Probiotics and synbiotics are known to have beneficial effects on human health and disease. Hirsutism, a disorder that is characterised by the presence of coarse terminal hairs in a male-like pattern, is usually caused by elevated androgen levels in blood plasma. This disorder is usually ob-served in PCOS women and it is linked to insulin resistance (IR). Although idiopathic hirsutism (IH) is not shown to have excess androgen production from the ovarian and adrenal glands, in-creased 5α-reductase in peripheral tissues and insulin resistance are common observations.
- probiotics
- synbiotics
- hirsutism
- androgens
- insulin resistance
- PCOS
Note: The following contents are extract from your paper. The entry will be online only after author check and submit it.
1. Introduction
Fermented food, such as yoghurt, bread, bear and wine, has been widely known since ancient times, and some have been used since then, for therapeutic purposes [1–3]. Fermented dairy products (yoghurt, kefir) were used to treat diseases like diarrhea and other infections of the intestinal tract [4,5]. Interaction between microorganisms and human health was first reported in 1907, where yoghurt microflora was described by Elie Metchnikoff [6]. Fermented food is still used as an additional treatment for disease, such as wounds [7–9], gastroenteric disorders and infections [7,10], as well as an overall support for health [7,8,10–12]. The term probiotic was introduced by Werner Kollath [13] and according to the World Health Organisation (WHO), this term refers to the microorganisms that ‘’when administered in adequate amounts, confer a health benefit on the host’’ [14]. Probiotics are found to have multiple beneficial roles on human health and disease, through restoration of gut microbiota (GM) [15,16], symptom improvement on intestinal disease, such as irritable bowel syndrome (IBS) [17], modulation of hormonal profile in animals and humans [18–22] and skin infections and healing [23–25]. Along with the beneficial microorganisms, prebiotics, which are fermented compounds that support and promote modifications in the activity and composition of GM [26], have also been studied. It is shown that a controlled combination of probiotics and prebiotics, called synbiotics, can provide a more enhanced beneficial effect on human health and disease [16,27–29].
Although the effect of probiotics and synbiotics are extensively studied, there has been limited research conducted on their effect on sex hormones and sex hormone imbalances, such as hirsutism, a disorder that is mainly characterised by elevated androgen levels in women. The aim of this review is to focus on the role of probiotics and synbiotics and their metabolic process on hirsutism.
2. Probiotics
Lactobacillus, Streptococcus, Bifidobacterium, Lactococci and Saccharomyces are some of the probiotic species that are known [30]. Microorganisms that are mostly used as treatments are Lactobacillus, Streptococcus, Bifidobacterium and Saccharomyces, whilst most of them are naturally present in the human GM [31–37]. There has been an increase in research on the effect of probiotics on health and disease, whilst they are shown to have both beneficial effects on healthy subjects and therapeutic effect on various diseases and conditions, such as intestinal disease [38–46], skin disease [10,24,47–52] and wound healing [53–57]. Probiotics have also been used for the restoration of disturbed GM [58]. Dysbiosis of gut microbiota (DOGMA) is the alteration of gut microflora that can occur due to a variety of reasons, such as antibiotic use [59,60] and diet [61,62]. The human gut, also described as the ‘’second brain’’ of the human body, plays an important role in human health and disease [63,64]. The GM is known to have a significant role in the functionality of the bowel, maintaining the gut mucosa through their role on gut homeostasis [63–65]. The probiotic E. coli Nissle 1917 protects and prevents against inflammatory response via TLR-4 and TLR-2-dependent pathways, whilst lower counts of Firmicutes prausnitzii are linked with potential inflammatory bowel disease pathogenesis due to its anti-inflammatory effects [65,66]. The impact of the metabolic processing of the gut microflora in the gut is extended outside of the bowel and can impact other functionalities of the human body, reaching the skin [10,24,67–69]. L. casei is shown to reduce skin inflammation through the regulation of CD8+T cells, which initiate inflammatory response [47]. The role of probiotics on endocrinology has also been reported and GM was shown to affect the production of hormones, such as leptin [62,70,71], stress hormones [72], insulin [73,74] and sex hormones [75,76] in the intestinal tract. Additionally, the disturbance of gut microbiota can affect the levels of endogenous hormones, such as estrogens, as well as administrated steroids, such as megestrol acetate, medroxyprogesterone acetate, norethisterone and others, suggesting that the use of antibiotics can cause hormonal imbalance and reduce the absorption of contraceptive hormones, which are used as a method of birth control and/or treatment for metabolic syndromes [75]. An altered microbiota during the early life of the diabetic mouse (Type 1) can determine sex hormones and cause metabolic changes, such as increased testosterone levels [76]. Administration of probiotics can restore the imbalanced microorganisms that live in the human intestine and improve certain conditions through their metabolic processes [58]. Additionally, DOGMA is also observed in patients suffering from inflammatory bowel disease, colitis [77], Crohn’s disease, IBS [63], polycystic ovary syndrome (PCOS) [78] and other conditions.
3. Synbiotics
Synbiotics are the controlled combination of probiotics and prebiotics and their supplementation aims to provide a more enhanced health benefit on human health and disease. Known prebiotics are fructans (e.g. inulin), complex polysaccharides, oligosaccharides and sugar alcohols [16,79] and in combination with probiotics, they have been used for the treatment of conditions and disease [18,27,28,80,81]. Synbiotics containing L. acidophilus NCC90, oligofructose and acacia gum can have a preventive role on bone mineral loss after ovariectomy in rats [16]. It has been reported that synbiotic treatments showed beneficial effects on non-alcoholic fatty liver disease (NAFLD), reducing fibrosis and hepatic steatosis in humans [82,83], total necrosis factor α (TNF-α), total nuclear factor κ-B (TNF-κB) and other NAFLD biomarkers, such as high-sensitivity C-reactive protein [83]. Moreover, synbiotics can bring improvements on Crohn’s disease through reduction in TNF-α production [84], IBS [85] and delayed Alzheimer’s disease in Drosofila melanogaster [86]; improvement of thyroid function was observed after 8 weeks of synbiotic supplementation in hypothyroid patients, decreasing thyroid stimulating hormone (TSH) levels and increasing tri-iodothyronine (FT3), whilst overall increasing FT3/TSH ratio [18]. Bifidobacterium Longum in combination with inulin, reduced levels of TNF-α and IL-1α in patients suffering from ulcerative colitis [77]. Another study on patients with ulcerative colitis showed that B. breve and galacto-oligosaccharide (GOS)-containing beverage (Yakult) managed to clinically improve the condition of the patients, through reduction of UC markers, such as myeloperoxidase, and by lowering the faecal pH [87].
4. Hirsutism
Hirsutism is a condition that appears in 5–10% of women and it is recognized by the presence of coarse terminal hairs in a male-like pattern [88]. Excess hair growth that consists of terminal hairs are present in areas were women normally have thinner hair. The clinical diagnosis of hirsutism is completed based on Ferriman and Gallwey criteria
(Figure 1) [88] and the areas that are scored include the face, chest, thighs, upper arms, abdomen and back. Scores (m-FG) from 1–4, with 1 describing minimal terminal hair and 4 describing frank virilization, are given to the mentioned areas whist total scores less than 8 are considered normal [88].
Figure 1. Hirsutism scoring system presenting scores ranking from 1—minimal hirsutism, to 4 virilization in 9 body parts. A total score of less than 8 is considered normal, whereas higher scores indicate mild to severe hirsutism [88].
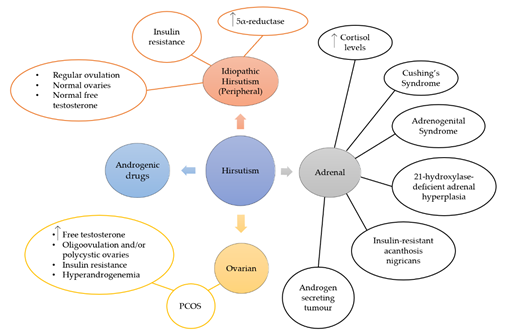
Hirsutism is a quite complex condition that can occur due to other syndromes or disease, such as PCOS (Figure 2). Although the main reason for this condition is the presence of excess androgens, such as testosterone (T) and dihydrotestosterone (DHT), IH shows normal levels of androgens [89,90]. The most common reason for the excess androgen levels is PCOS and 60–80% of PCOS women suffer from hirsutism [91]. The diagnosis of this condition is conducted according to the Rotterdam criteria, by which two of the three criteria have to be met: a) evidence of hyperandrogenism, b) oligo- and/or anovulation and c) polycystic ovaries [92]. Other clinical features are ovarian enlargement and IR, which is found to be very common amongst PCOS women, whilst the syndrome has also been linked with cardiovascular disease and inflammation. The heritability of this disorder has been studied and it is possible that genetic changes on the androgen receptor gene can lead to hirsutism [90]. During this study, a repeatability of the trinucleotide CAG in exon 1 was observed and more frequent repeats in the N-terminal domain of the androgen gene were linked with the development of the disorder. However, other researchers have not shown a significant role of CAG in the pathogenesis of hirsutism [93,94]. Hirsutism has also been linked with IR (Figure 3) [91,95–101], whilst excess insulin production leads to hyperinsulinemia, which increases luteinizing hormone (LH) through insulin receptor stimulation [97]. LH, along with follicle-stimulating hormone (FSH), is a hormone that regulates androgen production through the secretion of them from ovarian and adrenal glands. Moreover, high levels of insulin inhibit sex hormone-binding globulin (SHBG), a hormone that binds with plasma T and is considered its major determinant along with 17-β hydroxysteroids from plasma [102]. Consequently, both effects of IR are directly linked with hirsutism through excess androgen production. This relationship between IR and hirsutism was studied in healthy women, where adipose tissue was collected and in-vitro treatments with testosterone and/or anti-androgens were conducted on insulin stimulated adipose cells [100].
Figure 2. Hirsutism can originate from adrenal or ovarian disorders, or both. Various syndromes and disorders related to the adrenal glands, such as Cushing’s syndrome, adrenogenital syndrome, 21-hydroxylase-deficient adrenal hyperplasia, insulin-resistant acanthosis nigricans and androgen secreting tumour, show high levels of cortisol hormone and hirsutism. Ovarian hirsutism is caused by PCOS that is characterised from high levels of free testosterone and/or polycystic ovaries, insulin resistance and hyperandrogenemia. Idiopathic hirsutism is caused by peripheral increase of androgens, and women that suffer from it show increased levels of 5α-reductase and insulin resistance, whilst they do not show any abnormalities in their ovarian or adrenal function.
Adipose tissue contains adipocytes, also known as fat cells and are responsible for fat energy storage. This study showed that the exposure of these cells to testosterone led to insulin resistance, suggesting there is a link between hirsutism, androgen presence and insulin resistance development.
Other disorders that are known for the increased production of androgens are hyperandrogenic insulin-resistant acanthosis nigricans syndrome [103,104], 21-hydroxylase-deficient non-classic adrenal hyperplasia [90,105], androgen-secreting tumor [106], and rarely androgenic drug intake [107]. On the other hand, the causes of IH are not well known. However, when hormonal profiles of PCOS women and IH women were compared, IR was found to be significant in both groups compared to the control group. IR and hyperinsulinemia increase the insulin-like growth factor (IGF) which affects hair follicles [95,96], and therefore it is suggested that IR is potentially a cause of IH. This disorder is also characterised as an increase in 5α-reductase in peripheral tissues, an enzyme that converts T to DHT, and is generally responsible for the metabolism of steroids [95]. Potential causes of IH include increased sensitivity of hair follicles to androgens, and androgen receptor gene polymorphism [96].
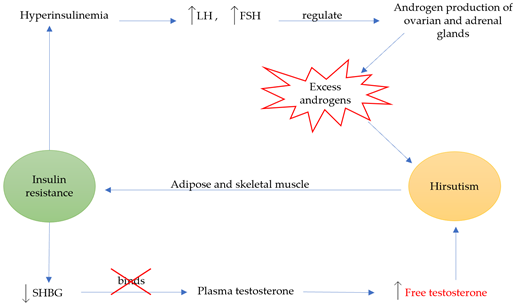
Figure 3. The relationship between insulin resistance and hirsutism. Hyperinsulinemia is caused when insulin resistance is left unmanaged, causing an increase in LH and FSH, which regulate the production of ovarian and adrenal androgens. This increase results in excess androgens, and eventually hirsutism. Moreover, insulin resistance reduces SHBG, which leaves plasma testosterone unbound leading to increased free testosterone and hirsutism. Chronic androgen exposure leads to adipose and skeletal muscle insulin resistance. The graph above presents the circular relationship between the two conditions, leading to a vicious cycle of effects.
This entry is adapted from the peer-reviewed paper 10.3390/fermentation7010010