Patient-specific three-dimensional (3D) printed models have been increasingly used in cardiology and cardiac surgery, in particular, showing great value in the domain of congenital heart disease (CHD). CHD is characterized by complex cardiac anomalies with disease variations between individuals; thus, it is difficult to obtain comprehensive spatial conceptualization of the cardiac structures based on the current imaging visualizations. 3D printed models derived from patient’s cardiac imaging data overcome this limitation by creating personalized 3D heart models, which not only improve spatial visualization, but also assist preoperative planning and simulation of cardiac procedures, serve as a useful tool in medical education and training, and improve doctor–patient communication.
- three-dimensional printing
- congenital heart disease
- medical education
1. Introduction
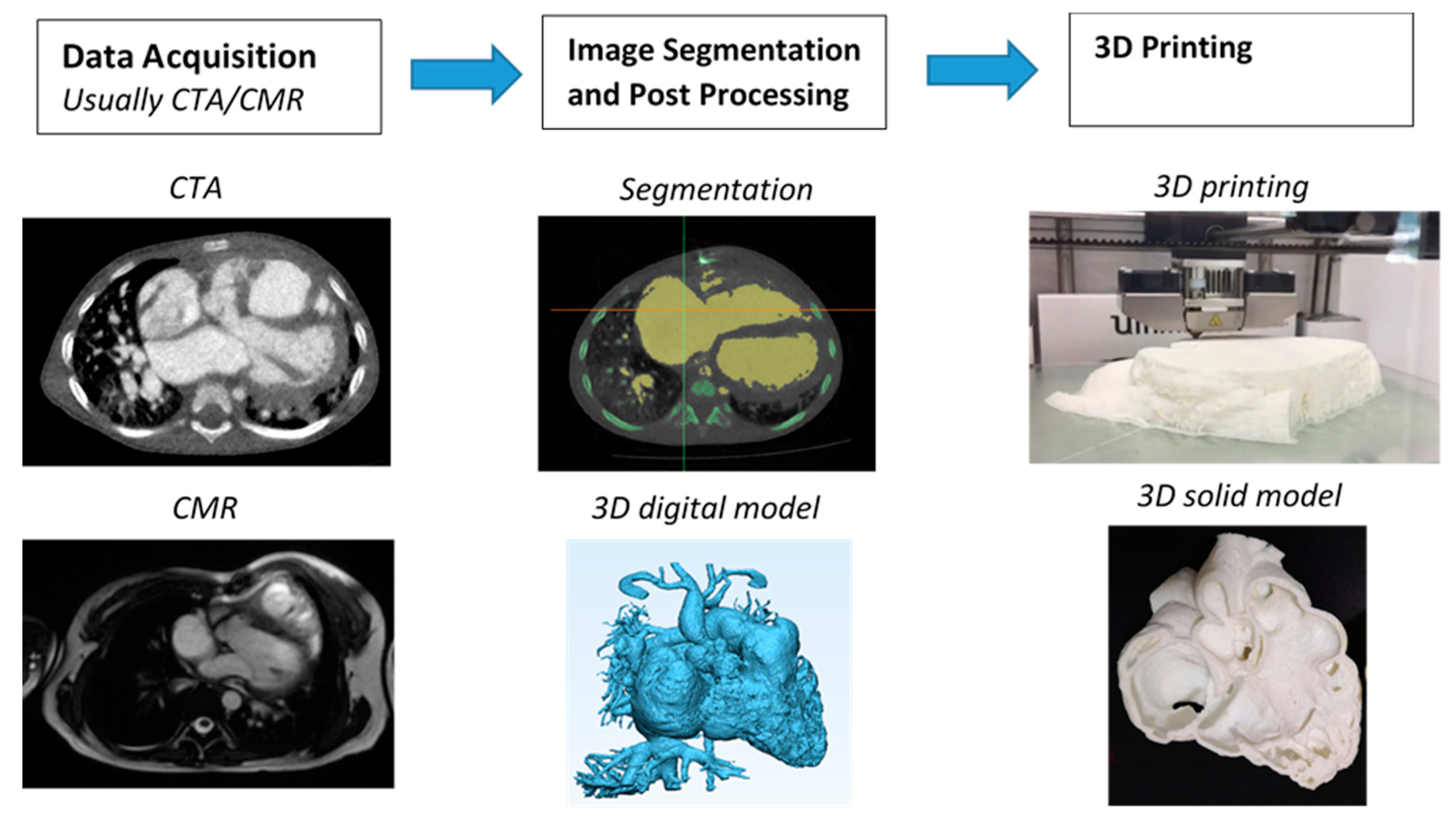
2. Image Post-Processing and Segmentation Process for Three-Dimensional (3D) Printing in Congenital Heart Disease (CHD)
3. Accuracy of 3D Printed Heart Models
4. 3D Printed Models in Medical Education and Training
| Authors | Study Design | Sample Size and Participants | Types of CHD | Key Findings |
|---|---|---|---|---|
| Loke et al. 2017 [22] | RCT: study group was presented with 3D printed models, while control group with 2D images | 35 pediatric residents:18 in study group and 17 in control group | Tetralogy of Fallot (ToF) | 3D printed models resulted in significantly higher satisfaction scores than 2D images (p = 0.03). 3D printed models improved residents’ self-efficacy scores in managing ToF, although this did not reach significant difference when compared to 2D images (p = 0.39). |
| Su et al., 2018 [23] | RCT: study group participated in teaching seminar including 3D printed models, while control group only attended teaching seminar without having 3D models | 63 medical students: 32 in study group and 31 in control group | Ventricular septal defect (VSD) | Significant improvement in VSD learning and structure conceptualization in the study group compared to the control group (p < 0.05). |
| White et al., 2018 [24] | RCT: study group was given 3D printed models in addition to lectures, while control group received only the lectures | 60 pediatric residents:31 in study group and 29 in control group | VSD and ToF | 3D printed models of CHD improved residents’ knowledge and confidence in managing complex CHD such as ToF but did not seem to improve simple CHD such as VSD. |
| Olivieri et al., 2016 [26] | Single-center report of 3D printed models for training and simulation | 10 3D printed models, 70 clinicians participated in the training sessions | Cardiac and vascular anomalies | 3D printed models can be used as a simulation training tool for multidisciplinary intensive care providers by enhancing their anatomic knowledge and clinical management of CHD patients. |
| Hoashi et al., 2018 [27] | Single-center experience | 20 cases | DORV and other cardiac anomalies | 3D printed heart models improved understanding of the relationship between intraventricular communications and great vessels. Further, 3D printed models allowed simulation of cardiac surgeries by creating intracardiac pathways, thus providing benefits to inexperienced cardiac surgeons. |
| Valverde et al., 2017 [21] | Multi-center study consisting of 10 international centers | 40 patients with complex CHD | DORV (50%) and other cardiac anomalies | 3D models were accurate in replicating anatomy. 3D models refined the surgical approach in nearly 50% cases. 3D models resulted in significant change in the surgical plan in 24% of cases. |
| Zhao et al., 2018 [28] | Single-center experience | 25 patients with 8 in 3D printing group and 17 in control group | DORV | 3D printed models showed high accuracy in measurements of aortic diameters and the size of VSD when compared to original CT data. 3D printed models significantly reduced ICU time and mechanical ventilation time (p < 0.05). |
| Ryan et al., 2018 [29] | Single-center experience | Of 928 cardiothoracic surgeries, 164 3D models were printed for various purposes | DORV, ToF and other cardiac anomalies | 3D printed models reduced mean time in the operating room and 30-day readmission and mortality rates when compared to the standard of care. |
5. 3D Printed Models in Pre-Surgical Planning and Simulation
6. 3D Printed Models in Doctor–Patient Communication
This entry is adapted from the peer-reviewed paper 10.3390/jcm8040522
References
- Yao, R.; Xu, G.; Mao, S.S.; Yang, H.Y.; Sang, X.T.; Sun, W.; Mao, Y.L. Three-dimensional printing: Review of application in medicine and hepatic surgery. Cancer. Biol. Med. 2016, 13, 443–451.
- Chepelev, L.; Souza, C.; Althobaity, W.; Miguel, O.; Krishna, S.; Akyuz, E.; Hodgdon, T.; Torres, C.; Wake, N.; Alexander, A.; et al. Preoperative planning and tracheal stent design in thoracic surgery: A primer for the 2017 Radiological Society of North America (RSNA) hands-on course in 3D printing. 3D Print Med. 2017, 3, 14.
- Matsumoto, J.S.; Morris, J.M.; Foley, T.A.; Williamson, E.E.; Leng, S.; McGee, K.P.; Kuhlmann, J.L.; Nesberg, L.E.; Vrtiska, T.J. Three-dimensional physical modeling: applications and experience at Mayo Clinic. Radiographics 2015, 35, 1989–2006.
- Mitsouras, D.; Liacouras, P.; Imanzadeh, A.; Giannopolous, A.A.; Cai, T.; Kumamaru, K.K.; George, E.; Wake, N.; Caterson, E.J.; Pomahac, B.; et al. Medical 3D printing for the radiologist. Radiographics 2015, 35, 1965–1988.
- Costello, J.; Olivieri, L.; Krieger, A.; Thabit, O.; Marshall, M.B.; Yoo, S.J.; Kim, P.C.; Jonas, R.A.; Nath, D.S. Utilizing three-dimensional printing technology to assess the feasibility of high-fidelity synthetic ventricular septal defect models for simulation in medical education. World J. Pediatr. Congenit. Heart Surg. 2014, 5, 421–426.
- Costello, J.P.; Olivieri, L.J.; Su, L.; Krieger, A.; Alfares, F.; Thabit, O.; Marshall, M.B.; Yoo, S.J.; Kim, P.C.; Jonas, R.A.; Nath, D.S. Incorporating three-dimensional printing into a simulation-based congenital heart disease and critical care training curriculum for resident physicians. Congenit. Heart Dis. 2015, 10, 185–190.
- Valverde, I.; Gomez, G.; Gonzales, A.; Suraz-Mejias, C.; Absuar, A.; Coserria, J.F.; Uribe, S.; Gomez-Cia, T.; Hosseinpour, A.R. Three-dimensional patient-specific cardiac model for surgical planning in Nikaidoh procedure. Cardiol. Young 2015, 25, 698–704.
- Hossien, A.; Gesomino, S.; Maessen, J.; Autschbach, R. The interactive use of multi-dimensional modeling and 3D printing in preplanning of type A aortic dissection. J. Card. Surg. 2016, 31, 441–445.
- Wang, H.; Liu, J.; Zheng, X.; Rong, X.; Zheng, X.; Peng, H.; Silber-Li, Z.; Li, M.; Liu, L. Three-dimensional virtual surgery models for percutaneous coronary intervention (PCI) optimization strategies. Sci. Rep. 2015, 5, 10945.
- Sun, Z.; Squelch, A. Patient-specific 3D printed models of aortic aneurysm and aortic dissection. J. Med. Imaging Health Inf. 2017, 7, 886–889.
- Sun, Z.; Lee, S. A systematic review of 3D printing in cardiovascular and cerebrovascular diseases. Anatol. J. Cardiol. 2017, 17, 423–435.
- Perica, E.; Sun, Z. A systematic review of three-dimensional printing in liver disease. J. Digit. Imaging 2018, 31, 692–701.
- Vukicevic, M.; Mosadegh, B.; Min, J.K.; Little, S.H. Cardiac 3D printing and its future directions. JACC. Cardiovasc. Imaging 2017, 10, 171–184.
- Giannopoulos, A.A.; Steigner, M.L.; George, E.; Barile, M.; Hunsaker, A.R.; Rybicki, F.J.; Mitsouras, D. Cardiothoracic applications of 3-dimensional printing. J. Thorac. Imaging 2016, 31, 253–272.
- George, E.; Liacouras, P.; Rybicki, F.J.; Mitsouras, D. Measuring and establishing the accuracy and reproducibility of 3D printed medical models. Radiographics 2017, 37, 1424–1450.
- Lau, I.; Liu, D.; Xu, L.; Fan, Z.; Sun, Z. Clinical value of patient-specific three-dimensional printing of congenital heart disease: Quantitative and qualitative Assessments. PLoS ONE 2018, 13, e0194333.
- Parimi, M.; Buelter, J.; Thanugundla, V.; Condoor, S.; Parkar, N.; Danon, S.; King, W. Feasibility and validity of printing 3D heart models from rotational angiography. Pediatr. Cardiol. 2018, 39, 653–658.
- Olivieri, L.J.; Krieger, A.; Loke, Y.H.; Nath, D.S.; Kim, P.C.; Sable, C.A. Three-dimensional printing of intracardiac defects from three dimensional echocardiographic images: feasibility and relative accuracy. J. Am. Soc. Echocardiogr. 2015, 28, 392–397.
- Ma, X.J.; Tao, L.; Chen, X.; Li, W.; Peng, Z.Y.; Jin, J.; Zhang, X.L.; Xiong, Q.F.; Zhong, Z.L.; Chen, X.F. Clinical application of three-dimensional reconstruction and rapid prototyping technology of multislice spiral computed tomography angiography for the repair of ventricular septal defect of tetralogy of fallot. Genet. Mol. Res. 2015, 14, 1301–1309.
- Ngan, E.M.; Rebeyka, I.M.; Ross, D.B.; Hirji, M.; Wolfaardt, J.F.; Seelaus, R.; Grosvenor, A.; Noga, M.L. The rapid prototyping of anatomic models in pulmonary atresia. J. Thorac. Cardiovasc. Surg. 2006, 132, 264–269.
- Valverde, I.; Gomez-Ciriza, G.; Hussain, T.; Suarez-Mejias, C.; Velasco-Forte, M.N.; Byrne, N.; Ordoñez, A.; Gonzalez-Calle, A.; Anderson, D.; Hazekamp, M.G.; et al. Three dimensional printed models for surgical planning of complex congenital heart defects: an international multicenter study. Eur. J. Cardiothorac. Surg. 2017, 52, 1139–1148.
- Loke, Y.H.; Harahsheh, A.S.; Krieger, A.; Olivieri, L.J. Usage of 3D models of tetralogy of Fallot for medical education: impact on learning congenital heart disease. BMC Med. Educ. 2017, 17, 54.
- Su, W.; Xiao, Y.; He, S.; Huang, P.; Deng, X. Three-dimensional printing models in congenital heart disease education for medical students: a controlled comparative study. BMC Med. Educ. 2018, 18, 178.
- White, S.C.; Sedler, J.; Jones, T.W.; Seckeler, M. Utility of three-dimensional models in resident education on simple and complex intracardiac congenital heart defects. Congenit. Heart Dis. 2018.
- Lim, K.H.A.; Loo, Z.Y.; Goldie, S.J.; Adams, J.W.; McMenamin, P.G. Use of 3D printed models in medical education: A randomized control trial comparing 3D prints versus cadaveric materials for learning external cardiac anatomy. Anat. Sci. Educ. 2016, 9, 213–221.
- Olivieri, L.J.; Su, L.; Hynes, C.F.; Krieger, A.; Alfares, F.A.; Ramakrishnan, K.; Zurakowski, D.; Marshall, M.B.; Kim, P.C.; Jonas, R.A.; et al. “Just-In-Time” simulation training using 3-D printed cardiac models after congenital cardiac surgery. World J. Pediatr. Congenit. Heart Surg. 2016, 7, 164–168.
- Lau, I.; Sun, Z. Three-dimensional printing in congenital heart disease: A systematic review. J. Med. Radiat. Sci. 2018, 65, 226–236.
- Jones, T.W.; Seckeler, M.D. Use of 3D models of vascular rings and slings to improve resident education. Congenit. Heart Dis. 2017, 12, 578–582.
- Biglino, G.; Capelli, C.; Leaver, L.K.; Shievano, S.; Taylor, A.M.; Wray, J. Involving patients, families and medical staff in the evaluation of 3D printing models of congenital heart disease. Commun. Med. 2015, 12, 157–169.
- Ryan, J.; Plasencia, J.; Richardson, R.; Velez, D.; Nigro, J.J.; Pophal, S.; Frakes, D. 3D printing for congenital heart disease: A single site’s initial three-year experience. 3D Print. Med. 2018, 4, 10.
- Fuertes, J.N.; Toporovsky, A.; Reyes, M.; Osborne, J.B. The physician-patient working alliance: Theory, research, and future possibilities. Patient Educ. Couns. 2017, 100, 610–615.
- Milano, E.G.; Capelli, C.; Wray, J.; Biffi, B.; Layton, S.; Lee, M.; Caputo, M.; Taylor, A.M.; Schievano, S.; Biglino, G. Current and future applications of 3D printing in congenital cardiology and cardiac surgery. Br. J. Radiol. 2019, 91, 20180389.
- Biglino, G.; Capelli, C.; Wray, J.; Schievano, S.; Leaver, L.K.; Khambadkone, S.; Giardini, A.; Derrick, G.; Jones, A.; Taylor, A.M. 3D-manufactured patient-specific models of congenital heart defects for communication in clinical practice: Feasibility and acceptability. BMJ Open 2015, 5, e007165.
