CD24 and its ligand Siglec-10 were described as an innate immune checkpoint in carcinoma. Here, we investigated this axis in B-cell lymphoma by assessing CD24 expression and evaluating pro-phagocytic effects of CD24 antibody treatment in comparison to hallmark immune checkpoint CD47. In mantle cell lymphoma (MCL) and follicular lymphoma patients, high mRNA expression of CD24 correlated with poor overall survival, whereas CD47 expression did not. Conversely, CD24 expression did not correlate with survival in diffuse large B-cell lymphoma (DLBCL), whereas CD47 did. CD24 was also highly expressed on MCL cell lines, where treatment with CD24 antibody clones SN3 or ML5 potently induced phagocytosis, with SN3 yielding >90% removal of MCL cells and triggering phagocytosis of primary patient-derived MCL cells by autologous macrophages. Treatment with CD24 mAb was superior to CD47 mAb in MCL and was comparable in magnitude to the effect observed in carcinoma lines. Reversely, CD24 mAb treatment was less effective than CD47 mAb treatment in DLBCL. Finally, phagocytic activity of clone SN3 appeared at least partly independent of antibody-dependent cellular phagocytosis (ADCP), suggesting CD24/Siglec-10 checkpoint activity, whereas clone ML5 solely induced ADCP. In conclusion, CD24 is an immunotherapeutic target of potential clinical relevance for MCL, but not DLBCL.
- mantle cell lymphoma
- CD24
- immunotherapy
- immune checkpoint
- phagocytosis
Introduction
Results
CD24 Is Expressed in Several B-Cell Lymphomas, Being Most Highly Expressed in MCL, Where It Correlates with Poor Prognosis in Contrast to Hallmark Immune Checkpoint CD47
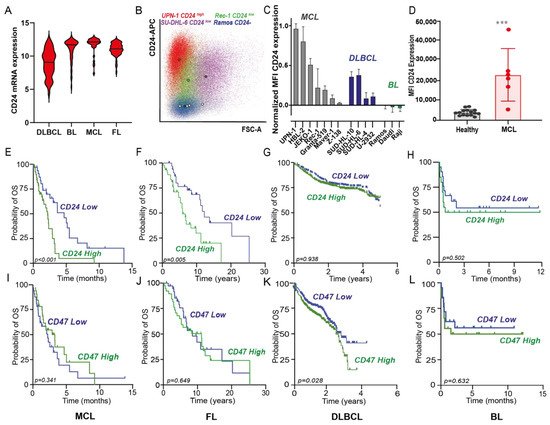
Figure 1. CD24 expression in several non-Hodgkin’s lymphomas (NHL) and correlation with survival. (A) CD24 mRNA expression (2log) in 4 subtypes of NHL, namely diffuse large B-cell lymphoma (DLBCL; n = 94), Burkitt lymphoma (BL; n = 58), mantle cell lymphoma (MCL; n = 42), and follicular lymphoma (FL; n = 64). (B) Dot-plot diagram of forward scatter vs. CD24 expression of representative cell line panel, illustrating high CD24 expression (UPN-1, red), low CD24 expression (Rec-1, green; SU-DHL-6, violet), or lack of CD24 expression (Ramos, blue) compared to isotype controls (gray). The colored circles indicate the mean value of the population. (C) Surface CD24 expression (mean ± SD of corrected MFI values, n = 3) in MCL, DLBCL and BL cell lines. Expression was normalized to the highest value, corresponding CD24 expression of UPN-1. (D) Surface CD24 expression (MFI values) of MCL blast cells (CD45+CD19+CD5+) (n = 6) and healthy donors (n = 13) (CD45+CD19+) cells. Mean ± SD, Student’s t-test, *** = p < 0.001 (E–H) Kaplan–Meier plots for CD24 and (I–L) CD47 expression in an MCL patient data set (n= 71) (E,I), an FL patient data set (n = 77) (F,J), a DLBCL patient data set (n = 1017) (G,K), and BL patient data set (n = 41) (H,L); log-rank test performed in all cases, with p < 0.05 considered significant.
CD24 Is a Target for Reactivation of Phagocytosis in MCL, with a Superior Effect Than CD47 Antibody Treatment
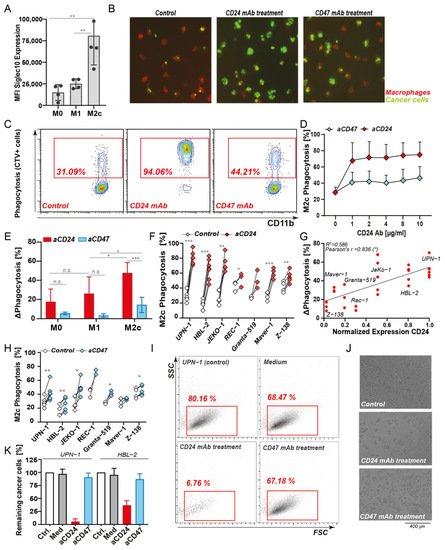
Figure 2. Phagocytic uptake and clearance of MCL cell lines upon CD24 and CD47 antibody treatment. (A) Levels of Siglec10 expression in M0, M1, and M2c type macrophages. (B) Microscopy images of macrophage-mediated phagocytosis of UPN-1 cells in M2c mixed culture (control, left), CD24 antibody SN3 (middle) or CD47 mAb InhibRx treatment (right), with macrophages in red (CD11b) and cancer cells in green (CSFE). (C) Flow cytometry analysis of UPN-1 phagocytosis with cell trace violet (CTV)-stained cancer cells and macrophages stained with CD11b-APC. Level of phagocytosis was determined as the percentage of CD11b+CTV+ cells. (D) Dose range of CD24 antibody SN3 and CD47 antibody InhibRx treatment in UPN-1 cells. (E) Phagocytosis levels of UPN-1 cells by M0, M1, and M2c-polarized macrophages upon SN3 and InhibRx treatment. (F) Percentage of phagocytosis upon CD24 SN3 antibody treatment vs. medium control of several MCL cell lines by M2c macrophages (of at least 3 independent donors). (G) Correlation between CD24 expression and increase in phagocytosis upon CD24 SN3 treatment in MCL cell lines. CD24 expression was normalized to the highest value, corresponding to UPN-1 CD24 expression. Pearson’s r = 0.836 (*) and linear regression p < 0.05. (H) Percentage of phagocytosis upon CD47 InhibRx treatment vs. medium control by M2c macrophages (of at least 3 independent donors) in several MCL cell lines. (I) Flow cytometry diagram showing the percentage of remaining UPN1 cell line after 2 h phagocytosis. (J) Bright-field microscopy pictures showing remaining UPN-1 cells after o/n co-culture with macrophages. (K) Percentage of remaining UPN-1 and HBL-2 cells in different experimental conditions (cancer cells only (Ctrl), mixed culture with medium control (Med), CD24 antibody SN3, and CD47 antibody InhibRx. All averaged values represent the mean ± SD of at least 3 independent experiments. Unless specified otherwise, statistics were performed using a two-sided paired Student’s t-test. ns: not significant; * p < 0.05; ** p < 0.01; *** p < 0.001.
CD24 mAb Treatment Increased Phagocytosis of Primary MCL Blasts by Autologous Macrophages and PMNs, but Did Not Induce High Level of Phagocytosis of Healthy Cells
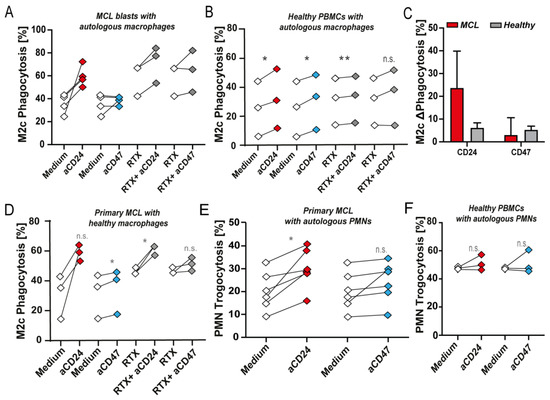
Figure 3. CD24 and CD47 antibody-mediated phagocytosis of MCL and healthy blasts by primary patient-derived autologous and allogeneic healthy donor macrophages. (A) Phagocytosis of MCL blasts by autologous macrophages upon CD24 mAb SN3 or CD47 mAb InhibRx treatment (n = 4) and combination treatment with RTX (n = 3). (B) Phagocytosis of healthy PBMCs by autologous macrophages upon CD24 mAb SN3 or CD47 mAb InhibRx treatment and in combination with RTX. (n = 3). (C) Comparison between phagocytosis levels induced upon CD24 and CD47 antibody treatment of MCL blasts (red) and healthy PBMCs (gray). (D) Phagocytosis of MCL blasts co-cultured with macrophages from healthy donors upon treatment with CD24 mAb SN3 or CD47 mAb InhibRx and in combination with RTX. (n = 3). (E) Trogocytosis of MCL blasts by autologous PMNs upon treatment with CD24 mAb SN3 or CD47 mAb InhibRx (n = 5). Statistical testing was performed using paired Student’s t-test. (F) Trogocytosis of healthy PBMCs by autologous PMNs upon treatment with CD24 mAb SN3 or CD47 mAb InhibRx (n = 3). Statistical testing was performed using paired Student’s t-test. Where indicated, n.s. = non-significant, * = p < 0.05; ** = p < 0.01.
CD24 Antibody-Mediated Phagocytosis Is Superior to CD47 Checkpoint Targeting in MCL and Carcinoma, but Not in DLBCL
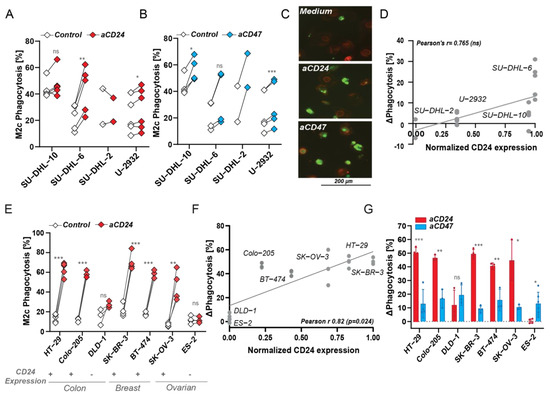
Figure 4. CD24 expression levels positively correlated with CD24 antibody-induced phagocytosis. (A) Percentage of phagocytosis upon CD24 SN3 antibody treatment vs. medium control by M2c macrophages (independent donors) in several DLBCL cell lines. Paired t-test. (B) Percentage of phagocytosis upon CD47 InhibRx antibody treatment vs. medium control by M2c macrophages (independent donors) in several DLBCL cell lines. Paired t-test. (C) Confocal microscopy images of phagocytosis of SU-DHL-6 where macrophages are in red and cancer cells are visible in green. (D) Correlation between CD24 expression and increase in phagocytosis upon CD24 SN3 treatment in DLBCL cell lines. CD24 expression was normalized to the highest value, corresponding to UPN-1 CD24 expression. Pearson’s r = 0.765 (ns) and linear regression p > 0.05. (E) Percentage of phagocytosis upon CD24 SN3 treatment vs. medium control by M2c macrophages (independent donors) in several colon (HT-29, Colo-205, DLD-1), breast (SK-BR-3, BT-474), and ovarian (SK-OV-3, ES-2) cell lines. Any effect was observed in CD24 negative cell lines (DLD-1, ES-2). Paired t-test. (F) Correlation between CD24 expression and increase in phagocytosis upon CD24 SN3 treatment in several colon (HT-29, Colo-205, DLD-1), breast (SK-BR-3, BT-474), and ovarian (SK-OV-3, ES2) cell lines. CD24 expression was normalized to the highest value, corresponding to SKBR3 CD24 expression. Pearson’s r = 0.82 (*) and linear regression p < 0.05. (G) Delta increase in phagocytosis compared to medium control upon CD24 and CD47 antibody treatment in several colon (HT-29, Colo-205, DLD-1), breast (SK-BR-3, BT-474), and ovarian (SK-OV-3, ES-2) cell lines. Student’s t-test. Where indicated, n.s. = non-significant, * = p < 0.05; ** = p < 0.01; *** = p < 0.001.
Induction of Phagocytosis of CD24 Expressing Cells Is Only in Part an Effect of Breaking CD24-Siglec-10 ‘Don’t Eat Me’ Signaling
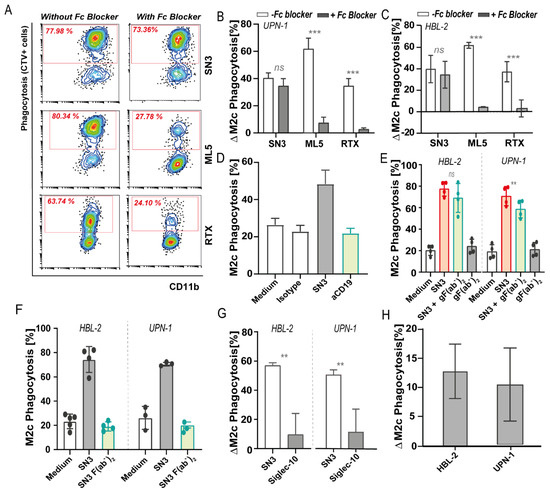
Figure 5. CD24 antibody treatment with two different murine anti-CD24 clones (SN3 and ML5) and Siglec-10 disruption of CD24/Siglec10 axis. (A) Flow cytometry diagrams showing the percentage of phagocytosis of UPN-1 cells upon CD24 antibody treatment with SN3 and ML5 clones by M2c macrophages in the presence or absence of high concentrations of Fc blocker. Rituximab (RTX) (anti-CD20) antibody was used as a control. (B) Increase in phagocytosis compared to medium control of UPN-1 cells upon CD24 antibody treatment with SN3 and ML5 antibody clones by M2c macrophages in the presence (gray) or absence (white) of high concentrations of Fc blocker. (C) Increase in phagocytosis compared to medium control of HBL-2 cells upon CD24 antibody treatment with SN3 and ML5 antibody clones by M2c macrophages in the presence (gray) or absence (white) of high concentrations of Fc blocker. n = 3, mean ± SD. n = 3, mean ± SD. Paired t-test, with p < 0.05 significant. (D) Phagocytosis of HBL-2 cells upon anti-CD24 (1 µg/mL, red) or anti-CD19 (10 µg/mL, green) treatment, being both mouse IgG1 antibodies. (E) Phagocytosis of HBL-2 and UPN-1 cells upon anti-CD24 treatment (SN3 clone) (red), same antibody pre-incubated with goat F(ab’)2 against mouse IgG Fc domain (gF(ab’)2) (green) or the goat F(ab’)2 alone (gray). Paired t-test, with p < 0.05 significant. (F) Phagocytosis levels of HBL-2 and UPN-1 cells upon CD24 SN3 treatment with the complete antibody (red) or F(ab’)2 preparations of the same antibody clone (SN3) (green). (G) Phagocytic uptake by M2c macrophages upon CD24 treatment with recombinant human Siglec-10 (His tagged) protein of HBL-2 and UPN-1 cells. (H) Increase in phagocytosis compared to medium control of HBL-2 and UPN-1 cells co-cultured with M2c macrophages previously incubated with 10 µg/mL of anti-Siglec-10 antibodies (5G6 clone). n = 3, mean ± SD. Where indicated, n.s. = non-significant, ** = p < 0.01; *** = p < 0.001.
Discussion
Conclusions
References
- Robert, C. A decade of immune-checkpoint inhibitors in cancer therapy. Nat. Commun. 2020, 11, 3801. [Google Scholar] [CrossRef] [PubMed]
- Lentz, R.W.; Colton, M.D.; Mitra, S.S.; Messersmith, W.A. Innate Immune Checkpoint Inhibitors: The Next Breakthrough in Medical Oncology? Mol. Cancer Ther. 2021, 20, 961–974. [Google Scholar] [CrossRef] [PubMed]
- Cendrowicz, E.; Sas, Z.; Bremer, E.; Rygiel, T.P. The Role of Macrophages in Cancer Development and Therapy. Cancers 2021, 13, 1946. [Google Scholar] [CrossRef] [PubMed]
- Tong, B.; Wang, M. CD47 is a novel potent immunotherapy target in human malignancies: Current studies and future promises. Future Oncol. 2018, 14, 2179–2188. [Google Scholar] [CrossRef]
- Cendrowicz, E.; Jacob, L.; Greenwald, S.; Tamir, A.; Pecker, I.; Tabakman, R.; Ghantous, L.; Tamir, L.; Kahn, R.; Avichzer, J.; et al. DSP107 combines inhibition of CD47/SIRPalpha axis with activation of 4-1BB to trigger anti-cancer immunity. J. Exp. Clin. Cancer Res. 2022, 41, 97. [Google Scholar] [CrossRef]
- Jalil, A.R.; Andrechak, J.C.; Discher, D.E. Macrophage checkpoint blockade: Results from initial clinical trials, binding analyses, and CD47-SIRPalpha structure-function. Antib. Ther. 2020, 3, 80–94. [Google Scholar] [CrossRef]
- Sikic, B.I.; Lakhani, N.; Patnaik, A.; Shah, S.A.; Chandana, S.R.; Rasco, D.; Colevas, A.D.; O’Rourke, T.; Narayanan, S.; Papadopoulos, K.; et al. First-in-Human, First-in-Class Phase I Trial of the Anti-CD47 Antibody Hu5F9-G4 in Patients With Advanced Cancers. J. Clin. Oncol. 2019, 37, 946–953. [Google Scholar] [CrossRef]
- Tseng, D.; Volkmer, J.P.; Willingham, S.B.; Contreras-Trujillo, H.; Fathman, J.W.; Fernhoff, N.B.; Seita, J.; Inlay, M.A.; Weiskopf, K.; Miyanishi, M.; et al. Anti-CD47 antibody-mediated phagocytosis of cancer by macrophages primes an effective antitumor T-cell response. Proc. Natl. Acad. Sci. USA 2013, 110, 11103–11108. [Google Scholar] [CrossRef]
- Advani, R.; Flinn, I.; Popplewell, L.; Forero, A.; Bartlett, N.L.; Ghosh, N.; Kline, J.; Roschewski, M.; LaCasce, A.; Collins, G.P.; et al. CD47 Blockade by Hu5F9-G4 and Rituximab in Non-Hodgkin’s Lymphoma. N. Engl. J. Med. 2018, 379, 1711–1721. [Google Scholar] [CrossRef]
- Barkal, A.A.; Weiskopf, K.; Kao, K.S.; Gordon, S.R.; Rosental, B.; Yiu, Y.Y.; George, B.M.; Markovic, M.; Ring, N.G.; Tsai, J.M.; et al. Engagement of MHC class I by the inhibitory receptor LILRB1 suppresses macrophages and is a target of cancer immunotherapy. Nat. Immunol. 2018, 19, 76–84. [Google Scholar] [CrossRef]
- Chen, H.M.; van der Touw, W.; Wang, Y.S.; Kang, K.; Mai, S.; Zhang, J.; Alsina-Beauchamp, D.; Duty, J.A.; Mungamuri, S.K.; Zhang, B.; et al. Blocking immunoinhibitory receptor LILRB2 reprograms tumor-associated myeloid cells and promotes antitumor immunity. J. Clin. Investig. 2018, 128, 5647–5662. [Google Scholar] [CrossRef] [PubMed]
- Yin, S.S.; Gao, F.H. Molecular Mechanism of Tumor Cell Immune Escape Mediated by CD24/Siglec-10. Front. Immunol. 2020, 11, 1324. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Ma, H.; Zhang, J.; Zhu, L.; Wang, C.; Yang, Y. Unraveling the roles of CD44/CD24 and ALDH1 as cancer stem cell markers in tumorigenesis and metastasis. Sci. Rep. 2017, 7, 13856. [Google Scholar] [CrossRef] [PubMed]
- Salaria, S.; Means, A.; Revetta, F.; Idrees, K.; Liu, E.; Shi, C. Expression of CD24, a Stem Cell Marker, in Pancreatic and Small Intestinal Neuroendocrine Tumors. Am. J. Clin. Pathol. 2015, 144, 642–648. [Google Scholar] [CrossRef] [PubMed]
- Yang, W.; Kim, D.; Kim, D.K.; Choi, K.U.; Suh, D.S.; Kim, J.H. Therapeutic Strategies for Targeting Ovarian Cancer Stem Cells. Int. J. Mol. Sci. 2021, 22, 5059. [Google Scholar] [CrossRef]
- Overdevest, J.B.; Knubel, K.H.; Duex, J.E.; Thomas, S.; Nitz, M.D.; Harding, M.A.; Smith, S.C.; Frierson, H.F.; Conaway, M.; Theodorescu, D. CD24 expression is important in male urothelial tumorigenesis and metastasis in mice and is androgen regulated. Proc. Natl. Acad. Sci. USA 2012, 109, E3588–E3596. [Google Scholar] [CrossRef]
- Altevogt, P.; Sammar, M.; Huser, L.; Kristiansen, G. Novel insights into the function of CD24: A driving force in cancer. Int. J. Cancer 2021, 148, 546–559. [Google Scholar] [CrossRef]
- Fang, X.; Zheng, P.; Tang, J.; Liu, Y. CD24: From A to Z. Cell Mol. Immunol. 2010, 7, 100–103. [Google Scholar] [CrossRef]
- Barkal, A.A.; Brewer, R.E.; Markovic, M.; Kowarsky, M.; Barkal, S.A.; Zaro, B.W.; Krishnan, V.; Hatakeyama, J.; Dorigo, O.; Barkal, L.J.; et al. CD24 signalling through macrophage Siglec-10 is a target for cancer immunotherapy. Nature 2019, 572, 392–396. [Google Scholar] [CrossRef]
- Kwon, M.J.; Han, J.; Seo, J.H.; Song, K.; Jeong, H.M.; Choi, J.S.; Kim, Y.J.; Lee, S.H.; Choi, Y.L.; Shin, Y.K. CD24 Overexpression Is Associated with Poor Prognosis in Luminal A and Triple-Negative Breast Cancer. PLoS ONE 2015, 10, e0139112. [Google Scholar] [CrossRef]
- Zhang, P.; Zheng, P.; Liu, Y. Amplification of the CD24 Gene Is an Independent Predictor for Poor Prognosis of Breast Cancer. Front. Genet. 2019, 10, 560. [Google Scholar] [CrossRef] [PubMed]
- Tarhriz, V.; Bandehpour, M.; Dastmalchi, S.; Ouladsahebmadarek, E.; Zarredar, H.; Eyvazi, S. Overview of CD24 as a new molecular marker in ovarian cancer. J. Cell Physiol. 2019, 234, 2134–2142. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.L.; Guo, C.R.; Su, W.Y.; Chen, Y.X.; Xu, J.; Fang, J.Y. CD24 Overexpression Related to Lymph Node Invasion and Poor Prognosis of Colorectal Cancer. Clin. Lab. 2018, 64, 497–505. [Google Scholar] [CrossRef] [PubMed]
- Kay, R.; Rosten, P.M.; Humphries, R.K. CD24, a signal transducer modulating B cell activation responses, is a very short peptide with a glycosyl phosphatidylinositol membrane anchor. J. Immunol. 1991, 147, 1412–1416. [Google Scholar] [PubMed]
- Lingwood, D.; Simons, K. Lipid rafts as a membrane-organizing principle. Science 2010, 327, 46–50. [Google Scholar] [CrossRef] [PubMed]
- Aigner, S.; Ruppert, M.; Hubbe, M.; Sammar, M.; Sthoeger, Z.; Butcher, E.C.; Vestweber, D.; Altevogt, P. Heat stable antigen (mouse CD24) supports myeloid cell binding to endothelial and platelet P-selectin. Int. Immunol. 1995, 7, 1557–1565. [Google Scholar] [CrossRef]
- Myung, J.H.; Gajjar, K.A.; Pearson, R.M.; Launiere, C.A.; Eddington, D.T.; Hong, S. Direct measurements on CD24-mediated rolling of human breast cancer MCF-7 cells on E-selectin. Anal. Chem. 2011, 83, 1078–1083. [Google Scholar] [CrossRef]
- Kristiansen, G.; Machado, E.; Bretz, N.; Rupp, C.; Winzer, K.J.; Konig, A.K.; Moldenhauer, G.; Marme, F.; Costa, J.; Altevogt, P. Molecular and clinical dissection of CD24 antibody specificity by a comprehensive comparative analysis. Lab. Investig. 2010, 90, 1102–1116. [Google Scholar] [CrossRef]
- Zhou, Q.; Wu, Y.; Nielsen, P.J.; Liu, Y. Homotypic interaction of the heat-stable antigen is not responsible for its co-stimulatory activity for T cell clonal expansion. Eur. J. Immunol. 1997, 27, 2524–2528. [Google Scholar] [CrossRef]
- Suzuki, T.; Kiyokawa, N.; Taguchi, T.; Sekino, T.; Katagiri, Y.U.; Fujimoto, J. CD24 induces apoptosis in human B cells via the glycolipid-enriched membrane domains/rafts-mediated signaling system. J. Immunol. 2001, 166, 5567–5577. [Google Scholar] [CrossRef]
- Mensah, F.F.K.; Armstrong, C.W.; Reddy, V.; Bansal, A.S.; Berkovitz, S.; Leandro, M.J.; Cambridge, G. CD24 Expression and B Cell Maturation Shows a Novel Link With Energy Metabolism: Potential Implications for Patients With Myalgic Encephalomyelitis/Chronic Fatigue Syndrome. Front. Immunol. 2018, 9, 2421. [Google Scholar] [CrossRef] [PubMed]
- Shapira, S.; Kazanov, D.; Mdah, F.; Yaakobi, H.; Herishanu, Y.; Perry, C.; Avivi, I.; Itchaki, G.; Shacham-Abulafia, A.; Raanani, P.; et al. Feasibly of CD24/CD11b as a Screening Test for Hematological Malignancies. J. Pers. Med. 2021, 11, 724. [Google Scholar] [CrossRef] [PubMed]
- Lancaster-Shorts, K.; Pirruccello, S. CD24 Expression in Follicular Lymphoma: An Alternative B-Cell Marker in Therapy Selected, Recurrent Lymphoma. Grad. Med. Educ. Res. J. 2020, 2, 65. [Google Scholar] [CrossRef]
- Jain, P.; Wang, M. Mantle cell lymphoma: 2019 update on the diagnosis, pathogenesis, prognostication, and management. Am. J. Hematol. 2019, 94, 710–725. [Google Scholar] [CrossRef] [PubMed]
- Maddocks, K. Update on mantle cell lymphoma. Blood 2018, 132, 1647–1656. [Google Scholar] [CrossRef] [PubMed]
- Hanel, W.; Epperla, N. Emerging therapies in mantle cell lymphoma. J. Hematol. Oncol. 2020, 13, 79. [Google Scholar] [CrossRef] [PubMed]
- Susanibar-Adaniya, S.; Barta, S.K. 2021 Update on Diffuse large B cell lymphoma: A review of current data and potential applications on risk stratification and management. Am. J. Hematol. 2021, 96, 617–629. [Google Scholar] [CrossRef] [PubMed]
- Qiao, L.Y.; Li, H.B.; Zhang, Y.; Shen, D.; Liu, P.; Che, Y.Q. CD24 Contributes to Treatment Effect in ABC-DLBCL Patients with R-CHOP Resistance. Pharmgenom. Pers. Med. 2021, 14, 591–599. [Google Scholar] [CrossRef]
- Ma, M.C.J.; Tadros, S.; Bouska, A.; Heavican, T.; Yang, H.; Deng, Q.; Moore, D.; Akhter, A.; Hartert, K.; Jain, N.; et al. Subtype-specific and co-occurring genetic alterations in B-cell non-Hodgkin lymphoma. Haematologica 2022, 107, 690–701. [Google Scholar] [CrossRef]
- Blenk, S.; Engelmann, J.C.; Pinkert, S.; Weniger, M.; Schultz, J.; Rosenwald, A.; Muller-Hermelink, H.K.; Muller, T.; Dandekar, T. Explorative data analysis of MCL reveals gene expression networks implicated in survival and prognosis supported by explorative CGH analysis. BMC Cancer 2008, 8, 106. [Google Scholar] [CrossRef]
- Glas, A.M.; Kersten, M.J.; Delahaye, L.J.; Witteveen, A.T.; Kibbelaar, R.E.; Velds, A.; Wessels, L.F.; Joosten, P.; Kerkhoven, R.M.; Bernards, R.; et al. Gene expression profiling in follicular lymphoma to assess clinical aggressiveness and to guide the choice of treatment. Blood 2005, 105, 301–307. [Google Scholar] [CrossRef] [PubMed]
- Dave, S.S.; Fu, K.; Wright, G.W.; Lam, L.T.; Kluin, P.; Boerma, E.J.; Greiner, T.C.; Weisenburger, D.D.; Rosenwald, A.; Ott, G.; et al. Molecular diagnosis of Burkitt’s lymphoma. N. Engl. J. Med. 2006, 354, 2431–2442. [Google Scholar] [CrossRef] [PubMed]
- Bouwstra, R.; He, Y.; de Boer, J.; Kooistra, H.; Cendrowicz, E.; Fehrmann, R.S.N.; Ammatuna, E.; Zu Eulenburg, C.; Nijland, M.; Huls, G.; et al. CD47 Expression Defines Efficacy of Rituximab with CHOP in Non-Germinal Center B-cell (Non-GCB) Diffuse Large B-cell Lymphoma Patients (DLBCL), but Not in GCB DLBCL. Cancer Immunol. Res. 2019, 7, 1663–1671. [Google Scholar] [CrossRef] [PubMed]
- Fadok, V.A.; de Cathelineau, A.; Daleke, D.L.; Henson, P.M.; Bratton, D.L. Loss of phospholipid asymmetry and surface exposure of phosphatidylserine is required for phagocytosis of apoptotic cells by macrophages and fibroblasts. J. Biol. Chem. 2001, 276, 1071–1077. [Google Scholar] [CrossRef] [PubMed]
- VanDerMeid, K.R.; Elliott, M.R.; Baran, A.M.; Barr, P.M.; Chu, C.C.; Zent, C.S. Cellular Cytotoxicity of Next-Generation CD20 Monoclonal Antibodies. Cancer Immunol. Res. 2018, 6, 1150–1160. [Google Scholar] [CrossRef] [PubMed]
- Invivogen. <review-ImmunoglobulinG-invivogen.pdf>. 2011. Available online: https://www.invivogen.com/review-antibody-generation (accessed on 29 April 2022).
- Waldmann, T.A. Monoclonal antibodies in diagnosis and therapy. Science 1991, 252, 1657–1662. [Google Scholar] [CrossRef] [PubMed]
- Benkerrou, M.; Jais, J.P.; Leblond, V.; Durandy, A.; Sutton, L.; Bordigoni, P.; Garnier, J.L.; Le Bidois, J.; Le Deist, F.; Blanche, S.; et al. Anti-B-cell monoclonal antibody treatment of severe posttransplant B-lymphoproliferative disorder: Prognostic factors and long-term outcome. Blood 1998, 92, 3137–3147. [Google Scholar] [CrossRef]
- Chen, G.Y.; Tang, J.; Zheng, P.; Liu, Y. CD24 and Siglec-10 selectively repress tissue damage-induced immune responses. Science 2009, 323, 1722–1725. [Google Scholar] [CrossRef]
- Forgione, R.E.; Di Carluccio, C.; Guzman-Caldentey, J.; Gaglione, R.; Battista, F.; Chiodo, F.; Manabe, Y.; Arciello, A.; Del Vecchio, P.; Fukase, K.; et al. Unveiling Molecular Recognition of Sialoglycans by Human Siglec-10. iScience 2020, 23, 101231. [Google Scholar] [CrossRef]
- Xiao, N.; Zhu, X.; Li, K.; Chen, Y.; Liu, X.; Xu, B.; Lei, M.; Xu, J.; Sun, H.C. Blocking siglec-10(hi) tumor-associated macrophages improves anti-tumor immunity and enhances immunotherapy for hepatocellular carcinoma. Exp. Hematol. Oncol. 2021, 10, 36. [Google Scholar] [CrossRef]
- Smith, S.C.; Oxford, G.; Wu, Z.; Nitz, M.D.; Conaway, M.; Frierson, H.F.; Hampton, G.; Theodorescu, D. The metastasis-associated gene CD24 is regulated by Ral GTPase and is a mediator of cell proliferation and survival in human cancer. Cancer Res. 2006, 66, 1917–1922. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, P.J.; Lorenz, B.; Muller, A.M.; Wenger, R.H.; Brombacher, F.; Simon, M.; von der Weid, T.; Langhorne, W.J.; Mossmann, H.; Kohler, G. Altered erythrocytes and a leaky block in B-cell development in CD24/HSA-deficient mice. Blood 1997, 89, 1058–1067. [Google Scholar] [CrossRef] [PubMed]
- Ayre, D.C.; Christian, S.L. CD24: A Rheostat That Modulates Cell Surface Receptor Signaling of Diverse Receptors. Front. Cell Dev. Biol. 2016, 4, 146. [Google Scholar] [CrossRef] [PubMed]
- Pallegar, N.K.; Ayre, D.C.; Christian, S.L. Repression of CD24 surface protein expression by oncogenic Ras is relieved by inhibition of Raf but not MEK or PI3K. Front. Cell Dev. Biol. 2015, 3, 47. [Google Scholar] [CrossRef]
- Bretz, N.P.; Salnikov, A.V.; Perne, C.; Keller, S.; Wang, X.; Mierke, C.T.; Fogel, M.; Erbe-Hofmann, N.; Schlange, T.; Moldenhauer, G.; et al. CD24 controls Src/STAT3 activity in human tumors. Cell Mol. Life Sci. 2012, 69, 3863–3879. [Google Scholar] [CrossRef]
- Lan, H.; Li, W.; Jiang, H.; Yang, Y.; Zheng, X. Intracellular signaling transduction pathways triggered by a well-known anti-GHR monoclonal antibody, Mab263, in vitro and in vivo. Int. J. Mol. Sci. 2014, 15, 20538–20554. [Google Scholar] [CrossRef]
- Tchernychev, B.; Furie, B.; Furie, B.C. Peritoneal macrophages express both P-selectin and PSGL-1. J. Cell Biol. 2003, 163, 1145–1155. [Google Scholar] [CrossRef]
- Finas, D.; Huszar, M.; Agic, A.; Dogan, S.; Kiefel, H.; Riedle, S.; Gast, D.; Marcovich, R.; Noack, F.; Altevogt, P.; et al. L1 cell adhesion molecule (L1CAM) as a pathogenetic factor in endometriosis. Hum. Reprod. 2008, 23, 1053–1062. [Google Scholar] [CrossRef]
- Went, P.; Dellas, T.; Bourgau, C.; Maurer, R.; Augustin, F.; Tzankov, A.; Dirnhofer, S. [Expression profile and prognostic significance of CD24, p53 and p21 in lymphomas. A tissue microarray study of over 600 non-Hodgkin lymphomas]. Dtsch. Med. Wochenschr. 2004, 129, 2094–2099. [Google Scholar] [CrossRef]
- Yao, Y.; Xu, X.H.; Jin, L. Macrophage Polarization in Physiological and Pathological Pregnancy. Front. Immunol. 2019, 10, 792. [Google Scholar] [CrossRef]
- Porta, C.; Riboldi, E.; Ippolito, A.; Sica, A. Molecular and epigenetic basis of macrophage polarized activation. Semin. Immunol. 2015, 27, 237–248. [Google Scholar] [CrossRef] [PubMed]
- Iribarren, K.; Buque, A.; Mondragon, L.; Xie, W.; Levesque, S.; Pol, J.; Zitvogel, L.; Kepp, O.; Kroemer, G. Anticancer effects of anti-CD47 immunotherapy in vivo. Oncoimmunology 2019, 8, 1550619. [Google Scholar] [CrossRef] [PubMed]
