Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Sharon Provost | + 3278 word(s) | 3278 | 2021-04-27 05:54:28 | | | |
| 2 | Lily Guo | Meta information modification | 3278 | 2021-05-27 03:53:42 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Provost, S. Violence Prevention Education in Healthcare. Encyclopedia. Available online: https://encyclopedia.pub/entry/10144 (accessed on 25 May 2026).
Provost S. Violence Prevention Education in Healthcare. Encyclopedia. Available at: https://encyclopedia.pub/entry/10144. Accessed May 25, 2026.
Provost, Sharon. "Violence Prevention Education in Healthcare" Encyclopedia, https://encyclopedia.pub/entry/10144 (accessed May 25, 2026).
Provost, S. (2021, May 26). Violence Prevention Education in Healthcare. In Encyclopedia. https://encyclopedia.pub/entry/10144
Provost, Sharon. "Violence Prevention Education in Healthcare." Encyclopedia. Web. 26 May, 2021.
Copy Citation
Violence from patients and visitors towards healthcare workers is a serious international issue affecting the safety and health of workers, quality of care, and healthcare system sustainability. The main intervention is violence prevention (VP) education for healthcare workers. Both the healthcare environment and reasons for patient violence are complex, making it challenging to evaluate VP education using traditional methods. An alternative realist evaluation approach offers the ability to understand how, why and for whom VP education is effective to prevent violence and related injuries.
healthcare
patient violence
violence prevention
violence prevention education
1. Introduction
Occupational violence refers to abuse, threats, intimidation, or assault of individuals in the course of their work [1], and is commonly categorized according to the relationship between the perpetrator and worker [2]. There may be no relationship such as in the case of violence related to crime (type I), a client/provider relationship (type II), a peer or work relationship (type III), or a personal relationship such as domestic violence brought into the workplace (type IV) [2].
Although type II workplace violence exists in many industries, including law enforcement, education, and retail services, healthcare workers suffer proportionately more type II violence than workers in any other sector [3][4][5] and have the highest percentage of violence-related injury claims [6]. A recent meta-analysis from 30 studies found that one in four healthcare workers experience physical violence by patients or visitors every year [7]. As evidenced in studies and literature reviews, type II violence from clients, patients and long-term care residents towards healthcare staff such as nurses, doctors, and care aides is an increasing issue that affects the wellbeing of healthcare workers and their ability to provide care [8][9][10][11][12][13][14]. Violence towards healthcare workers is a documented concern not only in the authors’ jurisdiction [15][16][17], but across many countries, as acknowledged by international organizations [9][11][18].
Type II violence in healthcare can be physical, including kicking, hitting, biting, pushing, sexual assault, stabbing, and assault with a weapon, or psychological, such as threats of immediate or future physical force or attack and verbal abuse or harassment [18]. Multiple contexts influence the risk of violence towards healthcare workers, including physical environments, policies, characteristics of populations served, individual patient disease processes, the nature of the patient/caregiver interactions, and consumer frustration with system issues, such as wait times or restrictive policies [8][19][20][21][22]. In particular, healthcare workers in emergency departments, psychiatry, and residential (long-term care) areas have been documented as being at high risk for type II violence [23][24].
Measuring the prevalence of type II violence in healthcare is challenging, as violence is chronically underreported due in part to differing interpretations of what behaviours constitute violence [17][20] and to the normalization of violence as ‘just part of the job’ and not worth reporting [10][20]. A published review of prevalence studies reported that 22% to 90% of healthcare workers have experienced verbal abuse, 12% to 64% experienced threats of physical violence, and 2% to 32% have suffered an actual assault [21].
The predominant intervention to address type II violence in healthcare is violence prevention (VP), which is administered through programs that teach healthcare workers how to prevent, manage, and report violence [10][22][25][26][27]. The curriculum of VP programs typically includes instruction on communication skills and de-escalation of aggression, and some programs also focus on defining and assessing the risk of violence, emotional self-management, and self-defense [20][28][29][30]. Delivery of VP education can involve online modules, classroom training sessions, or a hybrid of both, and can vary in length from one hour to multiple days [22][27][30][31]. As such, although VP education is extensively used as an intervention to address type II violence in healthcare, its content, context, and method of delivery vary widely.
Despite the frequency of its use, determining the overall effectiveness of violence prevention education has been challenging [21][22]. Changes in violence incidence rates may represent effects of the education, external factors, new patterns of reporting, or a combination of all three [21]. Traditional reviews of VP program evaluations are generally inconclusive regarding the efficacy of these programs, citing the variety of content across programs, underreporting of violence, and complexity of healthcare settings as major barriers [22][27][32][33][34]. To address some of these challenges, this review utilizes a realist approach, a method gaining in popularity that helps to synthesize evidence from the literature to provide findings and recommendations that are practical and useful for healthcare providers and administrators—the intended audience.
Developed in the United Kingdom by Pawson and Tilley [35], a realist review offers the ability to provide insights into the effectiveness of a program in ways that systematic or narrative reviews typically cannot: by utilizing information from existing literature to explore how and why interventions involving human behaviour succeed or fail [36]. Educational programs such as violence prevention which aim to change participant attitudes and actions are designed with an underlying theory of how participants will learn and apply the content [37]. Unlike a typical literature review that summarizes or synthesizes findings from different studies, a realist approach begins with a theory of how an intervention is intended to work and then seeks information from a wide range of literature to support, refine, or refute that initial theory [38]. The resulting program theory is described using realist explanations, known as context-mechanism-outcome (CMO) configurations “that spell out the relationship between particular features of context, particular mechanisms and particular outcomes” [39] (p. 13). As illustrated in the findings of this review, it is the context—such as the type of educational content or the format of delivery—which is necessary to trigger an underlying mechanism (e.g., participant’s confidence) that leads to intended outcomes (e.g., the application of VP skills). The realist approach is useful to policymakers who want to know what contextual factors are most likely to produce their desired outcomes, particularly with complex social and healthcare programs, where many interventions are possible [38] (further definitions are available in the Supplementary Materials: Table S1: Glossary of terms).
2. CMO Explanations 1–6: Decreasing Violent Incidents
Six CMO explanations contribute to decreasing violent incidents: VP education specific to clinical settings, content focused on communication, unit-level mentoring, team-based education and discussions, workload enabling meeting patient needs, and sufficient physical/emotional energy. (Figure 1).
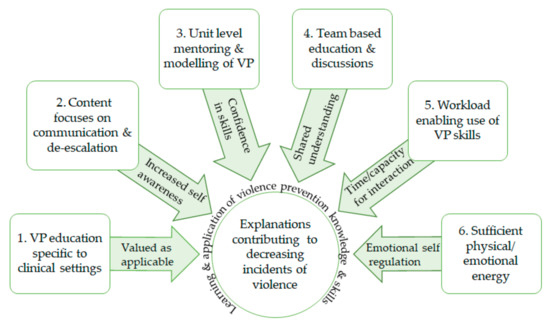
Figure 1. Context-mechanism-outcomes (CMOs) 1–6: explanations decreasing violent incidents. VP: violence prevention.
2.1. CMO 1: VP Education Specific to Clinical Settings
When content is specific to participants’ clinical settings (C), they are more likely to value (M) the education as applicable and engage in learning (O).
Valuing education as applicable involves two contextual factors: the content taught and—to a lesser degree—by whom. Participants perceive education as worth their attention when the content is specific to their clinical practice setting and content cases or examples reflect the workplace violence they experience. Additionally, when facilitators or trainers provide examples from their own clinical experiences with workplace violence, participants value the content and see it as more applicable.
“Participants in the workplace violence program were taught information that was directly applicable to their work environment. The tabletop exercise provided contextual meaning by using video case studies that were both realistic and applicable to the environment in which the acquired knowledge would be applied”[40] (p. 471)
“…ward specific training may address these limitations by facilitating the transfer of knowledge to practice, developing skills identifying problems and implementing prevention strategies”[41] (p. 7)
“Someone who teaches aggression management should be on the wards to get the feel of what actually happens’ (Ward security staff member). ‘Have the trainer experience the ward environment and apply the program to the situations on the ward’ (Nursing staff member)”[42] (p. 237)
2.2. CMO 2: Content Focuses on Communication and De-Escalation
When education focuses on communication and de-escalation skills (C), participants have increased self-awareness (M) and are more likely to use a VP approach to prevent escalation and violence (O).
VP education that focuses training on effective communication and de-escalation skills increases participants’ awareness of how their own emotions and approach in interactions with patients can influence the risk of violence. When participants are more self-aware, they are more likely to use communication and de-escalation skills, which may prevent violence. Participants’ focus on prevention may be diminished when training sessions introduce self-protection ‘break away’ maneuvers: ways in which healthcare workers can free themselves more easily if their arm, hair, or clothes are grabbed by patients. Although break-away techniques may provide a temporary sense of confidence in managing violence, studies indicate that limited or brief training in these methods is less effective, with few individuals utilizing these types of skills in practice [43][44].
“Direct skills teaching [provides] knowledge of behavioural skills and strategies for emotional regulation [leading to] increased confidence/self-efficacy [and] enhanced interpersonal style when managing aggressive behaviour [and] emotional regulation when faced with aggressive behaviour”[33] (p. 237)
“Crucially, training needs to help staff understand how problems, such as CB [challenging behaviour], can arise within and as a result of their routine interactions with clients”[45] (p. 237)
“…training helped them control their temperament in a challenging environment and also enabled them to effectively practice active listening and empathy”[46] (p. 297)
“…training interventions that enhance staff communication skills do decrease violent incident rates”[27] (p. 2828)
2.3. CMO 3: Unit Level Mentoring and Modeling of VP
Unit level mentoring and modelling of VP (C) increases confidence (M), resulting in increased use of VP approaches (O).
Participants’ attainment of knowledge and skills from VP education is influenced by their educational experience and by how their learning is reinforced and supported in their workplace. When participants see role modelling of VP skills and have access to expert advice and mentoring, they have more confidence to apply VP knowledge and skills in their practice.
“It is recommended that early contact is made with clinical experts when high-risk patients are first identified, rather than following an incident, and that key ward staff are trained and mentored to develop confidence in managing patients with a risk for violence/aggression”[41] (p. 13)
“Experienced workers can mentor and guide less experienced colleagues in communication and care delivery strategies that may calm patients and visitors, diffuse tense situations”[47] (pp. 182–183)
“Because of the sometimes impromptu nature of violence, consequent debriefing and the sensitivities involved, a change agent from within the clinical team may have been more successful as an internal ‘implementer’ working with peers”[48] (p. 12)
2.4. CMO 4: Team-Based Education and Discussions
Team-based VP education, reinforced with regular team discussions of violence incidents (C), increases teams’ shared understanding (M), supporting a consistent approach to prevent and manage violence (O).
Violence prevention activities that foster team interaction increase the team’s ability to respond effectively as a unit to situations of potential violence. Training as a team and learning from team-based discussions about violence and debriefing of incidents increases participants’ shared knowledge, optimizing consistent approaches to workplace violence [49].
“Wards adopting a whole-team approach are more likely to reduce the risk of assault than individual advances in knowledge and skills… Clinical managers should not only ensure that sufficient numbers of their staff are trained, but also that as many staff as possible are trained together at the same time, to foster such approaches and facilitate maximal gain”[33] (p. 453)
“Interventions to support nurses and nursing teams in processing transgressive behaviour in care relationships should be implemented on a team level, incorporating the culture of the ward and the dynamics of teams”[50] (p. 2381)
“Participants in the intervention group of a structured program for regular discussion of workplace violent incidents reported an improved awareness and management skills”[10] (p. 21)
2.5. CMO 5: Workload Enabling the Use of VP Skills
When workload enables sufficient time with patients (C), participants have the opportunity to apply VP knowledge and skills (M), decreasing the risk of violence.
A limiting factor in the application of violence prevention knowledge and skills is the availability of healthcare workers; time and workload capacity. When workload is reasonable, workers have the required time with patients to interact and communicate, observe behaviour, and apply VP knowledge and skills that prevent or de-escalate aggressive behaviours.
“Most ED RNs thought that the classes they were forced to take were not effective or had little efficacy in successfully de-escalating patient behaviours. Most ED RNs cited a lack of time to implement the tools taught in these classes”[51] (p. 549)
“Staff members also identified barriers that sometimes prevented their managing behaviour problems optimally. These included time pressure”[52] (p. 38)
“Training alone is not enough and staff need to be enabled to learn with adequate support and resources e.g., … reasonable workload to apply skills and communicate with patients or residents”[53] (p. 20)
2.6. CMO 6: Sufficient Physical/Emotional Energy
When healthcare workers have sufficient physical and emotional energy (C), they have an increased ability to self-regulate their emotions (M) and use VP approaches (O).
An individual healthcare worker’s physical and emotional state affects their ability to self-regulate their emotions and behaviours. Individuals who are stressed by personal life factors, poor working relationships with peers or supervisors, or from dealing with frequent violence, are less able to self-regulate and prevent violence.
“Participants are more able to apply skills when they are fresh and have energy early in their shift but when they are tired and nerves are frayed they resort to previous behaviour”[51] (p. 550)
“The high levels of physical, verbal and sexual violence combined with the structural violence of caring in an understaffed and under-resourced environment stretches workers to the limit. Personal support workers leave physically and mentally exhausted”[53] (p. 21)
3. CMO Explanations 7–10: Decreasing Injuries from Violence
Four CMO explanations were identified that contribute to decreasing physical and psychological injuries for healthcare workers: support during violence, support after a violent incident, clear and supported violence policies, and a nonjudgmental and blame-free work culture. (Figure 2)
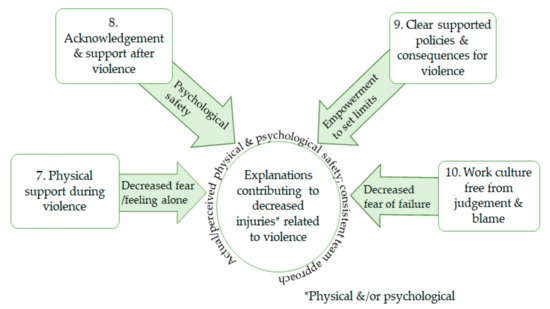
Figure 2. CMOs 7–10: explanations decreasing worker injury from violence.
3.1. CMO 7: Physical Support during Violence
Physical support from supervisors and peers during violence (C) decreases fear and feelings of being alone (M), increasing actual or perceived physical safety (O).
Experiencing verbal and physical violence from patients can be traumatic and create fear for personal safety at work. When healthcare workers can rely on peers and supervisors to be physically present and available to provide support during an incident of violence, they have less fear for their physical safety and feel less alone.
“’It feels great to have support at times like these. It helps me feel like I am not alone when these situations occur and that someone has my back’”[54] (p. 125)
“A sense of abandonment underlay accounts where a physical absence of support staff and managers on the wards meant that staff ‘often felt totally alone in a difficult and dangerous situation’”[55] (p. 5)
“The RN who steps in and either takes over for an RN who is experiencing a challenging patient or intervenes for another nurse who might be newer or more timid… ‘ We have a couple of nurses who just stand up, you know, for the weaker nurses who can get picked on by certain patients. They will just slip in and take over the assignment or whatever they can do to help, but in a positive way’”[51] (p. 552)
3.2. CMO 8: Acknowledgement and Support after Violence
When individuals receive acknowledgement and non-blaming emotional support from supervisors and peers after violence (C), they feel psychologically safer (M) and have less psychological injury from the violence (O).
When health care workers receive acknowledgement that violence occurred and feel supported instead of blamed by peers and leaders, they perceive the workplace as psychologically safe and are less likely to feel emotionally traumatized. Consistent with trauma experienced by victims of non-occupational violence [56], when a healthcare worker does not receive the support they expect, they may experience a secondary psychological trauma, potentially more damaging than the trauma from the violent event.
“More importantly nurses in the study felt most supported when the manager acknowledged the event as explained by this RN, ‘just having the event recognized as something that was critical and you know, it was traumatic and …they weren’t minimizing it and actually embracing it as something that was not acceptable’”[57] (p. 7)
“The nature of the organisational response to the traumatised staff member can therefore play a pivotal role in the process of recovery and, where the organisational response fails to understand or consider the needs of the victim(s) can itself constitute a source of secondary injury or trauma”[58] (p. 481)
“Participants actively looked toward their colleagues and managers for support and acknowledgment following client violence in the workplace, and indeed having supportive peers and supervisors can significantly improve a victim’s sense of coping and lessen their fear of further attacks”[59] (p. 293)
“Many other nurses described feeling very angry, unsupported and blamed by their managers. Some RNs never heard from their managers following events of patient violence, while others described receiving a phone call or a brief conversation, which was felt to be thoughtful, but not sufficiently supportive”[57] (p. 7)
3.3. CMO 9: Clear, Supported Policies and Consequences for Violence
Clear, supported policies with consequences for violence (C) empowers healthcare workers to set limits (M), resulting in a greater ability to manage aggression and violence (O).
When policies relating to violence are clear, visibly supported by leaders and include reasonable consequences for violent behaviours from patients and visitors, healthcare workers feel empowered to set limits and enact policies to manage aggression, resulting in a more consistent approach and decreased risk for injury.
“Organizational factors like clear expectations for patient behaviour and consequences empower management and staff members to feel less frustrated and more equipped to deal with violence”[51] (p. 549)
“Zero tolerance policy enforcement is thought to be constructive in terms of supporting and empowering staff to have confidence in managing problematic patients and hostile situations”[60] (p. 97)
“An organization that positively addresses violence through the themes of consistency, consequences, and collaboration potentially mitigates the development of cynicism and conflict as maladaptive reactions of staff”[61] (p. 15)
3.4. CMO 10: Work Culture Free from Judgement
When the work culture is free from shame and blame (C), healthcare workers have less fear of failure and of being perceived as incompetent (M) and are more likely to apply new knowledge and skills to effectively prevent or manage violence (O).
A supportive unit culture where healthcare workers are not blamed or judged for errors decreases their fear of being perceived as incompetent and increases confidence to try new skills and report incidents that have occurred.
“Staff may feel less confident in taking the risk to apply new skills if they fear that their image may be harmed and they are seen as ignorant or incompetent”[49] (p. 2)
“Nurses are reluctant to report violence in the workplace and may not seek support after incidents of violence because they think asking for help may be interpreted as personal weakness or professional failure”[62] (p. 45)
“When admitting (or simply calling attention to) mistakes, asking for help, or accepting the high probability of failure that comes with experimenting, people risk being seen as incompetent, whether in a narrow, particular domain, or more broadly. Reluctance to take such interpersonal risks can create physical risks in high-risk industries”[49] (p. 256)
4. CMO Explanation 11: Increasing Reporting
The final CMO explanation relates to how the actions that are taken by leaders after violence influences whether staff will formally report future violence (Figure 3).
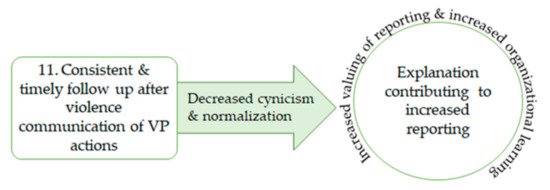
Figure 3. CMO 11: explanation increasing reporting.
CMO 11: Follow up after Violence
When leaders provide consistent, timely follow-up and action to prevent further violent incidents (C), healthcare workers are less likely to perceive violence as normal (M) and are more likely to formally report violent incidents (O).
“When staff do not see any result or change as a consequence of reporting violence when experience violence they feel hopeless and resigned that reporting is of no benefit and will not report”[63] (p. 271)
“Registration of violent incidents without regularly scheduled, structured feedback discussions may have increased frustration in the control group, leading to less likelihood of reporting”[64] (p. 674)
“Recordkeeping was rated as the second lowest subcomponent in terms of importance in reducing WPV. This finding may be related to employees not recognizing any benefit of recordkeeping as a form of WPV prevention”[65] (p. 381)
References
- Canadian Centre for Occupational Health and Safety, “Violence in the Workplace: OSH Answers”. 2019. Available online: (accessed on 22 January 2020).
- National Institute for Occupational Safety and Health, “NIOSH-WPVHC-Workplace Violence Types,” Workplace Violence Prevention for Nurses. 2013. Available online: (accessed on 7 October 2017).
- Milczarek, M. Workplace Violence and Harassment: A European Picture; European Risk Observatory Report; European Agency for Safety and Health at Work Luxembourg Publications Office of the European Union: Bilboa, Spain, 2010.
- Occupational Safety and Health Administration (OSHA). Guidelines for Preventing Workplace Violence for Healthcare and Social Services Workers; Report 3148-06R; US Department of Labor: Washington, DC, USA, 2016.
- Canadian Centre for Occupational Health and Safety. Violence in the Workplace, OSH Answers. 2018. Available online: (accessed on 4 January 2018).
- WorkSafeBC, 2015 Statistics. 2016. Available online: (accessed on 30 September 2017).
- Li, Y.L.; Li, R.Q.; Qiu, D.; Xiao, S.Y. Prevalence of workplace physical violence against health care professionals by patients and visitors: A systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2020, 17, 299.
- Edward, K.-L.; Stephenson, J.; Ousey, K.; Lui, S.; Warelow, P.; Giandinoto, J.-A. A systematic review and meta-analysis of factors that relate to aggression perpetrated against nurses by patients/relatives or staff. J. Clin. Nurs. 2015, 25, 289–299.
- International Council of Nurses. Position Statement: Prevention and Management of Workplace Violence; Joint Programme on Workplace Violence in the Health Sector: Geneva, Switzerland, 2017.
- Wang, S.; Hayes, L.; O’Brien-Pallas, L. A Review and Evaluation of Workplace Violence Prevention Programs in the Health Sector; Nursing Health Services Research Unit: Toronto, ON, Canada, 2008.
- WHO. Violence against health workers. Violence and Injury Prevention. 2018. Available online: (accessed on 12 March 2021).
- Speroni, K.G.; Fitch, T.; Dawson, E.; Dugan, L.; Atherton, M. Incidence and Cost of Nurse Workplace Violence Perpetrated by Hospital Patients or Patient Visitors. J. Emerg. Nurs. 2014, 40, 218–228.
- Liu, J.; Gan, Y.; Jiang, H.; Li, L.; Dwyer, R.; Lu, K.; Yan, S.; Sampson, O.; Xu, H.; Wang, C.; et al. Prevalence of workplace violence against healthcare workers: A systematic review and meta-analysis. Occup. Environ. Med. 2019, 76, 927–937.
- Adedokun, M. Workplace Violence in the Healthcare Sector A Review of the Literature; Malmö University: Malmö, Sweden, 2020.
- Havaei, F.; Astivia, O.L.O.; Macphee, M. The impact of workplace violence on medical-surgical nurses’ health outcome: A moderated mediation model of work environment conditions and burnout using secondary data. Int. J. Nurs. Stud. 2020, 109, 103666.
- Duncan, S.M.; Hyndman, K.; A Estabrooks, C.; Hesketh, K.; Humphrey, C.K.; Wong, J.S.; Acorn, S.; Giovannetti, P. Nurses’ experience of violence in Alberta and British Columbia hospitals. Can. J. Nurs. Res. 2001, 32, 57–78.
- Hesketh, K.L.; Duncan, S.M.; A Estabrooks, C.; A Reimer, M.; Giovannetti, P.; Hyndman, K.; Acorn, S. Workplace violence in Alberta and British Columbia hospitals. Health Policy 2003, 63, 311–321.
- ILO; ICN; WHO; PSI. Framework Guidelines for Addressing Workplace Violence in the Health Sector; Joint Programme on Workplace Violence in the Health Sector: Geneva, Switzerland, 2002.
- Gates, D.M.; Ross, C.S.; McQueen, L. Violence against emergency department workers. J. Emerg. Med. 2006, 31, 331–337.
- Lipscomb, J.; London, M. Not Part of the Job: How to Take a Stand Against Violence in the Work Setting; American Nurses Association: Silver Spring, MD, USA, 2015.
- Pompeii, L.; Dement, J.; Schoenfisch, A.; Lavery, A.; Souder, M.; Smith, C.; Lipscomb, H. Perpetrator, worker and workplace characteristics associated with patient and visitor perpetrated violence (Type II) on hospital workers: A review of the literature and existing occupational injury data. J. Saf. Res. 2013, 44, 57–64.
- Wassell, J.T. Workplace violence intervention effectiveness: A systematic literature review. Saf. Sci. 2009, 47, 1049–1055.
- Gerberich, S.G.; Church, T.R.; McGovern, P.M.; Hansen, H.; Nachreiner, N.M.; Geisser, M.S.; Ryan, A.D.; Mongin, S.J.; Watt, G.D.; Jurek, A. Risk Factors for Work-Related Assaults on Nurses. Epidemiology 2005, 16, 704–709.
- Casey, B. Violence facing health care workers in Canada: Report of the Standing Committee on Health; House of Commons Standing Committee on Health: Ottawa, ON, Canada, 2019.
- Morrison, E.F.; Love, C.C. An evaluation of four programs for the management of aggression in psychiatric settings. Arch. Psychiatr. Nurs. 2003, 17, 146–155.
- Vladutiu, C.J.; Casteel, C.; Nocera, M.; Harrison, R.; Peek-Asa, C. Characteristics of workplace violence prevention training and violent events among home health and hospice care providers. Am. J. Ind. Med. 2015, 59, 23–30.
- Tölli, S.; Partanen, P.; Kontio, R.; Häggman-Laitila, A. A quantitative systematic review of the effects of training interventions on enhancing the competence of nursing staff in managing challenging patient behaviour. J. Adv. Nurs. 2017, 73, 2817–2831.
- Kynoch, K.; Wu, C.-J.; Chang, A.M. Interventions for Preventing and Managing Aggressive Patients Admitted to an Acute Hospital Setting: A Systematic Review. Worldviews Evidence-Based Nurs. 2010, 8, 76–86.
- Health Employers Association of BC, Violence Prevention. Available online: (accessed on 5 September 2017).
- Forster, A.J.; Petty, M.T.; Schleiger, C.; Walters, H.C. kNOw workplace violence: Developing programs for managing the risk of aggression in the health care setting. Med. J. Aust. 2005, 183, 357–361.
- Beech, B.; Leather, P. Workplace violence in the health care sector: A review of staff training and integration of training evaluation models. Aggress. Violent Behav. 2006, 11, 27–43.
- Beech, B.; Leather, P. Evaluating a management of aggression unit for student nurses. J. Adv. Nurs. 2003, 44, 603–612.
- Price, O.; Baker, J.; Bee, P.; Lovell, K. Learning and performance outcomes of mental health staff training in de-escalation techniques for the management of violence and aggression. Br. J. Psychiatry 2015, 206, 447–455.
- Kannampallil, T.G.; Schauer, G.F.; Cohen, T.; Patel, V.L. Considering complexity in healthcare systems. J. Biomed. Informatics 2011, 44, 943–947.
- Clarke, A.; Pawson, R.; Tilley, N. Realistic Evaluation. Br. J. Sociol. 1998, 49, 331.
- Pawson, R. Evidence-Based Policy: A Realist Perspective; SAGE: London, UK, 2006.
- Pawson, R.; Greenhalgh, T.; Harvey, G.; Walshe, K. Realist synthesis: An introduction; University of Manchester: Manchester, UK, 2004.
- Wong, G.; Greenhalgh, T.; Westhorp, G.; Pawson, R.; The RAMESES Project. Quality standards for realist synthesis (for researchers and peer-reviewers). 2014. Available online: (accessed on 12 March 2021).
- Wong, G.; Westhorp, G.; Pawson, R.; Greenhalgh, T. Realist Synthesis. RAMESES Training Materials; RAMESES PROJECT: London, UK, 2013; p. 55.
- Gillespie, G.L.; Farra, S.L.; Gates, D.M. A workplace violence educational program: A repeated measures study. Nurse Educ. Pr. 2014, 14, 468–472.
- Adams, J.; Knowles, A.; Irons, G.; Roddy, A.; Ashworth, J. Assessing the effectiveness of clinical education to reduce the frequency and recurrence of workplace violence. Aust. J. Adv. Nurs. 2017, 34, 6–15.
- Ilkiw-Lavalle, O.; Grenyer, B.F.S.; Graham, L. Does prior training and staff occupation influence knowledge acquisition from an aggression management training program? Int. J. Ment. Health Nurs. 2002, 11, 233–239.
- Duffin, C. Researchers question the effectiveness of training staff in breakaway techniques. Ment. Health Pr. 2010, 13, 8.
- Dickens, G.; Rogers, G.; Rooney, C.; Mc Guinness, A.; Doyle, D. An audit of the use of breakaway techniques in a large psychiatric hospital: A replication study. J. Psychiatr. Ment. Health Nurs. 2009, 16, 777–783.
- A Farrell, G.; Salmon, P. Challenging behaviour: An action plan for education and training. Contemp. Nurse 2010, 34, 110–118.
- Baig, L.A.; Tanzil, S.; Shaikh, S.; Hashmi, I.; Khan, M.A.; Polkowski, M. Effectiveness of training on de-escalation of violence and management of aggressive behavior faced by health care providers in a public sector hospital of Karachi. Pak. J. Med Sci. 2018, 34, 294–299.
- Gillespie, G.L.; Gates, D.M.; Miller, M.; Howard, P.K. Workplace Violence in Healthcare Settings: Risk Factors and Protective Strategies. Rehabil. Nurs. 2010, 35, 177–184.
- MacGabhann, L.; Baker, S.; Dixon, P. Prevention and management of violence: Implementing clinically effective practice. Ment. Health Pr. 2002, 6, 8–13.
- Edmondson, A.C. Managing the Risk of Learning: Psychological Safety in Work Teams. In International Handbook of Organizational Teamwork and Cooperative Working; Wiley: Hoboken, NJ, USA, 2008; pp. 255–275.
- Vandecasteele, T.; Van Hecke, A.; Duprez, V.; Beeckman, D.; Debyser, B.; Grypdonck, M.; Verhaeghe, S. The influence of team members on nurses’ perceptions of transgressive behaviour in care relationships: A qualitative study. J. Adv. Nurs. 2017, 73, 2373–2384.
- Child, R.J.H.; Sussman, E.J. Occupational Disappointment: Why Did I Even Become a Nurse? J. Emerg. Nurs. 2017, 43, 545–552.
- Cassidy, E.L.; Rosen, C.; Walker, S.; Krinsky, A.; Kuhlman, G.; Wilson, D.; Solano, N.; Sheikh, J.I. Assessment to intervention: Utilizing a staff needs assessment to improve care for behaviorally challenging residents in long term care (Part II). Clin. Gerontol. 2005, 28, 29–42.
- Banerjee, A.; Daly, T.; Armstrong, H.; Armstrong, P.; Lafrance, S.; Szebehely, M. Out of Control; Violence against Personal Support Workers in Long-Term Care; York University: Toronto, ON, USA, 2008.
- Henderson, L.; Kamp, B.; Niedbalski, K.; Abraham, S.P.; Gillum, D.R. Nurses’ Perspectives on Patient and Visitor Violence: A Qualitative Study. Int. J. Stud. Nurs. 2018, 3, 117.
- Ashton, R.A.; Morris, L.; Smith, I.C. A qualitative meta-synthesis of emergency department staff experiences of violence and aggression. Int. Emerg. Nurs. 2018, 39, 13–19.
- National Center for Victims of Crime, “Trauma of Victimization,” Get Help Bulletins for Crime Victims. 2008. Available online: (accessed on 5 February 2020).
- Stevenson, K.N.; Jack, S.M.; O’Mara, L.; Legris, J. Registered nurses’ experiences of patient violence on acute care psychiatric inpatient units: An interpretive descriptive study. BMC Nurs. 2015, 14, 1–13.
- Paterson, B.; Leadbetter, D.; Bowie, V. Supporting nursing staff exposed to violence at work. Int. J. Nurs. Stud. 1999, 36, 479–486.
- Jussab, F.; Muiphy, H. I Just Can’t, I Am Frightened for My Safety, I Don’t Know How to Work With Her’: Practitioners’ Experiences of Client Violence and Recommendations for Future Practice. Prof. Psychol. Res. Pract. 2015, 46, 287–297.
- Bond, P.; Paniagua, H.; Thompson, A. Zero tolerance of violent patients: Policy in action. Pr. Nurs. 2009, 20, 97–99.
- Renker, P.; Scribner, S.A.; Huff, P. Staff perspectives of violence in the emergency department: Appeals for consequences, collaboration, and consistency. Work 2015, 51, 5–18.
- Allen, D.E.; de Nesnera, A.; Cummings, K.; Darling, F.E. Transforming the Culture of Caring Getting Hurt Is Not Part of the Job. J. Psychosoc. Nurs. 2011, 49, 45–49.
- Pich, J.; Hazelton, M.; Sundin, D.; Kable, A. Patient-related violence against emergency department nurses. Nurs. Health Sci. 2010, 12, 268–274.
- Arnetz, J.E.; Arnetz, B.B. Implementation and evaluation of a practical intervention programme for dealing with violence towards health care workers. J. Adv. Nurs. 2000, 31, 668–680.
- Gillespie, G.L.; Gates, D.M.; Mentzel, T.; Al-Natour, A.; Kowalenko, T. Evaluation of a Comprehensive ED Violence Prevention Program. J. Emerg. Nurs. 2013, 39, 376–383.
More
Information
Subjects:
Health Care Sciences & Services
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.2K
Revisions:
2 times
(View History)
Update Date:
27 May 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





