Personalized medicine is an emerging field that seeks to tailor the treatment of individual patients based on their clinical characteristics, biomarkers, genetics, and other factors
[1][2]. Other factors include specific comorbidities, complications, and patient background. To date, personalized medicine in Parkinson’s disease (PD) has not been fully realized due to barriers such as cost and genetic counseling although personalized medicine is used in PD patients in clinical settings when treatments are tailored based on motor and non-motor features
[3][4][5][6][7].
PD is a heterogeneous disorder in which motor and non-motor features of varying types and degrees may appear quite separately in individuals
[1][8]. Indeed, the etiology and pathogenesis of PD include a mixture of factors without any diagnostically reliable biomarkers; therefore, the diagnosis of PD is still based on a clinical assessment
[9][10]. It is known that the prognosis of PD differs between clinical types, with tremor-dominant types progressing slower than postural instability gait difficulty (PIGD) types
[11]. The Parkinson’s Progression Markers Initiative (PPMI) clinical study has revealed more detailed subtypes of PD
[12]. The authors classified PD into mild motor-predominant, intermediate, and diffuse malignant types
[12]. Several studies have been undertaken to address and detect possible biomarkers, which may predict the progression of individual PD patients
[13].
Historically, the first PD treatments involved a surgical approach. In 1952, Narabayashi et al. performed the world’s first pallidotomy for PD patients and described its positive effect
[14]. In the early 1960s, L-dopa therapy was initiated, but initially, low doses failed to show efficacy in many PD patients; Cotzias then initiated the use of high-dose therapy, and the modern regimen for L-dopa therapy was established
[15]. L-dopa is still the gold standard, and its combination with dopamine agonist, monoamine oxidase type B inhibitor, catechol-O-methyltransferase inhibitor and/or non-dopaminergic medication has been used to treat L-dopa related motor and non-motor complications for many years. However, in the advanced stage, despite adjustments to these medications, it is impossible to manage these complications, and finally surgical intervention is required in some patients. The use of stereotactic neurosurgery declined with the introduction of the drug L-dopa as an effective oral medication; but stereotactic neurosurgery was revived when it was shown to be effective in treating motor complications including wearing-off and dyskinesia
[16][17]. Later, deep brain stimulation (DBS) was introduced, and became the gold standard of treatment for advanced PD motor features
[18]. Today, various advanced treatments such as DBS, radiofrequency, MR–guided focused ultrasound (MRgFUS), gamma knife, levodopa-carbidopa intestinal gel (LCIG), and apomorphine are available, although the availability of treatments varies depending on country and region. Clinical practice guidelines for early treatment of PD have been published in various countries and are often recommended by experts
[19][20][21]. Standard pharmacological and non-pharmacological treatments are required during treatment, and the need for personalized medicine becomes more obvious when aiming to achieve an appropriate symptomatic and disease-modifying treatment with the right dose, right time, and minimum side effects in a specific patient. On the other hand, guidelines for the treatment of advanced PD have not been established, and in particular, the indication criteria and exclusion criteria for device-aided therapy have not been clarified. DBS and LCIG are the most established treatments for advanced stage PD in recent years, apomorphine subcutaneous infusion and MRgFUS have also become available, and efforts to incorporate them into personalized medicine will become important in the future. This review focuses on the advanced treatment of PD including cell therapy and gene therapy. Furthermore, we discuss aspects of personalized medicine that are currently available for the advanced treatment of PD.
2. Evaluation of the Efficacy of Advanced Treatment
Since there are no disease-modifying treatments for PD, the current goal of PD treatment is to improve patient and caregiver satisfaction. Physicians may tend to focus on the improvement rate of MDS UPDRS Part Three scores when evaluating the effectiveness of advanced treatment. However, the possibility of a gap between physician evaluation of surgical treatment effectiveness and patient and caregiver satisfaction should be noted; despite this, few studies have examined patient satisfaction with advanced treatment for PD
[22]. A large multicenter study of PD patients showed that MDS UPDRS Parts One and Two affect their quality of life (QOL)
[23]. Although the short-form PDQ-8 and the PDQ-39 have been used in many studies
[23][24][25], MDS UPDRS Parts One and Two, the patient reported outcome (PRO)-based assessments of patients’ activities of daily living (ADL), is also useful in the assessment of advanced treatment. Regarding non-motor features, the Non-Motor Symptoms Scale for Parkinson’s Disease (NMSS), the Non-Motor Symptoms Questionnaire (NMSQ), and MDS Non-Motor Rating Scale (MDS-NMS) may be useful for evaluating end points of advanced treatment. Furthermore, it is expected that outcomes assessed by caregivers
[26] will also be used to judge the effectiveness of advanced treatment of PD.
3. Team Approach
Organization of multidisciplinary clinical care teams is recommended in PD treatment
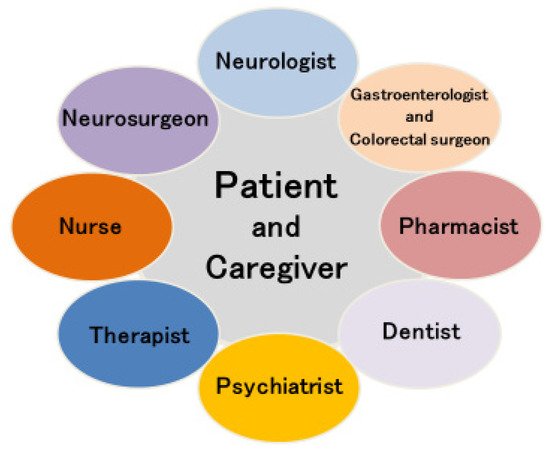
[27], and a team approach is essential for the realization of personalized medicine for advanced treatment in PD patients. An example of a team approach to advanced treatment of PD, particularly LCIG and stereotactic neurosurgery, is presented in
Figure 1. Neurologists take a lead in determining treatment plans, but neurosurgeons are responsible for stereotactic neurosurgery, and gastroenterologists and colorectal surgeons are responsible for LCIG. Furthermore, psychiatrists are important in the evaluation and treatment of psychiatric symptoms, and dentists are needed to evaluate and care for dysphagia which is frequently seen in PD. Therapists play an important role in sustained rehabilitation, and assessment of ADL requires cooperation with therapists. The presence of a nurse is important for assessment of the patient’s background, and PD nurses
[27] are indispensable during the long process of advanced treatment. Caregivers as well as patients require nursing care. Pharmacist medication guidance is also important for the continuous treatment of various drugs. Higuchi et al. reveals that screening through the use of a team approach may be useful for more than just patient selection of DBS
[28].
Supplementary Table S4 (DBS) and
Table S5 (LCIG) show concerns from a multidisciplinary perspective in determining indications for advanced treatment of PD patients. Since any advanced treatment is invasive, patients may expect notable effects of such treatment in return, which may lead to reduced patient satisfaction
[29]. Multidisciplinary informed consent is needed from patients and caregivers when advanced treatment is indicated. The above-mentioned improvement in QOL following cell therapy using iPSCs
[30] may also benefit patient satisfaction with a team approach. Moreover, a team approach will be increasingly necessary in the implementation of cell therapy and gene therapy, which are expected to become more widespread in the near future.
Figure 1. Team approach of advanced treatment for Parkinson’s disease.
A team approach also enables a tailored treatment plan for each patient based on patient-specific risks versus benefit analyses, accessibility to the center, supportive care circumstances, and cultural background. For example, surgical procedures requiring general anesthesia are contraindicated in patients with severe cardiopulmonary risks. Living in a remote area or poor supportive care circumstances may jeopardize LCIG, which requires daily medication renewal. Concerning cultural background, some patients may have a stigma against the use of devices, and in such cases lesion therapy and/or cell therapy may be a suitable option. Additionally, select patients may benefit from a combination of multiple treatment modalities (e.g., unilateral DBS and contralateral RF lesioning). We consider that a team approach at an experienced center would maximize the benefit of tailor-made treatment effects in the application of surgical procedures.
COVID-19 has led to major changes in medical systems globally
[31]. It affects PD patients and particularly those that may have lost healthcare resources during the period of the pandemic
[32]. During this period, the use of telemedicine, which is recommended in PD treatment, has been useful for outpatient care and may be continued into the future
[33]. We conducted a questionnaire survey regarding telemedicine among PD patients in Japan
[34]. The results revealed that a majority of patients were aware of the availability of this means of healthcare. Smartphone users, credit card users, and those who lived in regions distant from a hospital tend to prefer the convenience of this facility
[34]. Although individual situations vary between countries and regions, telemedicine may be useful for continuing outpatient treatment of PD patients who have undergone advanced treatment. Indeed, the usefulness of telemedicine has been reported in DBS and LCIG even before the COVID-19 pandemic
[35][36]. The spread of telemedicine may have a great impact on the choice of advanced treatment for PD.
4. Conclusions
Here, we have discussed various advanced treatments for advanced PD. In the future, there may be additional advanced treatment options, including cell therapy and gene therapy. In addition, the development of optogenetics, magnetogenetics, and sonogenetics is expected. Therefore, it is important to consider the individual symptoms, patient background, and cost of these options when deciding on advanced treatment.