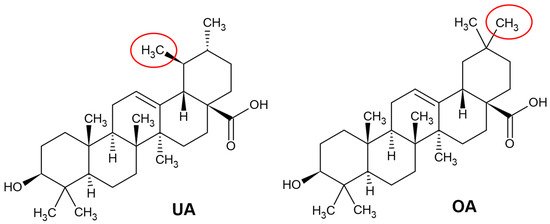
4.1. Neuroprotective Effects of Ursolic and Oleanolic Acids in Neurodegeneration
Neurological disorders can be regarded as impairments of the brain or nervous system, resulting in either physical, psychological or both symptoms. Cerebral ischaemia or brain trauma are examples of acute conditions, while gradual memory loss, neurodegenerative diseases or dementia are associated with aging [
77]. Proper brain function is dependent on neuronal signal transduction and supportive activity of glial cells. The brain is also characterised by the highest metabolic rate among all organs related to the intense ROS or RNS formation and consequently the requirement of an effective antioxidant system [
77]. The main antioxidative enzymes in the brain are glutathione peroxidase (GP), superoxide dismutase (SOD), catalase (CAT), peroxidase, haem oxygenase, quinone oxidoreductase 1 and γ-glutamylcysteine ligase. The expression of various antioxidant enzymes is regulated by nuclear factor erythroid 2-related factor 2 (Nrf2), an important transcription factor involved in the maintenance of redox and metabolic homeostasis. It is also known that non-enzymatic glutathione plays a critical role in ROS scavenging [
77]. Therefore, antioxidant properties are important for potential therapeutic agents. UA has been shown to possess antiradical activity in vitro. Salau et al. [
3] found that UA was more potent than ascorbic acid as reflected by IC
50 values obtained by DPPH (2,2-diphenyl-1-picrylhydrazyl) radical scavenging potential (2.08 μg/mL and 7.64 μg/mL, respectively) and ferric reducing antioxidant power (FRAP) (0.75 μg/mL and 20.17 μg/mL, respectively) assays. Although the difference may arise from the distinction of hydrophilicity and the selectivity of the assays [
78], it strongly suggests the antioxidant potential of UA. Moreover, the pre-treatment with UA has abolished kainate-induced free radical generation in primary culture of hippocampal neurons [
79]. Antioxidant effects of UA have been demonstrated in a wide range of experimental models (see ), both in vitro and in vivo, with single or repeated administration. UA has been shown to increase the activity of CAT [
80,
81,
82], SOD [
3,
77,
79,
81], glutathione (GSH) [
3,
80,
81,
82], GP [
78] and to activate the Nrf2-pathway [
83,
84]. The final result of the majority of experiments was the reduction of lipid peroxidation expressed as the decrease in the level of malondialdehyde (MDA) [
3,
80,
81,
82,
83,
84]. Ex vivo UA has been also able to decrease the activity of α-chymotrypsin, which is known as the marker of oxidative injury [
3]. OA has been found to elicit antioxidant effects in a similar manner to UA. It induced the reduction of intracellular ROS levels in vitro [
85], and it was demonstrated in vivo that OA activated GSH and SOD as well as decreased the level of MDA [
16,
86] (see ).
Neurodegenerative diseases (see also : Parkinson’s or multiple sclerosis experimental models) are associated with neuro-inflammation—a complex process, regulated by microglia and astrocytes [
87]. These cells produce pro-inflammatory factors such as tumour necrosis factor alpha (TNF-α) [
88]. Under certain conditions TNF-α can promote inflammation by activation of nuclear factor-κB (NF-κB) and mitogen-activated protein kinase (MAPK) signalling pathways and induce apoptotic processes [
89]. Therefore, cytokines and transcription factors are feasible targets for anti-inflammatory therapy and the effects of triterpenoids have received considerable attention. It has been shown that prolonged administration of UA can lead to downregulation of the NF-κB pathway [
82,
84,
90], possibly resulting in decreased levels of interleukins IL-1β [
90], IL-12 [
82], IL-6 [
90], interferon gamma (IFN-γ) [
82], matrix metalloproteinase-2 and 9 (MMP-2, MMP-9) [
91]. Moreover, UA can promote the expression of genes encoding anti-inflammatory cytokines IL-4 and IL-10 [
82]. The anti-inflammatory potential of OA has been also demonstrated. For example, OA could decrease the expression levels of TNF-α, IL-1β and IL-6 in BV2 cells [
16].
As UA and OA are able to modulate various anti-inflammatory pathways, they can also have neuroprotective effects. Indeed, it has been reported that UA increased the myelinated area, oligodendrocyte count and myelin basic protein (MBP) content in a multiple sclerosis mouse model after administration for six weeks, as UA acted as an agonist of peroxisome proliferator activated receptor γ (PPARγ) [
92,
93]. It is known that PPAR-dependent transcription factors play a crucial role in the inflammatory response of the CNS by inhibition of NF-κB [
94] and downregulation of genes encoding for pro-inflammatory proteins such as cyclooxygenase-2 (COX-2), MMP-9 [
91], scavenger receptor A, inducible nitric oxide synthase (iNOS), as well as the inhibition of the synthesis of pro-inflammatory cytokines [
95,
96,
97,
98]. It is well documented that NO in the brain is generated by neuronal nitric oxide synthase (nNOS), whereas inflammation triggers the activation of iNOS [
87]. It has been shown that prolonged administration of UA resulted in the reduced activity of iNOS [
77,
89]. Similarly, OA reduced the level of NO in BV2 cells, and this was associated with the downregulation of the expression of the iNOS encoding gene [
16]. Given the multiple interrelated molecular pathways described above, the protective effects of UA and OA can be ascribed to antioxidative and anti-inflammatory activity. Furthermore, the inhibition of apoptosis could also contribute to neuroprotection. Studies using different experimental models indicated that UA could decrease the level of apoptosis effectors, such as caspase 3 [
80,
99] and caspase 9 [
80]. The oxygen-glucose deprivation (OGD) experiments with organotypic hippocampus slices have also demonstrated the protective effect of UA evidenced by modulation of gene expression via AKT/mTOR/HIF-1α pathway, resulting in the increased level of Bcl-2 and the decreased level of Bad [
99].
It is noteworthy that the underlying target of UA and OA might be mitochondria, organelles that are involved in both oxidative stress and neuro-inflammation [
87]. Recently it has been shown that prolonged administration of UA affected the functionality of mitochondrial electron transport chain. In brain mitochondria, UA improved the enzymatic activity of mitochondrial complex I in rotenone-induced Parkinson’s disease model in vivo and increased the expression of mitochondrially encoded cytochrome c oxidase 1 (MrCO1) [
81]. Mitochondrial membrane potential has also been found to be sustained by UA (at 10 μM concentration for 10 min) in an excitotoxicity model of hippocampal neurons [
79]. In another study, it was revealed that after the treatment of PC12 cells with OA, H
2O
2-reduced mitochondrial membrane potential was restored and the activity of succinate dehydrogenase (SDH) was improved [
86]. It is worth mentioning that UA at 1–10 µM concentration had no effect on isolated mouse brain mitochondrial respiration at different metabolic states [
100]. However, it was previously observed that UA had uncoupling and antioxidant effects on rat heart mitochondria [
101]. Thus, the relationship between the administration of UA or OA and the favourable effects on mitochondrial functions under oxidative stress, ischaemic damage or neuro-inflammation requires further investigation as observed outcomes might depend on experimental models.
Table 2. Effects of UA and OA on experimental models of brain pathologies.
4.2. Glioblastoma and Ursolic/Oleanolic Acids
Glioblastoma is the most common and the most aggressive type of primary brain tumour, accounting for approximately 55% of gliomas [
103,
104]. The survival of patients with glioblastoma that have undergone standard treatment encompassing surgical resection and radiation therapy followed by chemotherapy with temozolomide (TMZ) remains within 14–18 months [
105,
106]. More importantly, tumour relapse occurs in almost all patients, and in such cases, glioblastoma often becomes resistant to chemotherapy [
107]. Therefore, novel agents and therapies for the treatment of glioblastoma are needed, as newly developed agents have failed to outmatch TMZ so far [
108].
Recently, in a number of reviews UA/OA-containing plant extracts, purified compounds and their natural or chemically synthesized derivatives have been reported to possess anti-tumour activity in skin, breast, lung, gastric, liver, intestine, prostate and pancreatic cancer models in vitro and in vivo with non-toxic or minimal inhibitory effect on normal cells [
14,
109,
110,
111,
112,
113,
114]. Moreover, new data about the potential of these pentacyclic triterpenoids against glioblastoma have also emerged [
15]. Byun et al. [
115] have recently isolated several C-27-carboxylated OA derivatives (C27OAs) from the dried roots of
Astilbe rivularis, and showed that 3β-hydroxyolean-12-en-27-oic acid, 3β,6β,7α-trihydroxyolean-12-en-27-oic acid and 3β-
trans-
p-coumaroyloxy-olean-12-en-27-oic acid at 10 µM concentration could exclusively sensitize the extrinsic apoptotic pathway via the p38 MAPK and CHOP-mediated DR5 expression without affecting the intrinsic pathway in human LN-428 and U-251 MG glioblastoma cell lines in vitro. The results suggest that certain C27OAs might be developed as specific TNF-related apoptosis-inducing ligand (TRAIL) sensitizers and used as chemotherapy agents in glioblastoma patients with low levels of caspase-8 or p53 activity. In another study [
116], synthetic OA derivatives, C-28 methyl ester (CDDO-Me) and C-28 imidazole (CDDO-Im) of 2-cyano-3,12-dioxooleana-1,9(11)-dien-28-oic acid, have been shown to exhibit potent apoptosis-inducing activity in human U-87 MG and U-251 MG glioblastoma cells. It is interesting that the tested compounds at 2.5–10 µM concentration induced apoptotic cell death through both extrinsic and intrinsic pathways, as the activation of pro-caspases-3, 8 and 9, mitochondrial depolarization and the release of cytochrome c from mitochondria were observed. Moreover, CDDO-Me inhibited the expression of anti-apoptotic and pro-survival signalling molecules (p-Akt, p65 and Notch1) in the same cell lines. In addition, OA has been also investigated for its ability to affect metabolic activity, viability and cell cycle of U-87 cells in vitro [
117]. It was found that after 24 h of treatment OA at 100 µg/mL (approx. 219 µM) induced both apoptosis and necrosis of cancer cells almost to the same extent, and the IC
50 value was determined as 163.6 µg/mL (approx. 358 µM). In addition, OA-treated glioblastoma cells exhibited the increase in expression levels of proteins involved in MAPK signalling, and cell cycle arrest at G1 phase.
UA has been also found to exert a cytotoxic effect in human U-251 MG glioblastoma cells with an IC
50 value as low as 20 µM [
118]. The treatment induced JNK-dependent, caspase-independent and lysosomal associated mechanism of cell death that resulted in rapid mitochondrial membrane depolarisation. In addition, UA demonstrated greater cytotoxicity than conventional chemotherapeutics like TMZ in spite of inactivity towards O-6-methylguanine-DNA methyltransferase (MGMT), which is a known player in TMZ-resistant glioblastomas. UA (at 20 µM) has been also found to induce apoptosis in U-251 cells by suppressing TGF-β1 signalling pathway, thus revealing an alternative mechanism of anti-cancer activity [
119]. In other in vitro glioblastoma models, UA (at 17.5 µM) has been shown to induce necrosis in TMZ-resistant human DBTRG-05MG cells through mitochondrial permeability transition pore opening and ATP level decline [
120] or at 40 µM concentration UA treatment has led to cell cycle arrest at G1 phase, endoplasmic reticulum stress-induced JNK activation and autophagy in U-87 MG cells [
121]. However, UA from
Chamaenerion angustifolium at 50 µM concentration induced both apoptosis and necrosis in U-87 MG cells, and this effect was explained by UA interaction with the PI3K/Akt signalling pathway as predicted by molecular docking [
122]. UA (at 12.5 µM) has also enhanced the cytotoxicity of TMZ in human LN-18 and T98G glioblastoma cells by downregulating MGMT expression, and at 50 mg/kg UA potentiated the efficacy of TMZ in BALB/c mice with LN-18 xenograft [
123]. Furthermore, UA from
Rosmarinus officinalis at 20 µM has reduced IL-1β or TNF-α-induced rat C6 glioma cell invasion in transwell chambers and inhibited the enzymatic activity and expression levels of MMP-9 via the blockage of the NF-kB-dependent pathway [
124]. UA from the methanolic extract of the leaves of
Sarauja roxburghii at 100 µM concentration has also exhibited cytotoxicity against C6 cells in vitro [
125]. Bergamin et al. [
126] found that UA at 15–20 µM increased the number of C6 glioma cells in sub-G1 phase, induced apoptotic cell death and also reduced the expression level and activity of protein kinase B (Akt) in vitro. However, 15 mg/kg/d (for 10 d) of UA did not affect the tumour size in an orthotopic glioma model in vivo [
126]. In another study utilizing an in vivo model of glioblastoma, the anti-tumour effects of triterpenoids have been established [
127]. When C6 tumour-bearing rats were given OA solution by gavage (40 mg daily for 7 d) and underwent irradiation therapy, the combined effect of OA and radiation was demonstrated, which resulted in the decreased growth rates of tumours and the prolonged survival period of tumour-bearing rats.
It is noteworthy that UA (20–100 µM, 48 h of incubation) suppressed metabolic activity, decreased ATP content and increased the number of necrotic cells in both rat C6 glioma and primary mouse astrocyte cell cultures to the same extent [
128]. Thus, it is obvious that the observed OA and UA anti-tumour effects are rather controversial, and additional research is certainly needed to clarify the molecular mechanism of action and neuroprotective potential of these pentacyclic triterpenes.