Essential oils (EOs) are extracted from plants and contain active components with therapeutic effects.
- inhalation therapy
- essential oil
- anti-depression
- anxiolytic
1. Introduction
Essential oil (EO), as the main component used in inhalation therapy, has been widely investigated for its therapeutic effects. Evidence indicates that EOs can successfully reduce anxiety and relieve pain when combined with conventional treatment [1,2]. EOs can be administered through oral consumption, direct skin contact, or inhalation [3]. Among all different administration routes, inhalation is the most commonly adopted method. In fact, EOs from different plant extracts have been studied to demonstrate different effects, with lavender and bergamot EOs being the most widely used ones for relaxation in either single use or mixed use with reported pharmacodynamic interactions [4]. It has been shown that the different positive effects were linked to specific constituents in EOs [5,6]. Therefore, the combined use of EOs consisting of different molecular compounds, is able to maximise the therapeutic effect [7,8].
2. Therapeutic Effects of EOs
Table 1 summarises the effect of EOs in human studies. For instance, the inhalation of lavender and chamomile EOs was found to decrease levels of depression, anxiety, and stress in older adults. It was suggested that the anxiolytic and antidepressant effects could be associated with the suppression of the activity of the sympathetic nervous system [11].
| EO(s) Scientific Name (Common Name) |
Author (Year) | Results | |
|---|---|---|---|
| Lavandula | |||
| Lavandula angustifolia (Lavender) | Burnett et al. (2004) | Anxiolytic effect | [8] |
| Lehrner et al. (2005) | Reduced anxiety; positive effect on mood; higher level of calmness | [18] | |
| Fayazi et al. (2011) | Anxiolytic effect | [17] | |
| Senturk et al. (2018) | Anxiolytic effect | [19] | |
| Karan et al. (2019) | Blood pressure control; anxiolytic effect; respiratory relaxation | [12] | |
| Ebrahimi et al. (2021) | Antidepressant effect; anxiolytic effect; reduced stress | [20] | |
| Citrus | |||
| Citrus sinensis (Sweet orange) | Lehrner et al. (2005) | Anxiolytic effect; positive effect on mood | [18] |
| Goes et al. (2012) | Anxiolytic effect | [21] | |
| Citrus junos (Yuzu) | Matsumoto et al. (2014) | Anxiolytic effect; antidepressant effect | [22] |
| Citrus bergamia (Bergamot) | Watanabe et al. (2015) | Reduced salivary cortisol level | [23] |
| Matricaria | |||
| Matricaria chamomilla (Chamomile) | McKay et al. (2006) | Antidepressant effect; anxiolytic effect | [24] |
| Ebrahimi et al. (2021) | Antidepressant effect; anxiolytic effect; reduced stress | [20] | |
| Salvia | |||
| Salvia rosmarinus (Rosemary) | Burnett et al. (2004) | Anxiolytic effect | [8] |
| Salvia officinalis (Sage) | Muss et al. (2010 | Positive effect on mood | [25] |
| Salvia lavandulaefolia (Spanish sage) | Muss et al. (2010) | Positive effect on mood | [25] |
| Mixture | |||
| Lavandula angustifolia (Lavender) + Rosa damascena (Damascus Rose) | Conrad et al. (2012) | Anxiolytic effect; antidepressant effect | [26] |
| Lavandula angustifolia (Lavender) Cananga odorata (Ylang-ylang) + Citrus aurantium (Neroli) | Song et al. (2017) | Anxiolytic effect | [27] |
Moreover, EOs have the potential to relieve depression and secondary depressive symptoms arising from different types of chronic conditions, like anxiety disorders and dementia [13,14,15,16]. Fayazi and co-workers have shown that patients inhaling lavender EO before undergoing heart and abdominal surgeries reported less anxiety, suggesting the potential anxiolytic effect of the EO [17]. The therapeutic effects of EOs have also been proven in animal studies (Table 2).
| EO(s) Scientific Name (Common Name) | Author (Year) | Animal | Behaviour Outcome (a) | Secondary Outcome (b) | Results | |
|---|---|---|---|---|---|---|
| Lavandula | ||||||
| Lavandula angustifolia (Lavender) | Chioca et al. (2013) | Mice | MBT, OFT | (a) Increase in locomotor activity (b) - |
[30] | |
| Chioca et al. (2013) | Mice | EPM | 5-HT | (a) Increase in open arm timing (b) Increase of 5-HT level |
[31] | |
| Coelho et al. (2014) | Rats | CFT | c-Fos | (a) Decrease in freezing response (b) Increase in c-Fos expression |
[41] | |
| Sanchez-Vidana et al. (2019) | Rats | OFT, FST | DCX, BDNF | (a) Increase in locomotor activity; decrease in immobility timing (b) Increase in DCX expression and BDNF level |
[35] | |
| Citrus | ||||||
| Citrus limon (Lemon) | Komiya et al. (2006) | Mice | EPM, OFT FST | DA, 5-HT | (a) Increase in open arm timing and locomotor activity; decrease in immobility timing (b) Increase of 5-HT and DA levels |
[32] |
| Citrus sinensis (Sweet orange) | Hocayen et al. (2019) | Mice | MBT, OFT, Light/dark test | NADPH-d | (a) Increase in locomotor activity and spending time in bright area (b) Decrease of NADPH cells |
[42] |
| Other | ||||||
| Acorus gramineus (Japanese sweet flag) | Koo et al. (2003) | Mice | NADPH-d | (a) - (b) Decrease of NADPH cells |
[43] | |
| Perilla frutescens (Perilla) | Ji et al. (2014) | Mice | OFT, FST, TST | 5-HT, 5-HIAA | (a) Decrease in immobility timing (b) Increase of 5-HT and 5-HIAA levels |
[34] |
| Coriandrum sativum (Coriander) | Cioanca et al. (2014) | Rats | EPM, FST | GSH | (a) Increase in open arm timing; decrease in immobility timing (b) Increase of GSH |
[44] |
| Asarum caudatum (Asarum) | Park et al. (2015) | Mice | FST, TST | CRF, 5-HT | (a) Decrease in immobility timing (b) Decrease of CRF; increase of 5-HT level |
[45] |
| Rosa disambiguation (Rose) | Villareal et al. (2017) | Rats | EPM | (a) Increase in open arm timing (b) - |
[46] | |
| Rosmarinus officinalis (Rosemary) | Villareal et al. (2017) | Mice | TST | DA, Cort | (a) Decrease in immobility timing (b) Decrease of serum Cort level and increase of brain DA levels |
[47] |
| Cananga odorata (Ylang ylang) | Zhang et al. (2018) | Mice | EPM | 5-HT | (a) Increase in open arm timing and locomotor activity (b) Increase of 5-HT level |
[33] |
3. Absorption of EO Molecules through Inhalation (Mechanisms behind the Effect of EOs on Brain)
EOs are composed of a variety of volatile chemical constituents. To facilitate the absorption of EOs, a novel administrative method utilising nanotechnology has been developed. By encapsulating EOs into nanoparticles, the uptake and effect of them can be enhanced. The inhaled EO molecules will be delivered to the brain region via different pathways according to their molecular sizes. The possible inhalation delivery pathway involves both the olfactory and respiratory systems (Figure 1).
There are three potential basic mechanisms enabling EOs to influence brain functioning. The first mechanism involves the activation of nasal olfactory chemoreceptors and the subsequent effect of olfactory signals on the brain. The olfactory system is unique among the sensory systems for having direct anatomical and functional links with the limbic system. Thus, olfactory stimuli can have a strong effect on mood. The second putative mechanism of action is direct penetration of EO molecules via the olfactory nerve into connected brain areas and the induction of cellular and molecular events. The third potential pathway is the alveolar absorption of EO molecules into the blood circulation, crossing the blood–brain barrier (BBB) to interact with specific brain regions.
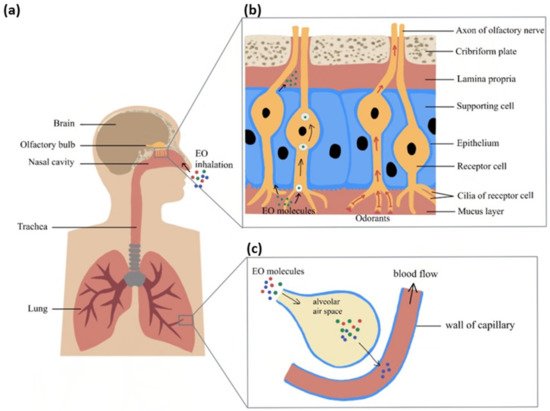
Figure 1. Inhaled EO response delivery to brain through the respiratory and olfactory systems: (a) Inhaled EO passes through the nasal cavity and reaches the olfactory system or respiratory system (b) Overview of EO molecules’ delivery pathway in the olfactory system (c) Overview of EO molecules crossing the air–blood barrier to reach the circulatory system.
4. Effect of EO on Cellular/Molecular Events
4.1. Regulation of Monoamines
According to the 5-HT hypothesis of depression [80], the signs and symptoms of depression are the result of 5-HT deprivation. The 5-HT hypothesis is currently the accepted hypothesis with regard to the pathophysiology of depression. The effect of EOs on the 5-HTergic system has been demonstrated in various studies. In a study, which used compound anshen EO, the inhalation of the EO improved sleep quality and promoted 5-HT increase in experimental mice [82]. An increase of 5-HT-expressing neurons in the dorsal raphe nucleus was found in animals that inhaled EO from asarum heterotropoides for 3 h [45], suggesting that the positive effect of EO inhalation may occur in both acute and chronic conditions.
4.2. Neurogenesis and Neurotrophic Factors
Studies on EOs and neurotrophic factors have mainly focused on the expression levels of brain-derived neurotrophic factor (BDNF). In a clinical study, women whose children were diagnosed with attention deficit and hyperactivity disorder were recruited, assuming that this particular population suffered from considerable stress affecting their mental health [96]. After a 4-week treatment program with EOs, the level of anxiety and depression of the subjects decreased, while the plasma BDNF level (reflecting the brain tissue level of BDNF) significantly increased. In other animal models of depression assessing the effect of EOs, similar findings have been observed as well.
4.3. Regulation of the Neuroendocrine System
It is believed that regulation of hormonal levels is a potential underlying mechanism explaining the effect of EOs, for instance, in the treatment of premenstrual syndrome [99] and menopausal disorder [100,101]. Since stress is a risk factor in depression and anxiety disorders, stress hormone cortisol has been the focus of studies examining the antidepressant and anxiolytic effects of EOs [102]. In human studies, acute exposure to lavender EO has been shown to decrease salivary and serum cortisol levels [103,104]. Simultaneously, findings indicated increased relaxation in subjects, including improved coronary flow velocity [104]. The cortisol-suppressing effect was reported in adults [105], pregnant women [106], mothers of children with developmental dysfunction [96], young children [107], as well as patients undergoing chemotherapy [108]. Apart from lavender, other EOs were also shown to affect cortisol levels, including bergamot [23,109] and grapefruit seed [110].
4.4. Other Possible Mechanisms: Oxidative Stress and Inflammation
Based on the assumption that ROS and inflammatory signalling have a role to play in depression, EOs may be beneficial in depression due to their antioxidant and anti-inflammatory properties. For instance, exposure to lavender and rosemary EOs was found to reduce free radical scavenging activity (FRSA), which further prevents the detrimental effects of oxidative stress [103]. In addition, cinnamomum cassia presl (CC-EO), the active component of cinamaldehyde EO also possesses antioxidant properties [117]. Exposure to MJ was effective in preventing depression-like behaviour induced by lipopolysaccharide (LPS) and attenuated the increase of malondialdehyde (MDA), glutathione (GSH), and tumour necrosis factor-alpha (TNF-α) in mice [113].
5. Future Studies
To facilitate the use of EOs in clinical practice when treating depression and anxiety disorders, further large-scale clinical trials are required to confirm the effectiveness and efficacy of them. Although various studies have illustrated that certain EOs possess antidepressant and anxiolytic effects [15,118], the choice of EOs is not standardised. As the active ingredients may vary among EOs due to non-standardised manufacturing processes, clinical trials with large sample size and standardised EOs as treatment agents are required.
This entry is adapted from the peer-reviewed paper 10.3390/ijms22094844
