Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Alessandro Di Federico | + 1830 word(s) | 1830 | 2021-08-04 07:53:51 | | | |
| 2 | Lily Guo | Meta information modification | 1830 | 2021-08-10 02:54:16 | | | | |
| 3 | Lily Guo | Meta information modification | 1830 | 2021-08-10 02:54:58 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Di Federico, A. DNA Damage Response and Repair. Encyclopedia. Available online: https://encyclopedia.pub/entry/12965 (accessed on 31 March 2026).
Di Federico A. DNA Damage Response and Repair. Encyclopedia. Available at: https://encyclopedia.pub/entry/12965. Accessed March 31, 2026.
Di Federico, Alessandro. "DNA Damage Response and Repair" Encyclopedia, https://encyclopedia.pub/entry/12965 (accessed March 31, 2026).
Di Federico, A. (2021, August 09). DNA Damage Response and Repair. In Encyclopedia. https://encyclopedia.pub/entry/12965
Di Federico, Alessandro. "DNA Damage Response and Repair." Encyclopedia. Web. 09 August, 2021.
Copy Citation
DNA damage response and repair (DDR) genes are necessary to maintain the integrity of cell DNA. Alterations of these mechanisms have been found in many cancer types, and may influence treatment outcomes as well as the prognosis of cancer patients. Recently, several treatment strategies taking advance of the presence of DDR alterations are emerging in oncology.
DNA Damage Response and Repair Genes
PARP inhibitors
olaparib
rucaparib
veliparib
talazoparib
BRCA
WEE1
ATM
CHK1
ATR
immunotherapy
PD-1/PD-L1
1. Introduction
The dysfunction of DNA repair machinery ultimately leads to the accumulation of somatic mutations, increasing the risk of developing cancer [1]. Six main DNA repair pathways operate depending on the type of DNA damage. Single-stranded breaks (SSBs) can lead to the activation of four different repair mechanisms based on the damage: base excision repair, nucleotide excision repair, mismatch repair, and translesion synthesis. Damage involving both DNA strands (double-stranded breaks) can activate two compensatory pathways: homologous recombination repair (HRR), an accurate system that uses a complementary strand from a sister chromatid to reproduce the original DNA sequence, and non-homologous end-joining, which is more error-prone as it utilizes no or limited homologous sequences to restore the damaged strand [2]. An increasing number of genes that help the DNA repair machinery to function have been identified, and the inherited deficiency of several genes, such as BRCA1/2, ATM, and PALB2, are linked to the predisposition of developing PC [3][4][5]. In particular, germline or somatic mutations of BRCA1, BRCA2, PALB2, ATM, and CHEK2 have been reported in 20% of PDAC, while a deficiency of HRR genes was documented in 15.4% of PC and ATM mutations in 9–18% of PC [6][7][8]. DDR deficiency is known to co-segregate with improved response to platinum derivatives consistently with the mechanism of action of these agents. Moreover, deficient DDR machinery can enhance an immune response in multiple ways, providing the rationale for the combination of DDR-targeting agents and immunotherapy [9]. The number of antitumor agents taking advantage of DDR deficiency is constantly expanding and many trials are ongoing (Table 1), hopefully to provide increasing treatment possibilities for PC patients.
Table 1. Ongoing trials evaluating activity and efficacy of PARP inhibitors in PC (Clinicaltrials.gov last accessed 10 June 2021).
| Target | Tumor | Setting | Treatment Arms | Phase | Primary Outcome | N of Patients | clinicaltrial.gov Identifier |
|---|---|---|---|---|---|---|---|
| PARP | PC | Advanced, pretreated, without germline BRCA1/2 mutations but with BRCAness phenotype | olaparib | II | ORR | 34 | NCT02677038 |
| PARP | AST | Advanced, pretreated | (1) AZD6738 | II | ORR | 68 | NCT03682289 |
| ATR | (2) AZD6738 + olaparib | ||||||
| PARP | AST | Advanced, pretreated | cediranib + olaparib | II | ORR | 126 | NCT02498613 |
| VEGF | |||||||
| PARP | PC | Advanced, with BRCA1/2 or PALB2 mutation | (1) veliparib + gemcitabine hydrochloride + cisplatin | II | ORR Dose-finding | 107 | NCT01585805 |
| (2) gemcitabine hydrochloride + cisplatin | |||||||
| (3) veliparib | |||||||
| PARP | PC | Metastatic, untreated, with HRD | rucaparib + nal-IRI, leucovorin, fluorouracil | II | ORR | 110 | NCT03337087 |
| DLTs | |||||||
| PARP | AST | Advanced, pretreated, with HRD | rucaparib | II | ORR | 220 | NCT04171700 |
| PARP | PC | Advanced, pretreated, with BRCA1/2, PALB2, CHEK2 or ATM mutation | niraparib | II | PFS | 32 | NCT03601923 |
| PARP | PC | Advanced, pretreated | niraparib + dostarlimab + RT | II | DCR | 25 | NCT04409002 |
| PARP | PC | Advanced, pretreated, with DDR genes alteration | niraparib | II | ORR | 18 | NCT03553004 |
| PARP | PC | Advanced, following platinum-based CT without PD | (1) niraparib + nivolumab | Ib/II | PFS | 84 | NCT03404960 |
| (2) niraparib + ipilimumab | |||||||
| PARP | PC | Resected, after completion of (neo)adjuvant CT (+/− RT), with BRCA1/2 or PALB2 mutation | (1) olaparib (2) placebo | II | RFS | 152 | NCT04858334 |
| PARP | PC | metastatic, following platinum-based CT without PD, with BRCA1/2 mutation | (1) olaparib + pembrolizumab (2) olaparib | II | PFS | 88 | NCT04548752 |
| PD-1 | |||||||
| PARP, PD-1 | PC | Metastatic, pretreated, with BRCA1/2, PALB2, BARD1, RAD51c/d mutation | niraparib + dostarlimab | II | DCR | 20 | NCT04493060 |
| PARP, PD-1 | PC | metastatic, untreated, following low-dose CT with gemcitabine, nab-paclitaxel, capecitabine, cisplatin, and irinotecan (GAX-CI) | olaparib + pembrolizumab | II | PFS | 38 | NCT04753879 |
| PARP | PC | Advanced, untreated, with BRCA1/2 or PALB2 mutation | (1) fluzoparib + mFOLFIRINOX followed by fluzoparib maintenance | Ib/II | DLTs MTD ORR |
66 | NCT04228601 |
| (2) placebo + mFOLFIRINOX followed by placebo maintenance | |||||||
| WEE1 | PC | Metastatic, untreated | (1) adavosertib (MK-1775) + nab-paclitaxel + gemcitabine | I/II | MTD PFS |
133 | NCT02194829 |
| (2) placebo + nab-paclitaxel + gemcitabine | |||||||
| RAD51 | AST | Advanced, any line | CYT-0851 | I/II | DLTs ORR |
165 | NCT03997968 |
2. PARP Inhibitors
Poly-ADP-ribose polymerase inhibitors (PARPis) take advantage of the concept of synthetic lethality, which is defined by the combination of inactivating mutations in two or more different genes essential for cell integrity, inducing cell death [10]. The PARP-1 gene is involved in several phases of the DNA repair machinery, especially in preventing SSBs [11]. Thus, PARPis determine the accumulation of unrepaired SSBs, which are converted into DSBs during cell replication (Figure 1). In this scenario, the concomitant presence of HRR deficiency, such as BRCA1/2 inactivating mutations, enhances a predisposition to synthetic lethality [12].
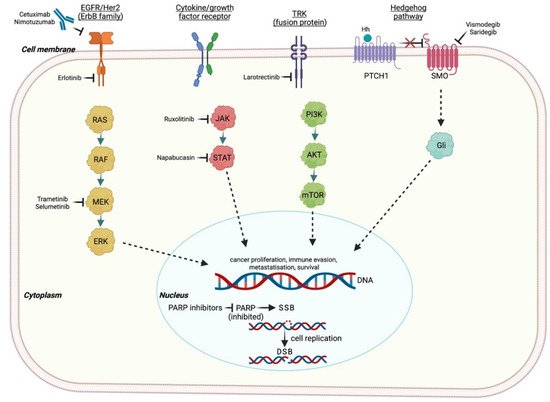
Figure 1. Main transmembrane receptor and intracellular pathways evaluated as potential therapeutic targets in PC. EGFR: epidermal growth factor receptor; HER-2: human epidermal growth factor receptor 2; NTRK: neurotrophic tyrosine receptor kinase; PTCH1: 12-transmembrane patched protein 1; SMO: 7-transmembrane smoothened protein: RAS: rat sarcoma; RAF: rapidly accelerated fibrosarcoma; MEK: mitogen-activated protein kinase; ERK: extracellular signal-regulated kinase; JAK: Janus kinase; STAT: signal transducer and activator of transcription; PI3K: phosphoinositide-3-kinase; mTOR: mechanistic target of rapamycin; Gli: 5-zinc-finger transcription factor; SSB: single-stranded break; DSB: double-stranded break; PARP: poly ADP-ribose polymerase. Created with BioRender.com (accessed on 14 July 2021).
Following this, we describe the current knowledge and the incoming opportunities concerning PARP inhibition in PC.
2.1. Olaparib
At the time of this review, olaparib represents the only approved PARPi in PC. The phase II trial conducted by Kaufman et al. evaluated olaparib monotherapy (400 mg twice daily) in patients with recurrent cancer that harbor germline BRCA1/2 mutations [13]. Twenty-three patients with PC who received a prior treatment with gemcitabine were included in the study. The objective response rate (ORR) was 21.7% (95% CI, 7.5 to 43.7), and stable disease (SD) lasting ≥8 weeks was observed in 34.8% of patients. A promising median progression-free survival (PFS) of 4.6 months and overall survival (OS) of 9.8 months were also documented. Olaparib approval in PC was obtained following the results of the randomized, double-blind, placebo-controlled, phase III POLO trial. A total of 154 patients with metastatic PC and a germline mutation of BRCA1/2 who did not progress during first-line platinum-based chemotherapy were randomized to receive olaparib monotherapy (300 mg twice daily) or placebo as maintenance therapy [14]. Median PFS was significantly prolonged in the olaparib group (7.4 vs. 3.8 months; HR 0.53; CI 95% 0.35–0.82; p = 0.004), while median OS was similar between groups. Notably, two studies evaluating the combination of olaparib and chemotherapy are discontinued due to severe toxicity issues [15][16].
2.2. Veliparib
Veliparib is an oral PARPi with lower PARP trapping ability compared with Olaparib [17][18]. A single arm, phase II trial tested this agent at a dose of 400 mg twice daily in previously treated stage III/IV PC patients with a germline BRCA1/2 or PALB2 mutation [19]. Unfortunately, no tumor response was documented, but SD lasting ≥4 months was observed in 25% of patients. The addition of veliparib (80 mg twice daily on days 1 to 12 every 3 weeks) to cisplatin, plus gemcitabine chemotherapy (25 mg/m2 and 600 mg/m2, respectively, both on days 3 and 10), was recently evaluated in a two-arm, phase II trial enrolling 50 patients with stage III/IV untreated PC and a germline BRCA1/2 or PALB2 mutation [20]. Both arms demonstrated high antitumor activity, with a disease control rate (DCR) of 100% in the combination arm versus 78.3% in the chemotherapy alone arm (p = 0.02), although no significant difference in ORR was observed (74.1% vs. 65.2% in the triplet and doublet arm, respectively; p = 0.055). Conversely, a notable increase of hematologic toxicities was reported in the combination arm. Veliparib was also tested, in addition to modified FOLFIRI, as a second-line treatment for metastatic PC patients, showing no additional benefit among biomarker unselected patients [21].
2.3. Rucaparib
The single-arm phase II RUCAPANC study investigated efficacy and safety of the oral PARPi rucaparib (600 mg twice daily) among 19 patients with pretreated locally advanced/metastatic PC harboring a germline or somatic BRCA1/2 mutation [22]. Rucaparib demonstrated an acceptable toxicity profile and provided clinical benefits, as ORR was 15.8% and DCR was 31.6%. Rucaparib (600 mg twice daily) was then investigated as maintenance monotherapy in a single-arm phase II trial, enrolling patients with advanced pancreatic cancer and harboring a BRCA1/2 or PALB2 mutation but who did not show PD following at least 4 months of platinum-based chemotherapy [23]. Again, this agent showed encouraging antitumor activity with a safe toxicity profile, as median PFS was 9.1 months, ORR was 36.8%, and 89.5% of patients achieved DCR lasting ≥8 weeks.
2.4. Talazoparib
Talazoparib is a novel, potent oral PARPi. The two-part, dose-escalation, phase I trial by de Bono et al. tested this agent in patients with advanced solid tumors and a germline BRCA1/2 mutation [24]. Talazoparib showed a tolerable profile and promising antitumor activity, as ORR was 20% among 20 patients with advanced PC.
Ongoing trials investigating the use of PARPis alone or combined with different agents for the treatment of advanced PC patients are summarized in Table 1. These agents have demonstrated a synergistic effect with programmed death-1/programmed death-ligand 1 (PD-1/PD-L1) inhibitors in murine models, possibly due to PD-L1 upregulation in the tumor microenvironment [25][26]. Moreover, the addition of a MEK inhibitor to a PARPi and a PD-(L)1 inhibitor is currently under evaluation to overcome RAS-mediated resistance to PARPis in RAS-mutant PC, which was reported in preclinical models [27].
3. Further DDR Targeting Agents
PARPis represent only a small part of the wide scenario of DDR gene inhibition. The interest in DDR genes has risen in recent years as an increasing number of specific agents targeting these pathways is in the testing or development phase. The ataxia-telangiectasia mutated (ATM) gene plays a central role in DNA damage response and DSB repair, and its germline mutation is known to produce a specific syndrome, as well as increasing the risk of developing several types of cancer, including PC [28]. Once the ATM signal is disrupted, the cell relies on downstream ATR and CHK1/2 pathways to ensure DNA repair, arresting the cell cycle and preventing the DNA fork from collapsing. These functions make them two possible targets in ATM-deficient tumors, which account for 9–18% of sporadic PC [29][30]. Consistently, a sensitization of ATM-mutated PC cell lines to PARP, ATR, and CHK1/2 inhibitors, alone or in combination with other agents, have been demonstrated in preclinical studies [31][32][33]. Considering these data, several ongoing clinical trials are evaluating the potential of ATM, ATR, and CHK1 inhibitors in patients with PDAC (Table 1).
WEE1 regulates the G2 DNA damage checkpoint in concert with CHK1 during cell replication, which delays the completion of mitosis of cells that suffer genomic damage, thus, increasing cell viability [34]. These functions provide the rationale of blocking WEE1 to increase the efficacy of DNA damaging agents and to enhance synthetic lethality. MK-1775 (also known as AZD1775 and adavosertib), a WEE1 inhibitor, has been tested in combination with several DNA damaging agents in preclinical studies, such as gemcitabine, mitomycin C, and platinum derivatives [35][36]. A phase I trial enrolling 176 patients with refractory solid tumors evaluated adavosertib in combination with chemotherapy (either carboplatin, cisplatin, or gemcitabine) and documenting a 10% ORR. The response rate was significantly higher (21%) in the subpopulation of TP53-deficient patients as these tumors strongly depend on WEE1 activation to arrest the cell cycle in response to DNA damage [37][38]. Recently, a dose-escalation trial enrolling treatment-naïve, locally advanced PC patients documented a median OS of 21.7 months (90% CI, 16.7 to 24.8 months), and a median PFS of 9.4 months (90% CI, 8.0 to 9.9 months) with a combination of adavosertib, gemcitabine, and radiation therapy (RT) [39]. A phase I/II trial evaluating the addition of adavosertib to chemotherapy in metastatic PC is ongoing (Table 1).
References
- Christopher J. Lord; Alan Ashworth; PARP inhibitors: Synthetic lethality in the clinic. Science 2017, 355, 1152-1158, 10.1126/science.aam7344.
- Jan H. J. Hoeijmakers; Genome maintenance mechanisms for preventing cancer. Nature 2001, 411, 366-374, 10.1038/35077232.
- Geeta Lal; Geoffrey Liu; B Schmocker; P Kaurah; H Ozcelik; S A Narod; M Redston; S Gallinger; Inherited predisposition to pancreatic adenocarcinoma: role of family history and germ-line p16, BRCA1, and BRCA2 mutations.. Cancer Research 2000, 60, 409-416.
- Nicholas Roberts; Yuchen Jiao; Jun Yu; Levy Kopelovich; Gloria M. Petersen; Melissa L. Bondy; Steven Gallinger; Ann G. Schwartz; Sapna Syngal; Michele L. Cote; et al.Jennifer E AxilbundRichard D SchulickSyed Z. AliJames R. EshlemanVictor VelculescuMichael GogginsBert VogelsteinNickolas PapadopoulosRalph H. HrubanKenneth W. KinzlerAlison P. Klein ATM Mutations in Patients with Hereditary Pancreatic Cancer. Cancer Discovery 2011, 2, 41-46, 10.1158/2159-8290.cd-11-0194.
- Siân Jones; Ralph H. Hruban; Mihoko Kamiyama; Michael Borges; Xiaosong Zhang; D. Williams Parsons; Jimmy Cheng-Ho Lin; Emily Palmisano; Kieran Brune; Elizabeth Jaffee; et al.Christine A. Iacobuzio-DonahueAnirban MaitraGiovanni ParmigianiScott E KernVictor VelculescuKenneth W. KinzlerBert VogelsteinJames R. EshlemanMichael GogginsAlison P. Klein Exomic Sequencing Identifies PALB2 as a Pancreatic Cancer Susceptibility Gene. Science 2009, 324, 217-217, 10.1126/science.1171202.
- Andrew J. Aguirre; Jonathan A. Nowak; Nicholas Camarda; Richard A. Moffitt; Arezou A. Ghazani; Mehlika Hazar-Rethinam; Srivatsan Raghavan; Jaegil Kim; Lauren K. Brais; Dorisanne Ragon; et al.Marisa W. WelchEmma ReillyDevin McCabeLori MariniKristin AnderkaKarla HelvieNelly OliverAna BabicAnnacarolina Da SilvaBrandon NadresEmily E. Van SeventerHeather A. ShahzadeJoseph P. St. PierreKelly P. BurkeThomas E ClancyJames M. ClearyLeona A. DoyleKunal JajooNadine J. McClearyJeffrey A. MeyerhardtJanet E. MurphyKimmie NgAnuj K. PatelKimberly PerezMichael H. RosenthalDouglas A. RubinsonMarvin RyouGeoffrey I. ShapiroEwa SicinskaStuart G. SilvermanRebecca J. NagyRichard B. LanmanDeborah KnoerzerDean J. WelschMatthew B. YurgelunCharles S. FuchsLevi A. GarrawayGad GetzJason L. HornickBruce E. JohnsonMatthew H. KulkeRobert J. MayerJeffrey MillerPaul B. ShynDavid A. TuvesonNikhil WagleJen Jen YehWilliam C. HahnRyan B. CorcoranScott L. CarterBrian M. Wolpin Real-time Genomic Characterization of Advanced Pancreatic Cancer to Enable Precision Medicine. Cancer Discovery 2018, 8, 1096-1111, 10.1158/2159-8290.cd-18-0275.
- Arielle L. Heeke; Michael J. Pishvaian; Filipa Lynce; Joanne Xiu; Jonathan R. Brody; Wang-Juh Chen; Tabari M. Baker; John L. Marshall; Claudine Isaacs; Prevalence of Homologous Recombination–Related Gene Mutations Across Multiple Cancer Types. JCO Precision Oncology 2018, 2018, 1-13, 10.1200/po.17.00286.
- Ronan Russell; Lukas Perkhofer; Stefan Liebau; Qiong Lin; André Lechel; Fenja M. Feld; Elisabeth Hessmann; Jochen Gaedcke; Melanie Güthle; Martin Zenke; et al.Daniel HartmannGuido Von FiguraStephanie E. WeissingerKarl Lenhard RudolphPeter MöllerJochen K. LennerzThomas SeufferleinMartin WagnerAlexander Kleger Loss of ATM accelerates pancreatic cancer formation and epithelial–mesenchymal transition. Nature Communications 2015, 6, 7677, 10.1038/ncomms8677.
- Giuseppe Lamberti; Elisa Andrini; Monia Sisi; Alessandro Di Federico; Biagio Ricciuti; Targeting DNA damage response and repair genes to enhance anticancer immunotherapy: rationale and clinical implication. Future Oncology 2020, 16, 1751-1766, 10.2217/fon-2020-0215.
- Nigel O'Neil; Melanie L. Bailey; Philip Hieter; Synthetic lethality and cancer. Nature Reviews Microbiology 2017, 18, 613-623, 10.1038/nrg.2017.47.
- Arnab Ray Chaudhuri; Arnab Ray Chaudhuri André Nussenzweig; The multifaceted roles of PARP1 in DNA repair and chromatin remodelling. Nature Reviews Molecular Cell Biology 2017, 18, 610-621, 10.1038/nrm.2017.53.
- Clare L. Scott; Elizabeth M. Swisher; Scott Kaufmann; Poly (ADP-Ribose) Polymerase Inhibitors: Recent Advances and Future Development. Journal of Clinical Oncology 2015, 33, 1397-1406, 10.1200/jco.2014.58.8848.
- Bella Kaufman; Ronnie Shapira-Frommer; Rita K. Schmutzler; M. William Audeh; Michael Friedlander; Judith Balmaña; Gillian Mitchell; Georgeta Fried; Salomon M. Stemmer; Ayala Hubert; et al.Ora RosengartenMariana SteinerNiklas LomanKarin BowenAnitra FieldingSusan M. Domchek Olaparib Monotherapy in Patients With Advanced Cancer and a Germline BRCA1/2 Mutation. Journal of Clinical Oncology 2015, 33, 244-250, 10.1200/jco.2014.56.2728.
- Talia Golan; Pascal Hammel; Michele Reni; Eric Van Cutsem; Teresa Macarulla; Michael J. Hall; Joon-Oh Park; Daniel Hochhauser; Dirk Arnold; Do-Youn Oh; et al.Anke Reinacher-SchickGiampaolo TortoraHana AlgülEileen M. O'ReillyDavid McGuinnessKaren Y. CuiKatia SchliengerGershon Y. LockerHedy L. Kindler Maintenance Olaparib for Germline BRCA-Mutated Metastatic Pancreatic Cancer. New England Journal of Medicine 2019, 381, 317-327, 10.1056/nejmoa1903387.
- J. Bendell; Eileen M. O'Reilly; M. R. Middleton; I. Chau; H. Hochster; A. Fielding; W. Burke; Iii H. Burris; Phase I study of olaparib plus gemcitabine in patients with advanced solid tumours and comparison with gemcitabine alone in patients with locally advanced/metastatic pancreatic cancer. Annals of Oncology 2015, 26, 804-811, 10.1093/annonc/mdu581.
- Mark Yarchoan; Melinda C. Myzak; Burles A. Johnson; Ana De Jesus-Acosta; Dung T. Le; Elizabeth Jaffee; Nilofer S. Azad; Ross C. Donehower; Lei Zheng; Paul E. Oberstein; et al.Robert L. FineDaniel A. LaheruMichael Goggins Olaparib in combination with irinotecan, cisplatin, and mitomycin C in patients with advanced pancreatic cancer. Oncotarget 2017, 8, 44073-44081, 10.18632/oncotarget.17237.
- Junko Murai; Shar-Yin N. Huang; Benu Brata DAS; Amelie Renaud; Yiping Zhang; James H. Doroshow; Jiuping Ji; Shunichi Takeda; Yves Pommier; Trapping of PARP1 and PARP2 by Clinical PARP Inhibitors. Cancer Research 2012, 72, 5588-5599, 10.1158/0008-5472.can-12-2753.
- Yves Pommier; Mark J. O’Connor; Johann De Bono; Laying a trap to kill cancer cells: PARP inhibitors and their mechanisms of action. Science Translational Medicine 2016, 8, 362ps17-362ps17, 10.1126/scitranslmed.aaf9246.
- Maeve A. Lowery; David P. Kelsen; Marinela Capanu; Sloane C. Smith; Jonathan W. Lee; Zsofia K. Stadler; Malcolm J. Moore; Hedy L. Kindler; Talia Golan; Amiel Segal; et al.Hannah MaynardEllen HollywoodMaryEllen MoynahanErin E. Salo-MullenRichard Kinh Gian DoAlice P. ChenKenneth H. YuLaura H. TangEileen M. O'Reilly Phase II trial of veliparib in patients with previously treated BRCA-mutated pancreas ductal adenocarcinoma. European Journal of Cancer 2017, 89, 19-26, 10.1016/j.ejca.2017.11.004.
- Eileen M. O’Reilly; Jonathan W. Lee; Mark Zalupski; Marinela Capanu; Jennifer Park; Talia Golan; Esther Tahover; Maeve Lowery; Joanne F. Chou; Vaibhav Sahai; et al.Robin BrennerHedy L. KindlerKenneth H. YuAlice ZervoudakisShreya VemuriZsofia K. StadlerRichard K. G. DoNeesha DhaniAlice P. ChenDavid P. Kelsen Randomized, Multicenter, Phase II Trial of Gemcitabine and Cisplatin With or Without Veliparib in Patients With Pancreas Adenocarcinoma and a Germline BRCA/PALB2 Mutation. Journal of Clinical Oncology 2020, 38, 1378-1388, 10.1200/jco.19.02931.
- E. Gabriela Chiorean; Katherine A Guthrie; Philip Agop Philip; Elizabeth M. Swisher; Florencia Jalikis; Michael J. Pishvaian; Jordan Berlin; Marcus Smith Noel; Jennifer Marie Suga; Ignacio Garrido-Laguna; et al.Dana Backlund CardinDanika L. LewAndrew M. LowyHoward S. Hochster Randomized phase II study of second-line modified FOLFIRI with PARP inhibitor ABT-888 (Veliparib) (NSC-737664) versus FOLFIRI in metastatic pancreatic cancer (mPC): SWOG S1513.. Journal of Clinical Oncology 2019, 37, 4014-4014, 10.1200/jco.2019.37.15_suppl.4014.
- Rachna T. Shroff; Andrew Hendifar; Robert R. McWilliams; Ravit Geva; Ron Epelbaum; Lindsey Rolfe; Sandra Goble; Kevin K. Lin; Andrew V. Biankin; Heidi Giordano; et al.Robert H. VonderheideSusan M. Domchek Rucaparib Monotherapy in Patients With Pancreatic Cancer and a Known Deleterious BRCA Mutation. JCO Precision Oncology 2018, 2, 1-15, 10.1200/po.17.00316.
- Kim A. Reiss Binder; Rosemarie Mick; Mark O'hara; Ursina Teitelbaum; Thomas Karasic; Charles Schneider; Peter J. O'dwyer; Erica Carpenter; Austin Pantel; Mehran Makvandi; et al.David MankoffKatherine NathansonKara MaxwellStacy CowdenMary Jane FuhrerJanae RomeoGregory L. BeattySusan Domchek Abstract CT234: A Phase II, single arm study of maintenance rucaparib in patients with platinum-sensitive advanced pancreatic cancer and a pathogenic germline or somatic mutation inBRCA1, BRCA2orPALB2. Clinical Trials 2019, 79, CT234-CT234, 10.1158/1538-7445.sabcs18-ct234.
- Johann De Bono; Ramesh K. Ramanathan; Lida Mina; Rashmi Chugh; John Glaspy; Saeed Rafii; Stan Kaye; Jasgit Sachdev; John Heymach; David Smith; et al.Joshua W. HenshawAshleigh HerriottMiranda PattersonNicola CurtinLauren Averett ByersZev A. Wainberg Phase I, Dose-Escalation, Two-Part Trial of the PARP Inhibitor Talazoparib in Patients with Advanced Germline BRCA1/2 Mutations and Selected Sporadic Cancers. Cancer Discovery 2017, 7, 620-629, 10.1158/2159-8290.cd-16-1250.
- Shiping Jiao; Weiya Xia; Hirohito Yamaguchi; Yongkun Wei; Mei-Kuang Chen; Jung-Mao Hsu; Jennifer L. Hsu; Wen-Hsuan Yu; Yi Du; Heng-Huan Lee; et al.Chia-Wei LiChao-Kai ChouSeung-Oe LimShih-Shin ChangJennifer LittonBanu ArunGabriel N. HortobagyiMien-Chie Hung PARP Inhibitor Upregulates PD-L1 Expression and Enhances Cancer-Associated Immunosuppression. Clinical Cancer Research 2017, 23, 3711-3720, 10.1158/1078-0432.ccr-16-3215.
- Liliane Robillard; Minh Nguyen; Andrea Loehr; Sandra Orsulic; Rebecca S. Kristeleit; Kevin Lin; Mitch Raponi; Thomas C. Harding; Andrew D. Simmons; Abstract 3650: Preclinical evaluation of the PARP inhibitor rucaparib in combination with PD-1 and PD-L1 inhibition in a syngeneic BRCA1 mutant ovarian cancer model. Immunology 2017, 77, 3650-3650, 10.1158/1538-7445.am2017-3650.
- Chaoyang Sun; Yong Fang; Jun Yin; Jian Chen; Zhenlin Ju; Dong Zhang; Xiaohua Chen; Christopher P. Vellano; Kang Jin Jeong; Patrick Kwok-Shing Ng; et al.Agda Karina B. EterovicNeil H. BholaYiling LuShannon N. WestinJennifer R. GrandisShiaw-Yih LinKenneth L. ScottGuang PengJoan BruggeGordon B. Mills Rational combination therapy with PARP and MEK inhibitors capitalizes on therapeutic liabilities in RAS mutant cancers. Science Translational Medicine 2017, 9, eaal5148, 10.1126/scitranslmed.aal5148.
- Colin C. Pritchard; Joaquin Mateo; Michael F. Walsh; Navonil De Sarkar; Wassim Abida; Himisha Beltran; Andrea Garofalo; Roman Gulati; Suzanne Carreira; Rosalind Eeles; et al.Olivier ElementoMark RubinDan RobinsonRobert LonigroMaha HussainArul ChinnaiyanJake VinsonJulie FilipenkoLevi GarrawayMary-Ellen TaplinSaud H AlDubayanG. Celine HanMallory BeightolColm MorrisseyBelinda NghiemHeather H. ChengBruce MontgomeryTom WalshSilvia CasadeiMichael BergerLiying ZhangAhmet ZehirJoseph VijaiHoward I. ScherCharles SawyersNikolaus SchultzPhilip KantoffDavid SolitMark RobsonEliezer M. Van AllenKenneth OffitJohann De BonoPeter S. Nelson Inherited DNA-Repair Gene Mutations in Men with Metastatic Prostate Cancer. New England Journal of Medicine 2016, 375, 443-453, 10.1056/nejmoa1603144.
- Samantha A. Armstrong; Christopher W. Schultz; Ariana Azimi-Sadjadi; Jonathan R. Brody; Michael J. Pishvaian; ATM Dysfunction in Pancreatic Adenocarcinoma and Associated Therapeutic Implications. Molecular Cancer Therapeutics 2019, 18, 1899-1908, 10.1158/1535-7163.mct-19-0208.
- Michael Choi; Thomas Kipps; Razelle Kurzrock; ATM Mutations in Cancer: Therapeutic Implications. Molecular Cancer Therapeutics 2016, 15, 1781-1791, 10.1158/1535-7163.mct-15-0945.
- Lukas Perkhofer; Anna Schmitt; Maria Carolina Romero Carrasco; Michaela Ihle; Stephanie Hampp; Dietrich A. Ruess; Elisabeth Hessmann; Ronan Russell; André Lechel; Ninel Azoitei; et al.Qiong LinStefan LiebauMeike HohwielerHanibal BohnenbergerMarina LesinaHana AlgülLaura GieldonEvelin SchröckJochen GaedckeMartin WagnerLisa WiesmüllerBence SiposThomas SeufferleinHans Christian ReinhardtPierre-Olivier FrappartAlexander Kleger ATM Deficiency Generating Genomic Instability Sensitizes Pancreatic Ductal Adenocarcinoma Cells to Therapy-Induced DNA Damage. Cancer Research 2017, 77, 5576-5590, 10.1158/0008-5472.can-17-0634.
- Yann Wallez; Charles R. Dunlop; Timothy I Johnson; Siang-Boon Koh; Chiara Fornari; James W.T. Yates; Sandra Bernaldo De Quirós Fernández; Alan Lau; Frances M. Richards; Duncan I. Jodrell; et al. The ATR Inhibitor AZD6738 Synergizes with Gemcitabine In Vitro and In Vivo to Induce Pancreatic Ductal Adenocarcinoma Regression. Molecular Cancer Therapeutics 2018, 17, 1670-1682, 10.1158/1535-7163.mct-18-0010.
- Min Liang; Tiangang Zhao; Linfeng Ma; Yingjie Guo; CHK1 inhibition sensitizes pancreatic cancer cells to gemcitabine via promoting CDK-dependent DNA damage and ribonucleotide reductase downregulation. Oncology Reports 2017, 39, 1322-1330, 10.3892/or.2017.6168.
- Matthew J. O'connell; Jeanette M. Raleigh; Heather Verkade; Paul Nurse; Chk1 is a wee1 kinase in the G2 DNA damage checkpoint inhibiting cdc2 by Y15 phosphorylation. The EMBO Journal 1997, 16, 545-554, 10.1093/emboj/16.3.545.
- N.V. RajeshKumar; Elizabeth De Oliveira; Niki Ottenhof; James Watters; David Brooks; Tim DeMuth; Stuart D. Shumway; Shinji Mizuarai; Hiroshi Hirai; Anirban Maitra; et al.Manuel Hidalgo MK-1775, a Potent Wee1 Inhibitor, Synergizes with Gemcitabine to Achieve Tumor Regressions, Selectively in p53-Deficient Pancreatic Cancer Xenografts. Clinical Cancer Research 2011, 17, 2799-2806, 10.1158/1078-0432.ccr-10-2580.
- Shruti Lal; Mahsa Zarei; Saswati N. Chand; Emanuela Dylgjeri; Nicole C. Mambelli-Lisboa; Michael J. Pishvaian; Charles J. Yeo; Jordan M. Winter; Jonathan R. Brody; WEE1 inhibition in pancreatic cancer cells is dependent on DNA repair status in a context dependent manner. Scientific Reports 2016, 6, 33323, 10.1038/srep33323.
- Suzanne Leijen; Robin M.J.M. Van Geel; Anna C. Pavlick; Raoul Tibes; Lee Rosen; Albiruni R. Abdul Razak; Raymond Lam; Tim Demuth; Shelonitda Rose; Mark A. Lee; et al.Tomoko FreshwaterStuart ShumwayLi Wen LiangAmit OzaJan H.M. SchellensGeoffrey I. Shapiro Phase I Study Evaluating WEE1 Inhibitor AZD1775 As Monotherapy and in Combination With Gemcitabine, Cisplatin, or Carboplatin in Patients With Advanced Solid Tumors. Journal of Clinical Oncology 2016, 34, 4371-4380, 10.1200/jco.2016.67.5991.
- Jos H. Beijnen; Jan H.M. Schellens; Abrogation of the G2 Checkpoint by Inhibition of Wee-1 Kinase Results in Sensitization of p53-Deficient Tumor Cells to DNA-Damaging Agents. Current Clinical Pharmacology 2010, 5, 186-191, 10.2174/157488410791498824.
- Kyle C. Cuneo; Meredith A. Morgan; Vaibhav Sahai; Matthew J. Schipper; Leslie A. Parsels; Joshua D. Parsels; Theresa Devasia; Mahmoud Al-Hawaray; Clifford S. Cho; Hari Nathan; et al.Jonathan MaybaumMark M. ZalupskiTheodore S. Lawrence Dose Escalation Trial of the Wee1 Inhibitor Adavosertib (AZD1775) in Combination With Gemcitabine and Radiation for Patients With Locally Advanced Pancreatic Cancer. Journal of Clinical Oncology 2019, 37, 2643-2650, 10.1200/jco.19.00730.
More
Information
Subjects:
Cell Biology
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.0K
Revisions:
3 times
(View History)
Update Date:
10 Aug 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





