Inflammatory bowel disease (IBD) is a chronic inflammation of the gastrointestinal tract (GIT), including Crohn’s disease (CD) and ulcerative colitis (UC), which differ in the location and lesion extensions. Both diseases are associated with microbiota dysbiosis, with a reduced population of butyrate-producing species, abnormal inflammatory response, and micronutrient deficiency (e.g., vitamin D hypovitaminosis). Vitamin D (VitD) is involved in immune cell differentiation, gut microbiota modulation, gene transcription, and barrier integrity. Vitamin D receptor (VDR) regulates the biological actions of the active VitD (1α,25-dihydroxyvitamin D3), and is involved in the genetic, environmental, immune, and microbial aspects of IBD. VitD deficiency is correlated with disease activity and its administration targeting a concentration of 30 ng/mL may have the potential to reduce disease activity. Moreover, VDR regulates functions of T cells and Paneth cells and modulates release of antimicrobial peptides in gut microbiota-host interactions. Meanwhile, beneficial microbial metabolites, e.g., butyrate, upregulate the VDR signaling.
- Autophagy
- antimicrobial peptides (AMP)
- Crohn’s disease
- Dysbiosis
- vitamin D receptor
- inflammation
- Paneth cells
- nuclear receptor
- ulcerative colitis
- Probiotics
- nutrients
1. Introduction
Inflammatory bowel disease (IBD) is defined as a chronic inflammation of the gastrointestinal tract (GIT) that affects more than six million people worldwide[1][2]. The most common types are Crohn’s disease (CD) and ulcerative colitis (UC) [1]. CD is a segmental, asymmetrical, and transmural inflammation that may affect the whole GIT, but is more frequently observed in the ileum and colon. UC is related to mucosal inflammation from the rectum to the proximal colon[1][3][4]. In fact, IBD has a great impact on the physical, psychological, and social aspects of life, and depression and anxiety are usually increased in these patients. Thus, the management of IBD is of utmost importance for the quality of life of the patients[2].
Several factors are associated with the risk of IBD development, such as country development degree, smoking, sex, age, use of antibiotics or oral contraceptives, lower serum levels of vitamin D, and diet[2][5]. IBD may be triggered by an abnormal immune response to gut commensal bacteria in genetically predisposed individuals and is associated with an impaired intestinal barrier function and a less diverse gut microbiota composition[6][7][8].
The gut microbiota is comprised of more than 2000 metagenomic species (MGS) of bacteria distributed throughout the GIT[9]. The population density increases from the stomach to the colon, reaching 10
10
12 CFU (colony forming units)/mL at the end of the large intestine. Innumerous functions are attributed to the gut microbiota, like metabolism of nutrients from the diet, fiber fermentation, SCFA (short-chain fatty acids) production, vitamin production, barrier function and tight junctions regulation, antimicrobial compounds secretion, immune regulatory, among others [9][10]. Microbial metabolites released by the gut microbiota circulate and may affect the proper function of other organs and systems of the body. Therefore, strategies that address the gut microbiota modulation, improvement of the gut barrier function, and decrease in the intestinal mucosa inflammation are of the greatest significance for IBD treatment [11][12].
Micronutrient deficiencies are often observed in IBD patients, and mostly low levels of vitamin D and zinc, even during disease remission[13]. Observational studies have reported that low levels of vitamin D are directly associated with increased disease activity, mucosal inflammation, clinical relapse, and quality of life. Thus, vitamin D deficiency might be both, the cause, and a consequence of IBD[13][14]. In fact, chronic diarrhea, nutrients malabsorption, low exposure to sunlight, and reduced consumption of vitamin D-fortified foods, like dairy products, are frequent in IBD patients, which may lead to vitamin D deficiency[15].
2. Vitamin D Critical Role in IBD
2. Vitamin D Critical Role in IBD
2.1. Mechanisms of Action of Vitamin D
3
2
2D (1,25-dihydroxyvitamin D), the active form of the vitamin[16] (
Figure 1).
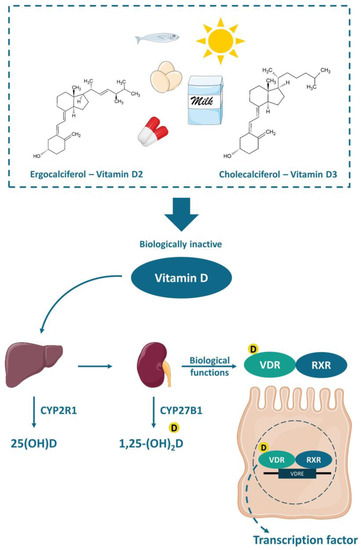
Figure 12.
2
2D forms a heterodimer with the retinoic acid receptor (RXR), which in turn attaches to the vitamin D-response element (VDRE) acting as a nuclear transcription regulator.
The functions of calcitriol in the body are mediated by the nuclear receptor VDR. VDR is expressed in various tissues (e.g., skin, parathyroid gland, adipocyte, small intestines, and colon). The VDR bounded to 1,25-(OH)
2D forms a heterodimer with the retinoic acid receptor (RXR), which migrates to the cell nucleus and binds to the vitamin D-response element (VDRE) in the promoter regions of target genes, acting as a nuclear transcription regulator[16][17][18](Figure 1). The VDRE is found in many genes, explaining the mechanisms associated with vitamin D, like autophagy[19], cell proliferation [20], intestinal barrier function [21][22], gut microbiota modulation[19][23][24], and immune functions[25][26], besides the most well-known mechanism, regarding calcium homeostasis and bone health [17][18][23].
2
2
2D harms regulatory T-cells (Tregs) differentiation and weakens its functions, which may trigger autoimmune diseases[27][28][29].
There is no consensus about the ideal circulating level of vitamin D. According to the Institute of Medicine (IOM), for the majority of the population, a minimum 25(OH)D serum level of 20 ng/mL (50 nmol/L) is considered enough, in case of a minimum sun exposure. Meanwhile, the risk of vitamin D deficiency is considered when the 25(OH)D serum level is below 12 ng/mL (30 nmol/L)[30]. Nevertheless, the Clinical Practice Guideline from the Endocrine Society defined vitamin D deficiency as serum level of 25(OH)D below 20 ng/mL (50 nmol/L) and values between 21–29 ng/mL (525–725 nmol/L) are considered as vitamin D insufficiency[31]. These thresholds of vitamin D serum levels were established for bone health. However, it is known that vitamin D deficiency may also be related to certain types of cancer, cardiovascular diseases and hypertension, type 2 diabetes and metabolic syndrome, autoimmune diseases (e.g., type 1 diabetes, rheumatoid arthritis, IBD, CD, systemic lupus erythematosus, and multiple sclerosis), and infectious diseases (e.g., tuberculosis and upper respiratory infections), autism, depression, and others[16][29][30][31]. A recent review has summarized 130 studies and demonstrated an inverse association between vitamin D and the development of several autoimmune diseases, such as CD, UC, SLE, thyrotoxicosis, type 1 diabetes, iridocyclitis, psoriasis vulgaris, seropositive RA, polymyalgia rheumatic, and MS. These studies support that vitamin D plays an important role on different aspects of the immune system. Furthermore, it is important to point out that the exposure to sunlight is the most effective natural source of vitamin D. However, people usually avoid sunlight exposure or use sunscreen due to skin cancer risk and it is difficult to reach the minimum required through the diet, thus supplementation is often necessary [16][30][31].
2.2. Implications of Vitamin D Deficiency in Inflammatory Bowel Diseases
Vitamin D deficiency in IBD patients has widely been discussed in numerous studies. It is common for patients with IBD to self-impose dietary restrictions, which is generally associated with insufficient macro and micronutrients in the diet[32]. One study compared patients with inactive or average CD with healthy controls. An inadequate nutrient intake due to the exclusion of food groups, such as milk, vegetables, and grains in CD group was observed[33]. More than a third of the individuals with IBD had BMI (body mass index) above 25, showing malnutrition accompanied by obesity, which may be due to physical inactivity or treatment with corticosteroids. The main micronutrient deficiencies observed in patients with IBD are zinc, iron, vitamin B12, and vitamin D, contributing to a critical condition and influencing on well-being[34][35].
p
p
p
p = 0.0004, I2 = 0%)]. Meanwhile, low vitamin D levels were associated with increased mucosal inflammation and low quality of life scores only in CD patients. In fact, mucosal inflammation may lead to malabsorption of vitamin D in CD, thus low levels of vitamin D could be considered as an inflammation biomarker for CD. Accordingly, MacMaster et al. observed that around 30% of 93 IBD patients in remission presented vitamin D deficiency[13]. Together, the use of standard medications may affect the absorption and use of micronutrients. Sulfasalazine, for example, is a folic acid antagonist, which may lead to anemia when used for a long period. Glucocorticoids decrease the absorption and use of calcium, zinc, and phosphorus and impair vitamin D metabolism[36].
According to an integrative review conducted by Rocha et al., malnutrition is associated to hospitalization of patients affected by the disease. Moreover, nutritional status may influence hospitalization in IBD, although no comparison with adequate nutritional status was evaluated[35]. Low or insufficient levels of vitamin D have already been linked to an increased need for hospitalization and surgery in IBD, when compared to normal serum levels[37][38]. This highlights the importance of maintaining levels considered as adequate for vitamin D, since its anti-inflammatory effect is very well studied, and these patients can benefit their well-being.
Supplementation of vitamin D in IBD patients is challenging due to nutrients malabsorption issues, and higher doses are often necessary to achieve the recommended circulating level (above 20 ng/mL, according to IOM). Nevertheless, it seemed to be a promising complementary treatment that may improve inflammation markers, such as high-sensitivity C-reactive protein (hs-CRP) and erythrocyte sedimentation rate (ESR), suppressing the Th1 immune response, while reduced clinical disease activity index[14][39][40][41][42][43][44][45].
Despite these challenges, Myint et al. published a guide for clinical practice, as a standard of care, aiming to achieve a concentration of 30 ng/mL of 25(OH)D in patients with IBD, using the following protocol: administration of 50,000 IU/week of ergocalciferol or 2000–4000 IU/day of cholecalciferol (2000 IU/day for 25[OH]D < 30 ng/mL or 4000 IU/day for 25[OH]D < 20 ng/mL), recheck after 8–12 weeks, and if the level of 30 ng/mL is reached, provide maintenance dose between 1000–2000 IU/day of cholecalciferol for the few next months and its discontinuation when the disease is quiescent. The authors explain that although it is not yet known whether vitamin D positively influences disease activity, if it helps, reaching the higher 25(OH)D concentration would have a positive impact, otherwise, reaching moderately high concentrations of 25(OH)D would not be as harmful as vitamin D deficiency would be. It is noteworthy that the authors highlight the methodological limitations and heterogeneity of the observational studies available so far, in addition to the high variability of the strength of association between vitamin D levels and IBD activity, which could be influenced by factors such as genetics, disease subtype or environment, and therefore requires further investigation[15]. However, the status of VDR in IBD patients is not considered in regular treatments. If patients with IBD have genetic variations of VDR or dysfunction of VDR in its biological roles, the supplementation of vitamin D may not work as expected.
2.3. Vitamin D and Gut Microbiota Modulation
IBD is characterized by an abnormal immune response to gut commensal bacteria in genetically predisposed individuals, which presents less diverse and imbalanced gut microbiota composition, with less abundance of butyrate producer’s species [7][8][11]. As discussed earlier, vitamin D status is implicated in the severity of IBD while the supplementation seemed to improve the disease status. Nonetheless, it has been suggested that this protective effect is directly related to the gut microbiota (
Figure 2).
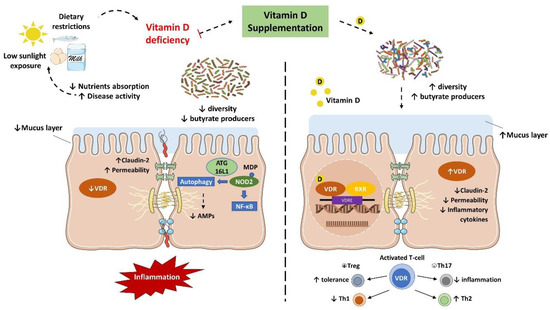
Figure 23.
Several in vivo studies have shown that vitamin D supplementation and VDR anti-inflammatory effect are directly associated with the gut microbiota. In fact, the downregulation of VDR or the inability to produce the active form of vitamin D were associated with a decrease in Lactobacillus in the gut microbiota, while Proteobacteria was increased. Meanwhile, butyrate may improve the VDR signaling, which together with the fact that prokaryotes do not express the VDR highlights that the gut microbiota plays a key role in the host intestinal immune response related to vitamin D mechanisms[46][47].
Interestingly, Du et al. reported that in inflammation conditions, the colonic VDR downregulation is associated with an increased expression of local CYP27B1, as a homeostatic protective effect to reduce inflammation and improve VDR signaling. Notably, the gut microbiota plays a critical role in this process. In fact, mice submitted to antibiotic treatment failed to upregulate the CYP27B1 while developed more severe colitis. Meanwhile, LPS treatment stimulated the upregulation of CYP27B1 as well, reinforcing the role of VDR in the barrier function and anti-inflammatory and anti-infection pathways [48].
VDR is known to negatively regulate bacterial-stimulated NF–κB activity[49], and this mechanism may also be an important contributor to intestinal homeostasis and host protection from bacterial invasion and infection. In an experimental colitis model, it was demonstrated that mice with the gut epithelium VDR deletion developed a more severe clinical colitis and worsened epithelial cell apoptosis, leading to an increased intestinal mucosa permeability[21], and promoted the Th1 and Th17 (T helper 17) mucosal response[50]. It suggests that the downregulation of the colonic VDR observed in patients with IBD may be related to impaired barrier functions in the intestine.
The VDR is also implicated in the anti-bacterial functions of Paneth cells. Lu et al. remarkably revealed that the downregulation of VDR and ATG16L1 genes were observed in small intestines tissue from CD patients, as well as a lower percentage and abnormal Paneth cells[51]. Meanwhile, mice with Paneth cells VDR knockout showed a reduction in the relative abundance of beneficial bacteria (e.g.,
Lactobacillus
Salmonella infection and DSS-induced colitis[51]. These findings confirm that Paneth cell abnormalities result in a reduced bacterial clearance ability through AMPs, and together with a reduction in autophagy responses could explain the association of dysbiosis and Paneth cell abnormalities observed in individuals with IBD.
E. coli in vitro while showed a protective effect to induced colitis in vivo[52].
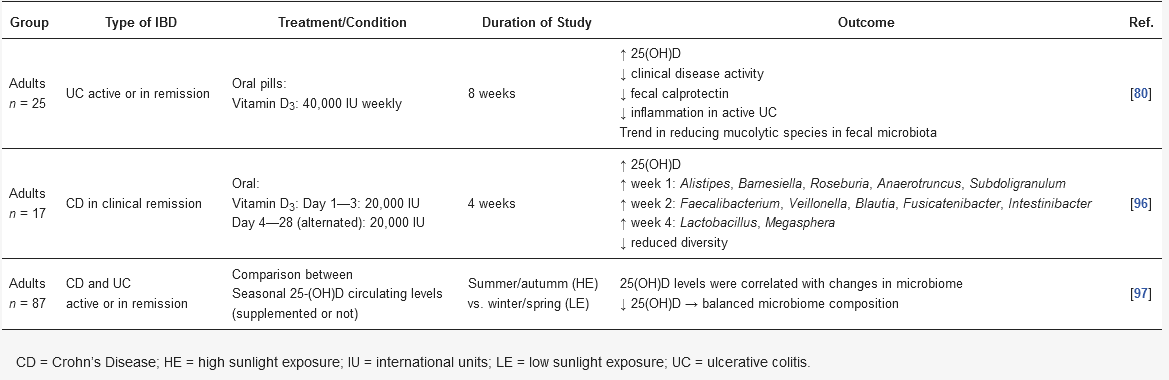
Table 1. Still, studies with healthy populations have shown promising outcomes about vitamin D and VDR functions in modulating the gut microbiota and improving the immune response[25][26][53][54].
Table 1. Summary of published human studies outcomes evaluating vitamin D3 and its modulation of microbiota in inflammatory bowel disease.
| Soy Products | Treatments (Bacterial Fermentation) | Health Benefits | References |
|---|---|---|---|
| Starter culture | |||
| Fermented soybean | Bacillus subtilis SHZ, B. subtilis MTCC 5480 | Antioxidant | [62,63] |
| Douchi qu | B. subtilis natto, B. subtilis B1 | ACE inhibitory | [64] |
| Cheonggukjang | B. licheniformis SCD 111067P | Antihypertensive, Antidiabetic | [65,66] |
| Soy Products | Treatments (Fungi Fermentation) | Health Benefits | References |
| Starter culture | |||
| Douchi qu | Aspergillus oryzae, Mucor wutungkiao | ACE inhibitory | [64] |
| Douchi | Aspergillus oryzae, Aspergillus egyptiacus | Antioxidant, Antihypertensive | [67,68] |
| Meju | Aspergillus oryzae | Antimicrobial | [69] |
| Soy Products | Heat Treatments | Effects | References |
| Soymilk | Microwave-assisted extraction | Increase protein content, viscosity, protein solubility, and digestibility | [70] |
| Raw soybean | Gamma irradiation | Increase total phenolic content, Decrease tannins and trypsin inhibitors | [71] |
| Soybeans | Infrared treatment | Inactivated both trypsin inhibitors and lipoxygenase | [72] |
Ruminococcus gnavus
E
coli
Fusobacterium nucleatum. Despite these findings, the UC group had improved inflammatory markers, such as fecal calprotectin, albumin, and platelet count, together with disease activity. Although a reduction in Enterobacteriaceae was expected, this increase does not imply a worsening in overall profile of microbiota, since this family of bacteria comprises other not harmful and commensal bacteria. These are very interesting results despite the small sample size of the study[39].
3
n
n
Alistipes
Parabacteroides
Roseburia
Faecalibacterium was observed, even though it was transient. The authors suggested that 4 weeks might have been a too short intervention period to detect a greater change. However, these results suggest that vitamin D administration has potential as an adjuvant therapy for CD patients[55]. It is noteworthy that the reduced abundance of the
Faecalibacterium genus is commonly associated with both diseases, UC and CD. Its characteristic of producing butyrate has already been shown to be a way to reduce inflammation and promote a balance between Th17 and Treg[56].
n
Pediococcus
Clostridium
Escherichia
Shigella
Eggerthella lenta
Fusobacterium
Helicobacter
Faecalibacterium prausnitzii showed lower relative abundance. Unlike other studies, low levels of vitamin D were associated with a more balanced composition of the microbiome. It should be noted that it was not a randomized controlled trial (RTC), but vitamin D levels were correlated with changes in the microbiome in individuals with IBD[57].
3 in modulating gut microbiota in human IBD. The study designs are heterogeneous together with a substantially small number of patients enrolled in human trials, resulting in inconsistent and controversial outcomes. It is difficult to state an effective dose so far. Meanwhile, it has been suggested that higher doses of vitamin D supplementation may increase the secretion of antimicrobial peptides, contributing to the gut microbiota modulation. Further human clinical trials, with appropriate intervention design, evaluating the impact of vitamin D on the gut microbiota of IBD patients are needed to better understand the mechanisms involved and support the indication of use as a complementary treatment. It is also needed to consider the influence of gender, age, ethnicity, genetics, metabolic disorders (e.g., obesity, diabetes, and NAFLD), and IBD subtype.
3. Conclusions and Future Directions
VDR is identified as the first human gene to shape the gut microbiome[23]. However, the variations of the
Vdr gene in human IBD are still unknown. In the future study, we need considering the status of VDR in the patients of IBD, in addition to the serum 25(OH) vitamin D concentration. We need well-designed therapeutic studies to examine whether enhanced vitamin D will restore functions of VDR and microbiome in inhibiting chronic inflammation, as well as to test the appropriate dose by considering the influence of gender, age, ethnicity, genetics, and metabolic disorders in the IBD subtype.
