth factors from cardiomyocytes in order to cause a parallel growth of the feeding vasculature.
Major fibroblast growth factor (bFGF, also called FGF2) is also expressed in endothelial cells, including the heart, and has been shown to enhance the development of vascular collaterals in the myocardium in an animal model of coronary occlusion in dogs [68]. Rajanayagam et al. established the proangiogenic role of FGF2 in canine ischemic myocardium [69].
Alternatively, the role of FGF2 in myocardial vascularization during hypoxia caused by pressure overload is less well understood. For example, thyroxine, a potent stimulator of cardiac hypertrophy and vascularization, has been shown to enhance FGF2 expression and increase cardiac capillary endothelial cell proliferation and angiogenesis [70].
Santiago et al. investigated the differential effects of high and low molecular weight FGF2 isoforms on myocardial hypertrophy, fibrosis, and inflammation [71]. Echocardiographic measurements, gravimetry, and cross-sectional area of cardiomyocytes showed that the absence of FGF2 results in a statistically less degree of hypertrophy during pressure overload. The presented results demonstrate that FGF2 is the main stimulating component of the growth of myocardial hypertrophy. In addition, it was shown that hemodynamic stress, rather than FGF2 and myocardial hypertrophy, correlates with switching of the studied isoforms. Despite the fact that transcriptional and post-transcriptional control determine the ratios of myosin isoforms in cardiomyofibrils, the isoform switching that occurs during hemodynamic stress is the result of changes in transcriptional rather than posttranscriptional regulation.
Yajima et al. evaluated whether FGF2 and/or heparin, which induce angiogenesis, affect myocardial function in hypertensive conditions [72]. The study showed that intramyocardial injection of FGF2 (plus heparin) in rats with hypertensive myocardial hypertrophy was associated with significant improvements in systolic pumping function and ventricular dilatation, as well as an increase in myocardial capillary density.
Chen et al. investigated other isoforms of FGF, such as acidic fibroblast growth factor (sp-FGF1) or FGF1 [73]. It has been found that a secreted version of the FGF1 gene contributes to the functional improvement of disrupted endothelial progenitor cells and that autologous transplantation of modified sp-FGF1 in these cells may promote neovascularization in a porcine model of chronic myocardial ischemia.
To elucidate the pathophysiological role of FGF in cardiomyopathy, Tomita et al. evaluated myocardial biopsies from 24 patients (nine with hypertrophic cardiomyopathy, 12 with dilated cardiomyopathy, and three with hypertensive hypertrophy) and six controls. All samples were stained for FGF1 (also known as aFGF) and basic FGF (bFGF) by immunohistochemistry. FGF expression was significantly increased in cardiomyocytes obtained from the left ventricle of patients with cardiomyopathy. As it was revealed, FGF-1 can promote myocardial hypertrophy as a reparative response to myocardial damage in patients with idiopathic cardiomyopathy [74].
In recent years, a significant amount of knowledge has been accumulated on the regulation of the formation of new vessels in a hypertrophied heart [14]. It became clear that myocardial endothelial cells not only respond to hemodynamic forces and paracrine signals from neighboring cells, but also actively participate in the processes of cardiac remodeling, stimulating the growth and contractility of cardiomyocytes or the production of extracellular matrix proteins in myofibroblasts. Moreover, in response to adequate signals, they can change their phenotype and transdifferentiate into extracellular cells that produce matrix. As myocardial vascularization plays a central role in the transition from adaptive cardiac hypertrophy to heart failure, endothelial cells and signaling mechanisms involved in the regulation or dysregulation of angiogenesis in the myocardium represent promising therapeutic targets for improving cardiac remodeling caused by pressure overload and preventing the transition to heart failure, which is important in sports practice.
FGF and the “Angiogenic Switch” in the Cerebrovascular and Cardiovascular Systems
FGFs constitute one of the most versatile and complex families of signaling in vertebrates, playing critical roles in a wide variety of biological processes, including a wide range of vascular functions. The multiple isoforms of FGFs generated by alternative splicing may play different roles in vascular development. FGFs are broad-spectrum mitogens that stimulate various cellular functions, including migration, proliferation, and differentiation [75]. The expression pattern of FGFs is highly variable, from almost ubiquitous (FGF1 and FGF2) to highly restricted, to certain cell subpopulations at certain stages of development (FGF3, FGF4, FGF8, FGF17, and FGF19). In pathological conditions such as inflammation, etc., FGF is secreted in large amounts by various types of cells, including monocytes, tissue macrophages, endothelial cells, stromal cells, and tumor cells [76].
Despite the recognition of FGF as a strong proangiogenic factor, the deciphering of its exact functions in the vascular system has not been adequately studied [77]. Mutations in the Fgfr1 or Fgfr2 genes in mouse embryos led to embryonic lethality at very early stages of development, which makes it impossible to further assess their contribution to vascular development [78]. By contrast, studies of angiogenic FGF isoforms such as FGF1 and FGF2 did not reveal abnormalities in embryonic vascular development, implying that there is significant redundancy in the system of these isoforms [79]. One of the difficulties in investigating the FGF system arises from its erratic action on various types of cells and tissues. However, using tissue-specific promoters, recent research has begun to uncover the role of FGFs in the “angiogenic switch” in the cardiovascular and cerebrovascular systems.
Analysis of FGF signaling in the vasculature of adult mice revealed a significant contribution of FGF to vascular development as well as maintaining vascular integrity. In adult mice, FGF is required for basal endothelial signaling and maintenance of vascular homeostasis. Inhibition of signaling through FGF leads to disassembly of endothelial junctions, progressing to severe disruption of vascular integrity [80]. In contrast to VEGF, which causes degradation of VE-cadherin-based compounds through activation of Src, FGF enhances the adhesion of the compounds by enhancing the binding of VE-cadherin to p120 catenin. The critical role of FGF signaling in neovascularization is also demonstrated in a more recent study that describes the cross-signaling mechanism between FGF and VEGF. The VEGFR2 gene expression levels are tightly controlled by endothelial FGF signaling, which is capable of activating VEGFR2 transcription through an Ets-dependent manner. Thus, FGF indirectly promotes neovascularization by regulating endothelial sensitivity to VEGF [81]. It has been repeatedly shown that although FGF-induced neovascularization is often impaired by VEGF inhibition in various angiogenic models, VEGF-induced vascular formation is not so strongly affected by depletion of FGF signaling [82]. Together, these studies support the hierarchical control of new vessel formation by which the FGF system promotes new vessel growth by controlling VEGF signaling.
References
- Baeriswyl, V.; Christofori, G. The angiogenic switch in carcinogenesis. Semin. Cancer Biol. 2009, 19, 329–337.
- Ribatti, D.; Nico, B.; Crivellato, E.; Roccaro, A.M.; Vacca, A. The history of the angiogenic switch concept. Leukemia 2007, 21, 44–52.
- Ruoslahti, E. Specialization of tumour vasculature. Nat. Rev. Cancer 2002, 2, 83–90.
- Apte, R.S.; Chen, D.S.; Ferrara, N. VEGF in Signaling and Disease: Beyond Discovery and Development. Cell 2019, 176, 1248–1264.
- Akhmetov, I.I.; Khakimullina, A.M.; Popov, D.V.; Missina, S.S.; Vinogradova, O.L.; Rogozkin, V.A. Polymorphism of the vascular endothelial growth factor gene (VEGF) and aerobic performance in athletes. Fiziol. Cheloveka 2008, 34, 97–101.
- Barroso, G.C.; Thiele, E.S. Muscle Injuries in Athletes. Rev. Bras. Ortop. 2015, 46, 354–358.
- Yan, Z.; Choi, S.; Liu, X.; Zhang, M.; Schageman, J.J.; Lee, S.Y.; Hart, R.; Lin, L.; Thurmond, F.A.; Williams, R.S. Highly coordinated gene regulation in mouse skeletal muscle regeneration. J. Biol. Chem. 2003, 278, 8826–8836.
- Arsic, N.; Zacchigna, S.; Zentilin, L.; Ramirez-Correa, G.; Pattarini, L.; Salvi, A.; Sinagra, G.; Giacca, M. Vascular endothelial growth factor stimulates skeletal muscle regeneration in Vivo. Mol. Ther. 2004, 5, 844–854.
- Murry, C.; Soonpaa, M.; Reinecke, H.; Nakajima, H.; Nakajima, H.O.; Rubart, M.; Pasumarthi, K.B.S.; Virag, J.I.; Bartelmez, S.H.; Poppa, V.; et al. Haematopoietic stem cells do not transdifferentiate into cardiac myocytes in myocardial infarcts. Nature 2004, 428, 664–668.
- Balsam, L.B.; Wagers, A.J.; Christensen, J.L.; Kofidis, T.; Weissman, I.L.; Robbins, R.C. Haematopoietic stem cells adopt mature haematopoietic fates in ischaemic myocardium. Nature 2004, 428, 668–673.
- Wu, G.; Rana, J.S.; Wykrzykowska, J.; Du, Z.; Ke, Q.; Kang, P.; Li, J.; Laham, R.J. Exercise-induced expression of VEGF and salvation of myocardium in the early stage of myocardial infarction. Am. J. Physiol. Heart Circ. Physiol. 2009, 296, H389–H395.
- Vona, M.; Rossi, A.; Capodaglio, P.; Rizzo, S.; Servi, P.; de Marchi, M.; Cobelli, F. Impact of physical training and detraining on endothelium-dependent vasodilation in patients with recent acute myocardial infarction. Am. Heart J. 2004, 147, 1039–1046.
- Ardakanizade, M. The effects of mid- and long-term endurance exercise on heart angiogenesis and oxidative stress. Iran. J. Basic Med. Sci. 2018, 21, 800–805.
- Gogiraju, R.; Bochenek, M.L.; Schäfer, K. Angiogenic Endothelial Cell Signaling in Cardiac Hypertrophy and Heart Failure. Front. Cardiovasc. Med. 2019, 6, 20.
- Russell, K.S.; Stern, D.F.; Polverini, P.J.; Bender, J.R. Neuregulin activation of ErbB receptors in vascular endothelium leads to angiogenesis. Am. J. Physiol. 1999, 277, H2205–H2211.
- Wang, Z.; Qin, G.; Zhao, T.C. HDAC4: Mechanism of regulation and biological functions. Epigenomics 2014, 6, 139–150.
- Kim, Y.W.; Byzova, T.V. Oxidative stress in angiogenesis and vascular disease. Blood 2014, 123, 625–631.
- Hyatt, H.W.; Smuder, A.J.; Sollanek, K.J.; Morton, A.B.; Roberts, M.D.; Kavazis, A.N. Comparative changes in antioxidant enzymes and oxidative stress in cardiac, fast twitch and slow twitch skeletal muscles following endurance exercise training. Int. J. Physiol. Pathophysiol. Pharmacol. 2016, 8, 160–168.
- Powers, S.K.; DeRuisseau, K.C.; Quindry, J.; Hamilton, K.L. Dietary antioxidants and exercise. J. Sports Sci. 2004, 22, 81–94.
- Rey, S.; Semenza, G.L. Hypoxia-inducible factor-1-dependent mechanisms of vascularization and vascular remodelling. Cardiovasc. Res. 2010, 86, 236–242.
- Keramidas, M.E.; Stavrou, N.A.; Kounalakis, S.N.; Eiken, O.; Mekjavic, I.B. Severe hypoxia during incremental exercise to exhaustion provokes negative post-exercise affects. Physiol. Behav. 2016, 156, 171–176.
- Hoeben, A.; Landuyt, B.; Highley, M.S.; Wildiers, H.; Van Oosterom, A.T.; De Bruijn, E.A. Vascular endothelial growth factor and angiogenesis. Pharmacol. Rev. 2004, 56, 549–580.
- Wu, H.; Naya, F.J.; McKinsey, T.A.; Mercer, B.; Shelton, J.M.; Chin, E.R.; Simard, A.R.; Michel, R.N.; Bassel-Duby, R.; Olson, E.N.; et al. MEF2 responds to multiple calcium-regulated signals in the control of skeletal muscle fiber type. EMBO J. 2000, 19, 1963–1973.
- Maiti, D.; Xu, Z.; Duh, E.J. Vascular endothelial growth factor induces MEF2C and MEF2-dependent activity in endothelial cells. Investig. Ophthalmol. Vis. Sci. 2008, 49, 3640–3648.
- Zhu, Y.; Lee, C.; Shen, F.; Du, R.; Young, W.L.; Yang, G.Y. Angiopoietin-2 facilitates vascular endothelial growth factor-induced angiogenesis in the mature mouse brain. Stroke 2005, 36, 1533–1537.
- Kajstura, J.; Rota, M.; Cappetta, D.; Ogórek, B.; Arranto, C.; Bai, Y.; Ferreira-Martins, J.; Signore, S.; Sanada, F.; Matsuda, A.; et al. Cardiomyogenesis in the aging and failing human heart. Circulation 2012, 126, 1869–1881.
- Dorn, G.W. The fuzzy logic of physiological cardiac hypertrophy. Hypertension 2007, 49, 962–970.
- Ferrara, N.; Gerber, H.P.; LeCouter, J. The biology of VEGF and its receptors. Nat. Med. 2003, 9, 669–676.
- Abhinand, C.S.; Raju, R.; Soumya, S.J.; Arya, P.S.; Sudhakaran, P.R. VEGF-A/VEGFR2 signaling network in endothelial cells relevant to angiogenesis. J. Cell Commun. Signal. 2016, 10, 347–354.
- Braile, M.; Marcella, S.; Cristinziano, L.; Galdiero, M.R.; Modestino, L.; Ferrara, A.L.; Varricchi, G.; Marone, G.; Loffredo, S. VEGF-A in Cardiomyocytes and Heart Diseases. Int. J. Mol. Sci. 2020, 21, 5294.
- Jaipersad, A.S.; Lip, G.Y.; Silverman, S.; Shantsila, E. The role of monocytes in angiogenesis and atherosclerosis. J. Am. Coll. Cardiol. 2014, 63, 1–11.
- Hong, K.H.; Ryu, J.; Han, K.H. Monocyte chemoattractant protein-1-induced angiogenesis is mediated by vascular endothelial growth factor-A. Blood 2005, 105, 1405–1407.
- Ylä-Herttuala, S.; Rissanen, T.T.; Vajanto, I.; Hartikainen, J. Vascular endothelial growth factors: Biology and current status of clinical applications in cardiovascular medicine. J. Am. Coll. Cardiol. 2007, 49, 1015–1026.
- Yu, Z.M.; Deng, X.T.; Qi, R.M.; Xiao, L.Y.; Yang, C.Q.; Gong, T. Mechanism of Chronic Stress-induced Reduced Atherosclerotic Medial Area and Increased Plaque Instability in Rabbit Models of Chronic Stress. Chin. Med. J. Engl. 2018, 131, 161–170.
- Cialoni, D.; Sponsiello, N.; Marabotti, C.; Marroni, A.; Pieri, M.; Maggiorelli, F.; Tonerini, M.; Frammartino, B. Prevalence of acute respiratory symptoms in breath-hold divers. Undersea Hyperb. Med. 2012, 39, 837–844.
- Bove, A.A. Pulmonary Aspects of Exercise and Sports. Methodist. Debakey. Cardiovasc. J. 2016, 12, 93–97.
- Tuder, R.M.; Yun, J.H. Vascular endothelial growth factor of the lung: Friend or foe. Curr. Opin. Pharmacol. 2008, 8, 255–260, Epub 28 May 2008.
- Barratt, S.L.; Flower, V.A.; Pauling, J.D.; Millar, A.B. VEGF (Vascular Endothelial Growth Factor) and Fibrotic Lung Disease. Int. J. Mol. Sci. 2018, 19, 1269.
- Mura, M.; dos Santos, C.C.; Stewart, D.; Liu, M. Vascular endothelial growth factor and related molecules in acute lung injury. J. Appl. Physiol. 2004, 97, 1605–1617.
- Gerber, H.P.; Hillan, K.J.; Ryan, A.M.; Kowalski, J.; Keller, G.A.; Rangell, L.; Wright, B.D.; Radtke, F.; Aguet, M.; Ferrara, N. VEGF is required for growth and survival in neonatal mice. Development 1999, 126, 1149–1159.
- Compernolle, V.; Brusselmans, K.; Acker, T.; Hoet, P.; Tjwa, M.; Beck, H.; Plaisance, S.; Dor, Y.; Keshet, E.; Lupu, F.; et al. Loss of HIF-2alpha and inhibition of VEGF impair fetal lung maturation, whereas treatment with VEGF prevents fatal respiratory distress in premature mice. Nat. Med. 2002, 8, 702–710.
- Barratt, S.L.; Blythe, T.; Jarrett, C.; Ourradi, K.; Shelley-Fraser, G.; Day, M.J.; Qiu, Y.; Harper, S.; Maher, T.M.; Oltean, S.; et al. Differential Expression of VEGF-Axxx Isoforms Is Critical for Development of Pulmonary Fibrosis. Am. J. Respir. Crit. Care Med. 2017, 196, 479–493.
- Henson, P.M.; Bratton, D.L.; Fadok, V.A. The phosphatidylserine receptor: A crucial molecular switch? Nat. Rev. Mol. Cell Biol. 2001, 2, 627–633.
- Golpon, H.A.; Fadok, V.A.; Taraseviciene-Stewart, L.; Scerbavicius, R.; Sauer, C.; Welte, T.; Henson, P.M.; Voelkel, N.F. Life after corpse engulfment: Phagocytosis of apoptotic cells leads to VEGF secretion and cell growth. FASEB J. 2004, 18, 1716–1718.
- Lin, C.K.; Huang, T.H.; Yang, C.T.; Shi, C.S. Roles of lung-recruited monocytes and pulmonary Vascular Endothelial Growth Factor (VEGF) in resolving Ventilator-Induced Lung Injury (VILI). PLoS ONE 2021, 16, e0248959.
- Crosby, L.M.; Waters, C.M. Epithelial repair mechanisms in the lung. Am. J. Physiol. Lung Cell Mol. Physiol. 2010, 298, L715–L731.
- Kim, Y.M.; Kim, S.J.; Tatsunami, R.; Yamamura, H.; Fukai, T.; Ushio-Fukai, M. ROS-induced ROS release orchestrated by Nox4, Nox2, and mitochondria in VEGF signaling and angiogenesis. Am. J. Physiol. Cell Physiol. 2017, 312, C749–C764.
- Medford, A.R.; Douglas, S.K.; Godinho, S.I.; Uppington, K.M.; Armstrong, L.; Gillespie, K.M.; van Zyl, B.; Tetley, T.D.; Ibrahim, N.B.; Millar, A.B. Vascular Endothelial Growth Factor (VEGF) isoform expression and activity in human and murine lung injury. Respir. Res. 2009, 10, 27.
- Herold, S.; Mayer, K.; Lohmeyer, J. Acute lung injury: How macrophages orchestrate resolution of inflammation and tissue repair. Front. Immunol. 2011, 2, 65.
- Burnham, E.L.; Janssen, W.J.; Riches, D.W.; Moss, M.; Downey, G.P. The fibroproliferative response in acute respiratory distress syndrome: Mechanisms and clinical significance. Eur. Respir. J. 2014, 43, 276–285.
- Loftus, T.J.; Thomson, A.J.; Kannan, K.B.; Alamo, I.G.; Millar, J.K.; Plazas, J.M.; Whitley, E.E.; Efron, P.A.; Mohr, A.M. Clonidine restores vascular endothelial growth factor expression and improves tissue repair following severe trauma. Am. J. Surg. 2017, 214, 610–615.
- Koh, H.; Tasaka, S.; Hasegawa, N.; Yamada, W.; Shimizu, M.; Nakamura, M.; Yonemaru, M.; Ikeda, E.; Adachi, Y.; Fujishima, S.; et al. Protective role of vascular endothelial growth factor in endotoxin-induced acute lung injury in mice. Respir. Res. 2007, 8, 60.
- Medford, A.R.; Ibrahim, N.B.; Millar, A.B. Vascular endothelial growth factor receptor and coreceptor expression in human acute respiratory distress syndrome. J. Crit. Care 2009, 24, 236–242.
- Ferrara, N.; Hillan, K.J.; Gerber, H.P.; Novotny, W. Discovery and development of bevacizumab, an anti-VEGF antibody for treating cancer. Nat. Rev. Drug Discov. 2004, 3, 391–400.
- Varet, J.; Douglas, S.K.; Gilmartin, L.; Medford, A.R.; Bates, D.O.; Harper, S.J.; Millar, A.B. VEGF in the lung: A role for novel isoforms. Am. J. Physiol. Lung Cell Mol. Physiol. 2010, 298, L768–L774.
- Watson, C.J.; Webb, N.J.; Bottomley, M.J.; Brenchley, P.E. Identification of polymorphisms within the vascular endothelial growth factor (VEGF) gene: Correlation with variation in VEGF protein production. Cytokine 2000, 12, 1232–1235.
- Prior, S.J.; Hagberg, J.M.; Paton, C.M.; Douglass, L.W.; Brown, M.D.; McLenithan, J.C.; Roth, S.M. DNA sequence variation in the promoter region of the VEGF gene impacts VEGF gene expression and maximal oxygen consumption. Am. J. Physiol. Heart Circ. Physiol. 2006, 290, H1848–H1855.
- Rommel, C.; Bodine, S.C.; Clarke, B.A.; Rossman, R.; Nunez, L.; Stitt, T.N.; Yancopoulos, G.D.; Glass, D.J. Mediation of IGF-1-induced skeletal myotube hypertrophy by PI(3)K/Akt/mTOR and PI(3)K/Akt/GSK3 pathways. Nat. Cell Biol. 2001, 3, 1009–1013.
- Tureckova, J.; Wilson, E.M.; Cappalonga, J.L.; Rotwein, P. Insulin-like growth factor-mediated muscle differentiation: Collaboration between phosphatidylinositol 3-kinase-Akt-signaling pathways and myogenin. J. Biol. Chem. 2001, 276, 39264–39270.
- Yun, Y.R.; Won, J.E.; Jeon, E.; Lee, S.; Kang, W.; Jo, H.; Jang, J.H.; Shin, U.S.; Kim, H.W. Fibroblast growth factors: Biology, function, and application for tissue regeneration. J. Tissue Eng. 2010, 2010, 218142.
- Schlessinger, J. Cell signaling by receptor tyrosine kinases. Cell 2000, 103, 211–225.
- Heineke, J.; Molkentin, J.D. Regulation of cardiac hypertrophy by intracellular signalling pathways. Nat. Rev. Mol. Cell Biol. 2006, 7, 589–600.
- Floss, T.; Arnold, H.H.; Braun, T. A role for FGF-6 in skeletal muscle regeneration. Genes Dev. 1997, 11, 2040–2051.
- Yablonka-Reuveni, Z.; Seger, R.; Rivera, A.J. Fibroblast growth factor promotes recruitment of skeletal muscle satellite cells in young and old rats. J. Histochem Cytochem. 1999, 47, 23–42.
- Doukas, J.; Blease, K.; Craig, D.; Ma, C.; Chandler, L.A.; Sosnowski, B.A.; Pierce, G.F. Delivery of FGF genes to wound repair cells enhances arteriogenesis and myogenesis in skeletal muscle. Mol. Ther. 2002, 5 Pt 1, 517–527.
- Fiore, F.; Sébille, A.; Birnbaum, D. Skeletal muscle regeneration is not impaired in Fgf6 -/- mutant mice. Biochem Biophys Res Commun. 2000, 272, 138–143.
- Richardson, R.S. Complementary studies of exercised-induced angiogenic growth factors in human skeletal muscle. Am. J. Physiol Heart Circ. Physiol. 2000, 279, H3146–H3147.
- Lazarous, D.F.; Shou, M.; Stiber, J.A.; Dadhania, D.M.; Thirumurti, V.; Hodge, E.; Unger, E.F. Pharmacodynamics of basic fibroblast growth factor: Route of administration determines myocardial and systemic distribution. Cardiovasc. Res. 1997, 36, 78–85.
- Rajanayagam, M.A.; Shou, M.; Thirumurti, V.; Lazarous, D.F.; Quyyumi, A.A.; Goncalves, L.; Stiber, J.; Epstein, S.E.; Unger, E.F. Intracoronary basic fibroblast growth factor enhances myocardial collateral perfusion in dogs. J. Am. Coll Cardiol. 2000, 35, 519–526.
- Tomanek, R.J.; Doty, M.K.; Sandra, A. Early coronary angiogenesis in response to thyroxine: Growth characteristics and upregulation of basic fibroblast growth factor. Circ. Res. 1998, 82, 587–593.
- Santiago, J.J.; McNaughton, L.J.; Koleini, N.; Ma, X.; Bestvater, B.; Nickel, B.E.; Fandrich, R.R.; Wigle, J.T.; Freed, D.H.; Arora, R.C.; et al. High molecular weight fibroblast growth factor-2 in the human heart is a potential target for prevention of cardiac remodeling. PLoS ONE 2014, 9, e97281.
- Yajima, S.; Ishikawa, M.; Kubota, T.; Moroi, M.; Sugi, K.; Namiki, A. Intramyocardial injection of fibroblast growth factor-2 plus heparin suppresses cardiac failure progression in rats with hypertensive heart disease. Int. Heart J. 2005, 46, 289–301.
- Chen, S.Y.; Wang, F.; Yan, X.Y.; Zhou, Q.; Ling, Q.; Ling, J.X.; Rong, Y.Z.; Li, Y.G. Autologous transplantation of EPCs encoding FGF1 gene promotes neovascularization in a porcine model of chronic myocardial ischemia. Int. J. Cardiol. 2009, 135, 223–232.
- Tomita, Y.; Kusama, Y.; Seino, Y.; Munakata, K.; Kishida, H.; Hayakawa, H. Increased accumulation of acidic fibroblast growth factor in left ventricular myocytes of patients with idiopathic cardiomyopathy. Am. Heart J. 1997, 134, 779–786.
- Murakami, M. Signaling required for blood vessel maintenance: Molecular basis and pathological manifestations. Int. J. Vasc. Med. 2012, 2012, 293641.
- Powers, C.J.; McLeskey, S.W.; Wellstein, A. Fibroblast growth factors, their receptors and signaling. Endocr. Relat. Cancer 2000, 7, 165–197.
- Murakami, M.; Simons, M. Fibroblast growth factor regulation of neovascularization. Curr. Opin. Hematol. 2008, 15, 215–220.
- Lavine, K.J.; White, A.C.; Park, C.; Smith, C.S.; Choi, K.; Long, F.; Hui, C.C.; Ornitz, D.M. Fibroblast growth factor signals regulate a wave of Hedgehog activation that is essential for coronary vascular development. Genes Dev. 2006, 20, 1651–1666.
- Miller, D.L.; Ortega, S.; Bashayan, O.; Basch, R.; Basilico, C. Compensation by fibroblast growth factor 1 (FGF1) does not account for the mild phenotypic defects observed in FGF2 null mice. Mol. Cell Biol. 2000, 20, 2260–2268, Erratum in 2000, 20, 3752.
- Murakami, M.; Nguyen, L.T.; Zhuang, Z.W.; Moodie, K.L.; Carmeliet, P.; Stan, R.V.; Simons, M. The FGF system has a key role in regulating vascular integrity. J. Clin. Investig. 2008, 118, 3355–3366, Erratum in 2009, 119, 2113.
- Murakami, M.; Nguyen, L.T.; Hatanaka, K.; Schachterle, W.; Chen, P.Y.; Zhuang, Z.W.; Black, B.L.; Simons, M. FGF-dependent regulation of VEGF receptor 2 expression in mice. J. Clin. Investig. 2011, 121, 2668–2678.
- Presta, M.; Dell’Era, P.; Mitola, S.; Moroni, E.; Ronca, R.; Rusnati, M. Fibroblast growth factor/fibroblast growth factor receptor system in angiogenesis. Cytokine Growth Factor Rev. 2005, 16, 159–178.
More
