Traditional diagnosis of HSV from lesions involves the direct detection of tissues or cells infected by the virus, viral proteins, whole virus, or genetic materials. The virus is collected from lesions on skin or genitals by swabbing or scraping with a scalpel. This is followed by detection using the various techniques discussed in the following sections.
2.1. Microscopy and Imaging
Brightfield Microscopy: Historically, the most widely used HSV diagnostic tests were based on Brightfield microscopy [
25,
26]. Brightfield microscopy involves imaging the transmitted light after passing through the specimen or the back-reflected light. The morphological information is obtained due to the attenuation of light because of absorption and/or scattering from the sample. The scattering and absorption from viral particles, which are <150 nm in size, are minuscule and, thus, individual viral particles cannot be directly observed using this modality [
42]. However, brightfield microscopy can be used to image cells and tissues infected with the virus. The specimen for this method is collected by scraping the lesion (Tzanck smears) using a scalpel blade and transferring the sample to a glass slide, followed by staining with Giemsa, methylene blue, or toluidine blue [
43,
44,
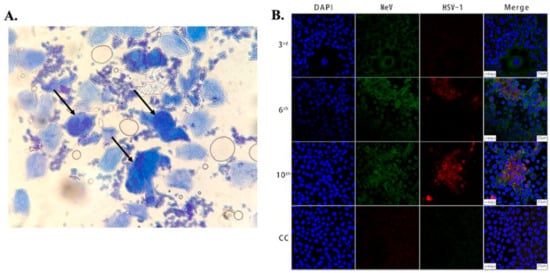
45]. These stained tissues are imaged in order to detect HSV cytopathic effects. A shows a Tzanck smear stained with methylene blue of a sample collected from the vesicles of an HSV-infected patient, showing multinucleated giant cells under brightfield microscopy. This method is simple, inexpensive, and can be used for a wide variety of clinical specimens. However, the major drawback of this method is its sensitivity (84%), which depends on proper sample preparation, which is complex. Additionally, a large amount of tissue is needed for accurate identification, and this can be painful for patients. Secondly, the accuracy of this method depends on the stage of lesions [
46,
47,
48]. Another drawback is its lack of specificity in differentiating HSV-1, HSV-2, and varicella-zoster virus (VZV).
Figure 1. (
A) Microscopic image showing large multinucleated giant cells (indicated by arrows) surrounded by multiple normal cells in an HSV-infected patient. The cells were stained with methylene blue, taken using an optical brightfield microscope [
45]. (
B) Images showing Vero/hSLAM cells coinfected by MeV and HSV-1 from different passages and a cell control (3rd, 6th, 10th, CC). As indicated in the 2nd and 3rd columns, the cells were subjected to immunostaining using antibodies against MeV M (green) and HSV-1 ICP0 (red) protein, and images were captured using laser scanning confocal microscopy at 40× magnification using a Leica TCS SP8 confocal microscope (Leica Microsystems; Wetzlar, Germany). The cell nuclei were stained with DAPI [
68].
In addition to tissues, the presence of the virus in swabs can be detected by culturing them in susceptible cell lines such as Hep-2, A549, MRC-5, WI38, Vero, rhabdomyosarcoma cells, rabbit kidney, and human diploid fibroblasts [
26]. The changes in cell morphology, such as cytoplasmic granulation, cell rounding, or lysis, indicate the presence of the virus. The process of specimen collection and transport is very sensitive as viral envelopes are extremely labile. Contamination of the samples with bacteria or fungus can be an issue and, thus, antibiotics are used in the transport media. The sensitivity of HSV detection depends on the cell line, e.g., rabbit kidney shows 100% sensitivity even at low viral inoculum [
49,
50,
51]. This process typically requires 5–14 days to generate the result and lacks specificity in differentiating HSV-1 and HSV-2; it also requires extreme care in collecting, handling, and transporting the specimen, which may have an effect on the test result.
Fluorescence Microscopy: In fluorescence microscopy, the fluorescently labeled specimen is illuminated with light of a specific wavelength, which is absorbed by the fluorophore, and results in the emission of another photon with lower energy (longer wavelength), which is captured by the photomultiplier tubes (PMT) or cameras in the microscope [
52]. In order to visualize the virus using fluorescence microscopy, it needs to be stained with fluorescent molecules [
53,
54,
55]. The most widely used method of visualizing the virus using fluorescence microscopy is direct immunofluorescence assay (DFA). DFA uses specific targeting moieties, such as antibodies, tagged with fluorophores to stain the virus [
52,
56,
57,
58,
59,
60,
61]. These antibodies typically target the glycoproteins present on the surface of the viral particles. A comparison between the efficiency of fluorescence microscopy and viral culture for detection of HSV was performed by Caviness et al. in pediatric patients [
62]. In this study, samples were collected by swabbing and scraping the base of a skin lesion of the infected patients. The sample obtained was then rubbed onto glass microscope slides, air-dried, fixed, and made to react with the commercially available monoclonal antibodies labeled with fluorescein isothiocyanate (a fluorescent probe specific to HSV type 1 and 2) to form an immunocomplex. The emission of green fluorescence from the cells indicated the presence of HSV infection, as observed under a fluorescence microscope. The turnaround time of this assay was about 60–90 min. The sensitivity of the DFA method in clinical samples was found to be 61% compared to viral culture, using HFF and A549 cell lines, and the specificity was greater than 90%. However, there can be an issue of cross-reactivity with the use of monoclonal antibodies, and this might give rise to false- negative or false-positive results. Another disadvantage is the requirement of clean microscopic glass slides with a controlled thickness that may not be available in resource-limited settings.
Confocal microscopy: Fluorescence confocal microscopy, which has a higher spatial resolution compared to conventional fluorescence microscopes, has been used to study viral cytopathology [
52,
63,
64,
65,
66,
67]. Confocal microscopes use a spatial slit/pinhole to eliminate the out-of-focus fluorescence photons during image formation, thereby increasing spatial resolution. Li et al. recently reported the detection and characterization of HSV-1 infection from throat swabs in measles patients [
68]. Serological assay (ELISA) and RT-PCR were performed to confirm and characterize the coinfection, evaluating the presence of IgG and IgM against HSV and measles virus and viral nucleic acid, respectively, in patient samples. Confocal laser scanning microscopy was used to demonstrate the dynamic of measles and HSV-1 coinfection in the Vero/hSLAM cell line using an indirect immunofluorescence assay (IFA) to stain the virus with fluorescent-labeled antibodies. The throat swab samples from confirmed measles patients were used to infect Vero/hSLAM cells for propagation. After a few days of incubation, the infected cells were extracted at different passage times, washed, and fixed on slides. After fixing, diluted antibodies specific to measles (rabbit Mev matrix protein) and HSV-1 (mouse anti-HSV-1 ICP0) were added, which formed the immunocomplex. A fluorescent-labeled secondary antibody (GFP against Mev matrix protein and RFP against HSV-1 ICP0 protein) was added to the sample to fluorescently stain the virus. The nucleus of the cells was stained with DAPI and imaged using LASER scanning confocal microscopy, as shown in B. Mev infection was detected using the antibody for the anti-Mev matrix protein, indicated by green fluorescence, whereas HSV-1 was detected using an anti-HSV ICP0 antibody, indicated by red fluorescence. It was observed that fluorescence (red) due to HSV-1 appears strong only after the 6th passage and gradually increases thereafter, whereas the green fluorescence (Mev) decreases. This study, conducted on 40 measles patients, suggests Mev as a primary infection, whereas HSV-1 infection was due to the reactivation of the latent virus in most cases. In another study, Cinotti et al. reported the identification of HSV infection by skin-dedicated ex-vivo fluorescence confocal microscopy using fluorescent antibodies [
66]. In this study, HSV samples were collected from skin lesions of infected patients and incubated with anti-HSV1 and anti-HSV2 antibodies tagged with fluorescein isothiocyanate for the identification of the virus.
Reflectance confocal microscopy (RCM) is another promising noninvasive skin imaging technique [
69,
70] used to study the histopathology of cells for diagnosing various skin diseases. It enables the imaging of the epidermis and papillary dermis directly, with high resolution at the cellular level without altering the skin surface. RCM imaging of a patient experiencing pustular eruptions showed the characteristics of large lobated multinucleated cells and acantholysis that are similar to the herpes-infected cytopathic effect on skin cells, and the findings were validated by the Tzanck cytodiagnosis method. These microscopic techniques are sensitive to light and motion and have a small field of view, which severely limits the throughput of the tests. A large number of images need to be acquired to obtain statistically relevant data so as to achieve results with a high degree of accuracy. In addition, these microscopes are expensive and involve complex instrumentations, making the instrument bulky and not readily available in resource-limited settings.
Transmission Electron Microscopy (TEM): The electron microscope (EM) uses a thin monochromatic beam of electrons that is focused on the sample using a magnetic lens operating at a high voltage of 200 kV. The transmitted electron beams are used to form an image and extract the structure and morphology of the samples. Unlike optical microscopy, electron microscopes can image the samples at extremely high magnifications of up to 1,000,000×, which enables high-resolution imaging of individual HSV viral particles [
34,
35,
71,
72,
73]. Folkers et al. demonstrated the use of electron microscopy to diagnose HSV infection and compared its efficiency with viral culture and the Tzanck smear method [
71]. For this study, the sample was collected from the base and edges of the lesion and adsorbed on a carbon-coated TEM grid. The sample was fixed with 1% glutaraldehyde, washed, and stained with 2% phosphotungstic acid (PTA) in order to observe the viruses at 10,000× magnification. Another technique is solid-phase immunoelectron microscopy, which involves viral capture using a bilayer of protein A and an antibody. The grid is first treated with protein A, followed by the immobilization of rabbit IgG anti-HSV. The grid is then washed and incubated with a drop of viral suspension, further washed with saline buffer, fixed with 1% glutaraldehyde, and stained with 2% PTA, which enables direct imaging of the virus.
Indirect labeling is another technique that involves capturing the virus using a monoclonal antibody specific to HSV-1 and HSV-2, followed by labeling with gold-tagged rabbit anti-mouse antibodies. The virus samples are prepared by collecting the lesions and homogenizing them with ultra-fine sterile quartz sand particles. This homogenized sample is centrifuged, and the virus particles present in the supernatant are used for testing [
71]. The sensitivity of the EM technique has been found to be 96% compared to viral culture and the Tzanck smear method. ImmunoEM has better specificity in differentiating HSV-1, HSV-2, and VZV from skin lesions. The requirement of bulky and expensive instruments and its low throughput, which are the major drawback of this technique, have limited its utilization. Nowadays, these techniques are largely replaced by immunofluorescence based assays that can provide more sensitive type-specific detection of HSV.
Digital Holographic Microscopy: Digital holographic microscopy (DHM) is an interferometric technique that has been extensively used for the detection and imaging of biological samples [
36,
74,
75,
76,
77,
78]. In this type of computational microscopy, the images are digitally reconstructed from holograms, which result from the interference between the scattered optical wave and the non-diffractive wave [
79]. Typically, a partially coherent light source is used to illuminate the sample, and the transmitted light (holograms) is recorded using a CMOS imaging chip placed close (<1 mm) to the sample. The holograms are then backpropagated to the object plane in order to reconstruct the images. The images contain both the phase and amplitude information. Several different algorithms can be used to reconstruct the images. For example, the widely used angular spectrum approach involves multiplying a transfer function with the Fourier transform of the captured hologram and then taking the inverse Fourier transform of the product to retrieve the image [
80]. The absence of lenses enables imaging over a wide field of view, giving this technique higher throughput compared to conventional lens based microscopy techniques. Additional advantages include low cost, portability, and ease of use, thereby making this technique a promising candidate for POC detection of HSV.
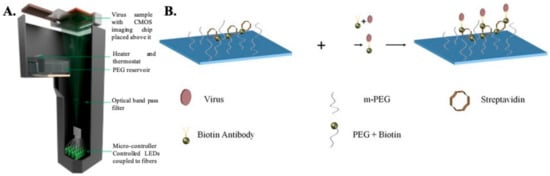
Detection of the whole virus using DHM is performed by first capturing the virus on a specially prepared substrate using monoclonal antibodies (as shown in ). The virus samples are first mixed with biotinylated antibodies to form an antibody–antigen complex and then incubated on a glass substrate coated with streptavidin. Once the virus is immobilized onto the glass surface due to the biotin–avidin bond, the samples are thoroughly washed and dried prior to imaging. Nonspecific binding is minimized by coating the bare glass surface with poly-ethylene glycol. The viruses are directly detected using DHM by creating localized liquid droplets, called nanolenses, specifically around the virus. These nanolenses help to amplify the signature of the virus, which would otherwise be too weak to detect. The nanolenses are created by depositing PEG vapor on the substrate containing the virus. The temporal evolution of the nanolenses is also used to estimate the size of the virus (~150 nm), which is then used to distinguish the viral particles from nonviral “junk” particles. The limit of detection (sensitivity) of this method has been calculated to be ~4 copies per mm
2 of the substrate imaged or ~160 copies/test [
36]. Another approach that utilizes a new method of creating nanolenses using acoustic actuation was used to detect the whole viral particles in solution, thereby expanding the capabilities of DHM for detecting HSV in both dry state and in solution [
81].
Figure 2. (
A) Schematic representation of lensless holographic microscope. (
B) Step-wise process showing attachment of the virus to the surface substrate. Firstly, the chip for specific capture of HSV-1 particles is prepared by coating a glass substrate with streptavidin and poly-ethylene-glycol. In the second step, HSV-1 particles in solution are conjugated with biotin-tagged antibodies and added onto the substrate; in the third step, HSV-1 particles captured on the substrate are then imaged by the computational holographic microscope for counting their density (counts/mm
2) [
36].
A separate microparticle aggregation assay was also used to detect HSV using DHM. In this approach, HSV-specific-antibody-coated polystyrene microparticles were added to the virus sample and imaged using DHM [
82,
83]. The presence of the virus and the viral antigen led to clustering of the microparticles, which were quantified using a deep-learning-based algorithm. The degree of clustering was used as a metric to detect the presence of the virus and its concentration. The sensitivity, i.e., the limit of detection for this approach, was ~5 viral copies/μL (i.e., ~25 copies/test). The specificity of these techniques depends on the type of antibodies used, their antigen-binding affinity, and their rates of association and dissociation.
2.3. Detecting Viral Genetic Material
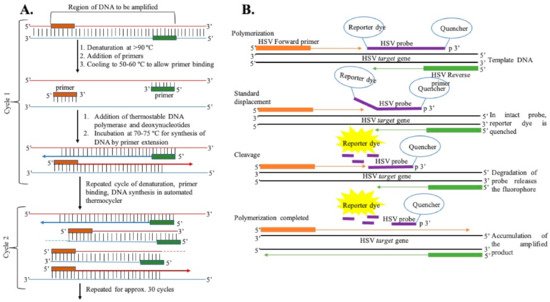
Polymerase Chain Reaction: The most common and standard molecular diagnosis technique is polymerase chain reaction (PCR), which allows the rapid amplification of viral genomes and can be used in clinical laboratories for the detection of HSV, as shown in [
27,
89,
90,
91,
92,
93,
94,
95,
96,
97]. The PCR method, involving the use of either a TaqMan probe or the HydProbe system that targets specific sequences of the genome, undergoes several thermal cycling processes of amplification and generates the result in the form of fluorescence signal readouts; gel electrophoresis can also be used. The advantages of the fluorescence-based real-time PCR technique have completely revolutionized the PCR-based system for the quantification of DNA [
98,
99]. This PCR technique is highly sensitive, has high precision, eliminates any post-amplification handling, and can be operated automatically. A fluorescence dye (SYBR green) or TaqMan probe is used in real-time PCR to monitor DNA amplification as the reaction progresses. Over the years, different PCR assays have been used for the detection of HSV [
97,
100,
101,
102,
103,
104,
105]. Marshall et al. have detected HSV from genital infections using a multiplex PCR assay [
106]. For this study, patient samples were collected, and DNA was extracted for the assay. Primers specific to the TK3 gene for HSV-1 and the POL gene for HSV-2 were chosen and incubated with the genomic DNA using the Taq polymerase method. After several thermal cycling steps, the amplified DNA was subjected to the gel-electrophoresis technique for HSV detection and typing. They were successful in detecting HSV infection in four suspected patients who were shown as negative with the viral culture method. This result indicates the sensitivity of PCR in HSV typing for diagnosing genital herpes.
Figure 3. (A) General representation of steps of DNA amplification using polymerase chain reaction. (B) DNA amplification using the TaqMan chemistry mechanism.
Recently, multiplexed quantitative PCR (qPCR) was used to detect HSV in intraoral commensal by Yap et al. [
107]. For this study, the DNA was extracted from samples collected from oral swabs and saliva samples and prepared using commercially available sample processing kits. This extracted fragment of DNA was amplified using qPCR with a fluorescent probe, which is useful for monitoring the real-time amplification of HSV-1 and HSV-2 DNAs. UL44 (HSV-1) and UL3 (HSV-2) target regions were chosen for the amplification. The limit of detection for each target was established using Vircell Quantified Amplirun DNA controls and was found to be 15 cp/PCR for HSV-1 and 8 cp/PCR for HSV-2. The viral load quantification was done with a standard curve. Among a pool of samples tested for the human herpes virus, 4.3% were reported to have HSV-1 with no trace of HSV-2 DNA.
A comparative study between PCR and viral culture methods showed 100% sensitivity and specificity for the PCR technique in detecting HSV-1 and -2 over the viral culture method, which has a sensitivity of 50% with 100% specificity [
108]. Another study compared the shell vial culture method and custom-designed FRET (fluorescence resonance energy transfer) based real-time- PCR, called LightCycler PCR, and found 100% specificity of LightCycler PCR, with increased sensitivity over shell vial techniques in detecting the virus [
109].
Loop-Mediated Isothermal Amplification Technique: DNA amplification, with high efficiency and specificity, can also be achieved using the loop-mediated isothermal amplification (LAMP) method [
28,
110,
111,
112,
113,
114,
115,
116,
117,
118]. It involves the use of
Bst DNA polymerase and a set of six primers that recognize specific sequences on the target DNA. An inner primer, along with a single strand displacing DNA polymerase, initiates DNA synthesis, which is primed by an outer primer releasing a single-stranded DNA that serves as the template for DNA synthesis. The single-stranded DNA is further primed by a second inner and outer primer hybridized to the other end of the target DNA, forming a loop DNA structure; it facilitates the amplification through the extension of the loop and the annealing of primers. The amplification cycling reaction continues, with the accumulation of 10
9 copies of the target in less than an hour. This method amplifies DNA at an optimum temperature (65 °C) without the need for several thermocycling steps; this speeds up the process, along with the use of six specific probes that increase efficiency and can be operated with cost-effective instruments in hospitals and clinics. A simple, sensitive LAMP assay was developed by Kaneko et al. for detecting HSV-1, HSV-2, and varicella-zoster virus (VZV) [
28]. These viral infections show similar symptoms but require different clinical prognoses, which makes it important to differentiate these viruses. Kaneko et al. used sets of clinically isolated strains of HSV-1, HSV-2, and VZV and used the viral DNA for their experiments. Six primers were used in the LAMP assay, including two outer primers (F3, B3), a forward inner primer (FIP), a backward inner primer (BIP), and two additional loop primers (LPF and LPB) for increased amplification efficiency. Virus-specific primers were designed to target specific gene origins, UL1 to UL2 for HSV-1, US4 for HSV-2, and ORF62 for VZV. The LAMP assay was performed using a LOOPamp DNA amplification kit. A reaction mixture containing each inner primer, outer primer, and additional loop primer,
Bst DNA polymerase, and DNA sample was incubated at 65 °C for 45 min and then above 80 °C to terminate the reaction. Each amplified product was further analyzed using the agarose gel electrophoresis technique. The specificity and sensitivity of the LAMP-amplified products were validated by digestion with a specific restriction enzyme, PstI for HSV-1 amplicons, HaeIII for HSV-2 amplicons, and AluI for VZV amplicons, and PCR using the primer sets. The limit of detection of HSV-1 and HSV-2 using the LAMP assay was as low as 10 copies/tube for all three different strains. Compared to PCR, this assay showed better specificity in differentiating HSV and VZV and, more importantly, between HSV-1 and HSV-2 with the specific primers used for the study. LAMP is more convenient due to its temperature-independent mechanism and less hardware requirement, which makes it suitable for point-of-care testing applications. However, optimization of the amplification of specific primer sets depends on the choice of polymer, design of primers, time, and ion concentrations, which makes the test labor-intensive and often leads to nonspecific amplification; this can compromise the assay’s specificity [
119].
Helicase-Dependent Amplification Technique: The helicase-dependent amplification technology is similar to PCR, but in this technique, a thermostable helicase enzyme is used to separate the DNA strands instead of thermal denaturation. This enables labeled primers hybridized to DNA templates and initiates the elongation process in the presence of DNA polymerase [
40,
120,
121]. The amplification can be operated at a single temperature of 64 °C, unlike the series of different temperatures in the case of PCR, which makes this technique suitable for point-of-care applications. Recently, the US food and drug administration (FDA) approved a test for HSV detection, called IsoAMP
® HSV (Biohelix Corp., Beverly, MA, USA), based on nucleic acid amplification technique for the detection of the HSV gB gene from oral and genital lesions of symptomatic patients [
40,
121,
122,
123]. The assay consists of helicase-dependent amplification (HDA) technology and a single-use detection device (Type II BESt
TM cassette) with a target-specific colorimetric probe. The sample specimen from the viral transport media is diluted and transferred to an amplification tube to which a master mix is added. The tube is then heated at 64 °C for 1 h to amplify the DNA and placed in the detection device to detect the amplicon. The target amplicon is fluorescein- and digoxigenin-labeled, which are captured and visualized as colored lines in the case of positive samples on a vertical flow strip within the disposable cassette. The turnaround time of the assay is less than 1.5 h. The sensitivity of this assay has been shown to be 97.1%, with a limit of detection of 5.5 and 34.1 copies/reaction for HSV-1 and HSV-2, respectively, and specificity of 93.4%; however, the major drawback of this assay is its inability to distinguish between HSV-1 and HSV-2. This assay has been replaced by a similar HDA assay, AmpliVue HSV 1 + 2 (Quidel, San Diego, CA, USA), which has 99.2% sensitivity and 99.7% specificity for HSV-1 and HSV-2, respectively [
121,
124,
125].
A modified version of the IsoAmp assay was employed by Tong et al. to develop a rapid, portable molecular test IsoGlow HSV typing assay for effective detection of HSV-1 and HSV-2 from genital and oral lesions [
126]. They used a portable fluorescence detection device, FireFly (BioHelix, Beverly, MA, USA), and cyclic probe technology for end-point detection of HSV products amplified by HDA. The FireFly instrument has onboard computer software for real-time and end-point data acquisition. The limit of detection for this assay was 10 copies/assay for both HSV-1 and HSV-2, and the sensitivity and specificity of the assay were found to be 100% and 98–100%, comparable to the ELVIS Shell vial assay (Diagnostic Hybrids, Athens, OH, USA) for HSV typing, with a turnaround time of 1 h. This technology has a great potential for type-specific detection of HSV in resource-limited setups, without the need for any expensive instrument, and can be easily formatted with other miniaturized detectors.
Recent studies by Jevšnik et al. have compared the effective detection of herpes simplex and varicella-zoster virus from skin lesions using a commercially available test, the RT-PCR (Argene, BioMerieux, Verniolle, France) test, performed on LC480 platform (Roche Applied Science, Mannheim, Germany) and the HDA assay (Solana HSV1 + 2/VZV assay, Quidel Corporation, San Diego, CA, USA). Both tests showed good agreement of 98.3% for HSV-1 and 99.3% for VZV [
127]. The limit of detection of RT-PCR reagents was about 107 copies/mL. The sensitivity of Solana’s assays was 97.7–100% for HSV-1, 92.7–99.1% for HSV-2, and 91.8–100% for VZV. The specificity recorded was 96.3–98.4% for HSV-1, 94.5–97.3% for HSV2, and 95.8–98.3% for VZV. This study indicates the significance of isothermal amplification assays in the type-specific sensitive detection of HSV, which can be easily translated for POC applications.