
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Muhammad Arif Mahmood | + 2220 word(s) | 2220 | 2021-09-28 08:33:59 | | | |
| 2 | Amina Yu | Meta information modification | 2220 | 2021-09-29 03:07:40 | | |
Video Upload Options
3D printing is gaining traction in the manufacturing industry, with the benefits of improving productivity and lowering both the cost and number of human-based faults. Given its enormous flexibility and capacity to modify and construct a range of simple to complicated geometries, 3D printing has altered production rates with process automation. 3D printing is swiftly transforming pharmaceutical production to achieve elevated quality therapeutic products with improved process sturdiness in bio-pharmaceutical product evolution, where there is a dependence on medicines manufacturing via conventional manufacturing procedures.
1. Significance of Personalized Medicines (PM)
The drug market has recently observed a profound revolution and development in patient therapy that delivers effective and harmless medications. Personalized medicine (PM) has seen renowned growth. It can offer maximum protection boundaries, which lessen the after-effects and guarantees improved patient safety [1][2]. PM seeks to provide a unique opportunity that attempts to change patient biology through medication preferences, dosages and treatments. Its goals are to provide improved health care facilities, simplify research, and discover diagnostics and remedies [3][4]. In 1997, to treat breast cancer, Herceptin was rejected in Phase-III patient trials as the medicine was found futile for all inhabitants. Still, after careful review, women who tested positive for HER2 exhibited a significantly improved response. In 1998, the food and drug administration, USA, offered medical experimental data for HER2-positive patients and permitted the drug [5]. In Europe, the Vectibix drug was unapproved by controllers because it could not be used for various patients [6]. This drug was supposed to treat Amgen colon cancer. The corporation completed an overall data assessment and exposed that Vectibix can perform well in the victims with tumor-lacked KRAS gene mutation, and the drug was allowed for such patients only [7].
Therefore, a physician can look into a patient’s gene variation profile, pick a medicine and suggest a treatment that decreases after-effects, thus yielding positive consequences. The individual vulnerability to specific diseases could be identified before manifestation. Hence, PM can be utilized to stop infections in vulnerable persons. With PM assistance, doctors can go for a one-size-fits-all model to prescribe medicines for an individual patient. Due to patient hereditary dissimilarities, gene reactions for specific drugs could differ from person to person. Hence, PM has propagated a unique discipline named “pharmacogenomics” that identifies an appropriate gene affecting medicine [1][2][8]. Scientists are exploring different strategies to develop personalized medicine, one of which is 3D printing. This article conducts a detailed analysis of 3D printing in drug delivery.
2. Three-Dimensional (3D) Printing
3D printing produces 3D parts in a layer-wise fashion using computer-aided (CAD) designs [9][10][11][12][13][14][15]. In 1996, for the very 1st time, 3D printing was used to prepare tablets [16]. Personalized 3D printed drugs can resolve various issues related to patients, including pharmacogenetic polymorphism [17]. Patients can also access more effective drugs with the least exposure to adverse drug reactions, which can elevate patients’ survival proportion [18][19][20]. 3D printers can produce various unique medicines, including transdermic patches and tablets. They also can produce a single dose containing various drugs to treat multiple diseases designed at the treatment point. It enhances patient compliance with the minimum side effects, resulting in a radical change in medicine design [21]. 3D printing technique has enormous characteristics and versatilities, producing any dose for various applications [22][23][24][25][26]. This method utilizes numerous health care facilities ranging from public drugstores to hospitals. Administration in these areas can increase medicine availability and decrease medicine consumption. Medication can be rapidly manufactured by using 3D printers in disaster zones, emergency sections, quick response units, and military missions [27]. 3D printing of reduced reaction vessels to synthesize API, on request, can deliver additional flexure to researchers and scientists. In comparison with traditional techniques, 3D printing can synthesize a wide variety of molecules at a mini scale, predominantly useful for those with elevated cost or deprived steadiness [28]. Clinical trials demand a vast range of doses [29].
3D printers can be handled easily with accurate material printing after changing the number of active ingredients. An accurate dosage with an anticipated design can be obtained that is not easy via other processing techniques [30]. The 3D printing technique can also produce even orphan drugs. These drugs are costly and, within Europe, affect 1 in 2000 people [31]. 3D printing has developed certain advantages, such as low-cost printing, wide availability, approved pharmaceutical ingredients, a substantial enhancement in morphology and mechanical confrontation, the appropriateness of various drug molecules, and the absence of post-printing steps [32].
In 3D printing, medicines, parts, medical implants, and devices are produced by accumulating material in a layer-wise fashion until the desired CAD file is obtained, physically [33]. Today, several printing processes are available with diverse printing techniques; however, each technique involves the following steps [13][34][35]: I. CAD software is applied to develop a three-dimensional model. II. Here, the model developed in step I is transformed into “.STL” format. III. Following on, the file is sliced via slicer (software). IV. A 3D part is manufactured via Computer Numerical Control codes.
This method uses a machine- or pneumatically-driven pressure to distribute bio-ink via an outlet and obeys a computer-designed model [36]. This process also involves printing in a layer-wise fashion same as other printing methods. Bio-inks are usually organic materials. This technique permits precise cells printing with minimal cells impairment. The printing technique is shown in Figure 1 .
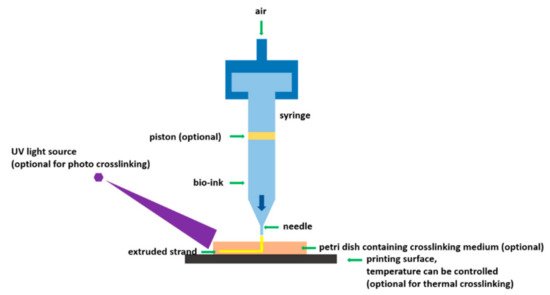
3. 3D Printing for Drugs Development: Early Phase Drugs, Complex Drugs, Unique Drugs, Solid Oral Drugs, and Polymeric Drugs
3D printing is gaining traction in the manufacturing industry, with the benefits of improving productivity and lowering both the cost and number of human-based faults [38][39]. Given its enormous flexibility and capacity to modify and construct a range of simple to complicated geometries, 3D printing has altered production rates with process automation. 3D printing is swiftly transforming pharmaceutical production to achieve elevated quality therapeutic products with improved process sturdiness in bio-pharmaceutical product evolution, where there is a dependence on medicines manufacturing via conventional manufacturing procedures [40][41]. Furthermore, 3D printing has proved its efficiency in biomedical engineering for diagnostics and treatments.
In this regard, 3D printing can aid in the benchmark establishment for community medicine success. Patients can determine their dosage demands based on their disease requirements rather than depending solely on the doctors [41][42][43]. The devoted software uses the provided information, which is utilized for medicine printing using an individual 3D printer. This process can easily be carried out at the community drugstore or household. Remote towns, military stations, and catastrophe administration zones can take advantage of this technique. The benefits of this strategy include reduction in medicines deficiencies and wastage, easier medicines access, and less dependency on paramedical staff. At the clinical drugstore, 3D printing can be utilized in the same way as “community medicine”. Patients typically take their doctor prescriptions to the pharmacist, and receive their medication [44]. In today’s world, the pharmacist may employ a 3D printer to give the medicine in a customized format utilizing the physician’s information. It can eliminate any medicine shortages and make individualized medicine treatment more widely available in clinical practices [45].
Solid oral drugs mainly comprise tablets with various geometrical and functional characteristics. 3D printing can manufacture different dosages with numerous medications to attain instant or prolonged release. Such medicines include rectum-, oral- and aspirin-based pills. Further, 3D printing increases the dissolution medicines which are poorly soluble [46][47][48][49]. To ensure quality, medicine transport structure by 3D printing must be exposed to regular pharmacopeial testing, comprised of rigidity, crumbliness, fragmentation and diffusing period assessment. Instant release pills are needed for the diseases that need quick medication. Medications can be divided into (a) fast resolving, (b) dispersible, (c) oral pills [41]. Traditional manufacturing of these medicines involves various steps, including proper quantity selection of ingredients to acquire required performance and machining. Using 3D printing, these formulations can be manufactured effectively. Generally, the medicine is distributed in a binding liquid, which is utilized for printing. FDM has also been applied to manufacture pills using polymeric filaments stuffed with drugs. Polymers, including polyvidone, Hypromellose, 2-hydroxypropyl ether and Polycaprolactone have been applied to filaments’ formulation, stuffed with drugs, and printed by extrusion (hot) process [50][51][52]. By changing the concentration of polymers within the filament, the medicine loading and releasing efficacies can be modified. Furthermore, 3D printing also delivers opportunities to change the pill/tablet’s geometrical features in correspondence to the medicine filling densities. These features are attained by varying the CAD model.
Furthermore, film characteristics optimization can be reached by altering the binding material ratio, inclusion of plasticizers and operating conditions [40]. These parameters also control the medication release performance. In contrary to instant release medicines, improved release medicines yield a characteristic medication spread outline that can be modified according to the patient’s disease. Different improved release medication systems have been manufactured, including complete- , prolonged-, administered-, and substituted-release [34][45][44]. Additional cases of improved release medication systems contain chronotherapeutic-, histopathological-, and multiple-APIs-release systems. Consequently, 3D printing is a valuable method to attain the intricate geometries of medicines. Rectum-release medicines were manufactured to regulate the medicine release and ingredient expansion within the intestines after providing safety to the medicine against the gastric acidic (stomach). These medicines need pre-coating with acid-resistant polymers to avoid the deprivation of drugs within the stomach. The pre-coating needs very good control of operating conditions to evade variations that occurred during the release of the medicine. For this purpose, 3D printing can be utilized to model the whole release structures by defining the particular area for medication release [53]. Different filling agents and polymeric materials are combined into the pill’s precise areas to attain personalized medication release outlines. Fused deposition modelling and binder jet printing can specifically be applied to design and print enteric-based releasing setups. Several enteric-based coating polymeric materials, including Hypromellose acetate succinate and 2-Methylpropenoic acid, were adopted for the prolonged spread of medication in the bowel section [54].
4. 3D Printing and Tissue Engineering
The goal of customized medicine delivery is to offer an effective product with fewer adverse side effects and better appropriateness. The antiepileptic medication “levetiracetam” was the primary FDA-approved 3D-printed medication. The pharmacologic activity was parallel to the traditional pills, although the solubilization period was shorter. After implementing the “Zip-dose” method, “Aprecia Pharmaceuticals” promoted a medication named “Spritam”. These pills were synthesized by selective laser melting. Its primary deposit contained APIs, filling materials, and a binder. The medication, having a dose amount of 1000 mg, was able to dissolve quickly within a few seconds [55]. Khaled et al. prepared a poly-pill with a self-sufficient and controlled releasing outline [56]. This technique was able to manufacture medicine for the human beings who are compelled to consume discrete pills in case of various diseases. Poly-pill was used for heat treatment using an instant releasing outline comprising two sections for acetylsalicylate and apo-hydro, and three separate sections for slektine, tenormin and altace. Anti-cancer medications encounter problems while arriving at the action site, and also get stuck in other organs, thus causing poisonousness. Similar to the vein injection and oral medicines, the traditional setups also flop, owing to the medication’s lower solubility, causing an increase in cancer patient problems. Therefore, modern tools can resolve the traditional medication limitation. Recently, a blotch was manufactured by combining efudex, 2-oxepanone homopolymer and polyglactin-910, which was effectively fixed on the pancreatic cancer area [57][58][59].
During organ transplantation, 3D printing of body tissues and key organs is crucial for patients. Given the scarcity of organ donors, 3D printing completed organs can bring a big influence on transplant waiting lists [60]. Organ printing has the potential to use the 3D printing method to develop tissues and organs utilizing a layer-wise accumulation method. Biomaterials, including collagen, hydrogels and various other synthetic materials are usually adopted in bio-printing to produce 3D tissues. In addition, stem cells are cultivated on hydrogel (supporting base) and used as a bio-link in the printing process [61]. The quality of the printed organ is usually identified by a variety of functional features, including material toughness, permeability and structure. Various pros of 3D bio-printing over conventional manufacturing processes include inexpensive printing, excellent shape accuracy and organ size, higher productivity, and visualization [61]. Inkjet printing and extrusion-based printing processes are commonly used techniques. These methods rely on bio-ink deposition over a base plate, guided by a 3D model of organs or tissues generated by computer-aided design software. The recent manufacturing of a full human heart and valves is an example of 3D-printed organs [62]. Bio-ink, a mixture of hydrogel derived from fatty acids and human tissues, was employed to manufacture organs via inkjet printing [63]. The printing of a heart with blood veins took 3–4 h, which was placed in a nutrient solution and oxygen was provided for a few days. As a result, the cells began to beat and behave like a functioning human heart [64]. Intriguingly, live 3D printing is also possible. According to the experts at the University of Sao Paulo Human Genome and Stem Cell Research Center, 3D printing of the liver organoids is achievable, and these organoids with mini-liver presented similar features to complete human liver cells [65]. Moreover, doctors at the University of Michigan, USA, used 3D printers and x-ray computed tomography scans to produce lungs airways [66]. Furthermore, 3D printing is also used to manufacture bladders [67]. At Boston Children Hospital, USA, researchers developed 3D printed bladders for patients with urine problems due to bladder disease. For dental surgeries, 3D printing is appropriate to manufacture teeth to substitute decayed teeth [68].
References
- Vogenberg, F.R.; Barash, C.I.; Pursel, M. Personalized medicine—Part 1: Evolution and development into theranostics. Pharm. Ther. 2010, 35, 560.
- Mancinelli, L.; Cronin, M.; Sadée, W. Pharmacogenomics: The promise of personalized medicine. AAPS PharmSci 2000, 2, 1–13.
- Abrahams, E.; Ginsburg, G.S.; Silver, M. The personalized medicine coalition: Goals and strategies. Am. J. Pharm. 2005, 5, 345–355.
- Langreth, B.R.; Waldholz, M. New Era of Personalized Medicine Targeting Drugs for Each Unique Genetic Profile. Oncologist 1999, 4, 426–427.
- Cobleigh, M.A.; Vogel, C.L.; Tripathy, D.; Robert, N.J.; Scholl, S.; Fehrenbacher, L.; Wolter, J.M.; Paton, V.; Shak, S.; Lieberman, G.; et al. Multinational Study of the Efficacy and Safety of Humanized Anti-HER2 Monoclonal Antibody in Women Who Have HER2-Overexpressing Metastatic Breast Cancer That Has Progressed After Chemotherapy for Metastatic Disease. J. Clin. Oncol. 1999, 17, 2639.
- Abrahams, E.; Silver, M. The case for personalized medicine. J. Diabetes Sci. Technol. 2009, 3, 680–684.
- Rizvi, U.Z. Looking forward, looking back. SAA Archaeol. Rec. 2008, 8, 6–8.
- Soni, N.; Jain, K.; Gupta, U.; Jain, N.K. Controlled delivery of Gemcitabine Hydrochloride using mannosylated poly(propyleneimine) dendrimers. J. Nanoparticle Res. 2015, 17, 1–17.
- Mahmood, M.A.; Popescu, A.C.; Hapenciuc, C.L.; Ristoscu, C.; Visan, A.I.; Oane, M.; Mihailescu, I.N. Estimation of clad geometry and corresponding residual stress distribution in laser melting deposition: Analytical modeling and experimental correlations. Int. J. Adv. Manuf. Technol. 2020, 111, 77–91.
- Mahmood, M.A.; Visan, A.I.; Ristoscu, C.; Mihailescu, I.N. Artificial Neural Network Algorithms for 3D Printing. Materials 2021, 14, 163.
- Mahmood, M.A.; Popescu, A.C.; Oane, M.; Ristoscu, C.; Chioibasu, D.; Mihai, S.; Mihailescu, I.N. Three-Jet Powder Flow and Laser–Powder Interaction in Laser Melting Deposition: Modelling Versus Experimental Correlations. Metals 2020, 10, 1113.
- Chioibasu, D.; Mihai, S.; Mahmood, M.A.; Lungu, M.; Porosnicu, I.; Sima, A.; Dobrea, C.; Tiseanu, I.; Popescu, A.C. Use of X-ray computed tomography for assessing defects in Ti grade 5 parts produced by laser melting deposition. Metals 2020, 10, 1408.
- Mahmood, M.A.; Popescu, A.C.; Mihailescu, I.N. Metal Matrix Composites Synthesized by Laser-Melting Deposition: A Review. Materials 2020, 13, 2593.
- Gross, B.C.; Erkal, J.L.; Lockwood, S.Y.; Chen, C.; Spence, D.M. Evaluation of 3D printing and its potential impact on biotechnology and the chemical sciences. Anal. Chem. 2014, 86, 3240–3253.
- Belhabib, S.; Guessasma, S. Compression performance of hollow structures: From topology optimisation to design 3D printing. Int. J. Mech. Sci. 2017, 133, 728–739.
- Wu, B.M.; Borland, S.W.; Giordano, R.A.; Cima, L.G.; Sachs, E.M.; Cima, M.J. Solid free-form fabrication of drug delivery devices. J. Control Release 1996, 40, 77–87.
- Bartlett, S. Printing organs on demand. Lancet Respir. Med. 2013, 1, 684.
- Khaled, S.A.; Burley, J.C.; Alexander, M.R.; Roberts, C.J. Desktop 3D printing of controlled release pharmaceutical bilayer tablets. Int. J. Pharm. 2014, 461, 105–111.
- Ursan, I.; Chiu, L.; Pierce, A. Three-dimensional drug printing: A structured review. J. Am. Pharm. Assoc. 2013, 53, 136–144.
- Banks, J. Adding value in additive manufacturing: Researchers in the United Kingdom and Europe look to 3D printing for customization. IEEE Pulse 2013, 4, 22–26.
- Lee Ventola, C. Medical applications for 3D printing: Current and projected uses. Pharm. Ther. 2014, 39, 704–711.
- Tagami, T.; Nagata, N.; Hayashi, N.; Ogawa, E.; Fukushige, K.; Sakai, N.; Ozeki, T. Defined drug release from 3D-printed composite tablets consisting of drug-loaded polyvinylalcohol and a water-soluble or water-insoluble polymer filler. Int. J. Pharm. 2018, 543, 361–367.
- Kadry, H.; Al-Hilal, T.A.; Keshavarz, A.; Alam, F.; Xu, C.; Joy, A.; Ahsan, F. Multi-purposable filaments of HPMC for 3D printing of medications with tailored drug release and timed-absorption. Int. J. Pharm. 2018, 544, 285–296.
- Wallin, T.J.; Pikul, J.; Shepherd, R.F. 3D printing of soft systems. Nat. Rev. Mate. 2018, 3, 84–100.
- Korte, C.; Quidbach, J. Formulation development and process analysis of drug-loaded filaments manufactured via hot-melt extrusion for 3D-printing of medicines. Phar. Dev. Tech. 2018, 23, 1117–1127.
- Awad, A.; Trenfield, S.J.; Gaisford, S.; Basit, A.W. 3D printed medicines: A new branch of digital healthcare. Int. J. Pharm. 2018, 548, 586–596.
- Norman, J.; Madurawe, R.D.; Moore, C.M.V.; Khan, M.A.; Khairuzzaman, A. A new chapter in pharmaceutical manufacturing: 3D-printed drug products. Adv. Drug Deliv. Rev. 2017, 108, 39–50.
- Hornung, C.H. The art of manufacturing molecules. Science 2019, 359, 273–274.
- Ku, M.S.; Dulin, W. A biopharmaceutical classification-based Right-First-Time formulation approach to reduce human pharmacokinetic variability and project cycle time from First-In-Human to clinical Proof-of-Concept. Pharm. Dev. Technol. 2012, 17, 285–302.
- Chen, D.; Heyer, S.; Ibbotson, S.; Salonitis, K.; Steingrímsson, J.G.; Thiede, S. Direct digital manufacturing: Definition, evolution, and sustainability implications. J. Clean. Prod. 2015, 107, 615–625.
- Cycle Pharmaceuticals to Use 3D Printing to Develop “Orphan Drugs”. Available online: https://www.cambridgeindependent.co.uk/business/cycle-pharmaceuticals-to-use-3d-printing-to-develop-orphan-drugs-9053341/ (accessed on 13 January 2021).
- Leonards, H.; Engelhardt, S.; Hoffmann, A.; Pongratz, L.; Schriever, S.; Bläsius, J.; Wehner, M.; Gillner, A. Advantages and drawbacks of Thiol-ene based resins for 3D-printing. In Laser 3D Manufacturing II, Proceedings of the SPIE LASE, San Francisco, CA, USA, 7–12 February 2015; Helvajian, H., Piqué, A., Wegener, M., Gu, B., Eds.; SPIE: Bellingham, WA, USA, 2015; Volume 9353, p. 93530F.
- Schubert, C.; Van Langeveld, M.C.; Donoso, L.A. Innovations in 3D printing: A 3D overview from optics to organs. Br. J. Ophthalmol. 2014, 98, 159–161.
- Khatri, P.; Shah, M.K.; Vora, N. Formulation strategies for solid oral dosage form using 3D printing technology: A mini-review. J. Drug Deliv. Sci. Technol. 2018, 46, 148–155.
- Mertz, L. New World of 3-D Printing Offers “Completely New Ways of Thinking”: Q&A with Author, Engineer, and 3-D Printing Expert Hod Lipson. IEEE Pulse 2013, 4, 12–14.
- Panwar, A.; Tan, L. Current Status of Bioinks for Micro-Extrusion-Based 3D Bioprinting. Molecules 2016, 21, 685.
- You, F.; Eames, B.F.; Chen, X. Application of Extrusion-Based Hydrogel Bioprinting for Cartilage Tissue Engineering. Int. J. Mol. Sci. 2017, 18, 1597.
- Choonara, Y.E.; Du Toit, L.C.; Kumar, P.; Kondiah, P.P.D.; Pillay, V. 3D-printing and the effect on medical costs: A new era? Expert Rev. Pharm. Outcomes Res. 2016, 16, 23–32.
- Palo, M.; Holländer, J.; Suominen, J.; Yliruusi, J.; Sandler, N. 3D printed drug delivery devices: Perspectives and technical challenges. Expert Rev. Med. Devices 2017, 14, 685–696.
- Mertz, L. Dream it, design it, print it in 3-D: What can 3-D printing do for you? IEEE Pulse 2013, 4, 15–21.
- El Aita, I.; Ponsar, H.; Quodbach, J. A Critical Review on 3D-printed Dosage Forms. Curr. Pharm. Des. 2018, 24, 4957–4978.
- Norman, C.; Mello, M.; Choi, B. Identifying frequent users of an Urban emergency medical service using descriptive statistics and regression analyses. West. J. Emerg. Med. 2016, 17, 39–45.
- Gu, B.K.; Choi, D.J.; Park, S.J.; Kim, M.S.; Kang, C.M.; Kim, C.H. 3-dimensional bioprinting for tissue engineering applications. Biomater. Res. 2016, 20, 1–8.
- Souto, E.B.; Campos, J.C.; Filho, S.C.; Teixeira, M.C.; Martins-Gomes, C.; Zielinska, A.; Carbone, C.; Silva, A.M. 3D printing in the design of pharmaceutical dosage forms. Pharm. Dev. Technol. 2019, 24, 1044–1053.
- Araújo, M.; Sa-Barreto, L.; Gratieri, T.; Gelfuso, G.; Cunha-Filho, M. The Digital Pharmacies Era: How 3D Printing Technology Using Fused Deposition Modeling Can Become a Reality. Pharmaceutics 2019, 11, 128.
- Lim, S.H.; Kathuria, H.; Tan, J.J.Y.; Kang, L. 3D printed drug delivery and testing systems—A passing fad or the future? Adv. Drug Deliv. Rev. 2018, 132, 139–168.
- Chia, H.-N.; Wu, B.-M. Recent advances in 3D printing of biomaterials. J. Biol. Eng. 2015, 9, 1–14.
- Sandler, N.; Preis, M. Printed Drug-Delivery Systems for Improved Patient Treatment. Trends Pharmacol. Sci. 2016, 37, 1070–1080.
- Vithani, K.; Goyanes, A.; Jannin, V.; Basit, A.W.; Gaisford, S.; Boyd, B.J. An Overview of 3D Printing Technologies for Soft Materials and Potential Opportunities for Lipid-based Drug Delivery Systems. Pharm. Res. 2019, 36, 1–20.
- Haleem, A.; Javaid, M.; Khan, R.H.; Suman, R. 3D printing applications in bone tissue engineering. J. Clin. Orthop. Trauma 2020, 11, S118–S124.
- Huang, W.; Zhang, X. 3D printing: Print the future of ophthalmology. Investig. Ophthalmol. Vis. Sci. 2014, 55, 5380–5381.
- Jammalamadaka, U.; Tappa, K. Recent advances in biomaterials for 3D printing and tissue engineering. J. Funct. Biomater. 2018, 9, 22.
- Guvendiren, M.; Molde, J.; Soares, R.M.D.; Kohn, J. Designing Biomaterials for 3D Printing. ACS Biomater. Sci. Eng. 2016, 2, 1679–1693.
- Jamróz, W.; Kurek, M.; Łyszczarz, E.; Brniak, W.; Jachowicz, R. Printing techniques: Recent developments in pharmaceutical technology. Acta Pol. Pharm.-Drug Res. 2017, 74, 753–763.
- SPRITAM (levetiracetam) Tablets. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/nda/2015/207958Orig1s000TOC.cfm (accessed on 17 January 2021).
- Khaled, S.A.; Burley, J.C.; Alexander, M.R.; Yang, J.; Roberts, C.J. 3D printing of five-in-one dose combination polypill with defined immediate and sustained release profiles. J. Control Release 2015, 217, 308–314.
- Singh, J.; Jain, K.; Mehra, N.K.; Jain, N.K. Dendrimers in anticancer drug delivery: Mechanism of interaction of drug and dendrimers. Artif. Cells Nanomed. Biotechnol. 2016, 44, 1626–1634.
- Yi, H.-G.; Choi, Y.-J.; Kang, K.-S.; Hong, J.-M.; Pati, R.G.; Park, M.N.; Shim, I.K.; Lee, C.M.; Kim, S.C.; Cho, D.W. A 3D-printed local drug delivery patch for pancreatic cancer growth suppression. J. Control Release 2016, 238, 231–241.
- Jain, A.; Jain, K.; Mehra, N.K.; Jain, N.K. Lipoproteins tethered dendrimeric nanoconstructs for effective targeting to cancer cells. J. Nanoparticle Res. 2013, 15, 1–18.
- Tappa, K.; Jammalamadaka, U. Novel Biomaterials Used in Medical 3D Printing Techniques. J. Funct. Biomater. 2018, 9, 17.
- Parak, A.; Pradeep, P.; du Toit, L.C.; Kumar, P.; Choonara, Y.E.; Pillay, V. Functionalizing bioinks for 3D bioprinting applications. Drug Discov. Today 2019, 24, 198–205.
- Mosadegh, B.; Xiong, G.; Dunham, S.; Min, J.K. Current progress in 3D printing for cardiovascular tissue engineering. Biomed. Mater. 2015, 10, 034002.
- Lueders, C.; Jastram, B.; Hetzer, R.; Schwandt, H. Rapid manufacturing techniques for the tissue engineering of human heart valves. Eur. J. Cardio-Thorac. Surg. 2014, 46, 593–601.
- Noor, N.; Shapira, A.; Edri, R.; Gal, I.; Wertheim, L.; Dvir, T. 3D Printing of Personalized Thick and Perfusable Cardiac Patches and Hearts. Adv. Sci. 2019, 6.
- Goulart, E.; De Caires-Junior, L.C.; Telles-Silva, K.A.; Araujo, B.H.S.; Rocco, S.A.; Sforca, M.; De Sousa, I.L.; Kobayashi, G.S.; Musso, C.M.; Assoni, A.F.; et al. 3D bioprinting of liver spheroids derived from human induced pluripotent stem cells sustain liver function and viability in vitro. Biofabrication 2020, 12, 015010.
- 3D-Airway Printed Splint|Otolaryngology|Michigan Medicine|University of Michigan. Available online: https://medicine.umich.edu/dept/otolaryngology/3d-airway-printed-splint (accessed on 17 January 2021).
- Youssef, R.F.; Spradling, K.; Yoon, R.; Dolan, B.; Chamberlin, J.; Okhunov, Z.; Clayman, R.; Landman, J. Applications of three-dimensional printing technology in urological practice. BJU Int. 2015, 116, 697–702.
- Dawood, A.; Marti, B.M.; Sauret-Jackson, V.; Darwood, A. 3D printing in dentistry. Br. Dent. J. 2015, 219, 521–529.





