Increased anxiety in these conditions may be linked to a high-salt diet through stimulation of the sympathetic nervous system, which increases blood pressure while releasing catecholamines, causing a “fight or flight” response. A rostral shift of fluid overload from the lower to the upper body occurs in obstructive sleep apnea associated with COVID-19 and cardiovascular disease, and may be related to sodium and fluid retention triggered by hypertonic dehydration. Chronic activation of the renin-angiotensin-aldosterone system responds to salt-induced dehydration by increasing reabsorption of sodium and fluid, potentially exacerbating fluid overload. Anxiety may also be related to angiotensin II that stimulates the sympathetic nervous system to release catecholamines.
- hypertension
- anxiety
- obstructive sleep apnea
- cardiovascular disease
- COVID-19
- dietary salt
- renin-angiotensin-aldosterone system
- sympathetic nervous system
- catecholamines
1. Introduction
2. Anxiety, CVD, and Sodium Toxicity
Diagnosis of anxiety according to criteria of the International Classification of Diseases-8 (ICD-8) was associated with an increased risk of subsequent coronary heart disease events in 49,321 Swedish men [61][9]. A 2010 meta-analysis of 20 studies found a higher incidence of coronary heart disease and cardiac mortality associated with anxiety, prompting the researchers to suggest that anxiety was an independent risk factor for cardiac morbidity and mortality [62][10]. More recently, a 2016 meta-analysis of 37 studies found that anxiety was associated with a 52% increased risk of CVD prevalence [63][11], and new onset CVD was associated with anxiousness in a 2020 study of a German population [64][12]. Nevertheless, the underlying mechanisms causatively linking anxiety with CVD are unknown. In an editorial in the Journal of the American College of Cardiology, Dimsdale [65][13] speculated that leading pathophysiological mediators in the causative pathway between anxiety and heart disease include “sympathetic nervous system activity and various inflammatory markers”. Dimsdale further noted the need to scrutinize potential underlying risk factors that are common to anxiety and CVD. The adrenal catecholamines epinephrine and norepinephrine of the sympathetic nervous system increase the “fight-or-flight” stress response, and dysregulation of this response under conditions of chronic stress can contribute to anxiety [66][14]. A high-salt diet in a model of salt-sensitive mice was found to stimulate an overactive response of the sympathetic nervous system, which was associated with increased blood pressure and increased levels of adrenal epinephrine production [67][15]. Additionally, a systematic review and meta-analysis of epidemiological studies found that hypertension is associated with anxiety [68][16]. Hypertonic saline infusion also increased activity of the sympathetic nervous system and raised plasma norepinephrine levels in normal men [69][17]. Similarly, hypertonic saline induced panic attacks in an animal model of panic disorder [70][18]. This evidence suggests an anxiogenic link with high dietary salt intake, which hypothetically may satisfy criteria for toxin exposure in substance/medication-induced anxiety disorder, listed in the Diagnostic and Statistics Manuel-5 (DSM-5) [71][19]. Furthermore, an inflammatory response induced by high salt intake in healthy humans increases interleukin-6 (IL-6) and IL-23 pro-inflammatory cytokines, while reducing anti-inflammatory cytokine IL-10 [72][20].3. OSA, Hypertension, and the Renin-Angiotensin-Aldosterone System
A nocturnal rostral shift that redistributes fluid overload from the lower body towards the head occurs in OSA [73][21], exacerbating obstruction in the upper airways and increasing blood pressure in patients with hypertension [74][22]. Secondary hyperaldosteronism, often present in OSA, occurs from excessive activation of the renin-angiotensin-aldosterone system (RAAS), which can be due to edematous disorders [75][23]. RAAS activation increases salt and fluid reabsorption in the kidneys which “is important for restoring homeostasis after dehydration”, and thirst responses to intracellular dehydration are mediated by angiotensin II type 2 receptors (AT2R) [76][24]. Importantly, infusion of hypertonic sodium chloride (hypernatremia) causes intracellular hypertonic dehydration [77][25], suggesting that excessive ingestion of sodium chloride and hypertonic dehydration could trigger RAAS activation and possibly chronic overcompensation as reabsorbed salt and fluid levels contribute to hypervolemia. Chronic RAAS activation causing tissue remodeling and dysfunction occurs in congestive heart failure, systemic hypertension, and chronic kidney disease [78][26]. Dysregulated RAAS response is also implicated in COVID-19 complications in patients with CVD [79][27]. The RAAS response related to edema and hypervolemia from high dietary salt intake could also explain excessive aldosterone levels associated with parapharyngeal edema and upper airway resistance in severe OSA [80][28]. Excessive salt consumed by 20 student volunteers in a study of OSA found that “the normal pattern of sleep was disturbed and the depth of sleep was decreased” [81][29]. A 2013 study found that OSA was prevalent in 77.3% of patients with resistant hypertension and hyperaldosteronism, and an increase in OSA severity was associated with high dietary salt intake [82][30]. The researchers hypothesized that high dietary salt intake was a causative factor in the study findings, and suggested that “interventional studies that use dietary salt restriction as a treatment strategy for OSA in patients with resistant hypertension and hyperaldosteronism are needed to test this hypothesis”. Subsequently, results of a randomized trial published in 2018 found only minor reductions in OSA severity after one week of testing the use of diuretics and reduced dietary sodium [83][31]. However, the sodium-restricted group in the study ingested a daily maximum intake of 3 g sodium, which is higher than the U.S. Dietary Reference Intake (DRI) of 2300 mg sodium advised to reduce chronic disease risk in adults, twice as high as the DRI of 1500 mg sodium considered adequate for adults [84][32], and six times higher than essential sodium requirements of 500 mg recommended by the U.S. National Heart, Lung, and Blood Institute [85][33]. Furthermore, a case–control study of sleep apnea in heart failure patients found that patients with sleep apnea had a mean daily sodium intake of 3000 mg compared to patients without sleep apnea with a mean daily sodium intake of 1900 mg [86][34]. More research is needed to test interventions with lower daily levels of sodium intake (500 mg–1500 mg) for OSA prevention.4. OSA, Anxiety, and Angiotensin II
Anxiety is associated with OSA and sleep disorders [87[35][36][37][38][39][40][41][42][43][44],88,89,90,91,92,93,94,95,96], although causative relationships are not clear and require more investigations. Additionally, sympathetic nervous system response is increased and parasympathetic response is decreased in OSA, the opposite effect of normal sleep, and increased variability of heart rate and blood pressure often extends into daytime wakefulness with normal breathing [97][45], suggesting causative factors involving the RAAS response. Angiotensin II (AngII) of the RAAS response, derived from angiotensin I through action of angiotensin-I converting enzyme, increases blood pressure and retention of sodium and fluids, but as humans adopted a salt diet, the protective effects of the RAAS response turned into “a negative factor” [98][46]. “Plasma angiotensin II is increased in humans and animals with chronic heart failure” [99][47]. Additionally, AngII is “known to facilitate catecholamine release from peripheral sympathetic neurons by enhancing depolarization-dependent exocytosis”, contributing to vasoconstriction and sodium retention [100][48]. Of relevance, elevated levels of catecholamines are present in the urine and serum of patients with OSA, including children with OSA [101,102][49][50]. This evidence suggests that increased interaction of AngII with the sympathetic nervous system and increased release of catecholamines forms a potential mechanism that mediates the association of high dietary salt with anxiety, proposed in Figure 1. More research is needed to explore this anxiogenic mechanism.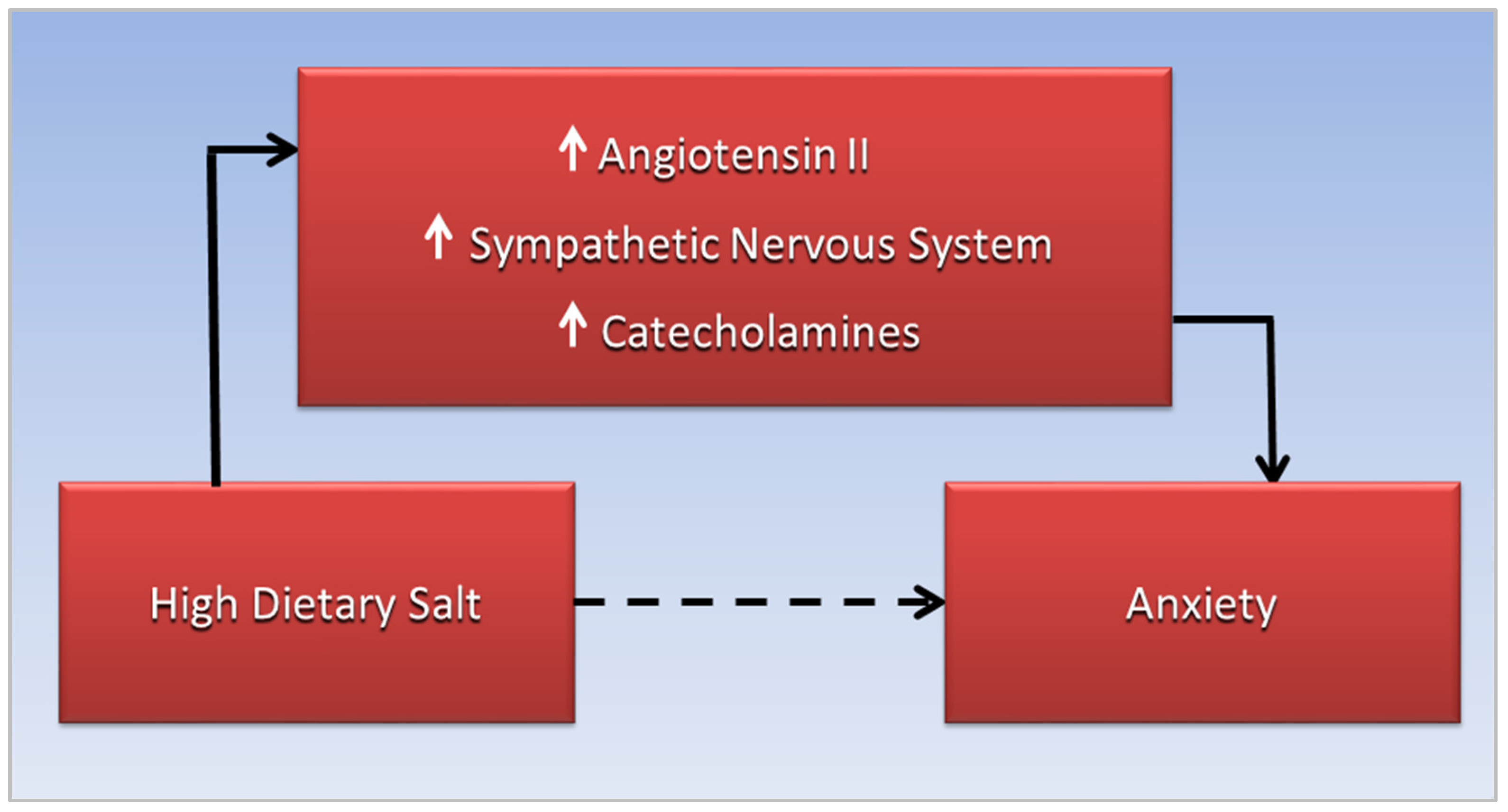
References
- Fuchs, F.D.; Whelton, P.K. High Blood Pressure and Cardiovascular Disease. Hypertension 2020, 75, 285–292.
- Wu, C.Y.; Hu, H.Y.; Chou, Y.J.; Huang, N.; Chou, Y.C.; Li, C.P. High Blood Pressure and All-Cause and Cardiovascular Disease Mortalities in Community-Dwelling Older Adults. Medicine 2015, 94, e2160.
- Hall, J.E.; Guyton, A.C.; Coleman, T.G.; Mizelle, H.L.; Woods, L.L. Regulation of arterial pressure: Role of pressure natriuresis and diuresis. Fed. Proc. 1986, 45, 2897–2903.
- Who.Int. Salt Reduction. Available online: https://www.who.int/news-room/fact-sheets/detail/salt-reduction (accessed on 30 August 2022).
- Choi, H.Y.; Park, H.C.; Ha, S.K. Salt Sensitivity and Hypertension: A Paradigm Shift from Kidney Malfunction to Vascular Endothelial Dysfunction. Electrolytes Blood Press. 2015, 13, 7–16.
- Grillo, A.; Salvi, L.; Coruzzi, P.; Salvi, P.; Parati, G. Sodium intake and hypertension. Nutrients 2019, 11, 1970.
- Rust, P.; Ekmekcioglu, C. Impact of Salt Intake on the Pathogenesis and Treatment of Hypertension. In Hypertension: From Basic Research to Clinical Practice; Islam, M.S., Ed.; Springer International Publishing: Cham, Switzerland, 2017; pp. 61–84.
- Luzardo, L.; Noboa, O.; Boggia, J. Mechanisms of Salt-Sensitive Hypertension. Curr. Hypertens. Rev. 2015, 11, 14–21.
- Janszky, I.; Ahnve, S.; Lundberg, I.; Hemmingsson, T. Early-Onset Depression, Anxiety, and Risk of Subsequent Coronary Heart Disease: 37-Year Follow-Up of 49,321 Young Swedish Men. J. Am. Coll. Cardiol. 2010, 56, 31–37.
- Roest, A.M.; Martens, E.J.; de Jonge, P.; Denollet, J. Anxiety and risk of incident coronary heart disease: A meta-analysis. J. Am. Coll. Cardiol. 2010, 56, 38–46.
- Batelaan, N.M.; Seldenrijk, A.; Bot, M.; van Balkom, A.J.; Penninx, B.W. Anxiety and new onset of cardiovascular disease: Critical review and meta-analysis. Br. J. Psychiatry 2016, 208, 223–231.
- Reiner, I.C.; Tibubos, A.N.; Werner, A.M.; Ernst, M.; Brähler, E.; Wiltink, J.; Michal, M.; Schulz, A.; Wild, P.S.; Münzel, T.; et al. The association of chronic anxiousness with cardiovascular disease and mortality in the community: Results from the Gutenberg Health Study. Sci. Rep. 2020, 10, 12436.
- Dimsdale, J.E. What does heart disease have to do with anxiety? J. Am. Coll. Cardiol. 2010, 56, 47–48.
- Goddard, A.W.; Ball, S.G.; Martinez, J.; Robinson, M.J.; Yang, C.R.; Russell, J.M.; Shekhar, A. Current perspectives of the roles of the central norepinephrine system in anxiety and depression. Depress. Anxiety 2010, 27, 339–350.
- Ralph, A.F.; Grenier, C.; Costello, H.M.; Stewart, K.; Ivy, J.R.; Dhaun, N.; Bailey, M.A. Activation of the Sympathetic Nervous System Promotes Blood Pressure Salt-Sensitivity in C57BL6/J Mice. Hypertension 2021, 77, 158–168.
- Pan, Y.; Cai, W.; Cheng, Q.; Dong, W.; An, T.; Yan, J. Association between anxiety and hypertension: A systematic review and meta-analysis of epidemiological studies. Neuropsychiatr. Dis. Treat. 2015, 11, 1121–1130.
- Peskind, E.R.; Radant, A.; Dobie, D.J.; Hughes, J.; Wilkinson, C.W.; Sikkema, C.; Veith, R.C.; Dorsa, D.M.; Raskind, M.A. Hypertonic saline infusion increases plasma norepinephrine concentrations in normal men. Psychoneuroendocrinology 1993, 18, 103–113.
- Molosh, A.I.; Johnson, P.L.; Fitz, S.D.; Dimicco, J.A.; Herman, J.P.; Shekhar, A. Changes in central sodium and not osmolarity or lactate induce panic-like responses in a model of panic disorder. Neuropsychopharmacology 2010, 35, 1333–1347.
- Arnold, E. Anxiety DSM-5 Diagnostic Criteria and Treatment Overview. Available online: https://pro.psycom.net/assessment-diagnosis-adherence/anxiety (accessed on 30 August 2022).
- Yi, B.; Titze, J.; Rykova, M.; Feuerecker, M.; Vassilieva, G.; Nichiporuk, I.; Schelling, G.; Morukov, B.; Choukèr, A. Effects of dietary salt levels on monocytic cells and immune responses in healthy human subjects: A longitudinal study. Transl. Res. 2015, 166, 103–110.
- da Silva, B.C.; Kasai, T.; Coelho, F.M.; Zatz, R.; Elias, R.M. Fluid Redistribution in Sleep Apnea: Therapeutic Implications in Edematous States. Front. Med. 2017, 4, 256.
- Bangash, A.; Wajid, F.; Poolacherla, R.; Mim, F.K.; Rutkofsky, I.H. Obstructive Sleep Apnea and Hypertension: A Review of the Relationship and Pathogenic Association. Cureus 2020, 12, e8241.
- Dominguez, A.; Muppidi, V.; Gupta, S. Hyperaldosteronism. Available online: https://www.ncbi.nlm.nih.gov/books/NBK499983/ (accessed on 1 October 2022).
- Coble, J.P.; Grobe, J.L.; Johnson, A.K.; Sigmund, C.D. Mechanisms of brain renin angiotensin system-induced drinking and blood pressure: Importance of the subfornical organ. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2015, 308, R238–R249.
- Tiarks, G. Hypertonic dehydration: What Is It, Causes, Treatment, and More. Available online: https://www.osmosis.org/answers/hypertonic-dehydration (accessed on 1 September 2022).
- Ames, M.K.; Atkins, C.E.; Pitt, B. The renin-angiotensin-aldosterone system and its suppression. J. Vet. Intern. Med. 2019, 33, 363–382.
- Augustine, R.; Abhilash, S.; Nayeem, A.; Salam, S.A.; Augustine, P.; Dan, P.; Maureira, P.; Mraiche, F.; Gentile, C.; Hansbro, P.M.; et al. Increased complications of COVID-19 in people with cardiovascular disease: Role of the renin–angiotensin-aldosterone system (RAAS) dysregulation. Chem. Biol. Interact. 2022, 351, 109738.
- Dudenbostel, T.; Calhoun, D.A. Resistant hypertension, obstructive sleep apnoea and aldosterone. J. Hum. Hypertens. 2012, 26, 281–287.
- Fereidoun, H.; Pouria, H. Effect of excessive salt consumption on night’s sleep. Pak J. physiol. 2014, 10, 6–9.
- Pimenta, E.; Stowasser, M.; Gordon, R.D.; Harding, S.M.; Batlouni, M.; Zhang, B.; Oparil, S.; Calhoun, D.A. Increased dietary sodium is related to severity of obstructive sleep apnea in patients with resistant hypertension and hyperaldosteronism. Chest 2013, 143, 978–983.
- Fiori, C.Z.; Martinez, D.; Montanari, C.C.; Lopez, P.; Camargo, R.; Sezerá, L.; Gonçalves, S.C.; Fuchs, F.D. Diuretic or sodium-restricted diet for obstructive sleep apnea—A randomized trial. Sleep 2018, 41, zsy016.
- National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Food and Nutrition Board; Committee to Review the Dietary Reference Intakes for Sodium and Potassium. The National Academies Collection: Reports funded by National Institutes of Health. In Dietary Reference Intakes for Sodium and Potassium; Oria, M., Harrison, M., Stallings, V.A., Eds.; National Academies Press (US): Washington, DC, USA, 2019.
- NHLBI. Implementing Recommendations for Dietary Salt Reduction: Where Are We? Where Are We Going? How Do We Get There?: A Summary of an NHLBI Workshop; National Institutes of Health, National Heart, Lung, and Blood Institute: Bethesda, MD, USA, 1996.
- Kasai, T.; Arcand, J.; Allard, J.P.; Mak, S.; Azevedo, E.R.; Newton, G.E.; Bradley, T.D. Relationship between sodium intake and sleep apnea in patients with heart failure. J. Am. Coll. Cardiol. 2011, 58, 1970–1974.
- Kim, J.Y.; Ko, I.; Kim, D.K. Association of Obstructive Sleep Apnea With the Risk of Affective Disorders. JAMA Otolaryngol. –Head Neck Surg. 2019, 145, 1020–1026.
- Rezaeitalab, F.; Moharrari, F.; Saberi, S.; Asadpour, H.; Rezaeetalab, F. The correlation of anxiety and depression with obstructive sleep apnea syndrome. J. Res. Med. Sci. 2014, 19, 205–210.
- Cox, R.C.; Olatunji, B.O. Sleep in the anxiety-related disorders: A meta-analysis of subjective and objective research. Sleep Med. Rev. 2020, 51, 101282.
- Akberzie, W.; Hesselbacher, S.; Aiyer, I.; Surani, S.; Surani, Z.S. The Prevalence of Anxiety and Depression Symptoms in Obstructive Sleep Apnea. Cureus 2020, 12, e11203.
- Duan, X.; Zheng, M.; Zhao, W.; Huang, J.; Lao, L.; Li, H.; Lu, J.; Chen, W.; Liu, X.; Deng, H. Associations of Depression, Anxiety, and Life Events With the Risk of Obstructive Sleep Apnea Evaluated by Berlin Questionnaire. Front. Med. 2022, 9, 799792.
- Daabis, R.; Gharraf, H. Predictors of anxiety and depression in patients with obstructive sleep apnea. Egypt. J. Chest Dis. Tuberc. 2012, 61, 171–177.
- Garbarino, S.; Bardwell, W.A.; Guglielmi, O.; Chiorri, C.; Bonanni, E.; Magnavita, N. Association of Anxiety and Depression in Obstructive Sleep Apnea Patients: A Systematic Review and Meta-Analysis. Behav. Sleep Med. 2020, 18, 35–57.
- Batzikosta, A.; Antoniadou, M.; Tiga, P.; Nena, E.; Xanthoudaki, M.; Voulgaris, A.; Sotiropoulou, R.; Kouratzi, M.; Froudarakis, M.; Steiropoulos, P. AB011. Assessment of anxiety and depressive symptoms in obstructive sleep apnea patients. Ann. Transl. Med. 2016, 4, 11.
- Wong, J.L.; Martinez, F.; Aguila, A.P.; Pal, A.; Aysola, R.S.; Henderson, L.A.; Macey, P.M. Stress in obstructive sleep apnea. Sci. Rep. 2021, 11, 12631.
- Sharafkhaneh, A.; Giray, N.; Richardson, P.; Young, T.; Hirshkowitz, M. Association of psychiatric disorders and sleep apnea in a large cohort. Sleep 2005, 28, 1405–1411.
- Mansukhani, M.P.; Kara, T.; Caples, S.M.; Somers, V.K. Chemoreflexes, sleep apnea, and sympathetic dysregulation. Curr. Hypertens. Rep. 2014, 16, 476.
- Benigni, A.; Cassis, P.; Remuzzi, G. Angiotensin II revisited: New roles in inflammation, immunology and aging. EMBO Mol. Med. 2010, 2, 247–257.
- Wang, Y.; Seto, S.W.; Golledge, J. Angiotensin II, sympathetic nerve activity and chronic heart failure. Heart Fail. Rev. 2014, 19, 187–198.
- Dendorfer, A.; Thornagel, A.; Raasch, W.; Grisk, O.; Tempel, K.; Dominiak, P. Angiotensin II induces catecholamine release by direct ganglionic excitation. Hypertension 2002, 40, 348–354.
- Hakim, F.; Gozal, D.; Kheirandish-Gozal, L. Sympathetic and catecholaminergic alterations in sleep apnea with particular emphasis on children. Front. Neurol. 2012, 3, 7.
- Sica, E.; De Bernardi, F.; Nosetti, L.; Martini, S.; Cosentino, M.; Castelnuovo, P.; Marino, F. Catecholamines and children obstructive sleep apnea: A systematic review. Sleep Med. 2021, 87, 227–232.
