Gout is a metabolic disorder, and one of the most common inflammatory arthritic conditions, caused by elevated serum urate (SU). Gout prevalence is globally rising, partly due to global dietary changes and the growing older adult population. Gout was known to affect people of high socioeconomic status. Currently, gout disproportionately affects specific population subgroups that share distinct racial and ethnic backgrounds. While genetics may predict SU levels, nongenetic factors, including diet, cultural traditions, and social determinants of health (SDOH), need to be evaluated to optimize patient treatment outcomes. A cultural assessment may inform the development of culturally tailored dietary recommendations for patients with gout. Causal and association studies investigating the interaction between diet, genetics, and gout, should be cautiously interpreted due to the lack of reproducibility in different racial groups. Optimal gout management could benefit from a multidisciplinary approach, involving pharmacists and nurses.
- acculturation
- gout management
- hyperuricemia
- culture
- diet
- genetics
1. Introduction
Gout is a metabolic disorder, and one of the most common inflammatory arthritic conditions worldwide, caused by persistent hyperuricemia. Developing gout is multifactorial, ushering in different methodological approaches to ascertain the risk factors associated with developing hyperuricemia and gout. Despite substantial advancement in understanding the biological basis of gout, it remains one of the most poorly managed chronic conditions in healthcare. Uncontrolled gout is associated with a poor quality of life, joint damage, an increase in missed days of work, and a higher utilization of the healthcare system resources [1][2][3].
Gout is a chronic inflammatory condition caused by persistent hyperuricemia, leading to the formation and deposition of monosodium urate crystals into and around the distal joints. The development of hyperuricemia and gout is heterogenous, and, therefore, different research approaches are needed to identify and quantify the distinct risk factors in the pathogenesis of both conditions. For example, the Mendelian Randomization (MR) approach provides a pathway to ascertain causality, exploiting the natural randomization of allele causal disease. However, this approach is not without limitations, possibly due to the pleiotropic effect of the selected instrumental variables [4]. As gout continues to disproportionately affect non-EUR populations, there is a growing need to increase the representation of minorities in genetic research and cross-validation of genetic findings in multiple populations. To that end, it recognized that developing hyperuricemia and gout is a multifactorial process founded in genetics and modulated by epigenetic factors, including medications, lifestyle factors, diet, and the potential interactions between all of them. While genetic polymorphisms in ABCG2 and SLC2A9 remain two of the most significant signals in developing hyperuricemia and gout across different populations, evaluating nongenetic factors across selected populations through a cultural lens is an adjunct approach to further stratify hyperuricemia and gout risk and optimize gout management. This encompassing approach could be a valuable tool for gout patients with strong cultural identities and distinct racial or ethnic backgrounds. A summary of the major genes associated with regulating uric acid in humans is listed in Table 1.
| Gene | Protein | Possible Functions |
|---|---|---|
| ABCG2 | ATP binding cassette subfamily G member 2: ABCG2 | Regulating renal and gut excretion of urate. Gene polymorphisms are strongly linked to urate underexcretion and the risk of early-onset gout in men. Genetic polymorphisms may also influence the therapeutic response to allopurinol and other statin medications. |
| GCKR | Glucokinase regulator | Regulatory protein that inhibits glucokinase in the liver and pancreatic islet cells by forming an inactive complex with the enzyme. Gene polymorphisms are associated with fasting glucose, maturity-onset type-2 diabetes, hyperuricemia, and gout. |
| LRRC16A | Capping protein regulator and myosin 1 linker 1: CARMIL1 | Cytoskeleton-associated protein. Gene polymorphisms are associated with urate concentrations and gout subtypes. |
| PDZK1 | PDZK domain-containing scaffolding protein | Mediates the localization of cell surface proteins and plays a critical role in cholesterol metabolism. Gene polymorphisms are linked to dyslipidemia, hyperuricemia, and gout. |
| SLC2A9 | Solute carrier family 2 member 9: GLUT9 | Regulating renal uric acid reabsorption. Gene polymorphisms are linked to the risk of gout in women. |
| SLC16A9 | Solute carrier family 16 member 9: MCT9 | Regulating monocarboxylic acid transporter. Gene polymorphisms are linked to uric acid concentrations. |
| SLC17A1 | Solute carrier family 17 member 1: NPT1 | Sodium phosphate cotransporter. Gene polymorphisms are linked with hyperuricemia and gout. |
| SLC22A11 | Solute carrier family 22 member 11: OAT4 | Urate reabsorption transporter. A target for some uricosuric drugs. Gene polymorphisms are associated with hyperuricemia. |
| SLC22A12 | Solute carrier family 22 member 12: URAT1 | Uric acid reabsorption transporter. A major target for uricosuric drugs. Gene polymorphisms are associated with hyperuricemia and gout. Loss of function in the gene can also lead to hypouricemia. |
2. Heritability of Urate Levels and Urate-Modifying Factors
| Diet/Food/Lifestyle Factor | Serum Urate Level | Incident Gout | Gout Flare Risk | ACR 2020 Recommendations [13] | References |
|---|---|---|---|---|---|
| DASH diet | 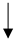 |
 |
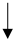 |
No recommendation | [14][15][16] |
| Mediterranean diet | 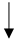 |
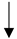 |
 |
No recommendation | [17] |
| Ketogenic diet |  |
No data | No data | No recommendation | [18] |
| Low-fat dairy products |
 |
 |
 |
No recommendation | [19][20] |
| Cherries |  |
 |
 |
No recommendation | [21][22] |
| Coffee |   |
 |
 |
No recommendation | [23][24][25][26] |
| Tea |   |
No data | No data | No recommendation | [25][26][27] |
| High-fructose corn syrup (HFCS) |  |
 |
 |
Conditionally recommends limiting the intake of HFCS | [28][29] |
| Weight loss | 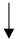 |
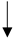 |
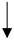 |
Conditionally recommends a weight loss program | [30][31] |
| Physical exercise | 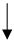 |
No data | No data | No recommendation | [9][30] |
| Smoking |   |
 |
No data | No recommendation | [32][33][34] |
| Alcohol |  |
 |
 |
Conditionally recommends limiting alcohol intake | [35][36][37] |
| Vitamin B complex (B6-B12-Folic acid) |  |
No data | No data | No recommendation | [38] |
| Vitamin C |   |
No data | 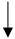 |
Conditionally recommends against use | [10][39][40] |
| Fish Oil/Omega-3-fatty acids |  |
No data | 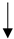 |
No recommendation | [11][41][42] |
3. Gout Risk and Acculturation
Dietary habits are mirrors of cultural customs and traditions. Certain population subgroups tend to follow a specific diet for personal, social, and religious norms [43][44]. Nonetheless, immigration or acculturation could significantly impact the lifestyle and dietary habits of the same population groups [44][45][46]. These changes could have significant effects on the individuals’ overall health, ranging from energy expenditure-related activities to their gut microbiome. Collectively, these changes could have a consequential impact on developing cardiometabolic risk factors, including hyperuricemia and gout. Similarly, Filipinos living in the US were reported to have higher gout rates and elevated means SU levels than those residing in the Philippines, suggesting significant gene–environment interactions [47][48]. Conversely, developing hyperuricemia or gout among US immigrant groups could be owing to a more permissive environment, increasing the penetrance of risk alleles by equivalent effects [44][49]. For example, the joint effect of alcohol consumption and carrying the risk allele of ABCG2 rs2231142 G > T was associated with a greater risk for developing hyperuricemia than the risk allele alone, especially among women [50]. Therefore, ascertaining the dietary and social lifestyle habits among distinct racial and ethnic groups could shed additional light on the hypothesis of gene–diet/gene–social habits interactions and population-specific risk for developing hyperuricemia or gout [35][51]. Additionally, this ascertainment may provide more evidence on the role of preserving a cultural identity in disease prevention and the generational effect on disease onset among immigrant groups.4. Gout Risk and Health Beliefs
5. Gout and Social Determinants of Health
6. Multidisciplinary Approach to Gout Management
7. Pharmacogenomics and Gout Management
This entry is adapted from the peer-reviewed paper 10.3390/nu14173590
References
- Singh, J.A. The impact of gout on patient’s lives: A study of African-American and Caucasian men and women with gout. Arthritis Res. Ther. 2014, 16, R132.
- Chandratre, P.; Mallen, C.; Richardson, J.; Muller, S.; Hider, S.; Rome, K.; Blagojevic-Bucknall, M.; Roddy, E. Health-related quality of life in gout in primary care: Baseline findings from a cohort study. Semin. Arthritis Rheum. 2018, 48, 61–69.
- Chandratre, P.; Roddy, E.; Clarson, L.; Richardson, J.; Hider, S.L.; Mallen, C.D. Health-related quality of life in gout: A systematic review. Rheumatology 2013, 52, 2031–2040.
- Davies, N.M.; Holmes, M.V.; Davey Smith, G. Reading Mendelian randomisation studies: A guide, glossary, and checklist for clinicians. BMJ 2018, 362, k601.
- Krishnan, E.; Lessov-Schlaggar, C.N.; Krasnow, R.E.; Swan, G.E. Nature versus nurture in gout: A twin study. Am. J. Med. 2012, 125, 499–504.
- Wilk, J.B.; Djousse, L.; Borecki, I.; Atwood, L.D.; Hunt, S.C.; Rich, S.S.; Eckfeldt, J.H.; Arnett, D.K.; Rao, D.C.; Myers, R.H. Segregation analysis of serum uric acid in the NHLBI Family Heart Study. Hum. Genet. 2000, 106, 355–359.
- Wang, Y.; Yan, S.; Li, C.; Zhao, S.; Lv, J.; Wang, F.; Meng, D.; Han, L.; Wang, Y.; Miao, Z. Risk factors for gout developed from hyperuricemia in China: A five-year prospective cohort study. Rheumatol. Int. 2013, 33, 705–710.
- Wang, W.; Krishnan, E. Cigarette smoking is associated with a reduction in the risk of incident gout: Results from the Framingham Heart Study original cohort. Rheumatology 2015, 54, 91–95.
- Chen, J.H.; Wen, C.P.; Wu, S.B.; Lan, J.L.; Tsai, M.K.; Tai, Y.P.; Lee, J.H.; Hsu, C.C.; Tsao, C.K.; Wai, J.P.; et al. Attenuating the mortality risk of high serum uric acid: The role of physical activity underused. Ann. Rheum. Dis. 2015, 74, 2034–2042.
- Juraschek, S.P.; Gaziano, J.M.; Glynn, R.J.; Gomelskaya, N.; Bubes, V.Y.; Buring, J.E.; Shmerling, R.H.; Sesso, H.D. Effects of vitamin C supplementation on gout risk: Results from the physicians’ health study II trial. Am. J. Clin. Nutr. 2022, nqac140.
- Stamp, L.K.; Grainger, R.; Frampton, C.; Drake, J.; Hill, C.L. Effect of omega-three supplementation on serum urate and gout flares in people with gout; a pilot randomized trial. BMC Rheumatol. 2022, 6, 31.
- Choi, H.K.; Soriano, L.C.; Zhang, Y.; Rodriguez, L.A. Antihypertensive drugs and risk of incident gout among patients with hypertension: Population based case-control study. BMJ 2012, 344, d8190.
- FitzGerald, J.D.; Dalbeth, N.; Mikuls, T.; Brignardello-Petersen, R.; Guyatt, G.; Abeles, A.M.; Gelber, A.C.; Harrold, L.R.; Khanna, D.; King, C.; et al. 2020 American College of Rheumatology Guideline for the Management of Gout. Arthritis Care Res. 2020, 72, 744–760.
- Juraschek, S.P.; Miller, E.R., 3rd; Wu, B.; White, K.; Charleston, J.; Gelber, A.C.; Rai, S.K.; Carson, K.A.; Appel, L.J.; Choi, H.K. A Randomized Pilot Study of DASH Patterned Groceries on Serum Urate in Individuals with Gout. Nutrients 2021, 13, 538.
- Tang, O.; Miller, E.R., 3rd; Gelber, A.C.; Choi, H.K.; Appel, L.J.; Juraschek, S.P. DASH diet and change in serum uric acid over time. Clin. Rheumatol. 2017, 36, 1413–1417.
- Rai, S.K.; Fung, T.T.; Lu, N.; Keller, S.F.; Curhan, G.C.; Choi, H.K. The Dietary Approaches to Stop Hypertension (DASH) diet, Western diet, and risk of gout in men: Prospective cohort study. BMJ 2017, 357, j1794.
- Stamostergiou, J.; Theodoridis, X.; Ganochoriti, V.; Bogdanos, D.P.; Sakkas, L.I. The role of the Mediterranean diet in hyperuricemia and gout. Mediterr. J. Rheumatol. 2018, 29, 21–25.
- Hussain, T.A.; Mathew, T.C.; Dashti, A.A.; Asfar, S.; Al-Zaid, N.; Dashti, H.M. Effect of low-calorie versus low-carbohydrate ketogenic diet in type 2 diabetes. Nutrition 2012, 28, 1016–1021.
- Lipkowitz, M.S. Regulation of uric acid excretion by the kidney. Curr. Rheumatol. Rep. 2012, 14, 179–188.
- Teng, G.G.; Pan, A.; Yuan, J.M.; Koh, W.P. Food Sources of Protein and Risk of Incident Gout in the Singapore Chinese Health Study. Arthritis Rheumatol. 2015, 67, 1933–1942.
- Zhang, Y.; Neogi, T.; Chen, C.; Chaisson, C.; Hunter, D.J.; Choi, H.K. Cherry consumption and decreased risk of recurrent gout attacks. Arthritis Rheum. 2012, 64, 4004–4011.
- Jacob, R.A.; Spinozzi, G.M.; Simon, V.A.; Kelley, D.S.; Prior, R.L.; Hess-Pierce, B.; Kader, A.A. Consumption of cherries lowers plasma urate in healthy women. J. Nutr. 2003, 133, 1826–1829.
- Bae, J.; Park, P.S.; Chun, B.Y.; Choi, B.Y.; Kim, M.K.; Shin, M.H.; Lee, Y.H.; Shin, D.H.; Kim, S.K. The effect of coffee, tea, and caffeine consumption on serum uric acid and the risk of hyperuricemia in Korean Multi-Rural Communities Cohort. Rheumatol. Int. 2015, 35, 327–336.
- Kiyohara, C.; Kono, S.; Honjo, S.; Todoroki, I.; Sakurai, Y.; Nishiwaki, M.; Hamada, H.; Nishikawa, H.; Koga, H.; Ogawa, S.; et al. Inverse association between coffee drinking and serum uric acid concentrations in middle-aged Japanese males. Br. J. Nutr. 1999, 82, 125–130.
- Choi, H.K.; Curhan, G. Coffee, tea, and caffeine consumption and serum uric acid level: The third national health and nutrition examination survey. Arthritis Rheum. 2007, 57, 816–821.
- Shirai, Y.; Nakayama, A.; Kawamura, Y.; Toyoda, Y.; Nakatochi, M.; Shimizu, S.; Shinomiya, N.; Okada, Y.; Matsuo, H.; Japan Gout Genomics Consortium. Coffee Consumption Reduces Gout Risk Independently of Serum Uric Acid Levels: Mendelian Randomization Analyses Across Ancestry Populations. ACR Open Rheumatol. 2022, 4, 534–539.
- Li, R.; Zeng, L.; Wu, C.; Ma, P.; Cui, H.; Chen, L.; Li, Q.; Hong, C.; Liu, L.; Xiao, L. Tea Consumption is associated with an Increased Risk of Hyperuricemia in an Occupational Population in Guangdong, China. Int. J. Gen. Med. 2022, 15, 2747–2757.
- Batt, C.; Phipps-Green, A.J.; Black, M.A.; Cadzow, M.; Merriman, M.E.; Topless, R.; Gow, P.; Harrison, A.; Highton, J.; Jones, P.; et al. Sugar-sweetened beverage consumption: A risk factor for prevalent gout with SLC2A9 genotype-specific effects on serum urate and risk of gout. Ann. Rheum. Dis. 2014, 73, 2101–2106.
- Tappy, L.; Le, K.A. Metabolic effects of fructose and the worldwide increase in obesity. Physiol. Rev. 2010, 90, 23–46.
- Zhou, J.; Wang, Y.; Lian, F.; Chen, D.; Qiu, Q.; Xu, H.; Liang, L.; Yang, X. Physical exercises and weight loss in obese patients help to improve uric acid. Oncotarget 2017, 8, 94893–94899.
- McCormick, N.; Rai, S.K.; Lu, N.; Yokose, C.; Curhan, G.C.; Choi, H.K. Estimation of Primary Prevention of Gout in Men Through Modification of Obesity and Other Key Lifestyle Factors. JAMA Netw. Open 2020, 3, e2027421.
- Haj Mouhamed, D.; Ezzaher, A.; Neffati, F.; Douki, W.; Gaha, L.; Najjar, M.F. Effect of cigarette smoking on plasma uric acid concentrations. Environ. Health Prev. Med. 2011, 16, 307–312.
- Hanna, B.E.; Hamed, J.M.; Touhala, L.M. Serum uric Acid in smokers. Oman. Med. J. 2008, 23, 269–274.
- Tomita, M.; Mizuno, S.; Yokota, K. Increased levels of serum uric acid among ex-smokers. J. Epidemiol. 2008, 18, 132–134.
- Tu, H.P.; Ko, A.M.; Chiang, S.L.; Lee, S.S.; Lai, H.M.; Chung, C.M.; Huang, C.M.; Lee, C.H.; Kuo, T.M.; Hsieh, M.J.; et al. Joint effects of alcohol consumption and ABCG2 Q141K on chronic tophaceous gout risk. J. Rheumatol. 2014, 41, 749–758.
- Wang, M.; Jiang, X.; Wu, W.; Zhang, D. A meta-analysis of alcohol consumption and the risk of gout. Clin. Rheumatol. 2013, 32, 1641–1648.
- Choi, H.K.; Atkinson, K.; Karlson, E.W.; Willett, W.; Curhan, G. Alcohol intake and risk of incident gout in men: A prospective study. Lancet 2004, 363, 1277–1281.
- Zhang, Y.; Qiu, H. Folate, Vitamin B6 and Vitamin B12 Intake in Relation to Hyperuricemia. J. Clin. Med. 2018, 7, 210.
- Bae, J.; Shin, D.H.; Chun, B.Y.; Choi, B.Y.; Kim, M.K.; Shin, M.H.; Lee, Y.H.; Park, P.S.; Kim, S.K. The effect of vitamin C intake on the risk of hyperuricemia and serum uric acid level in Korean Multi-Rural Communities Cohort. Jt. Bone Spine 2014, 81, 513–519.
- Stamp, L.K.; O’Donnell, J.L.; Frampton, C.; Drake, J.M.; Zhang, M.; Chapman, P.T. Clinically insignificant effect of supplemental vitamin C on serum urate in patients with gout: A pilot randomized controlled trial. Arthritis Rheum. 2013, 65, 1636–1642.
- Saito, H.; Toyoda, Y.; Takada, T.; Hirata, H.; Ota-Kontani, A.; Miyata, H.; Kobayashi, N.; Tsuchiya, Y.; Suzuki, H. Omega-3 Polyunsaturated Fatty Acids Inhibit the Function of Human URAT1, a Renal Urate Re-Absorber. Nutrients 2020, 12, 1601.
- Zhang, M.; Zhang, Y.; Terkeltaub, R.; Chen, C.; Neogi, T. Effect of Dietary and Supplemental Omega-3 Polyunsaturated Fatty Acids on Risk of Recurrent Gout Flares. Arthritis Rheumatol. 2019, 71, 1580–1586.
- Butler, F.; Alghubayshi, A.; Roman, Y. The Epidemiology and Genetics of Hyperuricemia and Gout across Major Racial Groups: A Literature Review and Population Genetics Secondary Database Analysis. J. Pers. Med. 2021, 11, 231.
- Roman, Y.M.; Lor, K.; Xiong, T.; Culhane-Pera, K.; Straka, R.J. Gout prevalence in the Hmong: A prime example of health disparity and the role of community-based genetic research. Per. Med. 2021, 18, 311–327.
- Coronado, G.; Chio-Lauri, J.; Cruz, R.D.; Roman, Y.M. Health Disparities of Cardiometabolic Disorders among Filipino Americans: Implications for Health Equity and Community-Based Genetic Research. J. Racial Ethn. Health Disparities 2021.
- Lee, J.R.; Maruthur, N.M.; Yeh, H.C. Nativity and prevalence of cardiometabolic diseases among U.S. Asian immigrants. J. Diabetes Complicat. 2020, 34, 107679.
- Roman, Y.; Tiirikainen, M.; Prom-Wormley, E. The prevalence of the gout-associated polymorphism rs2231142 G > T in ABCG2 in a pregnant female Filipino cohort. Clin. Rheumatol. 2020, 39, 2387–2392.
- Bayani-Sioson, P.S.; Skeith, M.; Healey, L.S., Jr. On Filipino hyperuricemia. Acta Med. Philipp. 1966, 3, 126–127.
- Roman, Y.M.; Culhane-Pera, K.A.; Menk, J.; Straka, R.J. Assessment of genetic polymorphisms associated with hyperuricemia or gout in the Hmong. Per. Med. 2016, 13, 429–440.
- Chen, I.C.; Chen, Y.J.; Chen, Y.M.; Lin, H.J.; Lin, Y.C.; Chagn, J.C.; Chen, P.C.; Lin, C.H. Interaction of Alcohol Consumption and ABCG2 rs2231142 Variant Contributes to Hyperuricemia in a Taiwanese Population. J. Pers. Med. 2021, 11, 1158.
- Yang, H.J.; Liu, M.; Kim, M.J.; Park, S. The haplotype of SLC2A9_rs3733591, PKD2_rs2725220 and ABCG2_rs2231142 increases the hyperuricaemia risk and alcohol, chicken and processed meat intakes and smoking interact with its risk. Int. J. Food Sci. Nutr. 2021, 72, 391–401.
- Guillen, A.G.; Te Karu, L.; Singh, J.A.; Dalbeth, N. Gender and Ethnic Inequities in Gout Burden and Management. Rheum. Dis. Clin. N. Am. 2020, 46, 693–703.
- Chen-Xu, M.; Yokose, C.; Rai, S.K.; Pillinger, M.H.; Choi, H.K. Contemporary Prevalence of Gout and Hyperuricemia in the United States and Decadal Trends: The National Health and Nutrition Examination Survey, 2007–2016. Arthritis Rheumatol. 2019, 71, 991–999.
- Yin, R.; Li, L.; Zhang, G.; Cui, Y.; Zhang, L.; Zhang, Q.; Fu, T.; Cao, H.; Li, L.; Gu, Z. Rate of adherence to urate-lowering therapy among patients with gout: A systematic review and meta-analysis. BMJ Open 2018, 8, e017542.
- Yokose, C.; McCormick, N.; Choi, H.K. The role of diet in hyperuricemia and gout. Curr. Opin. Rheumatol. 2021, 33, 135–144.
- Kong, D.C.H.; Sturgiss, E.A.; Dorai Raj, A.K.; Fallon, K. What factors contribute to uncontrolled gout and hospital admission? A qualitative study of inpatients and their primary care practitioners. BMJ Open 2019, 9, e033726.
- Emad, Y.; Dalbeth, N.; Weinman, J.; Chalder, T.; Petrie, K.J. Why Do Patients with Gout Not Take Allopurinol? J. Rheumatol. 2022, 49, 622–626.
- Krishnan, E.; Lienesch, D.; Kwoh, C.K. Gout in ambulatory care settings in the United States. J. Rheumatol. 2008, 35, 498–501.
- Roman, Y.M. The Daniel K. Inouye College of Pharmacy Scripts: Perspectives on the Epidemiology of Gout and Hyperuricemia. Hawaii J. Med. Public Health 2019, 78, 71–76.
- Singh, J.A. Racial and gender disparities among patients with gout. Curr. Rheumatol. Rep. 2013, 15, 307.
- Zhu, Y.; Pandya, B.J.; Choi, H.K. Comorbidities of Gout and Hyperuricemia in the US General Population: NHANES 2007–2008. Am. J. Med. 2012, 125, 679–687.
- Mikuls, T.R.; Cheetham, T.C.; Levy, G.D.; Rashid, N.; Kerimian, A.; Low, K.J.; Coburn, B.W.; Redden, D.T.; Saag, K.G.; Foster, P.J.; et al. Adherence and Outcomes with Urate-Lowering Therapy: A Site-Randomized Trial. Am. J. Med. 2019, 132, 354–361.
- Huang, I.J.; Liew, J.W.; Morcos, M.B.; Zuo, S.; Crawford, C.; Bays, A.M. Pharmacist-managed titration of urate-lowering therapy to streamline gout management. Rheumatol. Int. 2019, 39, 1637–1641.
- Goldfien, R.; Pressman, A.; Jacobson, A.; Ng, M.; Avins, A. A Pharmacist-Staffed, Virtual Gout Management Clinic for Achieving Target Serum Uric Acid Levels: A Randomized Clinical Trial. Perm. J. 2016, 20, 15–234.
- Roman, Y.M. COVID-19 pandemic: The role of community-based pharmacy practice in health equity. Int. J. Clin. Pharm. 2022.
- Alrajeh, K.Y.; Roman, Y.M. Pharmacogenetic Perspective for Optimal Gout Management. Future Pharmacol. 2022, 2, 135–152.
- Saito, Y.; Stamp, L.K.; Caudle, K.E.; Hershfield, M.S.; McDonagh, E.M.; Callaghan, J.T.; Tassaneeyakul, W.; Mushiroda, T.; Kamatani, N.; Goldspiel, B.R.; et al. Clinical Pharmacogenetics Implementation Consortium (CPIC) guidelines for human leukocyte antigen B (HLA-B) genotype and allopurinol dosing: 2015 update. Clin. Pharmacol. Ther. 2016, 99, 36–37.
- Roberts, R.L.; Wallace, M.C.; Phipps-Green, A.J.; Topless, R.; Drake, J.M.; Tan, P.; Dalbeth, N.; Merriman, T.R.; Stamp, L.K. ABCG2 loss-of-function polymorphism predicts poor response to allopurinol in patients with gout. Pharm. J 2017, 17, 201–203.
- Wen, C.; Yee, S.; Liang, X.; Hoffmann, T.; Kvale, M.; Banda, Y.; Jorgenson, E.; Schaefer, C.; Risch, N.; Giacomini, K. Genome-wide association study identifies ABCG2 (BCRP) as an allopurinol transporter and a determinant of drug response. Clin. Pharmacol. Ther. 2015, 97, 518–525.
- Kurzawski, M.; Dziewanowski, K.; Safranow, K.; Drozdzik, M. Polymorphism of genes involved in purine metabolism (XDH, AOX1, MOCOS) in kidney transplant recipients receiving azathioprine. Ther. Drug Monit. 2012, 34, 266–274.
- Roman, Y.; Culhane-Pera, K.; Lo, M.; Yang, S.; Yang, J.; Lo, M.; Straka, R. The Impact of Rs505802 for Slc22a12 on Oxipurinol and Uric Acid Disposition in Hmong Patients on Allopurinol from the Genetics of Hyperuricemia Therapy in Hmong (Gouth) Study. In Clinical Pharmacology & Therapeutics; Wiley-Blackwell: Hoboken, NJ, USA, 2017; p. S48.
- Dube, M.P.; Legault, M.A.; Lemacon, A.; Lemieux Perreault, L.P.; Fouodjio, R.; Waters, D.D.; Kouz, S.; Pinto, F.J.; Maggioni, A.P.; Diaz, R.; et al. Pharmacogenomics of the Efficacy and Safety of Colchicine in COLCOT. Circ. Genom. Precis. Med. 2021, 14, e003183.
