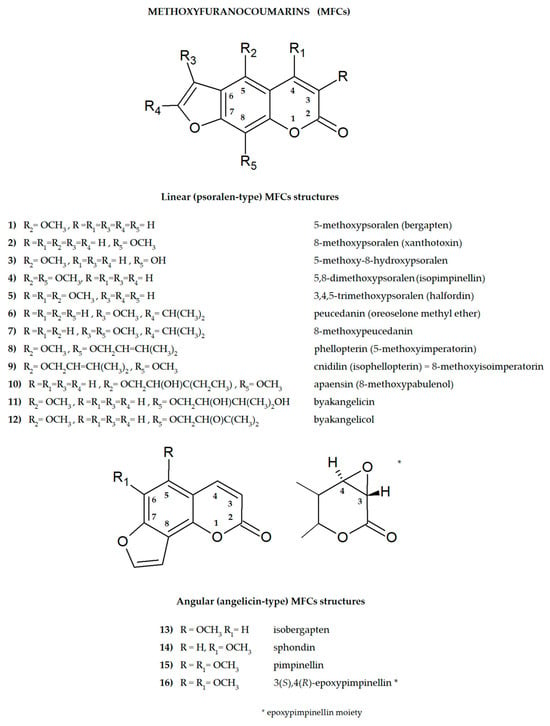
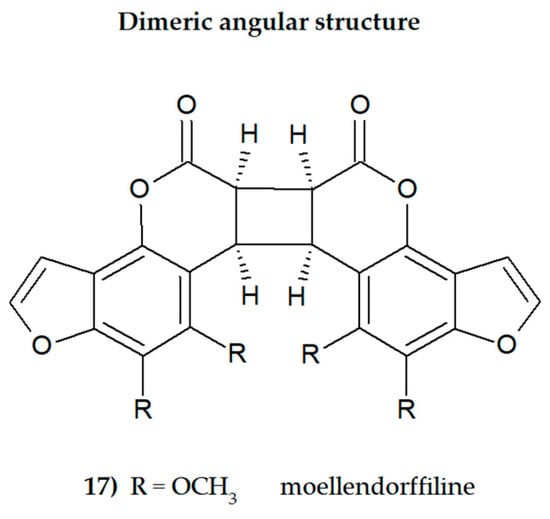
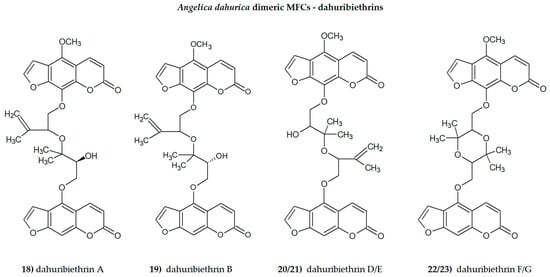
Plant secondary metabolites, including furanocoumarins, have attracted attention for decades as active molecules with therapeutic potential, especially those occurring in a limited number of species as evolutionarily specific and chemotaxonomically important. The most famous methoxyfuranocoumarins (MFCs), bergapten, xanthotoxin, isopimpinellin, phellopterin, byakangelicol, byakangelicin, isobergapten, pimpinellin, sphondin, as well as rare ones such as peucedanin and 8-methoxypeucedanin, apaensin, cnidilin, moellendorffiline and dahuribiethrins, have been investigated for their various biological activities.
- methoxyfuranocoumarins (MFCs)
- biological activity
- secondary metabolites
- plant drugs
1. Introduction
2. General Aspects of MFC Studies
2.1. Studies of the Active Substituents in the MFC Structure
When attached to the benzene ring at the para position, a methoxyl group is classified, according to Hammett’s equation (developed in 1935), as electron-donating, but at the meta position it is classified as an electron-withdrawing group (in the ortho position, steric effects may cause the same trend as that of the para position) [19]. Hammett’s equation covers chemical reactivity, spectroscopy, and other physical properties, and even the biological activity of the drugs; however, it has some limitations. As an example, for meta- and para-substituted aromatic compounds, inconsistency may be expected whenever the opportunity arises for strong electron delocalization between the substituent and the reaction sites [22]. In their recent work, Türker [23] discussed the MFC isomers with a single methoxy substituent attached to the psoralen backbone in various positions. This work, based on the density functional treatment (DFT), brings an interesting insight into the interactions of the methoxy groups (substituted at C-3, -4, -5, -6, -7, or -8 position) with heterocyclic oxygen, and with the carbonyl group in the tested molecules. The positional variations of the methoxy substituent in psoralen backbone result in electronically stable as well as thermally favourable isomers in all the studied cases. They all have exothermic heat of formation values, and the rings are found highly aromatic (especially isomers substituted at C-8 and C-5 positions on the benzoic ring) [23]. It is found that the heteroatoms in the rings have different extents of opposing and assisting effects on the net electron flow effect from the methoxy group. In the considered structures, lactone moiety acts as an electron-attracting, whereas the methoxy group acts as the electron-donating one, and the lactone carbonyl moiety embedded in the psoralen backbone attracts electrons mesomerically [23]. Hydroxylation of coumarin (attaching the -OH group to the carbon atom of the coumarin molecule) increases its solubility in water. In the human body, this mechanism facilitates the conjugation of the resulting hydroxyl derivative with glucuronide or sulfate metabolites and then its excretion from the body [24]. The double bond between C-3 and C-4 of the furanocoumarin molecule (as in the case of 3(S),4(R)-epoxypimpinelin—Figure 1) can be epoxidized. The epoxidized form of coumarin is unstable in the cellular environment and is therefore usually quickly eliminated/detoxified. It is also suspected that it may cause hepatotoxicity by itself or through its subsequent metabolites [25]. Prenylation is the conjugation reaction of the isoprenoid chain with various molecules, especially proteins. Prenyl groups have been shown to be important for protein–protein binding through a specialized prenyl-binding domain that may be important for enzymatic activity. There are also several groups of prenylated polyphenolic compounds in plants, including flavonoids, phloroglucinols, xanthones and coumarins [26]. Prenyl (3-methylbut-2-en-1-yl) moiety occurs in the structures of many MFCs and can be found as the simple 3-methylbut-2-en-1-yl unit, but is often found in the form of the corresponding epoxide or in an oxidized form. The prenyl group brings to the MFC structure the ability to interact with various molecules, especially with the active sites of enzymes, and offers these compounds new bioactive potential. The previously discussed effects influence the biological activity of MFCs at a molecular level. It would be interesting to investigate the relationship between different MFC substituents and interactions within molecules containing methoxy (more than one) and prenyl functional groups, as well as both groups simultaneously. Such studies aimed at determining interactions within more complex MFC molecules could provide additional information useful for assessing their biological potential.2.2. Structure–Activity Relationships of the Studied MFCs—A Short Summary
Some general observations regarding the structure–activity relationship of the analyzed MFCs could be concluded. The particular position of the methoxyl group and the count of these may influence the biological activity of linear MFCs. It was especially found when MFCs such as xanthotoxin, bergapten, and isopimpinellin as agonists of the bitter taste receptors were studied [89], where the specificity of the receptor target was also related to the position of the methoxy group in the furanocoumarin scaffold. The C-8 methoxy group was important for antiseizure activity of xanthotoxin, and bergapten with the C-5 methoxy group showed no protective properties [27]. In the case of α-glucosidase inhibitory activity [28] and antibacterial activity of MFCs [14], it was also important whether the molecule was in a linear or in an angular shape. Angular structures were more active (pimpinellin vs. isopimpinellin) and dimers were more active than monomers (moellendorffiline vs. pimpinellin).
The isopenthenyl group on the furanocoumarin skeleton increase their lipophilicity and the possibility of passage of the molecule through the bacterial membrane to its target site. Phellopterin possesses this group at the C-5 position. Double oxygenated substituents at C-5 and C-8 are necessary for antibacterial activity of linear furanocoumarins, such as in the case of isopimpinellin and phellopterin [29]. The latter one has a prenyl group, which increases lipophilicity, and therefore phellopterin was more active against bacterial strains than isopimpinellin [30]. Similar behavior was observed in the case of the adjuvant properties of byakangelicin, which increase the content of the co-ingested drugs in the brain by enhancing their penetration due to they own lipophilicity [31].
The presence of methoxy groups at C-8 and C-5 in the structure of furanocoumarin and the angular type of this structure are also beneficial for antifungal activity [32]. The analysis of the influence of methoxyl groups on the inhibition of AChE activity by angular MFCs indicated that pimpinellin (with two methoxy groups at C-5 and C-6 positions) exerted three-fold higher activity on AChE inhibition than isobergapten with one methoxy group at the C-5 position [33]. Pimpinellin was significantly (two-fold) more active compared to bergapten in the BChE inhibitory assay [34].
The furan ring fused at the C-6 and C-7 positions of the coumarin scaffold is necessary, and also the 5-methoxy group contributes greatly to reducing histamine release; however, the isopentane-derived groups in the molecule likely reduce histamine release as well [35]. Moellendorffiline (dimer of pimpinellin) exerts higher antioxidant activity compared to the monomeric compound, pimpinellin [28].
Inhibition of GABA-transaminase has been proposed as a possible mechanism for the antiepileptic effects of active MFCs. Analysis of the behavior of byakangelicin, byakangelicol and phellopterin (all these compounds have aliphatic chains at the C-8 position and are not active against GABA-transaminase) and in silico study showed that the three unblocked oxygen atoms in the MFC structure are necessary for the interaction of compounds with the enzyme pocket of GABA-transaminase. Therefore, if the compounds are to be active, the C-8 position cannot present an aliphatic chain [27].
All these observations are important, but many of them require additional, in-depth research, and this knowledge may be important when designing drugs based on MFC. It seems particularly interesting to examine the interaction of various substituents (methoxy, hydroxyl, isopropyl and prenyl groups) in the molecule, the position and number of which can modify activity. It should be taken into account that the impact of substituents may also depend on the selected research model and various factors, including physicochemical ones, and in the case of multi-component drugs, on the impact of co-existing molecules. All of this together makes this aspect even more difficult to explore, but it can also be an exciting challenge.
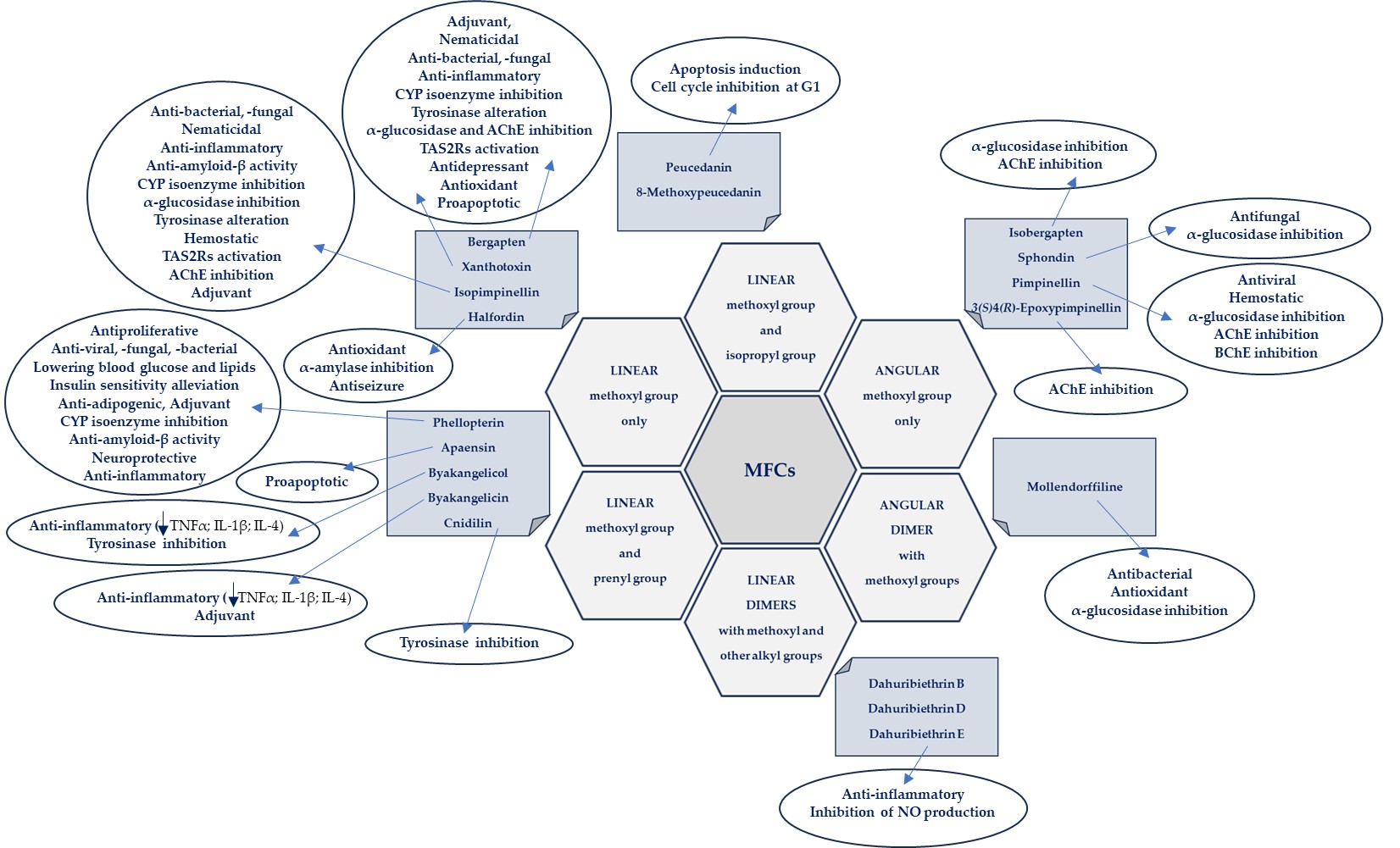
The biological activities of MFCs discussed in this text in relation to the structural type and substituents in the furanocoumarin molecule are briefly presented in Figure 4.
2.3. Bioavaiability Studies of MFCs
Bioavailability is related to the speed and the quantity of a drug appearing in the blood after a given dose, and many bioavailability studies involve determining the concentration of the ingested/injected active substance in blood or urine [5]. An important factor influencing the bioavailability and distribution of MFCs in the body is hydrophobicity, expressed in logP values (octanol/water partition coefficient). MFCs are mostly lipophilic and therefore have limited water solubility, which reduces their biological potential. On the other hand, as lipophilic substances, MFC diffuse well into the cell [36]. There are few studies concerning bioavailability of MFCs available, and there is still need to profoundly study the behavior of these molecules in the biological fluids of the body and membrane permeability investigations. The results of experiments exploring Parallel Artificial Membrane Permeability (PAMPA) models to predict transcellular passive absorption of MFC (bergapten and xanthotoxin) were recently published [37][38]. Using a hexadecane membrane, Petit et al. [37] studied the passive intestinal absorption of crude plant extracts of various compositions, including the extract of Angelica archangelica containing furanocoumarins. A. angelica MFCs have a high potential to easily cross the gastrointestinal barrier via the transcellular route, and it was found that the presence of multicomponent mixtures does not affect the passive permeability of these compounds as single components [37]. In another study, Li and co-investigators [38] found that the absorption of monocomponents (bergapten and isopimpinellin were analyzed) is related to their physicochemical properties (e.g., logP values); however, the chemical compatibility of the mixture components may change the absorption of co-existing compounds. Also, in the case of other MFCs, the use of the PAMPA model may provide new information on the absorption of these compounds into the bloodstream.2.4. Distribution and Metabolism of MFCs
Zhao and co-workers [39] studied the pharmacokinetics of coumarins (5-hydroxy-8-methoxypsoralen, bergapten, xanthotoxin, isopimpinellin, neobyakangelicol, byakangelicin and phellopterin) occurring in a lyophilized ethanol extract (70%) from Angelicae dahuricae radix (ADR; single dose 6.0 g/kg) in the plasma of male Sprague–Dawley (SD) rats after oral administration. It was found that the coexistence of ADR drug components can significantly alter the pharmacokinetic behavior of a single compound, improving its bioavailability and extending its time in systemic circulation. Due to the similar chemical composition and structure, when taking a mixture of compounds, a pharmacokinetic phenomenon was observed, leading to the creation of enterohepatic circulation in order to maintain the effective concentration of the substance in the plasma and leading to long-term pharmacological effectiveness [39]. The following pharmacokinetic parameters were calculated: Tmax—maximum concentration, T1/2—elimination half-lives, and AUC (Area Under the Curve), a crucial measure of the bioavailability of a drug after administration. After oral administration of ADR, all of the tested coumarins were absorbed from rat gastrointestinal tract and detected (LC–MS/MS) at 5 min in plasma. Tmax values of phellopterin, xanthotoxin, byakangelicin, and bergapten, were 1.7, 2.0 h, 2.3 h, and 2.4 h, respectively. 5-Hydroxy-8-methoxypsoralen, byakangelicin, bergapten, and phellopterin showed steeper slopes at the last time points of the concentration-time curves, which may indicate non-linear pharmacokinetics of these compounds due to, among others, the saturation of components in the system [39]. Liao et al. [40] analyzed xanthotoxin, isopimpinellin, and bergapten (from Cnidium monnieri fruit extract) in male SD rat plasma. Additionally, 24 metabolites of bergapten (13 in vitro and 23 in vivo) were detected, including 15 phase I metabolites and 9 phase II metabolites. It was found that oxidation and glucuronide conjugation might be the main methabolic pathways of MFCs. However, monooxidation, dioxidation and oxirolysis were the major metabolic pathways of bergapten in rat liver microsomes. The main biotransformation pathways in vivo were hydrolysis, hydrogenation and glucuronide conjugation. The pharmacokinetics study of MFCs was profoundly investigated. All of the compounds were absorbed rapidly and had similar elimination rates. However, isopimpinellin, with C-5 and C-8 methoxy groups, was eliminated slower than bergapten (C-5) and xanthotoxin (C-8). T1/2 values for isopimpinellin, bergapten, and xanthotoxin were 5.69, 4.21, and 3.40 h, respectively, and Tmax values for compounds were 3.0 h, 3.0 h, and 2.0 h, respectively. Analyzed MFCs were detected by the UHPLC-Q-TOF-MS method [40]. The distribution of MFCs (bergapten, xanthotoxin, isopimpinellin, byakangelicin, phellopterin, 2″R–neobyakangelicol, isobyakangelicol) in male SD rats after oral administration of ADR (75% ethanol) was studied by Zhang et al. [41]. The MFCs were distributed widely and rapidly, and they could be detected in all of the selected tissues. However, the concentrations of coumarins were obviously higher in kidney, liver, and stomach and lower in testis, brain, and muscle tissues. The stomach, liver, and kidney might be the main target organs of phellopterin and byakangelicin because in these organs the concentrations of these MFCs were obviously higher than in other tissues. The concentration of 2″R–neobyakangelicol was high in stomach and kidney, which suggested that these are the main target organs of this MFC. On the other hand, in other selected tissues, especially in testis tissue, distribution was relatively low. The concentrations of xanthotoxin in stomach and kidney were obviously higher than those in other tissues, and the next was heart, from which the elimination of xanthotoxin was slow. The high concentration of isopimpinellin and isobyakangelicol in stomach prompted the hypothesis that stomach might be the main target organ of the two compounds. It was concluded that the rapid distribution of byakangelicin compared to phellopterin could be associated with hydroxyl groups in the byakangelicin structure, and therefore higher water solubility, which increased in in vivo fluids [41]. Quantitative analysis of the compounds was performed using use ultra-performance liquid chromatographic–tandem mass spectrometry (UHPLC-MS/MS). Qiu and co-investigators [42] analyzed (HPLC-MS/MS) the amount of MFCs (isopimpinellin, pimpinellin and bergapten) after oral administration of Toddalia asiatica L. (Rutaceae) root extract (5.2 mL/kg, which was equal to 10.73 mg/kg isopimpinellin; 39.50 mg/kg pimpinellin; 9.73 mg/kg bergapten;) in plasma, urine, and feces of male SD rats. All of these MFCs were rapidly absorbed from the gastrointestinal tract. It was found that the amounts of the pimpinellin, isopimpinellin and bergapten excreted from urine and feces were extraordinarily limited (<0.5%), indicating that the four analytes were principally excreted in the form of bile or as metabolites. Tmax was 0.33 h for isopimpinellin and pimpinellin, and 0.50 h for bergapten; T1/2 were 1.43 h; 0.91 h and 0.77 h, respectively. The Cmax ratios and doses of pimpinellin, isopimpinellin, and bergapten were 1004, 201.6, and 107.6 ng/L, respectively [42].2.5. Gut Metabolism of MFCs by Human Microbiota
The human body is inhabited by a huge number of commensal microorganisms, which include bacteria, viruses, and fungi. The vast majority of them colonize the gastrointestinal tract (GIT) [43]. Intestinal microflora (the so-called microbiome) plays an important role in various mechanisms occurring in the human body, such as the maturation and development of the immune system, the central nervous system, the GIT system, and is also responsible for basic metabolic pathways. These microbiome/host interactions are an area of research that is constantly evolving and cannot be underestimated [44]. The study of biotransformation by human intestinal bacteria is essential to evaluate the effects of the bioactive compounds present in foods and in natural medicines, and it is of great interest due to the confirmed altered biological activity of metabolites [45]. In the recently conducted study, furanocoumarins (bergapten, xanthotoxin and byakangelicol, among others) isolated form A. dahurica roots were metabolized by a human fecal sample and each MFC was transformed by Blautia sp. (MRG-PMF1), bacterium responsible for intestinal O-demethylation (as confirmed previously in the study of gut metabolism of polymethoxyflavones) [46]. The gut microbial conversion of xanthotoxin and bergapten with MRG-PMF1 strain resulted in formation of xanthotoxol and bergaptol due to the methyl aryl ether cleavage by bacterial O-methyltransferase. As the result of the biotransformation of byakangelicol, which underwent O-demethylation and hydration, three metabolites were detected: new metabolite–desmethylbyakangelicol, byakangelicin and finally desmethylbyakangelicin (as confirmed by HPLC-DAD-MS). As was found for the first time, prenylated furanocoumarins such as imperatorin and isoimperatorin were transformed by MRG-PMF1 to deprenylated compounds, finally producing xanthotoxol and bergaptol [45]. Previously, it was known that prenyl groups in plant-derived polyphenols can undergo only hepatic I phase metabolism (with Cyt P-450 enzymes). Xanthotoxol can be more readily removed from the body with urine excretion due to its increased solubility, which is considered as a detoxification mechanism. As was confirmed in the described study, the human intestinal bacterium Blautia sp. MRG-PMF1 can metabolize MFCs isolated from A. dahurica roots [45]. Biotransformation studies of other MFCs by human microbiome could be beneficial for better understanding the biotransformation pathways of these compounds in the human body, and it is an area of study which is worth to be explored extensively.3. Toxicity and Safety Studies
As consumption of natural medicines continues to increase, attention should be paid to the potential risks associated with ingested bioactive compounds [92,93]. When developing new therapeutic strategies, including those related to natural medicines, safety of use (including toxicology) and assessment of side effects are an extremely important part of the related procedures. It has been demonstrated that toxicity induced by herbal medicines may result from the biotransformation of their components into electrophilic, reactive metabolites that can covalently bind to important macromolecules in the body. The complicated relationship between the active ingredients of natural drugs, their detoxification mechanisms and potential risks was highlighted in a recently published review article of Wen and Gorycki [47]. Furanocoumarins were also mentioned, metabolized to reactive toxic forms such as epoxides, cis-2-enedialdehyde, γ-ketoenal, and detoxified, the bioactivation of which may lead to the inactivation of drug metabolizing enzymes (including CYP isoenzymes); it clinically manifests itself through interactions and side effects when taking plant ingredients and synthetic drugs.
Bioactivation of the components of herbal extracts and the associated toxicity are largery governed by the complex composition of the said extracts [48], so understanding the complexity of natural medicines is of great importance [93]. As was underlined by Kharaman and co-investigators [48], the toxicity of a single compound can be reduced by interactions with accessory molecules present simultaneously in natural medicines. The different biological activities of these reactive metabolites can be viewed as a function of their reactivity, selectivity, concentration, and exposure time, as well as the pro-oxidant/antioxidant balance in cells [47].
A new approach to assessing the risk associated with the consumption of drugs and herbal preparations was proposed by Wang et al. [49] on the example of multi-component preparations of A. dahurica containing MFCs. It is worth undertaking and constantly developing this important aspect of the safety of natural medicines and functional foods [50][51].
4. New Approaches for Evaluation of MFC Activity
To enhance bioavailability of MFCs, nanoformulations of coumarins were examined to explore the anticancer potential of these compounds [52]. It is known that the basis of nanoformulation studies is divided into two main categories: nanocarriers (nanoparticles) and guest molecules. These may have influence on the solubility and biocompatibility of guest molecules. Microemulsions (thermodynamically stable isotropic systems with small particles < 100 nm) of xanthotoxin and chitosan-derivative-coated xanthotoxin were tried and found to be an effective way for drug delivery into the skin in dermal carcinomas [53]. New suitable animal models, such as zebrafish (Danio rerio), are currently being investigated, especially to evaluate the activity of MFCs in central nervous system (CNS) disorders, focusing on anticonvulsant and antiseizure effects [21]. Unfortunately, three-dimensional (3D) cell models/organoids for assessing the bioactivity of MFCs are still not available, and it should be emphasized that this may be a new approach worth trying, as the test model seems to be similar to in vivo tests. Three-dimensional organoids and organs on a chip are rapidly evolving, and these techniques have been widely characterized [54][55]. For example, three-dimensional (3D) in vitro models of the human brain, such as organoids, bioprinted three-dimensional models of brain tissues or functionalized organoids, may be important in the study of both stages of development and pathological changes within this organ [56], taking into account specific aspects such as anatomy, interactions at the cellular level and gene expression. These new models may provide a useful tool for investigating human-specific phenomena that cannot be studied in animal models. This may be important when designing new drugs, including those of natural origin. Such 3D cellular models can be produced from tissues taken from the patient, which provides a personalized approach to explaining disease mechanisms and developing treatment methods [55]. An interesting aspect of the research is the assessment of the activity of MFCs as agonists of human taste receptors, especially the T2R family, which are found not only in the oral cavity but also throughout the body, as, for example, in the GIT, the respiratory tract, the immune system and in the central nervous system. It has been found that these receptors are multi-targeted at the molecular level and for various compounds interacting with them, which may be related to their promising therapeutic potential [57]. Some MFCs, especially xanthotoxin, have been found to be effective molecules binding to T2R and exerting biological activity [58]. This, and many more (Figure 5) aspect of MFC activity deserves special consideration in planned future studies.
Figure 5. Future directions and prospects in the research of methoxyfuranocoumarins (MFCs).
References
- Limones-Mendez, M.; Dugrand-Judek, A.; Villard, C.; Coqueret, V.; Froelicher, Y.; Bourgaud, F.; Olry, A.; Hehn, A. Convergent evolution leading to the appearance of furanocoumarins in citrus plants. Plant Sci. 2020, 292, 110392.
- Fernandes, H.P.; Salome-Abarca, L.F.; Goncalves Pereira, R.; Brandao Seibert, J.; Jose-Silva Junior, G.; Das Gracas Fernandes da Silva, M.F.; Choi, J.H. Metabolomic investigation of Citrus latifolia and the putative role of coumarins in resistance to black spot disease. Front. Mol. Biosci. 2022, 9, 934401.
- Zhu, J.J.; Jiang, J.G. Pharmacological and Nutritional Effects of Natural Coumarins and Their Structure-Activity Relationships. Mol. Nutr. Food Res. 2018, 62, e1701073.
- Ahmed, S.; Khan, H.; Aschner, M.; Mirzae, H.; Küpeli Akkol, E.; Capasso, R. Anticancer Potential of Furanocoumarins: Mechanistic and Therapeutic Aspects. Int. J. Mol. Sci. 2020, 21, 5622.
- Sharifi-Rad, J.; Cruz-Martins, N.; López-Jornet, P.; Pons-Fuster Lopez, E.; Nidaa Harun, N.; Yeskaliyeva, B.; Beyatli, A.; Sytar, O.; Shaheen, S.; Sharopov, F.; et al. Natural Coumarins: Exploring the Pharmacological Complexity and Underlying Molecular Mechanisms. Oxid. Med. Cell. Longev. 2021, 2021, 6492346.
- Liang, Y.; Xie, L.; Liu, K.; Cao, Y.; Dai, X.; Wang, X.; Lu, J.; Zhang, X.; Li, X. Bergapten: A review of its pharmacology, pharmacokinetics, and toxicity. Phytother. Res. 2021, 35, 6131–6147.
- Wu, A.; Lu, J.; Zhong, G.; Lu, L.; Qu, Y.; Zhang, C. Xanthotoxin (8-methoxypsoralen): A review of its chemistry, pharmacology, pharmacokinetics, and toxicity. Phytother. Res. 2022, 36, 3805–3832.
- Flores-Morales, V.; Villasana-Ruíz, A.P.; Garza-Veloz, I.; González-Delgado, S.; Martinez-Fierro, M.L. Therapeutic Effects of Coumarins with Different Substitution Patterns. Molecules 2023, 28, 2413.
- Murray, R.D.H.; Mendez, J.; Brown, S.A. The Natural Coumarins: Occurrence, Chemistry and Biochemistry; Willey: Chichester, UK, 1982; p. 702.
- Brown, S.A. Biosynthesis of furanocoumarins in parsnips. Phytochemistry 1970, 9, 2471–2475.
- Stanjek, V.; Piel, J.; Boland, W. Biosynthesis of furanocoumarins: Mevalonate-independent prenylation of umbelliferone in Apium graveolens (Apiaceae). Phytochemistry 1999, 50, 1141–1146.
- Villard, C.; Munakata, R.; Kitajima, S.; Velzen, R.; Schranz, E.M.; Larbat, R.; Hehn, A. A new P450 involved in the furanocoumarin pathway underlies a recent case of convergent evolution. New Phytol. 2021, 231, 1923–1939.
- Yang, W.-Q.; Song, Y.-L.; Zhu, Z.-X.; Su, C.; Zhang, X.; Wang, J.; Shi, S.-P.; Tu, P.-F. Anti-inflammatory dimeric furanocoumarins from the roots of Angelica dahurica. Fitoterapia 2015, 105, 187–193.
- Dehghan, H.; Rezaee, P.; Aliahmadi, A. Bioassay screening of 12 Iranian plants and detection of antibacterial compounds from Heracleum persicum using a TLC bioautography method. J. Liquid Chrom. Rel. Technol. 2020, 43, 381–387.
- Lin, S.R.; Chang, C.H.; Tsai, M.J.; Cheng, H.; Chen, J.C.; Leong, M.K.; Weng, C.F. The perceptions of natural compounds against dipeptidyl peptidase 4 in diabetes: From in silico to in vivo. Ther. Adv. Chronic Dis. 2019, 10, 2040622319875305.
- Bartnik, M.; Sławińska-Brych, A.; Żurek, A.; Kandefer-Szerszeń, M.; Zdzisińska, B. 8-methoxypsoralen reduces AKT phosphorylation, induces intrinsic and extrinsic apoptotic pathways, and suppresses cell growth of SK-N-AS neuroblastoma and SW620 metastatic colon cancer cells. J. Ethnopharmacol. 2017, 207, 19–29.
- Bartnik, M.; Sławińska-Brych, A.; Mizerska-Kowalska, M.; Zdzisińska, B. Evaluation of the Biological Effect of Non-UV-Activated Bergapten on Selected Human Tumor Cells and the Insight into the Molecular Mechanism of Its Action. Int. J. Mol. Sci. 2023, 24, 15555.
- Lin, S.R.; Chang, C.H.; Hsu, C.F.; Tsai, M.J.; Cheng, H.; Leong, M.K.; Sung, P.J.; Chen, J.C.; Weng, C.F. Natural compounds as potential adjuvants to cancer therapy: Preclinical evidence. Br. J. Pharmacol. 2020, 177, 1409–1423.
- Madeiro, S.A.L.; Borges, N.H.P.B.; Souto, A.L.; de Figueiredo, P.T.R.; Siqueira-Junior, J.P.; Tavares, J.F. Modulation of the antibiotic activity against multidrug resistant strains of coumarins isolated from Rutaceae species. Microb. Pathog. 2017, 104, 151–154.
- Skalicka-Woźniak, K.; Orhan, I.E.; Cordell, G.A.; Nabavi, S.M.; Budzyńska, B. Implication of Coumarins towards Central Nervous System Disorders. Pharmacol. Res. 2016, 103, 188–203.
- Skiba, A.; Kozioł, E.; Luca, S.V.; Budzyńska, B.; Podlasz, P.; Van Der Ent, W.; Shojaeinia, E.; Esguerra, C.V.; Nour, M.; Marcourt, L.; et al. Evaluation of the Antiseizure Activity of Endemic Plant Halfordia kendack Guillaumin and Its Main Constituent, Halfordin, on a Zebrafish Pentylenetetrazole (PTZ)-Induced Seizure Model. Int. J. Mol. Sci. 2023, 24, 2598.
- John, D.R.; Marjorie, C.C. Basic Principles of Organic Chemistry, 2nd ed.; W. A. Benjamin, Inc.: Menlo Park, CA, USA, 1977; ISBN 0-8053-8329-8. Available online: https://chem.libretexts.org/Bookshelves/Organic_Chemistry/Basic_Principles_of_Organic_Chemistry_(Roberts_and_Caserio)/26%3A_More_on_Aromatic_Compounds/26.06%3A_Correlations_of_Structure_with_Reactivity_of_Aromatic_Compounds (accessed on 24 November 2023).
- Türker, L. Monomethoxyisomers of psoralen—DFT treatment. Earthline J. Chem. Sci. 2022, 8, 175–192.
- Lake, B.G. Coumarin metabolism, toxicity, and carcinogenicity: Relevance for human risk assessment. Food Chem. Toxicol. 1999, 37, 423–453.
- Born, S.; Rodriquez, P.; Eddy, C.; Lehman-McKeeman, L. Synthesis and reactivity of coumarin 3,4-epoxide. Drug Metab. Dispos. 1997, 25, 1318–1323.
- Karamat, F.; Olry, A.; Munakata, R.; Koeduka, T.; Sugiyama, A.; Paris, C.; Hehn, A.; Bourgaud, F.; Yazaki, K. A coumarin-specific prenyltransferase catalyzes the crucial biosynthetic reaction for furanocoumarin formation in parsley. Plant J. 2014, 77, 627–638.
- Kozioł, E.; Jóźwiak, K.; Budzyńska, B.; de Witte, P.A.M.; Copmans, D.; Skalicka-Woźniak, K. Comparative Antiseizure Analysis of Diverse Natural Coumarin Derivatives in Zebrafish. Int. J. Mol. Sci. 2021, 22, 11420.
- Dehghan, H.; Sarrafi, Y.; Salehi, P.; Ebrahimi, S.N. α-Glucosidase inhibitory and antioxidant activity of furanocoumarins from Heracleum persicum. Med. Chem. Res. 2017, 26, 849–855.
- Walasek, M.; Grzegorczyk, A.; Malm, A.; Skalicka-Woźniak, K. Bioactivity-guided isolation of antimicrobial coumarins from Heracleum mantegazzianum Sommier & Levier (Apiaceae) fruits by high-performance counter-current chromatography. Food Chem. 2015, 186, 133–138.
- Zuo, G.-Y.; Wang, C.-J.; Han, J.; Li, Y.-Q.; Wang, G.-C. Synergism of coumarins from Chinese drug Zanthoxylum nitidum with antibacterial agents against methicillin-resistent Staphylococcus aureus (MRSA). Phytomedicine 2016, 23, 1814–1820.
- Kang, Y.Y.; Song, J.; Kim, J.Y.; Jung, H.; Yeo, W.-S.; Lim, Y.; Mok, H. Byakangelicin as a modulator for improved distribution and bioactivity of natural compounds and synthetic drugs in the brain. Phytomed 2019, 62, 152963.
- He, Y.-H.; Shang, X.-F.; Li, H.-X.; Li, A.-P.; Tang, C.; Zhang, B.-Q.; Zhang, Z.-J.; Wang, R.; Ma, Y.; Du, S.-S.; et al. Antifungal activity and action mechanism study of coumarins from Cnidium monnieri fruit and structurally related compounds. Chem. Biodiv. 2021, 18, e2100633.
- Lee, S.J.; Depoortere, I.; Hatt, H. Therapeutic potential of ectopic olfactory and taste receptors. Nat. Rev. Drug Discov. 2019, 18, 116–138.
- Karakaya, S.; Koca, M.; Yılmaz, S.V.; Yıldırım, K.; Pınar, N.M.; Demirci, B.; Brestic, M.; Sytar, O. Molecular Docking Studies of Coumarins Isolated from Extracts and Essential Oils of Zosima absinthifolia Link as Potential Inhibitors for Alzheimer’s Disease. Molecules 2019, 24, 722.
- Li, D.; Wu, L. Coumarins from the roots of Angelica dahurica cause anti-allergic inflammation. Exper. Ther. Med. 2017, 14, 874–880.
- Kulikov, O.A.; Ageev, V.P.; Brodovskaya, E.P.; Shlyapkina, V.I.S.; Petrov, P.S.; Zharkov, M.N.; Yakobson, D.E.; Maev, I.V.; Sukhorukov, G.B.; Pyataev, A.N. Evaluation of photocytotoxicity liposomal form of furanocoumarins Sosnowsky’s hogweed. Chem.-Biol. Interact. 2022, 357, 109880.
- Petit, C.; Bujard, A.; Skalicka-Woźniak, K.; Cretton, S.; Houriet, J.; Christen, P.; Carrupt, P.-A.; Wolfender, J.-L. Prediction of the passive intestinal absorption of medicinal plant extract constituents with the parallel artificial membrane permeability assay (PAMPA). Planta Med. 2016, 82, 424–431.
- Li, H.; Zeng, H.; He, D.; Wang, M.; Liu, L.; Liang, W.; Shu, Y.; Zhao, S.; Sun, G.; Lv, C.; et al. A new approach to examining the extracton process of Zhishi and Zhiqiao considering the synergistic effect of complex mixtures by PAMPA. J. Chrom. B 2018, 1099, 10–17.
- Zhao, A.-H.; Zhang, Y.-B.; Yang, X.-W. Simultaneous determination, and pharmacokinetics of sixteen Angelicae dahurica coumarins in vivo by LC–ESI-MS/MS following oral delivery in rats. Phytomedicine 2016, 23, 1029–1036.
- Liao, M.; Song, G.; Cheng, X.; Diao, X.; Sun, Y.; Zhang, L. Simultaneous determination of six coumarins in rat plasma and metabolites identification of bergapten in vitro and in vivo. J. Agric. Food Chem. 2018, 66, 4602–4613.
- Zhang, Y.B.; Deng, G.G.; Wang, T.X.; Liu, L.; Yang, X.W. Tissue distribution study of Angelica dahurica cv. Yubaizhi in rat by ultra-performance liquid chromatography with tandem mass spectrometry. J. Pharm. Biomed. Anal. 2019, 174, 43–49.
- Qiu, J.; Zhu, M.; Wang, Y.; Chen, B.; Bai, R.; Chen, F.; Li, Y.; Zhou, Y.; Zhang, L. Pharmacokinetic and excretion study of eight active constituents in rat by LC-MS/MS after oral administration of the Toddalia asiatica extract. Anal. Biochem. 2022, 640, 114407.
- Sorboni, S.G.; Moghaddam, H.S.; Jafarzadeh-Esfehani, R.; Soleimanpour, S. A Comprehensive Review on the Role of the Gut Microbiome in Human Neurological Disorders. Clin. Microbiol. Rev. 2022, 35, e0033820.
- Afzaal, M.; Saeed, F.; Shah, Y.A.; Hussain, M.; Rabail, R.; Socol, C.T.; Hassoun, A.; Pateiro, M.; Lorenzo, J.M.; Rusu, A.V.; et al. Human gut microbiota in health and disease: Unveiling the relationship. Front. Microbiol. 2022, 13, 999001.
- Susanto Tan, S.R.; Eser, B.E.; Han, J. Gut metabolism of furanocoumarins: Proposed function of Co O-methyltransferase. ACS Omega 2020, 5, 30696–30703.
- Kim, M.; Kim, N.; Han, J. Metabolism od Kaempferia parviflora polymethoxyflavones by human intestinal bacterium, Blautia sp. MRG-PMF1. J. Agric. Food. Chem. 2014, 62, 12377–12383.
- Wen, B.; Gorycki, P. Bioactivation of herbal constituents: Mechanisms and toxicological relevance. Drug Metab. Rev. 2019, 51, 453–497.
- Kahraman, C.; Ceren Arituluk, Z.; Irem Tatli Cankaya, I. The Clinical Importance of Herb-Drug Interactions and Toxicological Risks of Plants and Herbal Products. In Medical Toxicology; IntechOpen: London, UK, 2021.
- Wang, Z.; Zan, K.; Hu, X.-W.; Kang, S.; Li, H.-L.; Zuo, T.-T.; Jin, H.-Y.; Ma, S.-C. The Simultaneous Determination of Nine Furocoumarins in Angelica dahurica Using UPLC Combined with the QAMS Approach and Novel Health Risk Assessment Based on the Toxic Equivalency Factor. Separations 2023, 10, 508.
- Yordi, E.G.; Matos, M.J.; Martinez, A.P.; Tornes, A.C.; Santana, L.; Molina, E.; Uriarte, E. In silico genotoxicity of coumarins: Application of the Phenol-Explorer food database to functional food science. Food Funct. 2017, 8, 2958–2966.
- Zhang, Y.; Li, Z.; Wei, J.; Kong, L.; Song, M.; Zhang, Y.; Xiao, X.; Cao, H.; Jin, Y. Network pharmacology and molecular docking reveal the mechanism of Angelica dahurica against Osteosarcoma. Medicine 2022, 101, e31055.
- Yerer, M.B.; Dayan, S.; Han, M.I.; Sharma, A.; Tuli, H.S.; Sak, K. Nanoformulations of coumarins and the hybrid molecules of coumarins with potential anticancer effects. Anticancer Agents Med. Chem. 2020, 20, 1797–1816.
- Wu, J.Y.; Li, Y.J.; Liu, T.T.; Ou, G.; Hu, X.B.; Tang, T.T.; Wang, J.M.; Liu, X.Y.; Xiang, D.X. Microemulsions vs chitosan derivative-coated microemulsions for dermal delivery of 8-methoxypsoralen. Int. J. Nanomed. 2019, 14, 2327–2340.
- Del Dosso, A.; Urenda, J.; Nguyen, T.; Quadrato, G. Upgrading the Physiological Relevance of Human Brain Organoids. Neuron 2020, 107, 1014–1028.
- D’Antoni, C.; Mautone, L.; Sanchini, C.; Tondo, L.; Grassmann, G.; Cidonio, G.; Bezzi, P.; Cordella, F.; Di Angelantonio, S. Unlocking Neural Function with 3D In Vitro Models: A Technical Review of Self-Assembled, Guided, and Bioprinted Brain Organoids and Their Applications in the Study of Neurodevelopmental and Neurodegenerative Disorders. Int. J. Mol. Sci. 2023, 24, 10762.
- Steimberg, N.; Chiono, V.; Era, P.D.; Di Angelantonio, S. iPS, Organoids and 3D Models as Advanced Tools for In Vitro Toxicology. ALTEX Altern. Anim. Exp. 2020, 37, 136–140.
- Ki, S.Y.; Jeong, Y.T. Taste Receptors beyond Taste Buds. Int. J. Mol. Sci. 2022, 23, 9677.
- Qin, C.; Yuan, Q.; Han, H.; Chen, C.; Wu, J.; Wei, X.; Liu, M.; Zhang, H.; Ping, J.; Xu, L.; et al. Biomimetic integrated gustatory and olfactory sensing array based on HL-1 cardiomyocyte facilitating drug screening for tachycardia treatment. Biosens. Bioelectr. 2023, 223, 115034.
