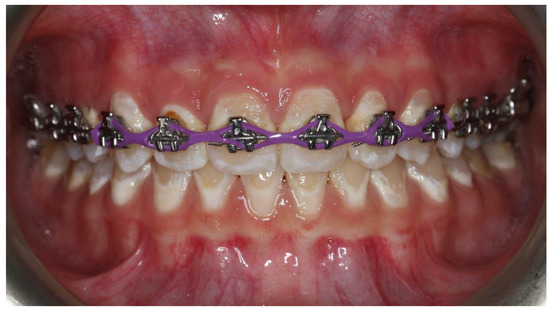
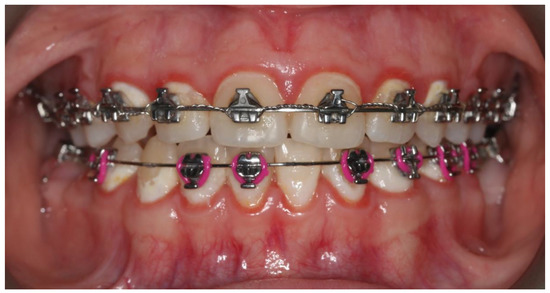
2.1. Comparison of Ultrasonic Scaling and Antimicrobial Photodynamic Therapy
Abellan et al. (2019) conducted studies about the effectiveness of PDT and US on periodontal health in patients treated with fixed braces. They divided 20 people aged 12 to 18 into two groups who underwent seven sessions (days 0, 15, 30, 45, 90, 180, 270) of PDT or US. The researchers showed a statistically significant decrease in the plaque index (PI), gingival index (GI), and probing depth (PD) in both groups compared to the starting point, but no differences between PDT and US. The multiplex map of human high sensitivity immunoassays showed a decrease in IL-1b, IL-10, TNF-a levels, persistent levels of IL-6, IL-1ra, and an increase in FGF-2, but no differences for both groups. In both groups, there was a similar decrease in colony-forming units (CFU) for
P. gingivalis,
P. intermedia, and
F. nucleatum. The researchers emphasize that PDT can be considered a safe alternative to gingivitis therapy with a slightly longer-lasting effect
[24].
Gomez et al. (2018) assessed the effectiveness of US and PDT in preventing gingivitis and white spot lesions during orthodontic treatment. Patients received seven PDT and US sessions, four sessions at two-week intervals at baseline (T0), followed by three boosters every three months (T1, T2, T3). In the international caries detection and assessment system (ICDAS), starting from T1, a slight increase was observed. However, these differences were not statistically significant. Periodontal indicators reduced their levels. full-mouth bleeding score (FMBS) and PD recorded the most significant decrease in T1 and full-mouth plaque score (FMPS) in T2, with no differences between the PDT and the US group. In the studies on a microbiome, the number of periopathogens and cariogenic bacteria decreased, without statistically significant variations between the two groups
[25].
2.2. Comparison of Ultrasonic Scaling and Ultrasonic Scaling with Adjunct Antimicrobial Photodynamic Therapy
Al Nazeh et al. (2020) divided the 22 subjects into two groups. The first group was subject to US only and the second group to both US and PDT. Methylene blue at a concentration of 0.0005% was used as a photosensitizer and then irradiated with light at a wavelength of 670 nm, fluence 22 J/cm
2, and fluence rate 150 mW. Before the intervention, one week after, and four weeks after, the following clinical parameters were assessed: dichotomous recording for plaque scores (PS) and bleeding on probing (BOP). The researchers collected plaque samples for bacterial analysis. There was a statistically significant decrease in PS and BoP for both groups, compared to the baseline values, but no difference between them. In the US group, there was a decrease in CFU for
T. forsythia after one week. In turn, for the US-and-PDT group, there was a statistically significant decrease in CFU for
T. forsythia and
P. gingivalis both after one week and four weeks
[26].
Alqerban (2020) compared the effectiveness of US with adjunct aPDT and US with adjunct photobiomodulation (PBM) to US alone in anti-gingivitis therapy in patients treated with fixed appliances. The researcher divided 45 patients into three equal groups. Alqerban measured PD, BoP, and PS in each group and collected plaque samples and gingival crevicular fluid (GCF) at baseline and on days 30 and 60 of the study. In the group with aPDT, methylene blue with a concentration of 0.0005% was used as a photosensitizer and then irradiated with light with the following parameters: 670 nm, 22 J/cm
2, 150 mW. There was a statistically significant decrease in PS and BoP in all groups compared to the baseline, with no variation between each group. In the aPDT group, there was a progressive decrease in PD, yet the variations between the groups were not statistically significant. The level of Human β-defensins in GCF assessed through the ELISA test showed a statistically significant decrease after 30 days for all groups. In the aPDT group, there was a further decrease observed after 60 days and a decrease in
T. denticola after 30 and 60 days
[27].
Alshahrani et al. (2020) compared the use of full- mouth periodontal debridement (FMPD) and FMPD with adjunct PDT. Yet another PS was MB in a concentration of 0.0005%, which they photoactivated with light with the following properties: 670 nm, 22 J/cm
2, 150 mW. A total of 26 people diagnosed with an orthodontic treatment-induced gingival enlargement (OTGE) were qualified for the study and divided into two research groups. In the clinical examination, the researchers assessed the values of PS, BOP, PD, and hyperplastic index (HI) at baseline, two and four weeks after the applied therapy. There was a statistically significant decrease in value for all items in both groups after two and four weeks. It is worth noting that there was a statistically significant decrease in HI for the FMPD-PDT group compared to the FMPD group in both time intervals. There was a significant reduction in
P. gingivalis,
T. forsythia, and
T. denticola from baseline. A statistically significantly higher reduction in mean log CFU/mL for the FMPD-PDT group after two and four weeks was observed for
P. gingivalis,
T. forsythia, while for
T. denticola, a significant difference occurred only after a two-week follow-up. In ELISA, IL-1β showed a significant reduction after four weeks of observation for both groups. There were significant differences in the reduced levels of IL-6 between the groups, to the FMPD-PDT group’s benefit, after a four-week follow up
[28].
Baeshen et al. (2020) assessed the effect of PDT on clinical parameters, pain levels, cytokine secretion, and bacterial microflora in adolescent orthodontic patients with gingivitis. Group 1 underwent US and PDT treatment using MB as a PS, while Group 2 underwent US only. However, when comparing the groups with each other, there were no differences in PS and BoP. There was a statistically significant decrease in the value in favor of the group with adjunct PDT. The use of the therapies did not change the level of perceived pain and PD values. There was a significant decrease in
T. forsythia for Group 1 compared to Group 2, but only after a one-week follow up. After four weeks, there was a re-increase in microbial counts. The researchers demonstrated a significant decrease in TNF-α and IL-6 for both groups compared to baseline. For TNF-α, a significant difference between the groups was present at week four and for the second cytokine at week one
[29].
Kamran (2020) also compared US alone with US with adjunct PDT. The latter used MB as a PS. The studies showed a reduction in PS and BoP compared to baseline for both groups after three weeks and further after six weeks. In both groups, the PS and BoP’s value reduced significantly after six and three and six weeks, respectively, always to the US-PDT group’s benefit. Both protocols lowered the levels of IL-6 and TNF-a. The US-PDT group showed a significant decrease in IL-6 in week three and for TNF-a in week six. The amount of
P. intermedia and
P. gingivalis in the plaque samples was much lower in both follow-up periods in the case of the adjunct PDT group
[30].
Malik et al. (2020) also compared the efficacy of aPDT in combination with US to US alone, but against oral yeast. At the beginning of the study and 6 months after the intervention, the gingival index was tested and unstimulated whole saliva (UWS) samples were collected. In the case of the GI, the results were comparable between the two groups. On the other hand, in the case of the yeast, there was a significant decrease in the amount of CFU/mL for the combined therapy, while the decrease for the US alone with respect to the baseline value was not statistically significant
[31].
2.3. Comparison of Antimicrobial Photodynamic Therapy and Chlorhexidine Products
Panhoca et al. (2016) evaluated the efficacy of aPDT using curcumin, which was modified by adding sodium dodecyl sulfate (SDS) surfactant to improve activity against bacterial biofilm. The 24 patients treated with fixed orthodontic appliances were divided into four groups. The first group was exposed to light only, the second group underwent PDT with curcumin, the third group underwent PDT with modified PS containing SDS, and the last group of patients used a mouth rinse with chlorhexidine gluconate solution (CHX). The study used light sources with a wavelength of 450 nm ±+/− 10 nm. A statistically significant decrease in the number of bacteria was found in UWS samples for groups 2, 3, and 4. However, researchers found no significant differences between the PDT + SDS group and the CHX group
[32].
Paschoal et al. (2015) compared the effects of aPDT with curcumin as PS with CHX varnish applied to teeth in the prophylaxis of white spot lesions and gingivitis. The mentioned therapies were applied four times at weekly intervals. Researchers compared PI and GBI at baseline one month after the intervention and three months after. In the case of the aPDT group, a light source with a wavelength of 450 nm, fluence of 96 J/cm
2, and a fluence rate of 165 mW/cm
2 was used. After a one-month follow-up period, no significant changes in PI values were observed for all groups, but, at the 3-month follow-up period in the aPDT group, an increase in the aforementioned index was observed. The GBI reduction was present at the first follow-up visit and then returned to the baseline values
[33].