Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is an old version of this entry, which may differ significantly from the current revision.
Subjects:
Infectious Diseases
Helicobacter pylori is a class I carcinogen that infects more than 100 million individuals in the United States. Antimicrobial therapy for H. pylori has typically been prescribed empirically rather than based on susceptibility testing.
- clarithromycin
- antimicrobial stewardship
- Helicobacter pylori
1. Introduction
Helicobacter pylori infects approximately one-half of the world’s population and causes gastritis/gastric atrophy that may result in peptic ulcer disease and/or gastric cancer [1]. The problems of providing effective H. pylori therapy are not currently being embraced by the infectious disease community. For example, triple therapy that combines clarithromycin, amoxicillin, and an antisecretory drug called clarithromycin remains the most used regimen despite generally poor cure rates [2,3,4,5]. The regimen was approved by the U.S. Food and Drug Administration (FDA) in 1996, at which time the FDA’s focus was on ulcer healing and recurrence rather than on the treatment of a new infectious disease [6,7,8]. Because the clinical manifestations were gastrointestinal and obtaining cultures required gastroscopy, this has led to the functional transfer of H. pylori from infectious disease to gastroenterology, which has managed the disease as any another common GI disease [9] and without employing the principles of antibiotic stewardship [10,11,12].
Antimicrobial resistance among H. pylori rapidly increased such that clarithromycin, nitroimidazoles, and fluoroquinolones are no longer effective when given empirically [13]. Nonetheless, clarithromycin-containing triple therapy remains the most widely used anti-H. pylori regimen worldwide [14,15]. Gastroenterology considered the unavailability of susceptibility testing as unsolvable, requiring “work arounds”. One approach was to add another antibiotic or antibiotics to current regimens to produce multi-antibiotic clarithromycin-containing regimens (e.g., sequential, hybrid, and concomitant therapies) (reviewed in [12]). The most successful regimen was concomitant therapy [16], which is equivalent to the simultaneous administration of clarithromycin and metronidazole triple therapies. Concomitant therapy failure requires resistance to both metronidazole and clarithromycin [17].
The FDA recently approved vonoprazan–clarithromycin–amoxicillin triple therapy in which more than 90% of patients receive clarithromycin unnecessarily [20]. Vonoprazan is a potassium-competitive acid blocker (P-CAB), more potent than traditional PPIs. The effectiveness of vonoprazan triple therapy is driven by the success of the dual P-CAB plus amoxicillin component [20,21].
2. Effect of Clarithromycin Resistance on Treatment Success
Clarithromycin resistance is considered “all or none”, such that clarithromycin resistance reduces clarithromycin triple therapy effectively to just amoxicillin and the antisecretory drug. This results in resistant infections receiving a PPI or P-CAB plus amoxicillin dual therapy and susceptible infections receiving PPI or P-CAB plus amoxicillin and clarithromycin. The results are visualized using an H. pylori nomogram (Figure 1) [22].
High H. pylori cure rates with amoxicillin require the antisecretory drug to achieve and sustain a high pH [23]. Effectiveness is thus positively related to the potency of the antisecretory drug and inversely correlated with the ability of the stomach to make acid. PPIs’ relative potency is assessed as the proportion of a 24-h day during which the pH is maintained at pH 4 or above (pH4 time) [24]. Pantoprazole, omeprazole, and lansoprazole are rapidly metabolized by CYP2C19, which reduces their effectiveness in populations where rapid metabolizers are common (e.g., most of the Western world). Rabeprazole and esomeprazole are the most potent PPIs and are minimally affected by CYP2C19. They are preferred PPIs for H. pylori therapy [25].
Amoxicillin dual therapy using traditional PPIs is unable to reliably cure a high proportion of cases in Western populations. In contrast, rabeprazole or esomeprazole dual therapies have often proved effective in Japan and in some Chinese populations [26,27,28,29,30,31,32,33,34,35].
3. Potassium-Competitive Acid Blockers (P-CABs)
The effectiveness of vonoprazan plus antibiotics for the treatment of H. pylori infections was first demonstrated in Japan [36]. The Japanese pivotal clinical study compared b.i.d dosing of a low potency PPI (lansoprazole 30 mg; equivalent to 27 mg omeprazole) [24] with 20 mg of vonoprazan (approximately equivalent to >40 mg of esomeprazole b.i.d.), each given b.i.d. for the cure of H. pylori infections [36]. With clarithromycin-susceptible infections, both the vonoprazan- and PPI-containing triple therapies produced high (~97%) and near-identical cure rates [36]. However, in the presence of clarithromycin resistance, the regimens were reduced to the antisecretory drug plus amoxicillin. The cure rates of the dual therapies were therefore dependent on the relative antisecretory potency of the antisecretory drug (i.e., the cure rate was 40% with lansoprazole vs. 82% with the more potent vonoprazan) [21]. The overall high cure rate obtained (82%) with clarithromycin resistance was consistent with the notion that clarithromycin was responsible for only a small proportion of those cured (i.e., 82% would have been cured without clarithromycin) [21]. It was also noted that the optimization of the vonoprazan–amoxicillin dual therapy should produce a highly effective dual therapy without the need for clarithromycin. However, vonoprazan triple therapy was introduced despite more than 80% receiving unneeded clarithromycin. Vonoprazan–clarithromycin triple therapy is currently the most widely used treatment of H. pylori in Japan with more than 1.5 million patients treated yearly [37]. However, over time, the overall cure rates have fallen closer to 80% as clarithromycin resistance has continued to increase [38]. In the U.S./European trial, the cure rates for both clarithromycin-susceptible and resistant strains were unacceptably low and the proportion receiving unneeded clarithromycin was higher (>90%) (see below) [39]. Despite the poor outcomes, both vonoprazan triple and dual therapies were approved in the United States and Europe, although neither has yet been released due to manufacturing issues.
4. Unnecessary Clarithromycin Resulting from Vonoprazan Triple Therapy
The results of the Japanese pivotal study (high success with the amoxicillin dual therapy and a high rate of unnecessary clarithromycin) have been confirmed by 11 vonoprazan triple therapy studies that provide cure rates in relation to clarithromycin resistance (i.e., the success is attributable to the amoxicillin) [36,40,41,42,43,44,45,46,47,48,49,50] (Figure 1).
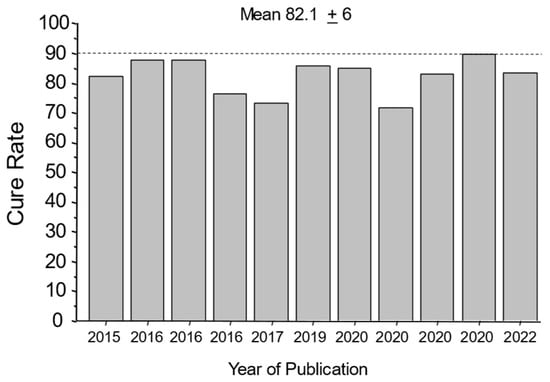
Figure 1. Cure rates with 7-day vonoprazan, clarithromycin, and amoxicillin therapy in the presence of clarithromycin-resistant infections in Japan. This illustrates the high proportion of patients cured while functionally receiving only the amoxicillin.
The mean cure rate attributable to amoxicillin dual therapy with a 7-day vonoprazan triple therapy was 81.7 ± 6% [36,40,41,42,43,44,45,46,47,48,49,51]. A second approach to quantitate the proportion receiving unnecessary clarithromycin was to examine the cure rates of dual therapy (which functionally contains no clarithromycin) vs. triple therapy with clarithromycin in the same populations (Figure 2A) [50]. These different comparisons all confirmed that the majority of the clarithromycin given in vonoprazan triple therapy was unneeded.
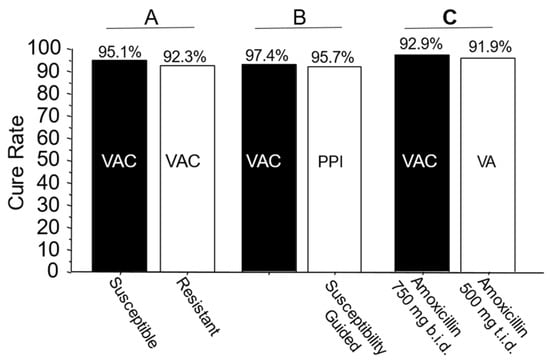
Figure 2. Examples of comparative studies in Japan. Legend: Panel A: Cure rates of 7-day vonoprazan, clarithromycin, and amoxicillin therapy in clarithromycin-susceptible and resistant infections in Japan. The resistant infections are functionally seen in vonoprazan and amoxicillin dual therapy. Panel B: Comparison of the effectiveness of vonoprazan–clarithromycin triple therapy vs. susceptibility-based PPI clarithromycin triple therapy in the same population. Panel C: Comparison of 7-day vonoprazan triple and dual therapy in the same population. In the triple therapy, 1500 mg of amoxicillin was given as 750 b.i.d. vs. 500 mg t.i.d. in the dual therapy. VAC—vonoprazan, amoxicillin, clarithromycin; PPI AC—PPI, amoxicillin, clarithromycin; VA—vonoprazan, amoxicillin. Vonoprazan was 20 mg b.i.d., clarithromycin was 200 mg b.i.d., amoxicillin was 750 mg b.i.d. except where shown.
The U.S./European vonoprazan–amoxicillin–clarithromycin clinical trial differed from the Japanese trials in dosing, duration, and effectiveness. Despite higher doses of antibiotics and doubling the duration from 7 to 14 days, both the U.S./European study and a study in Thailand yielded relatively poor cure rates compared to Japan, even with susceptible strains (e.g., 85.7% with the P-CAB) [39,54]. This was both unexpected and unprecedented [20,55] (Figure 3).
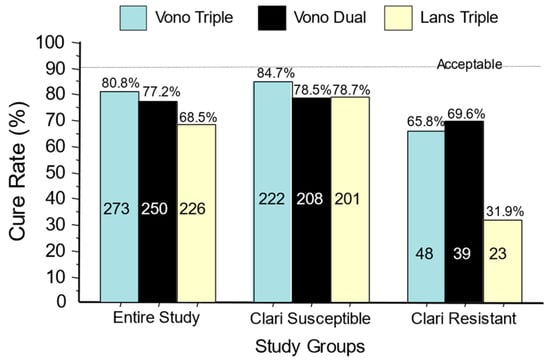
Figure 3. Cure rates for the U.S./European vonoprazan clinical trial of vonoprazan, clarithromycin, and amoxicillin; vonoprazan plus amoxicillin dual therapy; and lansoprazole–clarithromycin triple therapy. The data are shown for the entire group and separately for those with clarithromycin-susceptible infections and those with clarithromycin-resistant infections. No arm achieved the expected cure rate of >90%.
The cure rate with susceptible strains using amoxicillin b.i.d. was 6.2% greater than dual therapy with amoxicillin t.i.d. The proportion receiving unnecessary clarithromycin was also evaluated both in relation to the differences in cure rates with susceptible vs. resistant infections and with dual vs. triple therapies (Figure 3 and Figure 4) [20].
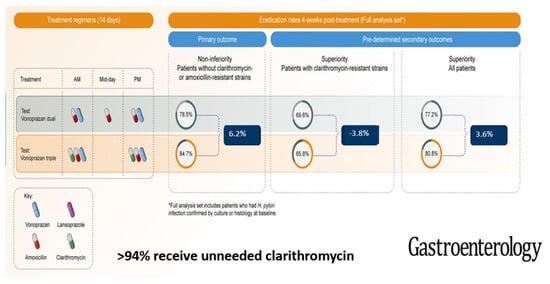
Figure 4. Results of the U.S./European vonoprazan clinical trial graphical abstract, limited to the comparison of the vonoprazan triple and dual arms. Modification consisted of subtraction of the results with vonoprazan dual therapy from the results with triple therapy to show the relative benefits of adding clarithromycin. The vonoprazan dual therapy contained 3 g of amoxicillin vs. 2 g for the triple therapy, which also contained clarithromycin. The maximum difference in those with susceptible strains was 6.2%, showing that >93% received no antimicrobial benefits from the presence of clarithromycin.
5. Quantifying the Amount of Unnecessary Clarithromycin Used with Vonoprazan Triple Therapy
In Japan, the quantity of clarithromycin used per million cases treated using either the 200 or 400 mg b.i.d. approved dosages of clarithromycin (i.e., dose times duration times the number participants) would be, respectively, 2800 kg and 5600 kg. In the United States and Europe, where the clarithromycin dosage is 1 g/day for 14 days, the results per million treated is equivalent to 14,000 kg/year or 6.35 tons/year/million treated. In both instances, 80% to 90% of the clarithromycin would be unnecessary (i.e., misused). As noted above and evident in Figure 4, optimizing the vonoprazan–amoxicillin dual therapy should achieve equivalent or superior results without the need for clarithromycin.
This entry is adapted from the peer-reviewed paper 10.3390/pharma3010006
This entry is offline, you can click here to edit this entry!
