The most frequent intracranial neoplasm is meningioma. About 30% of these are represented by skull base meningiomas (SBMs). Patients with SBMs can be treated with a multimodal approach based on surgery, medical treatment and radiation-based therapy; however, the gold standard treatment for the majority of symptomatic meningiomas is still surgery. Surgical intervention is performed with the goal of maximum safe resection. This, however, poses technical challenges because of the proximity of these tumors with deep critical neurovascular structures, tumoral texture and consistency. A multimodal treatment, in combination with stereotactic radiosurgery and radiation therapy, is thus of utmost importance to achieve a satisfactory functional outcome and tumor control.
- skull base meningioma
- surgery
- radiotherapy
- radiosurgery
1. Background
2. Modern Surgical Planning
2.1. The Role of Computer-Aided Approaches
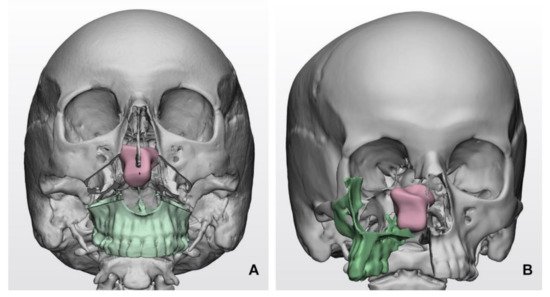
2.2. The Role of Tractography
3. The Role of Surgery
| Skull Base Region | Location | Incidence | Surgical Approaches | IONM | Surgical Pitfalls | Complications | ||
|---|---|---|---|---|---|---|---|---|
| Vascular | Nerves | Others | Clinical Manifestations | |||||
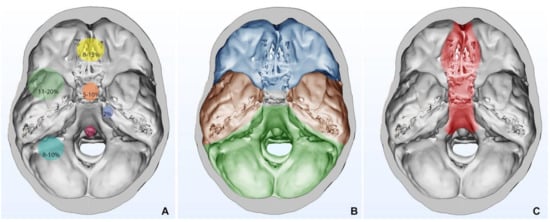
| Anterior Fossa 4, 27–36,49,51 |
Olfactory Groove Meningiomas | 8–13% | Subfrontal approach Transbasal Approach Pterional approach Fronto-lateral approach Supraorbital keyhole Endoscopic endonasal approach *Transfacial reconstitutive approach also known as facial translocation, further subdivided into:
|
EEG, MEPs, SSEPs, VEPs (in selected cases) | branches of the OA, ICA, ACoA, A2 Ethmoidal arteries |
CN I, II, III, IV | EOM | Anosmia, CSF leak Visual disturbances (diplopia, anopsia, eye globe injury) Hemorrhage Hemorrhage, epiphora, diplopia and dystopia, soft tissue swelling, ectropion (associated with Weber–Ferguson incision). Poor bone consolidation, misalignment (related to bad osteosynthesis), wound dehiscence (cutaneous and intraoral) |
| Sphenoid wing Meningiomas | 11–20% | Pterional approach Fronto-temporal-orbito-zygomatic approach Lateral, superior, medial orbitotomy |
anterior circulation arteries Ethmoidal artery in medial accesses |
CN II, III, VI supraorbital nerve, facial nerve |
EOM, medial and lateral canthal tendons | |||
| Tuberculum Sellae/Planum Meningiomas | 5–10% | Pterional approach Endoscopic endonasal approach Supraorbital key-hole |
Anterior circulation arteries | CN II, III, IV, V, VI | aesthetic orbital reconstruction | |||
| Cavernous Sinus Meningiomas | 1% | Pterional approach Fronto-temporo-orbito- Zygomatic approach |
Anterior circulation arteries | CN II, III, IV, V, VI | ||||
| Middle Fossa 4,35,44 |
Middle fossa and Sphenoid wing | 1.1–1.4% | Pterional approach (anterolateral approach) Fronto-temporo-orbito- zygomatic |
EEG, MEPs, SSEPs EMG CNs III, IV, VI can be considered |
ICA Vein of Labbè |
CN II, III, IV, V, VI | Temporal lobe | Language deficit, hemiparesis, hemianopsia, hemorrhages, temporal lobe edema, trigeminal anesthesia, |
| Middle fossa and cavernous sinus | ||||||||
| Middle fossa with infratemporal extension | Subtemporal approach (lateral approach) |
|||||||
| Middle fossa and petrous ridge | ||||||||
| Posterior Fossa 4,35,38–43,45,46,51 |
Cerebellopontine Angle | 10% | Anterior Petrosectomy Approach Posterior and Combined Petrosal Approaches Retrolabyrinthine Approach Translabyrinthine Approach Combined Petrosal Approach Retrosigmoid approach |
EEG, MEPs, SSEPs, CB-MEP (CN VII) EMG (CNs VI, VII) BAERs |
Intrapetrous ICA, SCA and AICA encasement | CN V, VI, VII, VIII | Brainstem adhesion | Brain steam and cerebellum edema, CSF leak Venous infarction Cranial nerve injury Vertebral artery injury, Hydrocephalus, CSF leak Infection Hemorrhage, cerebrospinal fluid leakage, soft tissue edema of the oral cavity, infection, wound dehiscence, velopalatine dysfunction, malocclusion, dysphagia, malocclusion when osteotomies are required, oro-nasal fistula, laceration of nasal mucosa, lesion of teeth apices |
| Foramen Magnum | 2.5% | Posterior Suboccipital Approach with C1 laminectomy; Far Lateral Approach Extreme Lateral Approach |
EEG, MEPs, SSEPs, CB-MEP (CN VII, IX, X, XI, XII) EMG (CNs VI, VII, IX, X, XI, XII) BAERs |
VA encasement JV encasement |
CN IX, X, XI, XII | Brainstem adhesion Extradural extension |
||
| Clival Meningiomas | <1% | Retrosigmoid approach Petrosal approach Transoral:
far-lateral approach Endoscopic approach |
Internal maxillary artery Palatine artery |
CN VI, VII, VIII, XI, X, XI, XII | Brainstem adhesion | |||
| Petroclival Meningiomas | 2% of posterior fossa meningiomas | Retrosigmoid approach Combined transpetrosal Retrolabyrinthine Approach Translabyrinthine Approach |
BA BA perforating arteries |
CN V, VI, VII, VIII | Brainstem adhesion | |||
3.1. Intraoperative Neurophysiological Monitoring in Skull Base Meningiomas
3.2. Preoperative Embolization
3.3. Reconstruction of the Surgical Route
4. Histopathological Features
| Altered Gene | Preferential Tumor Localization | Main Histotype |
|---|---|---|
| NF2 | Posterior and lateral skull base | Fibrous, Transitional, Atypical |
| AKT1, PI3K | Anterior and middle skull base | Meningothelial |
| SMO | Olfactory groove | Meningothelial * |
| TRAF7/KLF4 | Middle skull base | Meningothelial, Secretory for co-occurring TRAF7/KLF4 |
| POL2RA | Tuberculum sellae | Meningothelial |
5. Radiation Therapy
5.1. Fractionated Radiotherapy
| Authors | Patients (N) | Radiation Modality | Median Dose/ Dose per Fraction (Gy) | Median Volume (mL) | Median Follow-Up (Months) | Local Control | Late Toxicity (%) |
|---|---|---|---|---|---|---|---|
| Goldsmith et al., 1994 [79] | 117 | CRT | 54 | NA | 40 | 89 at 5 and 77 at 10 years | 3.6 |
| Maire et al., 1995 [80] | 91 | CRT | 52 | NA | 40 | 94 | 6.5 |
| Nutting et al., 1999 [81] | 82 | CRT | 55–60 | NA | 41 | 92 at 5 and 83 at 10 years | 14 |
| Vendrely et al., 1999 [82] | 156 | 3D-RT | 50 | NA | 40 | 79 at 5 years | 11.5 |
| Mendenhall et al., 2003 [83] | 101 | 3D-RT | 54 | NA | 64 | 95 at 5, 92 at 10 and 15 years | 8 |
| Henzel et al., 2006 [93] | 84 | fSRT | 56 | 11,1 | 30 | 100 | NA |
| Tanzler et al., 2010 [94] | 144 | fSRT | 52.7 | NA | 87 | 97 at 5 and 95 at 10 years | 7 |
| Minniti et al., 2011 [95] | 52 | fSRT | 50 | 35.4 | 42 | 93 at 5 years | 5.5 |
| Slater et al., 2012 [101] | 68 | Protons | 56 | 27.6 | 74 | 99 at 5 years | 9 |
| Weber et al., 2012 [102] | 24 | Protons | 56/1.8–2.0 | 21.5 | 62 | 100 at 5 years | 15.5 |
| Solda et al., 2013 [96] | 222 | fSRT | 50/55 | 12 | 43 | 100 at 5 and 10 years | 4.5 |
| Combs et al., 2013 [97] | 507 | fSRT/IMRT | 57.6/1.8–2.0 | 53.4 | 107 | 95.5 at 5 and 88 at 10 years | 1.8 |
| Fokas et al., 2014 [98] | 253 * | fSRT | 55.8/1.8–2.0 | 16 | 50 | 92.9 at 5 and 87.5 at 10 years | 12 (G2) |
| Han et al., 2014 [100] | 143 | fSRT | 50.4/1.8 | 11.1 | 32 | 95% | 0.7 |
| Kaul et al., 2014 [104] | 136 | fSRT | 57/1.8–2.0 | 24 | 44.9 | 93.8 at 5 and 91.5 at 10 years | G1 only |
| Sanford et al., 2017 [103] | 44 | Protons | 55.8–63 | 39.7/13.2 | 195 | 98 at 10 and 90 at 15 years | 59% (≥G2) |
| Lillie O’steen et al., 2019 [84] | 149 | 3D-RT | 50–52/1.7–1.8 | NA | 144 | 95 at 10 and 92 at 20 years | NA |
| Authors | Patients (N) | Technique | Median Dose (Gy)/Fractions | Median Volume (mL) | Median Follow-Up (Months) | Local Control | Late Toxicity |
|---|---|---|---|---|---|---|---|
| Colombo et al., 2009 [108] | 150 * | CK | 16–25/2–5 | 7.5 (0.1–64) | 30 | 96 | 3.5 |
| Fokas et al., 2014 [98] | 49 * | LINAC | 25–35/5 | 6.11 (1.9–35.7) | 50 | 92.9 at 5 and 87.5 at 10 years | 12 (G2) |
| Han et al., 2014 [100] | 22 * | LINAC | 25/5 | 4.8 (0.88–20.38) | 32 | 95 | 0.7 |
| Navarria et al., 2015 [109] | 26 | LINAC | 25/5 | 13° | 24.5 | 93% at 2 years | G3, none |
| Marchetti et al., 2016 [110] | 143 | CK | 21–25/2–5 | 8 (0.1–126.3) | 44 | 93 at 5 years | 5.1 |
| Marchetti et al., 2019 [111] | 168 | CK | 25/5 | 7.3 (0.1–76.8) | 51 | 94% at 5 years | 3.7 |
5.2. Radiosurgery
5.2.1. Overview
5.2.2. Posterior Fossa
5.2.3. WHO Grade II and III
5.2.4. Combined MS–SRS Approach
5.2.5. Long-Term Follow-Up
This entry is adapted from the peer-reviewed paper 10.3390/cancers13112664
