In order to contribute to the mitigation of COVID-19 symptoms, the pharmaceutical industry aims to develop antiviral drugs to inhibit the SARS-CoV-2 replication and produce anti-inflammatory medications that will inhibit the acute respiratory distress syndrome (ARDS), which is the primary cause of mortality among the COVID-19 patients. Licorice (Glycyrrhiza glabra), which belongs to the shrub category, whose phytochemicals have shown antiviral and anti-inflammatory properties through previous studies. Phytochemicals from many other medicinal plants are also known to have similar properties, such as Sambucus nigarac, Desmodium canadense, Lamiaceae family, Asteraceae, Geraniaceae, etc. but licorice has explicitly been suggested due to its: (i) considerable antiviral property against several viruses, including SARS-CoV, (ii) strong anti-inflammatory property, which has been observed in many rat model studies, (iii) autophagy-enhancing mechanism, (iv) established use in Chinese and Indian Ayurvedic medicines, and (v) wide distribution.
- ARDS
- antiviral drug
- anti-inflammatory drug
- coronavirus
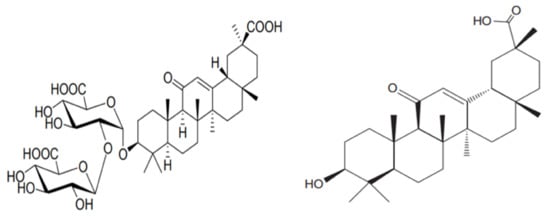
- glycyrrhizic acid
- glycyrrhetinic acid
- medicinal plants
1. Licorice (Glycyrrhiza glabra)

| Bioactive Compounds | Properties | References |
|---|---|---|
| Glycerrhizin (GL) | Antimicrobial | [26][27][28] |
| 18β-Glycerrhitinic acid | Antimicrobial, anti-inflammatory | |
| (GA) | Against Helicobacter pylori, | [29][30][31] |
| MRSA, | ||
| Clarithromycin-resistant H. pylori | ||
| 18α-GC, 18β-GC | Anti-inflammatory | |
| Flavonoids (13 Ns below) | Anti-inflammatory | |
| Licochalcone A/B/C/D/E, isoliquiritigenin (ISL) echinatin (EC), glabridin (GLD), soangustone A (ISOA), licoricidin (LID), licorisoflavan A (LIA), dehydroglyasperin C (DGC), & dehydroglyasperin D (DGD) Glabridin |
Antimicrobial, anti-inflammatory | [32] |
| Antimicrobial | [33] | |
| Aqueous extract | B. Subtilis and E. Coli | [34] |
| Methanol extract | Phytopathogenic fungi | [35] |
| Glycyrhetinic acid | MRSA | [30] |
| Licochalcone and Anti-fungal | [36] | |
| Acetate root extract | K. pneumonia and A. baylyi | [37] |
| Glabron | ||
| Licochalcone A/C/E | Staphylococcus aureus | [38] |
| Glycyrrhizin | Helicobacter pylori | [39] |
| 18β-Glycerrhetinic acid | Clarithromycin-resistant H. pylori | [31] |
2. Antimicrobial Activity
2.1. Antiviral Activity
In Vitro Studies
| Compounds in Licorice | Antiviral Property against | Reference |
| Glycyrrhizic acid | SARS-CoV | [57] |
| Glycyrrhizic acid derivatives | SARS-CoV | [56] |
| Glycyrrhizic acid | Hepatitis A (HAV) | [59] |
| Glycyrrhizic acid | Hepatitis B (HBV) | [27][60][61] |
| Glycyrrhizic acid | Hepatitic C virus | [47][48][62][63] |
| Glycyrrhizic acid | Human immune deficiency (HIV) Virus | [49][64][65][66] |
| Alkali root extract | HIV | [55] |
| Glycyrrhizic acid | Herpes viridae (varicella) | [67] |
| Zoster virus (VZV) | [68] | |
| Epstien-Barr virus (EBV) | [68] | |
| Cytomegalovirus (CMV) | [69] | |
| Coxasackievirus B3 (CVB3) | [70] | |
| Coxasackievirus A16 (CVA16) | [2] | |
| Glycyrrhizic acid | H5N1 influenza virus | [50][51][52] |
| Duck Hepatitis virus | [54] | |
| Herpes simplex virus–1 | [53] | |
| [71] | ||
| Water extract | HSV | [55] |
| 18β-glycyrrhetinic acid | Rotavirus | [72] |
In Vivo Studies
Human Studies
3. Anti-Inflammatory Property
3.1. In Vitro Studies
3.2. Animal Studies
| Compound | Tissue/Disease | Concentration | Method | Inhibition Rate | Reference(s) |
|---|---|---|---|---|---|
| In vitro studies | |||||
| 8β-GL | LPS (1 μg mL−1)-induced l Murine cell (RAW 264.7) |
75 μM | ELISA | 51%-NO, 51%-IL-1β, 49%-PGE2 & 42%-IL-6 | [90] |
| 18β-GL | LPS (1 μg mL−1)-induced murine Cell (RAW 264.7 macrophages) | 0.5 or 1 mg mL−1 | ELISA | Supress PGE2, PGI2,TXB2 & LTB4 | [101] |
| 18β-GL | Leishmania donovani infected Macrophages-BALB/c mice (age: 4–6 weeks) | 50 mg mL−1 | ELISA | 90.94%-parasite load | [102] |
| 18β-GA | LPS (1 μg mL−1)-induced murine cell (RAW 264.7 cell) |
75 μM | ELISA | 34%-NO | [90] |
| 18β-GA | 75 μM | ELISA | 58%-PEG2, 42%-1L-1β, 35%-IL-6, 34%-TNF-ἁ | [90] | |
| LID | LPS (0.1 μg mL−1)-induced U937 Cell line (human monoblastic leukaemia cell line) | 0.1, 0.5, 1 μg mL−1 | Decreased the secretion of IL-6, MMP-7, MMP-8, & MMP-9 | [103] | |
| DGC | Glutamte (5 nM)-induced HT22 cells |
2 μM | 2,7-DCF assay | Dose-dependent inhibition of ROS assay & WB production | [104] |
| LIA | LPS (0.1 μg mL−1)-induced U937 cell line (human monoblastic leukaemia cell line) |
0.1, 0.5, 1 μg mL−1 | Decreased the secretions of CCL5 @ (1 μg mL−1), MMP-7 @ (0.5, 1 μg mL−1) MMP-8 @ (0.5, 0.1, 1 μg mL−1) | [103] | |
| LCA | LPS (μg mL−1) induced murine cells (RAW 264.7) | 3 &10 μM | DCFH-DA | >80% PGE2 inhibition @ 10 μM fluorometric >50% NO inhibition at | [97] |
| 18β-GL | LPS (μg mL−1) induced | 75 μm | ELISA | 51% reduction in NO | [90] |
| Murine cells (RAW 264.7 cells) | 51% reduction in IL-1β 49% reduction in PGE2 46% reduction in TNF-ἁ 42% reduction in IL-6 |
||||
| 18β-GA | 75 μm | ELISA | 58% reduction in PEG2 | [105] | |
| Glabridin & isoliquiritigenin | 20-40 μg mL−1 | Cell culture & cell viability assay | anti-inflammatory activity is due to the individual or synergistic effects | ||
| In vivo studies | |||||
| Compounds | Inflammation Details | Models | Treatment | Result(s) | Reference |
| 18ἁ-GL | 20% paraquat poisoning solution @ 15 mg kg−1 | Sprague Dawley rats-male 30 Ns (180–200 g) | injection-IP 30 mg kg−1 | Significant decrease in intercellular adhesion molecules (ICAM-1) and matrix metalloproteinase-9 (MMP-9) | [93] |
| 18β-GL | LPS (1 mg kg−1)-Intratracheal installation | BALB/C mice (male 20–25 gm) | injection-IP 10, 25 & 50 mg kg−1 | Noted decrease in NO and MPO activity | [106] |
| LCA | Topical inflammation induced instantly at the posterior surface of the ear (using xylene 0.05 mL) | Kunming mice (20–25 gm) & Wistar rats (150–200 gm) | 50 mg kg−1 | Decrease in ear oedema rate by 30.3% | [107] |
| Human Studies | |||||
| GL | Hepatitis B virus induced inflammation | Humans | oral and IV (60 mL daily) for a week) | Effective in normalizing serum (for 7 days, later 3 days transaminases) | [61] |
| GL | Hepatitis C virus induced inflammation | Humans | 40 mL transaminases | Found effective in normalizing serum | [62] |
| GL | Hepatitis virus induced Inflammation | Humans | 40 mg of GL (IV) | Suppressed ALT | [26] |
3.3. Human Studies
4. Effect on Autophagy
This entry is adapted from the peer-reviewed paper 10.3390/plants10122600
References
- Fiore, C.; Eisenhut, M.; Krausse, R.; Ragazzi, E.; Pellati, D.; Armanini, D.; Bielenberg, J. Antiviral effects ofGlycyrrhiza species. Phytother. Res. Int. J. Devoted Pharmacol. Toxicol. Eval. Nat. Prod. Deriv. 2008, 22, 141–148.
- Wang, L.; Yang, R.; Yuan, B.; Liu, Y.; Liu, C. The antiviral and antimicrobial activities of licorice, a widely-used Chinese herb. Acta Pharm. Sin. B 2015, 5, 310–315.
- Gupta, V.K.; Fatima, A.; Faridi, U.; Negi, A.S.; Shanker, K.; Kumar, J.; Rahuja, N.; Luqman, S.; Sisodia, B.S.; Saikia, D.; et al. Antimicrobial potential of Glycyrrhiza glabra roots. J. Ethnopharmacol. 2008, 116, 377–380.
- Aly, A.M.; Al-Alousi, L.; Salem, H.A. Licorice: A possible anti-inflammatory and anti-ulcer drug. AAPS PharmSciTech 2005, 6, E74–E82.
- Hanrahan, C. Gale Encyclopedia of Alternative Medicine, Licorice ; Thomson Gale: Farmington Hills, MI, USA, 2001.
- Lust, J. The Herb Book; Bantam Books: New York, NY, USA, 1994.
- Yang, R.; Yuan, B.-C.; Ma, Y.-S.; Zhou, S.; Liu, Y. The anti-inflammatory activity of licorice, a widely used Chinese herb. Pharm. Biol. 2016, 55, 5–18.
- Dioscorides. De Materia Medica. 1555. Available online: http://bdh.bne.es/bnesearch/detalle/bdh0000037225 (accessed on 25 September 2021).
- Ayurvedic Pharmacopoeia of India. Vol. I: Part I, Department of Ayush, Ministry of Health and Family Welfare; Government of India: New Delhi, India, 2001.
- Obolentseva, G.V.; Litvinenko, I.V.I.; ammosov, A.S.; Popova, T.P.; Sampiev, A.M. Pharmacological and therapeutic properties of licorice preparations—A Review (Translated from Khimiko-Farmatsevticheskii Zhurnal). Med. Plants 1999, 33, 24–31. Available online: https://fdocuments.in/document/pharmacological-and-therapeutic-properties-of-licorice-preparations-a-review.html (accessed on 17 August 2021).
- RPRM. Resources of Plant Raw Materials in the USSR: Flowering Plants, Their Chemical Compositions, and Use; Nauka: Moscow, Russia, 1987.
- Somjen, D.; Tamir, S.; Vaya, J. Estrogen-Like Activity of Licorice Root Extract and Its Constituents. Oxidative Stress Dis. 2004, 14, 615–634.
- Van Rossum, T.G.; Vulto, A.G.; Hop, W.C.; Brouwer, J.T.; Niesters, H.; Schalm, S.W. Intravenous glycyrrhizin for the treatment of chronic hepatitis C: A double-blind, randomized, placebo-controlled phase I/II trial. J. Gastroenterol. Hepatol. 1999, 14, 1093–1099.
- Bahmani, M.; Rafieian-Kopaei, M.; Jeloudari, M.; Eftekhari, Z.; Delfan, B.; Zargaran, A.; Forouzan, S. A review of the health effects and uses of drugs of plant licorice (Glycyrrhiza glabra L.) in Iran. Asian Pac. J. Trop. Dis. 2014, 4, S847–S849.
- Zang, Y. Pharmacological Activities of Coumarin Compounds in Licorice: A Review. Nat. Prod. Commun. 2020, 15.
- Badkhane, Y.; Yadav, A.S.; Bajaj, A.; Sharma, A.K.; Raghuwanshi, D.K. Glycyrrhiza glabra L. a miracle medicinal herb. Indo Am. J. Pharm. Res. 2014, 4, 5808–5816.
- Dhingra, D.; Sharma, A. Evaluation of antidepressant-like activity of glycyrrhizin in mice. Indian J. Pharmacol. 2005, 37, 390.
- Fuhrman, B.; Volkova, N.; Kaplan, M.; Presser, D.; Attias, J.; Hayek, T.; Aviram, M. Antiatherosclerotic effects of licorice extract supplementation on hypercholesterolemic patients: Increased resistance of LDL to atherogenic modifications, reduced plasma lipid levels, and decreased systolic blood pressure. Nutrition 2002, 18, 268–273.
- Armanini, D.; De Palo, C.B.; Mattarello, M.J.; Spinella, P.; Zaccaria, M.; Ermolao, A.; Palermo, M.; Fiore, C.; Sartorato, P.; Francini-Pesenti, F.; et al. Effect of licorice on the reduction of body fat mass in healthy subjects. J. Endocrinol. Investig. 2003, 26, 646–650.
- Jung, J.-C.; Lee, Y.-H.; Kim, S.H.; Kim, K.-J.; Kim, K.-M.; Oh, S.; Jung, Y.-S. Hepatoprotective effect of licorice, the root of Glycyrrhiza uralensis Fischer, in alcohol-induced fatty liver disease. BMC Complement. Altern. Med. 2015, 16, 19.
- Thakur, V.; Nargis, S.; Gonzalez, M.; Pradhan, S.; Terreros, D.; Chattopadhyay, M. Role of Glycyrrhizin in the Reduction of Inflammation in Diabetic Kidney Disease. Nephron 2017, 137, 137–147.
- Li, X.; Sun, R.; Liu, R. Natural products in licorice for the therapy of liver diseases: Progress and future opportunities. Pharmacol. Res. 2019, 144, 210–226.
- Armanini, D.; Fiore, C.; Mattarello, M.J.; Bielenberg, J.; Palermo, M. History of the Endocrine Effects of Licorice. Exp. Clin. Endocrinol. Diabetes 2002, 110, 257–261.
- Li, Y.-J.; Chen, J.; Li, Y.; Li, Q.; Zheng, Y.-F.; Fu, Y.; Li, P. Screening and characterization of natural antioxidants in four Glycyrrhiza species by liquid chromatography coupled with electrospray ionization quadrupole time-of-flight tandem mass spectrometry. J. Chromatogr. A 2011, 1218, 8181–8191.
- Liu, H.; Wang, J.; Zhou, W.; Wang, Y.; Yang, L. Systems approaches and polypharmacology for drug discovery from herbal medicines: An example using licorice. J. Ethnopharmacol. 2013, 146, 773–793.
- Miyake, K.; Tango, T.; Ota, Y.; Mitamura, K.; Yoshiba, M.; Kako, M.; Hayashi, S.; Ikeda, Y.; Hayashida, N.; Iwabuchi, S.; et al. Efficacy of Stronger Neo-Minophagen C compared between two doses administered three times a week on patients with chronic viral hepatitis. J. Gastroenterol. Hepatol. 2002, 17, 1198–1204.
- Takahara, T.; Watanabe, A.; Shiraki, K. Effects of glycyrrhizin on hepatitis B surface antigen: A biochemical and morphological study. J. Hepatol. 1994, 21, 601–609.
- Zhang, L.; Wang, B.; Coordinating Group of SNMC Trial’s Society of Hepatology in China. Randomized clinical trial with two doses (100 and 40 ml) of Stronger Neo-Minophagen C in Chinese patients with chronic hepatitis B. Hepatol. Res. 2002, 24, 220–227.
- Celik, M.M.; Duran, N. An experimental in-vitro study to evaluate the anti-helicobacter activity of Glycyrrhetinic acid. Rev. Romana Med. Lab. 2019, 27, 63–71.
- Long, D.R.; Mead, J.; Hendricks, J.M.; Hardy, M.E.; Voyich, J.M. 18bGlycyrrhetinic acid inhibits methicillin-resistant Staphylococcus aureus survival and attenuates virulence gene expression. Antimicrob. Agents Chemother. 2013, 57, 241–247.
- Krausse, R.; Bielenberg, J.; Blaschek, W.; Ullmann, U. In vitro anti-Helicobacter pylori activity of Extractum liquiritiae, glycyrrhizin and its metabolites. J. Antimicrob. Chemother. 2004, 54, 243–246.
- Kolbe, L.; Immeyer, J.; Batzer, J.; Wensorra, U.; Dieck, K.T.; Mundt, C.; Wolber, R.; Stäb, F.; Schönrock, U.; Ceilley, R.I.; et al. Anti-inflammatory efficacy of Licochalcone A: Correlation of clinical potency and in vitro effects. Arch. Dermatol. Res. 2006, 298, 23–30.
- Kwon, H.-J.; Kim, H.-H.; Ryu, Y.B.; Kim, J.H.; Jeong, H.J.; Lee, S.-W.; Chang, J.S.; Cho, K.-O.; Rho, M.-C.; Park, S.-J.; et al. In vitro anti-rotavirus activity of polyphenol compounds isolated from the roots of Glycyrrhizauralensis. Bioorg. Med. Chem. 2010, 18, 7668–7674.
- Al-Turki, A.I.; El-Ziney, M.G.; Abdel-Salam, A.M. Chemical and antibacterial characterization of aqueous extracts of oregano, marjoram, sage and licorice and their application in milk and labneh. J. Food Agric. Environ. 2008, 6, 39–44.
- Park, I.-K.; Kim, J.; Lee, Y.-S.; Shin, S.-C. In vivofungicidal activity of medicinal plant extracts against six phytopathogenic fungi. Int. J. Pest Manag. 2008, 54, 63–68.
- Messier, C.; Grenier, D. Effect of licorice compounds licochalcone A, glabridin and glycyrrhizic acid on growth and virulence properties of Candida albicans. Mycoses 2011, 54, e801–e806.
- Maas, H.; Cock, I.E. The Interactive Antimicrobial Activity of Glycyrrhiza glabra L. Root Extracts and Conventional Antibiotics Against some Bacterial Triggers of Autoimmune Inflammatory Diseases. Pharmacogn. Commun. 2018, 8, 66–74.
- Wu, S.-C.; Yang, Z.-Q.; Liu, F.; Peng, W.-J.; Qu, S.-Q.; Li, Q.; Song, X.-B.; Zhu, K.; Shen, J.-Z. Antibacterial Effect and Mode of Action of Flavonoids from Licorice against Methicillin-Resistant Staphylococcus aureus. Front. Microbiol. 2019, 10, 2489.
- Chung, J.G. Inhibitory Actions of Glycyrrhizic Acid on Arylamine N-Acetyltransferase Activity in Strains of Helicobacter Pylori from Peptic Ulcer Patients. Drug Chem. Toxicol. 1998, 21, 355–370.
- Pastorino, G.; Cornara, L.; Soares, S.; Rodrigues, F.; Oliveira, M.B.P.P. Liquorice (Glycyrrhiza glabra): A phytochemical and pharmacological review. Phytother. Res. 2018, 32, 2323–2339.
- Fukai, T.; Marumo, A.; Kaitou, K.; Kanda, T.; Terada, S.; Nomura, T. Antimicrobial activity of licorice flavonoids against methicillin-resistant Staphylococcus aureus. Fitoter 2002, 73, 536–539.
- Demizu, S.; Kajiyama, K.; Takahashi, K.; Hiraga, Y.; Yamamoto, S.; Tamura, Y.; Okada, K.; Kinoshita, T. Antioxidant and antimicrobial constituents of licorice: Isolation and structure elucidation of a new benzofuran derivative. Chem. Pharm. Bull. 1988, 36, 3474–3479.
- Haraguchi, H.; Tanimoto, K.; Tamura, Y.; Mizutani, K.; Kinoshita, T. Mode of antibacterial action of retrochalcones from Glycyrrhiza inflata. Phytochemistry 1998, 48, 125–129.
- Zhou, T. Antimicrobial Activity of Licochalcone E against Staphylococcus aureus and Its Impact on the Production of Staphylococcal Alpha-Toxin. J. Microbiol. Biotechnol. 2012, 22, 800–805.
- Fukai, T.; Marumo, A.; Kaitou, K.; Kanda, T.; Terada, S.; Nomura, T. Anti-Helicobacter pylori flavonoids from licorice extract. Life Sci. 2002, 71, 1449–1463.
- Pompei, R.; Flore, O.; Marccialis, M.A.; Pani, A.; Loddo, B. Glycyrrhizic acid inhibits virus growth and inactivates virus particles. Nat. Cell Biol. 1979, 281, 689–690.
- Matsumoto, Y.; Matsuura, T.; Aoyagi, H.; Matsuda, M.; Hmwe, S.S.; Date, T.; Watanabe, N.; Watashi, K.; Suzuki, R.; Ichinose, S.; et al. Antiviral Activity of Glycyrrhizin against Hepatitis C Virus In Vitro. PLoS ONE 2013, 8, e68992.
- Ashfaq, U.A.; Masoud, M.S.; Nawaz, Z.; Riazuddin, S. Glycyrrhizin as antiviral agent against Hepatitis C Virus. J. Transl. Med. 2011, 9, 112.
- Huang, W.; Chen, X.; Li, Q.; Li, P.; Zhao, G.; Xu, M.; Xie, P. Inhibition of Intercellular Adhesion in Herpex Simplex Virus Infection by Glycyrrhizin. Cell Biophys. 2011, 62, 137–140.
- Michaelis, M.; Geiler, J.; Naczk, P.; Sithisarn, P.; Ogbomo, H.; Altenbrandt, B.; Leutz, A.; Doerr, H.W.; Cinatl, J., Jr. Glycyrrhizin inhibits highly pathogenic H5N1 influenza A virus-induced pro-inflammatory cytokine and chemokine expression in human macrophages. Med. Microbiol. Immunol. 2010, 199, 291–297.
- Moisy, D.; Avilov, S.V.; Jacob, Y.; Laoide, B.M.; Ge, X.; Baudin, F.; Naffakh, N.; Jestin, J.-L. HMGB1 Protein Binds to Influenza Virus Nucleoprotein and Promotes Viral Replication. J. Virol. 2012, 86, 9122–9133.
- Smirnov, V.S.; Zarubaev, V.V.; Anfimov, P.M.; Shtro, A.A. Effect of a combination of glutamyl-tryptophan and glycyrrhizic acid on the course of acute infection caused by influenza (H3H2) virus in mice. Vopr. Virusol. 2012, 57, 23–27.
- Laconi, S.; Madeddu, M.A.; Pompei, R. Autophagy Activation and Antiviral Activity by a Licorice Triterpene. Phytother. Res. 2014, 28, 1890–1892.
- Soufy, H.; Yassein, S.; Ahmed, A.R.; Khodier, M.H.; Kutkat, M.; Nasr, S.M.; Okda, F. Antiviral and immune stimulant activities of glycyrrhizin against duck hepatitis virus. Afr. J. Tradit. Complement. Altern. Med. 2012, 9, 389–395.
- Fukuchi, K.; Okudaira, N.; Adachi, K.; Odai-Ide, R.; Watanabe, S.; Ohno, H.; Yamamoto, M.; Kanamoto, T.; Terakubo, S.; Nakashima, H.; et al. Antiviral and Antitumor Activity of Licorice Root Extracts. In Vivo 2016, 30, 777–786.
- Hoever, G.; Baltina, L.; Michaelis, M.; Kondratenko, R.; Baltina, L.; Tolstikov, G.A.; Doerr, H.W.; Cinatl, J. Antiviral Activity of Glycyrrhizic Acid Derivatives against SARS−Coronavirus. J. Med. Chem. 2005, 48, 1256–1259.
- Cinatl, J.; Morgenstern, B.; Bauer, G.; Chandra, P.; Rabenau, H.; Doerr, H. Glycyrrhizin, an active component of liquorice roots, and replication of SARS-associated coronavirus. Lancet 2003, 361, 2045–2046.
- Murray, M.T. Glycyrrhiza glabra (Licorice). In Textbook of Natural Medicine; Elsevier: Amsterdam, The Netherlands, 2020; pp. 641–647.e3.
- Crance, J.M.; Biziagos, E.; Passagot, J.; van Cuyck-Gandré, H.; Deloince, R. Inhibition of hepatitis A virus replication in vitro by antiviral compounds. J. Med. Virol. 1990, 31, 155–160.
- Sato, H.; Goto, W.; Yamamura, J.-I.; Kurokawa, M.; Kageyama, S.; Takahara, T.; Watanabe, A.; Shiraki, K. Therapeutic basis of glycyrrhizin on chronic hepatitis B. Antivir. Res. 1996, 30, 171–177.
- Tandon, A. Treatment of subacute hepatitis with Lamivudine and intravenous Glycyrrhizin: A pilot study. Hepatol. Res. 2001, 20, 1–8.
- Orlent, H.; Hansen, B.; Willems, M.; Brouwer, J.T.; Huber, R.; Kullak-Ublick, G.A.; Gerken, G.; Zeuzem, S.; Nevens, F.; Tielemans, W.C.; et al. Biochemical and histological effects of 26 weeks of glycyrrhizin treatment in chronic hepatitis C: A randomized phase II trial. J. Hepatol. 2006, 45, 539–546.
- Ikeda, K. Glycyrrhizin injection therapy prevents hepatocellular carcinogenesis in patients with interferon-resistant active chronic hepatitis C. Hepatol. Res. 2007, 37, S287–S293.
- De Clercq, E. Current lead natural products for the chemotherapy of human immunodeficiency virus (HIV) infection. Med. Res. Rev. 2000, 20, 323–349.
- Sasaki, H.; Takei, M.; Kobayashi, M.; Pollard, R.B.; Suzuki, F. Effect of Glycyrrhizin, an Active Component of Licorice Roots, on HIV Replication in Cultures of Peripheral Blood Mononuclear Cells from HIV-Seropositive Patients. Pathobiology 2002, 70, 229–236.
- Harada, S. The broad anti-viral agent glycyrrhizin directly modulates the fluidity of plasma membrane and HIV-1 envelope. Biochem. J. 2005, 392, 191–199.
- Baba, M.; Shigeta, S. Antiviral activity of glycyrrhizin against varicella-zoster virus in vitro. Antivir. Res. 1987, 7, 99–107.
- Lin, J.-C. Mechanism of action of glycyrrhizic acid in inhibition of Epstein-Barr virus replication in vitro. Antivir. Res. 2003, 59, 41–47.
- Numazaki, K.; Nagata, N.; Sato, T.; Chiba, S. Effect of glycyrrhizin, cyclosporin A, and tumor necrosis factor α on infection of U-937 and MRC-5 cells by human cytomegalovirus. J. Leukoc. Biol. 1994, 55, 24–28.
- Zhang, H.; Song, Y.; Zhang, Z. Glycyrrhizin Administration Ameliorates Coxsackievirus B3-Induced Myocarditis in Mice. Am. J. Med. Sci. 2012, 344, 206–210.
- Lampis, G.; Deidda, D.; Pinza, M.; Pompei, R. Enhancement of Anti-Herpetic Activity of Glycyrrhizic Acid by Physiological Proteins. Antivir. Chem. Chemother. 2001, 12, 125–131.
- Hardy, R.S.; Raza, K.; Cooper, M.S. Endogenous glucocorticoids in inflammation: Contributions of systemic and local responses. Swiss Med. Wkl. 2012, 142, w13650.
- Utsunomiya, T.; Kobayashi, M.; Pollard, R.B.; Suzuki, F. Glycyrrhizin, an active component of licorice roots, reduces morbidity and mortality of mice infected with lethal doses of influenza virus. Antimicrob. Agents Chemother. 1997, 41, 551–556.
- Sekizawa, T.; Yanagi, K.; Itoyama, Y. Glycyrrhizin increases survival of mice with herpes simplex encephalitis. Acta Virol. 2001, 45, 51–54.
- Lu, H.; Huo, N.; Wang, G.; Li, H.; Nie, L.; Xu, X. Clinical observation of therapeutic effect of compound glycyrrhizin on SARS. China Pharm. 2003, 10, 34–36.
- Wu, H.B.; Li, H.M.; Lu, C.A.; Gao, Y.J.; Li, X.Q.; Zhou, A.X. Experimental study on Shuanghuanglian dispersible tablets against viruses. Chin. J. Exp. Tradit. Med. Formul. 2004, 10, 48–50.
- Yang, H.; Ko, H.-J.; Yang, J.-Y.; Kim, J.-J.; Seo, S.-U.; Park, S.G.; Choi, S.S.; Seong, J.K.; Kweon, M.-N. Interleukin-1 Promotes Coagulation, Which Is Necessary for Protective Immunity in the Lung against Streptococcus pneumoniae Infection. J. Infect. Dis. 2012, 207, 50–60.
- Krishnaswamy, K. Traditional Indian spices and their health significance. Asia Pac. J. Clin. Nutr. 2008, 17, 265–268.
- Tapsell, L.C.; Hemphill, I.; Cobiac, L.; Sullivan, D.R.; Fenech, M.; Patch, C.S.; Roodenrys, S.; Keogh, J.; Clifton, P.; Williams, P.; et al. Health benefits of herbs and spices: The past, the present, the future. Med. J. Aust. 2006, 185 (Suppl. 5), S1–S24.
- Mueller, M.; Hobiger, S.; Jungbauer, A. Anti-inflammatory activity of extracts from fruits, herbs and spices. Food Chem. 2010, 122, 987–996.
- Hanada, T.; Yoshimura, A. Regulation of cytokine signaling and inflammation. Cytokine Growth Factor Rev. 2002, 13, 413–421.
- Guo, J.; Shang, E.; Zhao, J.; Fan, X.; Duan, J.; Qian, D.; Tao, W.; Tang, Y. Data mining and frequency analysis for licorice as a “on Chinese Formulae Database” herb in Chinese Formulae based on Chinese Formulae. Phytomedicine 2014, 21, 1281–1286.
- Murray, M.T. The Healing Power of Herbs, 2nd ed.; Three Rivers Press: New York, NY, USA, 1995.
- Szapary, P.O. Tyler’s Herbs of Choice: The Therapeutic Use of Phytomedicinals; Robberts, J.E., Tyler, V.E., Eds.; Haworth Herbal: Binghamton, NY, USA, 1999; ISBN 0789001608.
- Wu, T.-Y.; Khor, T.O.; Saw, C.; Loh, S.C.; Chen, A.I.; Lim, S.S.; Park, J.H.Y.; Cai, L.; Kong, A.-N.T. Anti-inflammatory/Anti-oxidative Stress Activities and Differential Regulation of Nrf2-Mediated Genes by Non-Polar Fractions of Tea Chrysanthemum zawadskii and Licorice Glycyrrhiza uralensis. AAPS J. 2010, 13, 1–13.
- Chandrasekaran, C.V.; Deepak, H.B.; Thiyagarajan, P.; Kathiresan, S.; Sangli, G.K.; Deepak, M.; Agarwal, A. Dual inhibitory effect of Glycyrrhiza glabra (GutGardTM) on COX and LOX products. Phytomedicine 2011, 18, 278–284.
- Kao, T.-C.; Wu, C.-H.; Yen, G.-C. Bioactivity and Potential Health Benefits of Licorice. J. Agric. Food Chem. 2014, 62, 542–553.
- Yu, J.-Y.; Ha, J.Y.; Kim, K.-M.; Jung, Y.-S.; Jung, J.-C.; Oh, S. Anti-Inflammatory Activities of Licorice Extract and Its Active Compounds, Glycyrrhizic Acid, Liquiritin and Liquiritigenin, in BV2 Cells and Mice Liver. Molecules 2015, 20, 13041–13054.
- Xia, S.; Li, X.; Johnson, T.; Seidel, C.; Wallace, D.P.; Li, R. Polycystin-dependent fluid flow sensing targets histone deacetylase 5 to prevent the development of renal cysts. Development 2010, 137, 1075–1084.
- Wang, C.-Y.; Kao, T.-C.; Lo, W.-H.; Yen, G.-C. Glycyrrhizic Acid and 18β-Glycyrrhetinic Acid Modulate Lipopolysaccharide-Induced Inflammatory Response by Suppression of NF-κB through PI3K p110δ and p110γ Inhibitions. J. Agric. Food Chem. 2011, 59, 7726–7733.
- Bai, M.; Yao, G.-D.; Ren, Q.; Li, Q.; Liu, Q.-B.; Zhang, Y.; Wang, X.-B.; Huang, X.-X.; Song, S.-J. Triterpenoid saponins and flavonoids from licorice residues with anti-inflammatory activity. Ind. Crops Prod. 2018, 125, 50–58.
- Frattaruolo, L.; Carullo, G.; Brindisi, M.; Mazzotta, S.; Bellissimo, L.; Rago, V.; Curcio, R.; Dolce, V.; Aiello, F.; Cappello, A.R. Antioxidant and Anti-Inflammatory Activities of Flavanones from Glycyrrhiza glabra L. (licorice) Leaf Phytocomplexes: Identification of Licoflavanone as a Modulator of NF-kB/MAPK Pathway. Antioxidants 2019, 8, 186.
- Xiao, Y.; Xu, J.; Mao, C.; Jin, M.; Wu, Q.; Zou, J.; Gu, Q.; Zhang, Y.; Zhang, Y. 18β-Glycyrrhetinic Acid Ameliorates Acute Propionibacterium acnes-induced Liver Injury through Inhibition of Macrophage Inflammatory Protein-1α. J. Biol. Chem. 2010, 285, 1128–1137.
- Wang, X.-R.; Hao, H.-G.; Chu, L. Glycyrrhizin inhibits LPS-induced inflammatory mediator production in endometrial epithelial cells. Microb. Pathog. 2017, 109, 110–113.
- Ishida, T.; Miki, I.; Tanahashi, T.; Yagi, S.; Kondo, Y.; Inoue, J.; Kawauchi, S.; Nishiumi, S.; Yoshida, M.; Maeda, H.; et al. Effect of 18β-glycyrrhetinic acid and hydroxypropyl γcyclodextrin complex on indomethacin-induced small intestinal injury in mice. Eur. J. Pharmacol. 2013, 714, 125–131.
- Kim, Y.W.; Ki, S.H.; Lee, J.R.; Lee, S.J.; Kim, C.W.; Kim, S.C.; Kim, S.G. Liquiritigenin, an aglycone of liquiritin in Glycyrrhizae radix, prevents acute liver injuries in rats induced by acetaminophen with or without buthionine sulfoximine. Chem. Biol. Interact. 2006, 161, 125–138.
- Fu, Y.; Chen, J.; Li, Y.-J.; Zheng, Y.-F.; Li, P. Antioxidant and anti-inflammatory activities of six flavonoids separated from licorice. Food Chem. 2013, 141, 1063–1071.
- Yao, L.; Sun, T. Glycyrrhizin administration ameliorates Streptococcus aureus-induced acute lung injury. Int. Immunopharmacol. 2019, 70, 504–511.
- Yu, Z.; Ohtaki, Y.; Kai, K.; Sasano, T.; Shimauchi, H.; Yokochi, T.; Takada, H.; Sugawara, S.; Kumagai, K.; Endo, Y. Critical roles of platelets in lipopolysaccharide-induced lethality: Effects of glycyrrhizin and possible strategy for acute respiratory distress syndrome. Int. Immunopharmacol. 2005, 5, 571–580.
- Menegazzi, M.; di Paola, R.; Mazzon, E.; Genovese, T.; Crisafulli, C.; Dalbosco, M.; Zou, Z.; Suzuki, H.; Cuzzocrea, S. Glycyrrhizin attenuates the development of carrageenan-induced lung injury in mice. Pharmacol. Res. 2008, 58, 22–31.
- Xie, C.; Li, X.; Wu, J.; Liang, Z.; Deng, F.; Xie, W.; Zhu, M.; Zhu, J.; Zhu, W.; Geng, S.; et al. Anti-inflammatory activity of magnesium isoglycyrrhizinate through inhibition of phospholipase A2/Arachidonic acid pathway. Inflammation 2015, 38, 1639–1648.
- Bhattacharjee, S.; Bhattacharjee, A.; Majumder, S.; Majumdar, S.B. Glycyrrhizic acid suppresses Cox-2-mediated anti-inflammatory responses during Leishmania donovani infection. J. Antimicrob. Chemother. 2012, 67, 1905–1914.
- La, V.D.; Tanabe, S.-I.; Bergeron, C.; Gafner, S.; Grenier, D. Modulation of Matrix Metalloproteinase and Cytokine Production by Licorice Isolates Licoricidin and Licorisoflavan A: Potential Therapeutic Approach for Periodontitis. J. Periodontol. 2011, 82, 122–128.
- Kim, H.J.; Seo, J.-Y.; Suh, H.-J.; Lim, S.S.; Kim, J.-S. Antioxidant activities of licorice-derived prenylflavonoids. Nutr. Res. Pract. 2012, 6, 491–498.
- Thiyagarajan, P.; Chandrasekaran, C.V.; Deepak, H.B.; Agarwal, A. Modulation of lipopolysaccharide-induced pro-inflammatory mediators by an extract of Glycyrrhiza glabra and its phytoconstituents. Inflammopharmacology 2011, 19, 235–241.
- Ni, Y.-F.; Kuai, J.-K.; Lu, Z.-F.; Yang, G.-D.; Fu, H.-Y.; Wang, J.; Tian, F.; Yan, X.-L.; Zhao, Y.-C.; Wang, Y.-J.; et al. Glycyrrhizin Treatment Is Associated with Attenuation of Lipopolysaccharide-Induced Acute Lung Injury by Inhibiting Cyclooxygenase-2 and Inducible Nitric Oxide Synthase Expression. J. Surg. Res. 2011, 165, e29–e35.
- Cui, Y.; Ao, M.; Hu, J.; Yu, L. Anti-Inflammatory Activity of Licochalcone A Isolated from Glycyrrhiza inflata. Zeitschrift für Naturforschung C 2008, 63, 361–365.
- Acharya, S.K.; Dasarathy, S.; Tandon, A.; Joshi, Y.K.; Tandon, B.N. A preliminary open trial on interferon stimulator (SNMC) derived from Glycyrrhiza glabra in the treatment of subacute hepatic failure. Indian J. Med. Res. 1993, 98, 69–74.
- Seo, E.-H.; Song, G.-Y.; Kwak, B.O.; Oh, C.-S.; Lee, S.H.; Kim, S.-H. Effects of Glycyrrhizin on the Differentiation of Myeloid Cells of the Heart and Lungs in Lipopolysaccharide-Induced Septic Mice. Shock 2017, 48, 371–376.
- Levine, B.; Deretic, V. Unveiling the roles of autophagy in innate and adaptive immunity. Nat. Rev. Immunol. 2007, 7, 767–777.
- Leib, D.A.; Alexander, D.E.; Cox, D.; Yin, J.; Ferguson, T.A. Interaction of ICP34.5 with Beclin 1 Modulates Herpes Simplex Virus Type 1 Pathogenesis through Control of CD4 + T-Cell Responses. J. Virol. 2009, 83, 12164–12171.
- Gassen, N.C.; Niemeyer, D.; Muth, D.; Corman, V.M.; Martinelli, S.; Gassen, A.; Hafner, K.; Papies, J.; Mösbauer, K.; Zellner, A.; et al. SKP2 attenuates autophagy through Beclin1-ubiquitination and its inhibition reduces MERS-Coronavirus infection. Nat. Commun. 2019, 10, 5770.
- Shojaei, S.; Suresh, M.; Klionsky, D.J.; Labouta, H.I.; Ghavami, S. Autophagy and SARS-CoV-2 infection: A possible smart targeting of the autophagy pathway. Virulence 2020, 11, 805–810.
