
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Aldo Pagano | + 2205 word(s) | 2205 | 2021-07-02 11:35:49 | | | |
| 2 | Amina Yu | Meta information modification | 2205 | 2021-07-09 10:19:49 | | |
Video Upload Options
High-risk neuroblastoma (HR-NB) still remains the most dangerous tumor in early childhood. For this reason, the identification of new therapeutic approaches is of fundamental importance. Recently, we combined the conventional pharmacological approach to NB, represented by cisplatin, with fendiline hydrochloride, an inhibitor of several transporters involved in multidrug resistance of cancer cells, which demonstrated an enhancement of the ability of cisplatin to induce apoptosis. In this work, we co-administrated acetazolamide, a carbonic anhydrase isoform IX (CAIX) inhibitor which was reported to increase chemotherapy efficacy in various cancer types, to the cisplatin/fendiline approach in SKNBE2 xenografts in NOD-SCID mice with the aim of identifying a novel and more effective treatment. We observed that the combination of the three drugs increases more than twelvefold the differences in the cytotoxic activity of cisplatin alone, leading to a remarkable decrease of the expression of malignancy markers. Our conclusion is that this approach, based on three FDA-approved drugs, may constitute an appropriate improvement of the pharmacological approach to HR-NB.
1. Introduction
2. The Co-Administration of Acetazolamide with Cis/Fen Therapy Increased the Mice’s Survival and Inhibits Tumor Nodule Growth
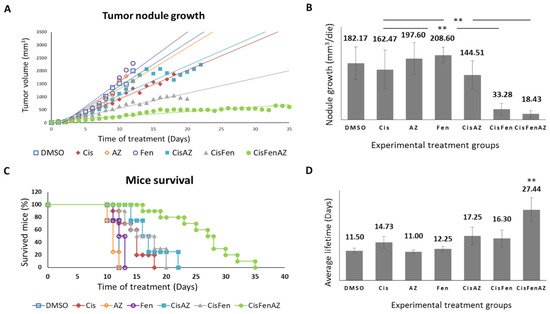
3. Acetazolamide in Combination with Cisplatin and Fendiline Hydrochloride Reduces the Expression of Malignancy Markers of NB Xenografts In Vivo
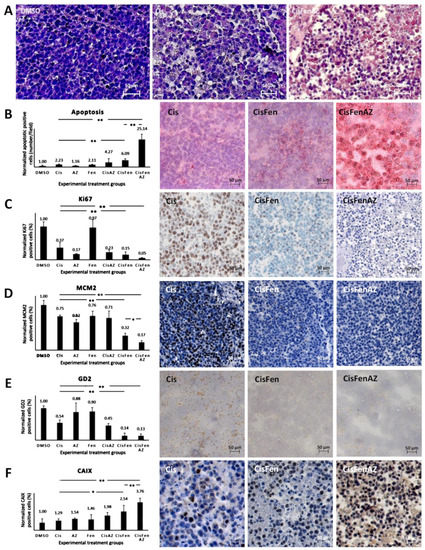
4. Discussion
References
- Maris, J.M. Recent Advances in Neuroblastoma. N. Engl. J. Med. 2010, 362, 2202–2211.
- Maris, J.M.; Hogarty, M.D.; Bagatell, R.; Cohn, S.L. Neuroblastoma. Lancet 2007, 369, 2106–2120.
- Whittle, S.B.; Smith, V.; Doherty, E.; Zhao, S.; McCarty, S.; Zage, P.E. Overview and recent advances in the treatment of neuroblastoma. Expert Rev. Anticancer Ther. 2017, 17, 369–386.
- Würth, R.; Thellung, S.; Bajetto, A.; Mazzanti, M.; Florio, T.; Barbieri, F. Drug-repositioning opportunities for cancer therapy: Novel molecular targets for known compounds. Drug Discov. Today 2016, 21, 190–199.
- Sidarovich, V.; De Mariano, M.; Aveic, S.; Pancher, M.; Adami, V.; Gatto, P.; Pizzini, S.; Pasini, L.; Croce, M.; Parodi, F.; et al. A high-content screening of anticancer compounds suggests the multiple tyrosine kinase inhibitor ponatinib for repurposing in neuroblastoma therapy. Mol. Cancer Ther. 2018, 17, 1405–1415.
- Vella, S.; Penna, I.; Longo, L.; Pioggia, G.; Garbati, P.; Florio, T.; Rossi, F.; Pagano, A. Perhexiline maleate enhances antitumor efficacy of cisplatin in neuroblastoma by inducing over-expression of NDM29 ncRNA. Sci. Rep. 2015, 5, 18144.
- Brizzolara, A.; Garbati, P.; Vella, S.; Calderoni, M.; Quattrone, A.; Tonini, G.P.; Capasso, M.; Longo, L.; Barbieri, R.; Florio, T.; et al. Co-Administration of Fendiline Hydrochloride Enhances Chemotherapeutic Efficacy of Cisplatin in Neuroblastoma Treatment. Molecules 2020, 25, 5234.
- Gavazzo, P.; Vella, S.; Marchetti, C.; Nizzari, M.; Cancedda, R.; Pagano, A. Acquisition of neuron-like electrophysiological properties in neuroblastoma cells by controlled expression of NDM29 ncRNA. J. Neurochem. 2011, 119, 989–1001.
- Giaginis, C.; Vgenopoulou, S.; Vielh, P.; Theocharis, S. MCM proteins as diagnostic and prognostic tumor markers in the clinical setting. Histol. Histopathol. 2010, 25, 351–370.
- Mujoo, K.; Cheresh, D.A.; Yang, H.M.; Reisfeld, R.A. Disialoganglioside GD2 on Human Neuroblastoma Cells: Target Antigen for Monoclonal Antibody-mediated Cytolysis and Suppression of Tumor Growth. Cancer Res. 1987, 47, 1098–1104.
- McFarland, B.C.; Benveniste, E.N. Reactive astrocytes foster brain metastases via STAT3 signaling. Ann. Transl. Med. 2019, 7, S83.
- Kamijo, T. Role of stemness-related molecules in neuroblastoma. Pediatr. Res. 2012, 71, 511–515.
- Cheung, N.K.V.; Heller, G. Chemotherapy dose intensity correlates strongly with response, median survival, and median progression-free survival in metastatic neuroblastoma. J. Clin. Oncol. 1991, 9, 1050–1058.
- Troncone, L.; Rufini, V.; Luzi, S.; Mastrangelo, R.; Riccardi, R. The treatment of neuroblastoma with [131I]MIBG at diagnosis. Q. J. Nucl. Med. 1995, 39, 65–68.
- Mastrangelo, S.; Tornesello, A.; Diociaiuti, L.; Pession, A.; Prete, A.; Rufini, V.; Troncone, L.; Mastrangelo, R. Treatment of advanced neuroblastoma: Feasibility and therapeutic potential of a novel approach combining 131-I-MIBG and multiple drug chemotherapy. Br. J. Cancer 2001, 84, 460–464.
- Kim, D.W.; Jo, Y.H.; Jee, H.K.; Wu, H.G.; Chae, S.R.; Chol, H.L.; Kim, T.Y.; Dae, S.H.; Bang, Y.J.; Noe, K.K. Neoadjuvant etoposide, ifosfamide, and cisplatin for the treatment of olfactory neuroblastoma. Cancer 2004, 101, 2257–2260.
- Norris, M.D.; Bordow, S.B.; Haber, P.S.; Marshall, G.M.; Kavallaris, M.; Madafiglio, J.; Cohn, S.L.; Salwen, H.; Schmidt, M.L.; Hipfner, D.R.; et al. Evidence that the MYCN oncogene regulates MRP gene expression in neuroblastoma. Eur. J. Cancer 1997, 33, 1911–1916.
- Casinelli, G.; LaRosa, J.; Sharma, M.; Cherok, E.; Banerjee, S.; Branca, M.; Edmunds, L.; Wang, Y.; Sims-Lucas, S.; Churley, L.; et al. N-Myc overexpression increases cisplatin resistance in neuroblastoma via deregulation of mitochondrial dynamics. Cell Death Discov. 2016, 2, 16082.
- Vella, S.; Conaldi, P.G.; Florio, T.; Pagano, A. PPAR Gamma in Neuroblastoma: The Translational Perspectives of Hypoglycemic Drugs. PPAR Res. 2016, 2016, 3038164.
- Costa, D.; Gigoni, A.; Würth, R.; Cancedda, R.; Florio, T.; Pagano, A. Metformin inhibition of neuroblastoma cell proliferation is differently modulated by cell differentiation induced by retinoic acid or overexpression of NDM29 non-coding RNA. Cancer Cell Int. 2014, 14, 59.
- Raghunand, N.; He, X.; Van Sluis, R.; Mahoney, B.; Baggett, B.; Taylor, C.W.; Paine-Murrieta, G.; Roe, D.; Bhujwalla, Z.M.; Gillies, R.J. Enhancement of chemotherapy by manipulation of tumour pH. Br. J. Cancer 1999, 80, 1005–1011.
- Ameis, H.M.; Drenckhan, A.; Freytag, M.; Izbicki, J.R.; Supuran, C.T.; Reinshagen, K.; Holland-Cunz, S.; Gros, S.J. Carbonic anhydrase IX correlates with survival and is a potential therapeutic target for neuroblastoma. J. Enzyme Inhib. Med. Chem. 2016, 31, 404–409.
- Supuran, C.T.; Briganti, F.; Tilli, S.; Chegwidden, W.R.; Scozzafava, A. Carbonic anhydrase inhibitors: Sulfonamides as antitumor agents? Bioorganic Med. Chem. 2001, 9, 703–714.
- Bolden, J.E.; Peart, M.J.; Johnstone, R.W. Anticancer activities of histone deacetylase inhibitors. Nat. Rev. Drug Discov. 2006, 5, 769–784.
- Bayat Mokhtari, R.; Baluch, N.; Ka Hon Tsui, M.; Kumar, S.; Homayouni, S.T.; Aitken, K.; Das, B.; Baruchel, S.; Yeger, H. Acetazolamide potentiates the anti-tumor potential of HDACi, MS-275, in neuroblastoma. BMC Cancer 2017, 17, 156.





