Polycystic Kidney Disease (PKD) is a disorder that affects the kidneys and other organs, and its major forms are encoded by polycystin-1 (PC1) and polycystin-2 (PC2), as PKD1 and PKD2. It is located sandwiched inside and outside cell membranes and interacts with other cells. This protein is most active in kidney cells before birth, and PC1 and PC2 work together to help regulate cell proliferation, cell migration, and interactions with other cells. The molecular relationship and the function between PKD1 and cancer is well known, such as increased or decreased cell proliferation and promoting or suppressing cell migration depending on the cancer cell type specifically.
- PKD1
- umbilical cord blood-derived mesenchymal stem cell (UCB-MSC)
- stemness
- osteogenic differentiation
1. Introduction
Cell therapy is one of the basic treatments used in regenerative medicine and tissue engineering. Among the cells used in cell therapy, stem cells are now used as an indispensable element in the development of artificial organs called organoids. Stem cells are an undifferentiated state cell that has self-renewal ability and is a pluripotent cell that can develop into any tissue [1]. It is also known to have various functions such as peripheral secretion signal, immune regulation, apoptosis prevention, and blood supply by angiogenesis [2]. There are many reports that stem cell-based cell therapies have excellent effects and application ability, and various studies are under-explored for the clinical use of stem cells [3].
However, stem cells still have a long way to go due to the major shortcomings, such as the limitations of cell viability, cell proliferation, time-dependent cell passage, cell expansion, and the differentiation into desired cells, in an administered site in vivo. Its curative efficacy will be significantly greater than it is now if they can overcome the disadvantages in stem cell-based cell therapies. Many studies have introduced various methods to overcome the shortcomings of stem cells. It has been researched to improve the viability and differentiation of stem cells by enhancing the function of stem cells through genetic engineering and producing stem cell complexes using biocompatible materials and nanomaterials. New and fusion methods are required to further enhance the efficacy of stem cells [2][3][4]. From this point of view, we focused on PKD genes as genetic material to overcome the obstacles of stem cells.
However, stem cells still have a long way to go due to the major shortcomings, such as the limitations of cell viability, cell proliferation, time-dependent cell passage, cell expansion, and the differentiation into desired cells, in an administered site in vivo. Its curative efficacy will be significantly greater than it is now if they can overcome the disadvantages in stem cell-based cell therapies. Many studies have introduced various methods to overcome the shortcomings of stem cells. It has been researched to improve the viability and differentiation of stem cells by enhancing the function of stem cells through genetic engineering and producing stem cell complexes using biocompatible materials and nanomaterials. New and fusion methods are required to further enhance the efficacy of stem cells [2,3,4]. From this point of view, we focused on PKD genes as genetic material to overcome the obstacles of stem cells.
Polycystic kidney disease (
PKD) is a genetic disorder in which a specific protein is generated by an abnormal gene and the kidney tubules are abnormally deformed, causing multiple cysts in the kidney to cause developmental disorders [5][6][7][8]. When this protein causes multiple cysts filled with fluid in the nephron in the kidney, the size of the kidney becomes larger than normal, and the tissue is damaged, leading to physiological dysfunction [9].
) is a genetic disorder in which a specific protein is generated by an abnormal gene and the kidney tubules are abnormally deformed, causing multiple cysts in the kidney to cause developmental disorders [5,6,7,8]. When this protein causes multiple cysts filled with fluid in the nephron in the kidney, the size of the kidney becomes larger than normal, and the tissue is damaged, leading to physiological dysfunction [9].
Eighty-five percent of
PKDs
are caused by mutations in the polycysin-1 protein of the gene. Polycystin-1 is called
PKD1
or
PC1
, and this protein is the most active in kidney cells before birth and interacts and functions with polycystin-2
(PKD2
) [10]. According to the current study, there is no precise treatment with the development of
PKD caused by mutation, and the correlation with other cells has not been studied much [11][12][13][14]. Only a study on the correlation with cancer cells was recently published. Although it is known that
caused by mutation, and the correlation with other cells has not been studied much [11,12,13,14]. Only a study on the correlation with cancer cells was recently published. Although it is known that
PKD1
affects cell growth, proliferation, and migration, the results were observed differently depending on cancer cell lines [15].
PKD1
also regulates cell proliferation and cell migration through mammalian target of rapamycin (mTOR) and Janus kinase (JAK) signals, but in the lung cancer cell line (A549),
PKD1 inhibits cell migration and functions as a tumor-suppressor protein in some cases. On the other hand, the glioblastoma cell line (GOS3) showed different results in the cell line, such as acting as a tumor gene protein by improving cell migration, but the exact mechanism has not been revealed [12][15][16]. There is still a controversial part about the function of the
inhibits cell migration and functions as a tumor-suppressor protein in some cases. On the other hand, the glioblastoma cell line (GOS3) showed different results in the cell line, such as acting as a tumor gene protein by improving cell migration, but the exact mechanism has not been revealed [12,15,16]. There is still a controversial part about the function of the
PKD
gene, but it affects cell growth, proliferation, and migration with
PKD2 [7][10][17][18]. Although there are various reports of
[7,10,17,18]. Although there are various reports of
PKD
gene in cancer cell, the function and relationship between the
PKD
gene and stem cells has not been reported so far.
2. Expression of PKD1 at Transcript and Protein Level in Various Cell Lines
In order to confirm the expression level of PKD1 in stem cells, RNA at the transcriptome level was extracted from various cell lines, and then cDNA was synthesized by RT-PCR from each cells. The various cells used for this experiment are adipose-derived mesenchymal stem cell (ADSC), breast cancer cell MCF7, MCF7 breast cancer-derived stem cell (BCSC), lung cancer cell A549, and umbilical cord blood-derived mesenchymal stem cell (UCB-MSC). After conventional PCR for the detection of PKD1 gene, GAPDH was normalized and graphed to quantify the data [19]. As shown in the results of , the expression level of the PKD1 gene was differently observed by cell lines. Among them, PKD1 expression in UCB-MSC and BCSC was observed lower compared with those of other cells. Especially, stem cells showed different PKD1 expression depending on their derived origins. As shown in A, quantitative data of the detected band of PKD1 also showed a similar tendency (B). Therefore, based on this result, we generated over-expression vectors tagged with the GFP gene to identify the function of PKD1 in this stem cell. Lentiviral vector with PKD1 and GFP expression cassette was characterized and validated in . The expression of PKD1 in UCB-MSC by this vector was confirmed in the results of . Green fluorescent protein-expressing vector (gWIZ/GFP) was used as positive control againstPKD1
-expressing vector.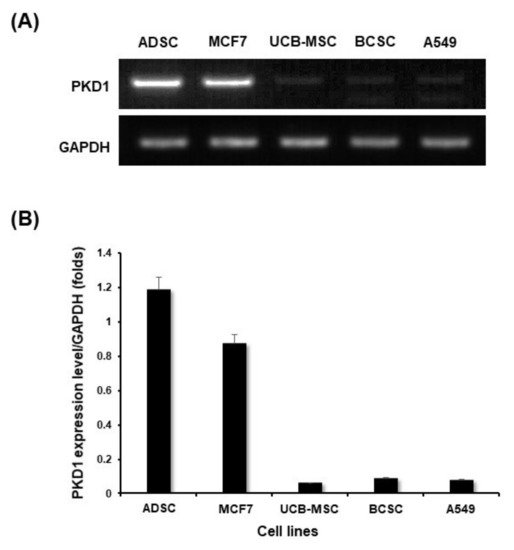
Figure 1.
A
PKD1
B
PKD1
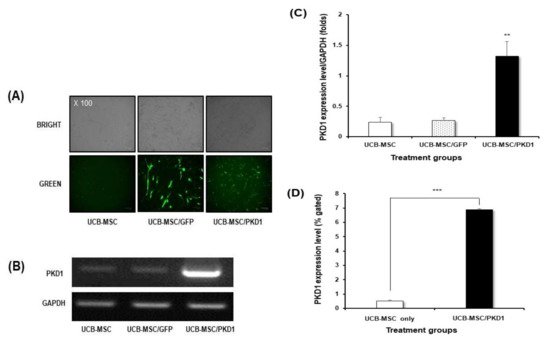
Figure 2.
PKD1
PKD1
A
PKD1
PKD1
B
C
PKD1
D
PKD1
n
p
p
PKD1
-expressing vector was well transfected despite stem cells being known to have poor transfection efficiency. For this,PKD1
vector with a large gene size of 12 Kbs was transfected twice to induce an efficient expression of gene under the conditions of minimal toxicity. Next, we checked at the transcript level through RNA extraction after transfection to confirm whether thePKD1
gene is well expressed by the transfectedPKD1
vector. As shown in the result in B, the highestPKD1
expression was examined in the cells transfected withPKD1
vector. The transfectedPKD1
vector induced higherPKD1
expression than those of other groups. These patterns were similarly observed in quantitative data (C).PKD1 spans the cell membrane of cells, with one end of the protein present in the cell and the other protruding out of the cell for the extracellular mechanical stimulation into intracellular biochemical signals [15][16][17][18]. Therefore, we examined whether
spans the cell membrane of cells, with one end of the protein present in the cell and the other protruding out of the cell for the extracellular mechanical stimulation into intracellular biochemical signals [15,16,17,18]. Therefore, we examined whetherPKD1
is actually well expressed at the protein level byPKD1
expression vector via flow cytometry. As shown in the flow cytometer analysis (D), the cell transfected withPKD1
vector showed the increasedPKD1
expression compared with that of non-transfected cells. Taken together, these results mean that thePKD1
expression system works well in UCB-MSC.3. The Biological Functions of PKD1 in UCB-MSC Effects of PKD1 on Cell Expansion and under the Condition of Oxidative Stress in UCB-MSC
After checking
PKD1
by
PKD1
-expressing vector, we assessed how this gene actually affects in stem cells when it is expressed. It is known that
PKD1
has a function of cell proliferation, but some studies now report that the function of
PKD
varies from cell to cell. To examine this in stem cells, a cell proliferation experiment was carried out by MTT assay in a time-dependent manner. In the result of
A, cell viability did not increase significantly in
PKD1
-transfected UCB-MSC compared with those of other treated groups at all the times tested. This result demonstrates that the expression of
PKD1
did not affect cell proliferation in UCB-MSC, although
PKD1
originally had a function of cell proliferation.
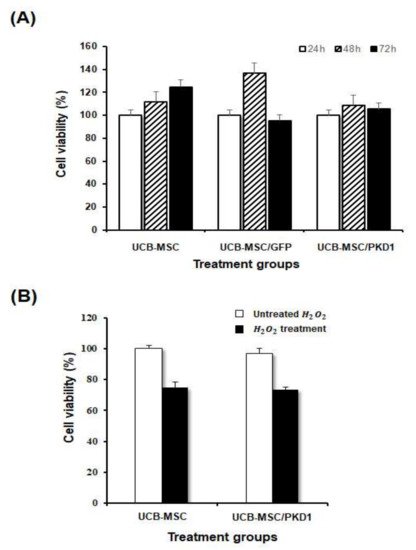
Figure 3.
PKD1
PKD1
PKD1
PKD1
A
B
2
2
n
It is known that the
PKD gene correlates with the oxidative stress pathway in relation to the RTK/MAPK pathway in other cancer cell lines, including bladder cancer [20][21][22]. Therefore, we evaluated whether
gene correlates with the oxidative stress pathway in relation to the RTK/MAPK pathway in other cancer cell lines, including bladder cancer [20,21,22]. Therefore, we evaluated whether
PKD1
expressed in stem cells is resistant to oxidative stress. After selecting the optimal concentration of hydrogen peroxide (H
2
O
2
) to mimic oxidative cellular damage, the antioxidant function of
PKD
was evaluated.
As a result, H
2
O
2
well induced the cytotoxicity in UCB-MSC and the cell viability of UCB-MSC transfected with
PKD1
also decreased (
B), which is consistent with the above proliferation result (
A). In addition, there was no significant difference between the results of
PKD1
-expressing cells treated with H
2
O
2
(UCB-MSC/
PKD1
+ H
2
O
2
group) and non-transfected cells treated with H
2
O
2
(UCB-MSC + H
2
O
2
group). This result means that the
PKD1
gene is ineffective against oxidative stress.
Polycystin-1 also regulates cell proliferation and cell migration through mTOR and JAK signals in the cancer cell line [15][17]. Based on this fact, we evaluated whether
also regulates cell proliferation and cell migration through mTOR and JAK signals in the cancer cell line [15,17]. Based on this fact, we evaluated whether
PKD1
gene affects the migration of stem cells. For this, when the cell confluence reached 80%, scratches were given at regular intervals with a 200 μL pipette tip, and the same part was brightly photographed at 0 and 12 h using a microscope. At 12 h, the cell was stained with crystal violet solution to more accurately check the degree of migration (
A). The scratch area at 0 h and the scratch area at 12 h were photographed with a microscope and then measured and graphed to confirm the reduced area using image J (
B). Using Pixels as the mean value, the pixels at 0 and 12 h were measured by repeating three times each, and the average values for each group measured by image J are shown in the
. As shown in the results, all groups showed a decreased area at 12 h compared to 0 h. However, UCB-MSC transfected with
PKD1
significantly observed a decreased area by migrated cells at 12 h compared with that of 0 h. These results demonstrate that
PKD1
has a great influence on the migration of UCB-MSC, meaning that this could improve stem cell mobility to target areas.
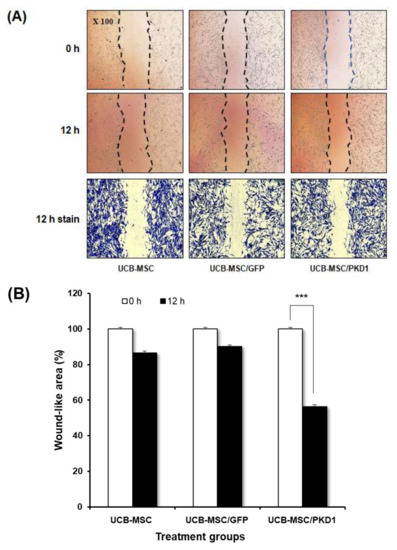
Figure 4.
Improved cell migration ability of UCB-MSC by
PKD1
expression. (
A
) To the migration ability of UCB-MSC in the presence of
PKD1
expression, the cells were scratched by a 200 uL pipette tip. At 12 h, the cells were stained with crystal violet; (
B
) Open area was calculated using image J and quantified by percentage values. Data shown represent the mean ± SD (
n
= 3).
*** p
< 0.01 for the comparison of 0 h and 12 h in
PKD1
expressing UCB-MSC.
4. Discussion
Some studies about
PKD
, which is known as a mutant gene that causes autosomal dominant polycystic kidney disease (
PKD
), reported only basic functions in the kidney. Biologically, the amount of
PKD
protein produced in normal adults is very small, and most are produced in kidney cells before birth. Structurally speaking, this protein is a form that spans the inside and outside of the cell membrane, and it is known that this affects the growth, proliferation, and migration of cells. Among the two types (
PKD1
and
PKD2
) of
PKD
gene, the function of
PKD1
and its role in various cells have not been identified yet. Most recently, some papers have been published on the correlation between
PKD1
and
PKD2 and cancer [7][8][10][17][18]. These studies have revealed many of the functions of
and cancer [7,8,10,17,18]. These studies have revealed many of the functions of
PKD
proteins. The correlation between cancer cell lines and
PKD was studied through the mTOR and JAK signaling pathway [14][15][16][23]. As a result, unlike what is known, the function of
was studied through the mTOR and JAK signaling pathway [14,15,16,26]. As a result, unlike what is known, the function of
PKD
showed different results depending on the cancer cell line, and the opposite result was also shown [15]. Therefore, its research is still controversial and limited. Based on these reference papers, we attempted to evaluate the biological function of
PKD1
in stem cells and to overcome the obstacles induced when stem cells are administrated in vivo, using the biological function of
PKD1
.
For this, the expression of the
PKD1
gene in various cells was confirmed, and UCB-MSC showed a low expression level of
PKD1
among stem cells derived from various origins (
). Therefore, the function of the
PKD1
gene in UCB-MSC was evaluated after the transfection of over-expressing vectors to induce
PKD1
high expression. The confirmation of
PKD1
expression was assessed at the transcript and protein level (
). In this study, we tried two transfections because stem cells are known to have low transfection efficiency by DNA degradation before going to the nucleus, and they have the properties of primary cells. In addition, considering that the
PKD1
plasmid vector size used in this experiment was 19.5 kbs, the cells were transfected twice. The actual expression of
PKD1
was confirmed through the FACS analysis results, using the characteristic that
PKD1
spans the cell membrane structurally. In conclusion, we checked
PKD1
expression in UCB-MSC despite the large size of
PKD1
.
Based on these results, three kinds of experiments were conducted to evaluate the biological function of
PKD1
in UCB-MSC. The
PKD1
protein is exposed to the outside of the cell membrane and has the function of cell proliferation due to this characteristic. Therefore, in order to confirm whether
PKD1
induces a cell proliferation function in UCB-MSC, the cells transfected with a
PKD1-
overexpressing vector were cultured in a time-dependent manner. As shown in the results of
A, cell proliferation of
PKD1
-expressing UCB-MSC was decreased compared with the UCB-MSC only group. Unexpectedly,
PKD1
was found to be not helpful for cell proliferation in stem cells, unlike in cancer cells. As aforementioned,
PKD1
controls or regulates the cell proliferation and migration of cells via mTOR and JAK signals. At this point, we think additional experiments with signal pathways are needed as to why
PKD1
does not induce the increased proliferation of stem cells.
It is known that
PKD
affects anti-oxidative effects in cancer for cell survival. This means that
PKD1 improves cell viability by making tissues resistant to changes in the surrounding environment for cancer growth [19][20][21][22]. Therefore, we assessed whether these
improves cell viability by making tissues resistant to changes in the surrounding environment for cancer growth [19,20,21,22]. Therefore, we assessed whether these
PKD1
functions also appear to have resistance in stem cells against oxidative stress. To induce oxidative cellular damage, H
2
O
2
was treated, and the survival rate of cells was measured. The result in this experiment indicates that
PKD1
did not have resistance to oxidative stress in UCB-MSC (
B), just as
PKD1
does not affect cell viability and proliferation in UCB-MSC.
Another function of
PKD is well known to improve cell mobility [24][25]. To address this function in UCB-MSC, migration analysis was performed to evaluate the migration effect of
is well known to improve cell mobility [27,28]. To address this function in UCB-MSC, migration analysis was performed to evaluate the migration effect of
PKD1
. As a result, the open area at 12 h in
PKD1
expressing UCB-MSC was significantly reduced compared to UCB-MSC only (
), meaning that
PKD1
regulates stem cell migration.
These results mean that the introduction of these extrinsic substances, which improve the ability of stem cells to move, will facilitate the movement of stem cells to damaged areas and enhance their therapeutic effectiveness. Marco Tatullo et al. reported research results supporting this fact [26]. In this study, they used human platelet lysate (PL) in dental pulp stem cells containing autologous growth factors, instead of FBS. As a result, the PL-added stem cells showed the improved osteogenic, chondrogenic differentiation and migration ability.
These results mean that the introduction of these extrinsic substances, which improve the ability of stem cells to move, will facilitate the movement of stem cells to damaged areas and enhance their therapeutic effectiveness. Marco Tatullo et al. reported research results supporting this fact [29]. In this study, they used human platelet lysate (PL) in dental pulp stem cells containing autologous growth factors, instead of FBS. As a result, the PL-added stem cells showed the improved osteogenic, chondrogenic differentiation and migration ability.
Similar to these results, we believe that
PKD1
, which induced expression, will be a useful substance to enhance the function of stem cells. If
PKD1 positively affects the homing effect, which is one of the biggest characteristics of stem cells, it will have potential as a cell therapy for tissue damage with slow cell turnover and low regenerative capacity [27].
positively affects the homing effect, which is one of the biggest characteristics of stem cells, it will have potential as a cell therapy for tissue damage with slow cell turnover and low regenerative capacity [30].
In this point of view, we focused on the differentiation of stem cells. One of the many advantages of stem cells for clinical application is their potential ability to differentiate into cells of various tissues. Thus, we tried to examine whether
PKD1 can function in the stemness and differentiation ability of UCB-MSC [28]. First, we evaluated the expression level of three kinds of stemness biomarkers, such as Oct4, Nanog, and Sox2. As it is known, Oct4 is essential for the self-renewal of stem cells, and Oct4 is controlled by SOX2. A decrease in Sox2 accompanies an increase in Oct4 and eventually promotes mesenchymal differentiation. In addition, Nanog is often known to be highly expressed in cancer stem cells, and it eventually functions as oncogenes but increases self-renewal ability in stem cells. As shown in the result of
can function in the stemness and differentiation ability of UCB-MSC [23]. First, we evaluated the expression level of three kinds of stemness biomarkers, such as Oct4, Nanog, and Sox2. As it is known, Oct4 is essential for the self-renewal of stem cells, and Oct4 is controlled by SOX2. A decrease in Sox2 accompanies an increase in Oct4 and eventually promotes mesenchymal differentiation. In addition, Nanog is often known to be highly expressed in cancer stem cells, and it eventually functions as oncogenes but increases self-renewal ability in stem cells. As shown in the result of
A, when the expression of
PKD1
was increased, the expression of stemness markers was significantly increased. It is an important point that the expression of stemness markers is increased. Increasing and regulating the expression of stemness indicators in mesenchymal stem cells using the
PKD1
gene can prolong the lifespan of cells and inhibit aging, and increase cell growth and viability to grow cells so that cells can be cultured at a large scale. This means that there is a possibility to overcome the shortcomings of mesenchymal stem cells and that it has potential for clinical cell therapy and regenerative medicine as well. This result means that
PKD1
can influence differentiation ability by the increased expression of stemness markers in UCB-MSC.
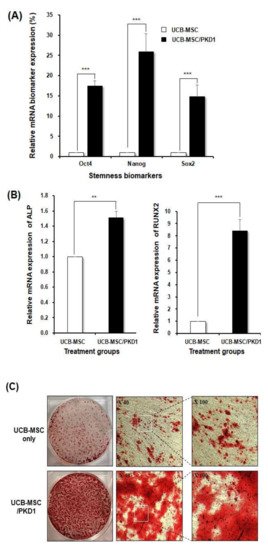
Figure 5. The expression of the increased stemness biomarkers and improved osteogenic differentiation ability of
So, next, we assessed whether the increased expression of potential stemness biomarkers by
PKD1-expressing UCB-MSC. To evaluate the potential of stem cells by
substantially improves the osteogenic differentiation ability of stem cells because UCB-MSC can differentiate into various tissues such as chondrocytes and adipocytes. We induced differentiation into osteocytes [14,31,32]. After transfection, the cells were cultured in an osteocyte differentiation medium for 12 days. At the 12th day, the cells of each group were analyzed by RT-PCR and alizarin red S staining. As a result, when
PKD1 transfection, the expression of stemness markers Oct4, Nanog, and Sox2 was detected by RT-PCR, and the differentiation ability of UCB-MSC was examined by alizarine red S staining to confirm the induction level of osteogenic differentiation: (A) The expression level of stemness biomarkers and (B) the expression level of osteogenic differentiation biomarkers induced by PKD1 in UCB-MSC; (C) The degree of the differentiation into osteocyte in PKD1-expressing UCB-MSC via alizarin red S staining. Data shown represent the mean ± SD (n = 3). ** p < 0.02, *** p < 0.01, for UCB-MSC only group versus UCB-MSC/PKD1 group.
So, next, we assessed whether the increased expression of potential stemness biomarkers by PKD1 substantially improves the osteogenic differentiation ability of stem cells because UCB-MSC can differentiate into various tissues such as chondrocytes and adipocytes. We induced differentiation into osteocytes [14][29][30]. After transfection, the cells were cultured in an osteocyte differentiation medium for 12 days. At the 12th day, the cells of each group were analyzed by RT-PCR and alizarin red S staining. As a result, when PKD1 was expressed, representative osteocyte biomarkers Runx2 and ALP were significantly expressed. In addition, as shown in
was expressed, representative osteocyte biomarkers Runx2 and ALP were significantly expressed. In addition, as shown in
C, the visual results using alizarin red S staining solution to evaluate the differentiation potency of
PKD1
demonstrated that
PKD1
can improve the osteogenic differentiation ability of stem cells, leading to an increase in the therapeutic efficacy as cell therapeutics.
To further refine this biological function of
PKD1
in stem cells, we evaluated the differentiation performance of the stem cells expressing
PKD1 by using 3D cell culture and the 3D printing technique. The three-dimension cell culture system is a culture method that artificially creates an environment similar to the shape of cells in the body by reproducing the realistic intracellular microenvironment. When cells are cultured in a 3D environment, the behavior and physiological characteristics of cells show more effectiveness in in vivo culture than in vitro culture. In addition, since cell–cell interaction becomes active and affects cell behavior and intracellular organs, the proliferation, migration, and differentiation of stem cells can be promoted, and 3D cell tissue induces cell aggregation and allows long-term culture [31][32][33][34][35].
by using 3D cell culture and the 3D printing technique. The three-dimension cell culture system is a culture method that artificially creates an environment similar to the shape of cells in the body by reproducing the realistic intracellular microenvironment. When cells are cultured in a 3D environment, the behavior and physiological characteristics of cells show more effectiveness in in vivo culture than in vitro culture. In addition, since cell–cell interaction becomes active and affects cell behavior and intracellular organs, the proliferation, migration, and differentiation of stem cells can be promoted, and 3D cell tissue induces cell aggregation and allows long-term culture [33,34,35,36,37].
To substantially verify the ability for the differentiation induction of
PKD1, 3D printing technology was used to make an artificial tooth mimetic 3D model applied with a 3D hydrogel cell culture system. The sodium alginate hydrogel used in this experiment is a natural material and has excellent biocompatibility, and when mixed with cells, it can deliver nutrients and oxygen to the inner part of the cells to increase the survival rate of cells [28][36][37].
, 3D printing technology was used to make an artificial tooth mimetic 3D model applied with a 3D hydrogel cell culture system. The sodium alginate hydrogel used in this experiment is a natural material and has excellent biocompatibility, and when mixed with cells, it can deliver nutrients and oxygen to the inner part of the cells to increase the survival rate of cells [23,25,38].
As shown in the result of
, UCB-MSCs expressing
PKD1
in a tooth mimetic 3D model showed significant differentiation ability through alizarin red S stain and osteogenic marker expression in the transcriptome. In addition, when comparing the RNA expression levels of ALP and Runx2 in 2D cell culture and 3D cell culture, it can be seen that the expression of Runx2 is higher than that of ALP in a 2D cell culture (
B and
Figure 6D), and ALP expression was higher in a 3D cell culture system. In the process of osteogenic differentiation of UCB-MSC, Runx2, a major transcription factor related to osteoblast differentiation, is first expressed, undergoes the osteoprogenitor process, and then other enzymes including ALP that promote bone formation are involved [38][39][40]. Therefore, the increased ALP expression level of stem cells cultured in a 3D cell culture environment compared with that of UCB-MSC only means that the differentiation is induced faster when
D), and ALP expression was higher in a 3D cell culture system. In the process of osteogenic differentiation of UCB-MSC, Runx2, a major transcription factor related to osteoblast differentiation, is first expressed, undergoes the osteoprogenitor process, and then other enzymes including ALP that promote bone formation are involved [39,40,41]. Therefore, the increased ALP expression level of stem cells cultured in a 3D cell culture environment compared with that of UCB-MSC only means that the differentiation is induced faster when
PKD1
is expressed.
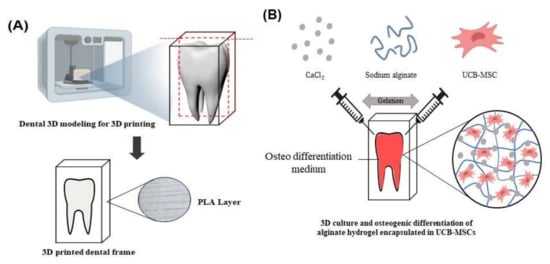
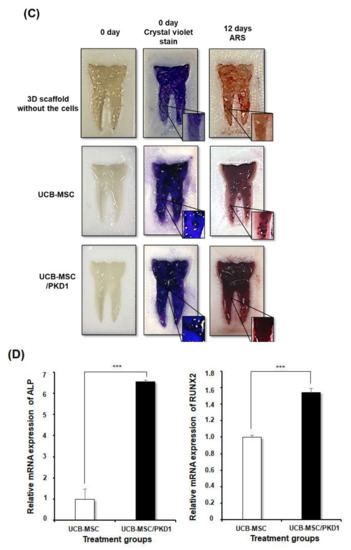
The implication of this study is that stem cells expressing
PKD1 in a tooth mimetic 3D model by 3D cell culture and 3D printing. (A) The fabrication of artificial tooth model by 3D printer technique. (B) Tooth mimetic 3D model scheme with alginate hydrogel encapsulated with UCB-MSC/have applicable potential for clinical autologous dental treatment that can replace artificial teeth. When a tooth is lost, various side effects are caused by methods to treat this, and the treatment is limited. However, introducing a stem cell-based mimetic tooth cell therapy method as an alternative for this can reduce its side effects. The results of the osteogenic differentiation of stem cells into effective by
PKD1 in a 3D tooth template for inducing osteogenic differentiation. (C) The images of cell viability and the differentiation levels by crystal violet and alizarin red S staining. (D) The mRNA expression levels of osteogenic differentiation markers of UCB-MSC expressing PKD1 in artificial tooth mimetic 3D model. Data shown represent the mean ± SD (n = 3). *** p < 0.01 for the UCB-MSC only group versus the UCB-MSC/PKD1 group.in our tooth-mimicking 3D model have a future clinically applicable source, and this suggests the possibility of regenerative medicine clinical application using stem cells.
The implication of this study is that stem cells expressing
In the end, the
PKD1 have applicable potential for clinical autologous dental treatment that can replace artificial teeth. When a tooth is lost, various side effects are caused by methods to treat this, and the treatment is limited. However, introducing a stem cell-based mimetic tooth cell therapy method as an alternative for this can reduce its side effects. The results of the osteogenic differentiation of stem cells into effective by PKD1 in our tooth-mimicking 3D model have a future clinically applicable source, and this suggests the possibility of regenerative medicine clinical application using stem cells.
In the end, the PKD1 gene showed the potential to act as a useful genetic material to overcome the shortcomings of stem cells by strengthening the function in the stem cells.
gene showed the potential to act as a useful genetic material to overcome the shortcomings of stem cells by strengthening the function in the stem cells.
