Nucleic acid-based therapies have the potential to address numerous diseases that pose significant challenges to more traditional methods. RNA-based therapies have emerged as a promising avenue, utilizing nanoformulation treatments to target a range of pathologies. Nanoformulation offers several advantages compared to other treatment modalities, including targeted delivery, low toxicity, and bioactivity suitable for drug loading. Various types of nanoformulations are available, such as liposomes, polymeric nanoparticles (NPs), magnetic NPs, nanoshells, and solid lipid nanoparticles (SLNs). RNA-based therapy utilizes intracellular gene nanoparticles with messenger RNA (mRNA) emerging prominently in cancer therapy and immunotechnology against infectious diseases. The approval of mRNA-based technology opens doors for future technological advancements, particularly self-amplifying replicon RNA (repRNA). RepRNA is a novel platform in gene therapy, comprising viral RNA with a unique molecular property that enables the amplification of all encoded genetic information countless times. As a result, repRNA-based therapies have achieved significant levels of gene expression.
- RNA replicon therapy
- RNA replicon vaccines
- self-amplifying RNA
1. Introduction
2. Nanotechnology’s Impact on Healthcare: Advancements, Applications, and RNA Nanotechnology
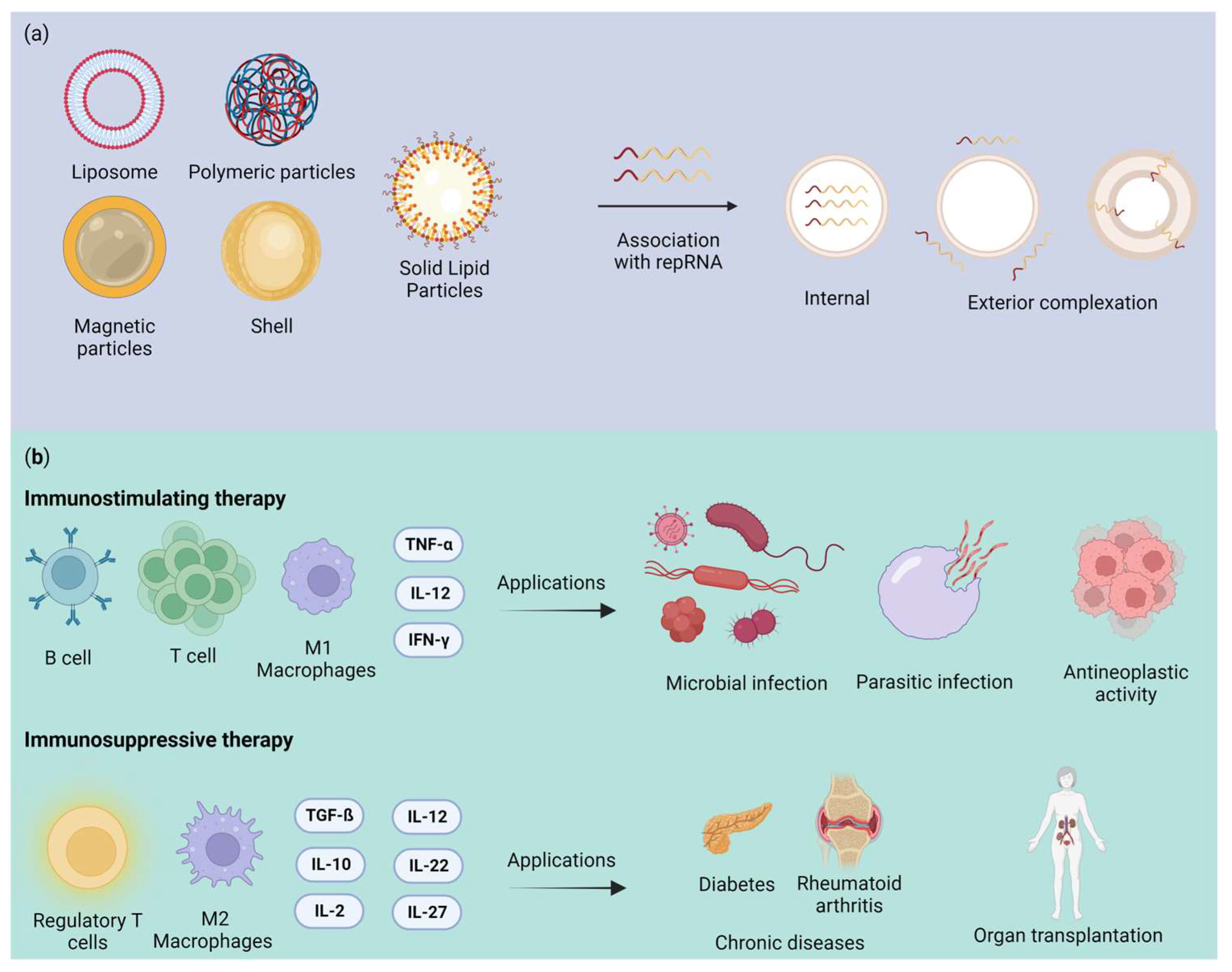
2.1. Nanoformulation
|
Classification |
Name (Trade Tame) |
Main Component |
Delivery Route |
Indication |
Approval (Year) |
|---|---|---|---|---|---|
|
Liposome |
AmBisome |
Liposomal amphotericin B |
Intravenous |
Fungal/protozoal infections |
FDA (1997) EMA (2006) ANVISA (1997) |
|
Doxil/ Caelyx |
Liposomal doxorubicin |
Intravenous |
Antineoplastic agents (ovarian and breast cancer; multiple myeloma; Karposi’s Sarcoma) |
FDA (1995, 2005, 2008) EMA (1996) ANVISA (2011) |
|
|
Myocet (Myoce liposomal) |
Liposomal doxorubicin |
Intravenous |
Antineoplastic agents (breast neoplasms) |
FDA (2000) EMA (2000) |
|
|
Visudyne |
Liposomal verteporfin |
Intravenous |
Ophthalmic agents (myopia; ocular histoplasmosis; macular degeneration, wet age-related) |
FDA (2000) ANVISA (2004) EMA (2007) |
|
|
Marqibo |
Liposomal vincristine |
Intravenous |
Antineoplastic agents (hematologic malignancies and solid tumors) |
FDA (2012) |
|
|
Onivyde (Onivyde pegylated liposomal) |
Liposomal irinotecan |
Intravenous |
Antineoplastic agents (pancreatic cancer) |
FDA (2015) EMA (2016) |
|
|
Polymer-based nanoparticles |
Eligard |
Leuprolide acetate and polymer (PLGH (poly (DL-Lactide-co-glycolide))) |
Subcutaneous |
Antineoplastic agents (prostate cancer) |
FDA (2002) ANVISA (2006) |
|
Mircera |
Methoxy polyethylene glycol-epoetin beta |
Subcutaneous/ Intravenous |
Anemia associated with chronic kidney disease |
FDA (2007) EMA (2007) ANVISA (2008) |
|
|
Cimzia |
PEGylated antibody fragment (Certolizumab) |
Subcutaneous |
Anti-inflammatory action (Crohn’s disease; rheumatoid arthritis; psoriatic arthritis; ankylosing spondylitis) |
FDA (2008, 2009, 2013) EMA (2009) ANVISA (2017) |
|
|
PegIntron |
PEGylated IFN alpha-2b protein |
Subcutaneous |
Immunomodulator (hepatitis C) |
FDA (2001) EMA (2000) ANVISA (2011) |
|
|
Magnetic nanoparticles |
NanoTherm |
Iron oxide coated with amino silane |
Intratumoral injection |
Antineoplastic agents (glioblastoma) |
FDA (2010) EMA (2013) |
|
Feraheme |
Iron oxide and a polyglucose sorbitol carboxymethyether |
Intravenous |
Treatment of anemia |
FDA (2009) EMA (2012) |
|
|
Lipid nanoparticle |
Patisiran (Onpattro) |
Phospholipids, cholesterol, ionizable cationic lipid (DLin-MC3-DMA), and polyethylene glycol-modified lipid |
Intravenous |
Polyneuropathy |
FDA (2018) |
2.2. Nanotoxicology Challenges and Opportunities
3. Virus-Based Delivery System
4. Advantages and Challenges of Replicon RNA Therapy
|
Carrier |
RNA Replicon |
Results |
Reference |
|---|---|---|---|
|
Cationic nanocarrier |
RepRNA PMIF (macrophage migration inhibitory factor and cytokine). |
It improved host cellular and humoral immunity against Plasmodium infection in the liver and blood and conferred complete protection against malaria reinfection in murine mice. |
[71] |
|
Nanostructured lipid transporters (NLCs) |
RepRNA ZIKV-117 mAb. |
Rapid protection against Zika virus infection in mice. |
[72] |
|
Lipid InOrganic Nanoparticles (LION) |
LION/repRNA-CoV2S |
LION/repRNA-CoV2S vaccine intramuscularly to mice, a significant amount of anti-SARS-CoV-2 S protein IgG antibody isotypes, resembling a Type 1 T helper cell response, were produced. |
[63] |
|
Cationic nanocarrier |
RepRNA CCHFV (Crimean–Congo hemorrhagic fever virus) encoding NP (nucleoprotein), GPC (glycoprotein precursor) or both |
It provided robust protection against Crimean–Congo hemorrhagic fever virus in lethal mice. |
[73] |
|
Cationic liposomes |
samPfRH5 replicon (Plasmodium falciparum reticulocyte binding protein homologue 5) |
The liposome–replicon complexes showed high transfection efficiencies. They elicited antibodies capable of inhibiting the growth of the parasite in vitro |
[74] |
|
Mannosylation of lipid nanoparticles (LNPs) |
Self-amplifying mRNA encoded an influenza (hemagglutinin) |
Compared to LNPs, mannnosylated lipid nanoparticles (MLNPs) showed higher levels of IgG1 and IgG2a. |
[75] |
|
Polymeric nanoparticle |
Nanoparticle (MDNP)-delivered VEEV replicon RNA encoding the hemagglutinin protein (HA) of an H1N1 influenza virus (A/WSN/33) or the Ebola virus (EBOV) glycoprotein (GP) |
The vaccine elicits both CD8+ T-cell and antibody responses and can be created with numerous antigen-expressing replicons. |
[76] |
This entry is adapted from the peer-reviewed paper 10.3390/ph16121634
References
- Lundstrom, K. Nanoparticle-Based Delivery of Self-Amplifying RNA. Gene Ther. 2020, 27, 183–185.
- Sergeeva, O.V.; Koteliansky, V.E.; Zatsepin, T.S. MRNA-Based Therapeutics–Advances and Perspectives. Biochemistry 2016, 81, 709–722.
- Guo, P.; Haque, F.; Hallahan, B.; Reif, R.; Li, H. Uniqueness, Advantages, Challenges, Solutions, and Perspectives in Therapeutics Applying RNA Nanotechnology. Nucleic Acid. Ther. 2012, 22, 226–245.
- Tenchov, R.; Bird, R.; Curtze, A.E.; Zhou, Q. Lipid Nanoparticles from Liposomes to MRNA Vaccine Delivery, a Landscape of Research Diversity and Advancement. ACS Nano 2021, 15, 16982–17015.
- Beck, J.D.; Reidenbach, D.; Salomon, N.; Sahin, U.; Türeci, Ö.; Vormehr, M.; Kranz, L.M. MRNA Therapeutics in Cancer Immunotherapy. Mol. Cancer 2021, 20, 69.
- Sahin, U.; Karikó, K.; Türeci, Ö. MRNA-Based Therapeutics-Developing a New Class of Drugs. Nat. Rev. Drug Discov. 2014, 13, 759–780.
- Démoulins, T.; Englezou, P.C.; Milona, P.; Ruggli, N.; Tirelli, N.; Pichon, C.; Sapet, C.; Ebensen, T.; Guzmán, C.A.; McCullough, K.C. Self-Replicating RNA Vaccine Delivery to Dendritic Cells. In Methods in Molecular Biology; Humana Press Inc.: Totowa, NJ, USA, 2017; Volume 1499, pp. 37–75.
- Lin, G.; Yan, H.; Sun, J.; Zhao, J.; Zhang, Y. Self-Replicating RNA Nanoparticle Vaccine Elicits Protective Immune Responses against SARS-CoV-2. Mol. Ther. Nucleic Acids 2023, 32, 650–666.
- Lundstrom, K. Self-Replicating RNA Viruses for RNA Therapeutics. Molecules 2018, 23, 3310.
- Nakamura, A.; Kotaki, T.; Nagai, Y.; Takazawa, S.; Tokunaga, K.; Kameoka, M. Construction and Evaluation of a Self-Replicative RNA Vaccine against SARS-CoV-2 Using Yellow Fever Virus Replicon. PLoS ONE 2022, 17, e0274829.
- Dana, H.; Mahmoodi Chalbatani, G.; Mahmoodzadeh, H.; Karimloo, R.; Rezaiean, O.; Moradzadeh, A.; Mehmandoost, N.; Moazzen, F.; Mazraeh, A.; Marmari, V.; et al. Molecular Mechanisms and Biological Functions of SiRNA. Int. J. Biomed. Sci. IJBS 2017, 13, 48–57.
- Alshaer, W.; Zureigat, H.; Al Karaki, A.; Al-Kadash, A.; Gharaibeh, L.; Hatmal, M.M.; Aljabali, A.A.A.; Awidi, A. SiRNA: Mechanism of Action, Challenges, and Therapeutic Approaches. Eur. J. Pharmacol. 2021, 905, 174178.
- Yu, B.; Tai, H.C.; Xue, W.; Lee, L.J.; Lee, R.J. Receptor-Targeted Nanocarriers for Therapeutic Delivery to Cancer. Mol. Membr. Biol. 2010, 27, 286–298.
- Friedrich, M.; Aigner, A. Therapeutic SiRNA: State-of-the-Art and Future Perspectives. BioDrugs 2022, 36, 549–571.
- Shu, Y.; Pi, F.; Sharma, A.; Rajabi, M.; Haque, F.; Shu, D.; Leggas, M.; Evers, B.M.; Guo, P. Stable RNA Nanoparticles as Potential New Generation Drugs for Cancer Therapy. Adv. Drug Deliv. Rev. 2014, 66, 74–89.
- Li, M.; Li, Y.; Li, S.; Jia, L.; Wang, H.; Li, M.; Deng, J.; Zhu, A.; Ma, L.; Li, W.; et al. The Nano Delivery Systems and Applications of MRNA. Eur. J. Med. Chem. 2022, 227, 113910.
- Antunes Filho, S.; Backx, B.P. Nanotecnologia e Seus Impactos Na Sociedade. Rev. Tecnol. Soc. 2020, 16, 1–15.
- Bayda, S.; Adeel, M.; Tuccinardi, T.; Cordani, M.; Rizzolio, F. The History of Nanoscience and Nanotechnology: From Chemical-Physical Applications to Nanomedicine. Molecules 2020, 25, 112.
- Fialkoski, D.; Malfatti, C.R.M. Nanotecnologia: Uma Prospecção Tecnológica No Âmbito Nacional e Internacional. Cad. Prospecção 2019, 12, 590.
- Nunes, A.R.; Costa, E.C.; Alves, G.; Silva, L.R. Nanoformulations for the Delivery of Dietary Anthocyanins for the Prevention and Treatment of Diabetes Mellitus and Its Complications. Pharmaceuticals 2023, 16, 736.
- Chakravarty, M.; Vora, A. Nanotechnology-Based Antiviral Therapeutics. Drug Deliv. Transl. Res. 2021, 11, 748–787.
- Cui, F.; Liu, J.; Pang, S.; Li, B. Recent Advance in Tumor Microenvironment-Based Stimuli-Responsive Nanoscale Drug Delivery and Imaging Platform. Front. Pharmacol. 2022, 13, 929854.
- Guo, P. The Emerging Field of RNA Nanotechnology. Nat. Nanotechnol. 2010, 5, 833–842.
- Jasinski, D.; Haque, F.; Binzel, D.W.; Guo, P. Advancement of the Emerging Field of RNA Nanotechnology. ACS Nano 2017, 11, 1142–1164.
- Guo, P.; Zhang, C.; Chen, C.; Garver, K.; Trottier, M. Inter-RNA Interaction of Phage Φ29 PRNA to form a Hexameric Complex for Viral DNA Transportation. Mol. Cell 1998, 2, 149–155.
- Zafar, A.; Alruwaili, N.K.; Imam, S.S.; Alharbi, K.S.; Afzal, M.; Alotaibi, N.H.; Yasir, M.; Elmowafy, M.; Alshehri, S. Novel Nanotechnology Approaches for Diagnosis and Therapy of Breast, Ovarian and Cervical Cancer in Female: A Review. J. Drug Deliv. Sci. Technol. 2021, 61, 102198.
- Maji, R.; Dey, N.S.; Satapathy, B.S.; Mukherjee, B.; Mondal, S. Preparation and Characterization of Tamoxifen Citrate Loaded Nanoparticles for Breast Cancer Therapy. Int. J. Nanomed. 2015, 9, 3107–3118.
- Carvalho Lopes, J.; Pereira Torres, M.L. Utilização de Nanopartículas No Tratamento Do Câncer: Aspectos Gerais, Mecanismos de Ação Antineoplásicos e Aplicabilidades Tumorais. Rev. Bras. Cancerol. 2020, 65, e-13400.
- Assadpour, E.; Rezaei, A.; Das, S.S.; Krishna Rao, B.V.; Singh, S.K.; Kharazmi, M.S.; Jha, N.K.; Jha, S.K.; Prieto, M.A.; Jafari, S.M. Cannabidiol-Loaded Nanocarriers and Their Therapeutic Applications. Pharmaceuticals 2023, 16, 487.
- Lashkari, A.; Ranjbar, R. Nanoparticles and Nanoformulated Drugs as Promising Delivery System in Treatment of Microbial-Induced CNS Infection: A Systematic Review of Literature. J. Neurovirol. 2021, 27, 542–549.
- Lopalco, A.; Denora, N. Nanoformulations for Drug Delivery: Safety, Toxicity, and Efficacy. In Methods in Molecular Biology; Humana Press Inc.: Totowa, NJ, USA, 2018; Volume 1800, pp. 347–365.
- Sharma, S.; Parveen, R.; Chatterji, B.P. Toxicology of Nanoparticles in Drug Delivery. Curr. Pathobiol. Rep. 2021, 9, 133–144.
- Huang, H.J.; Lee, Y.H.; Hsu, Y.H.; Liao, C.T.; Lin, Y.F.; Chiu, H.W. Current Strategies in Assessment of Nanotoxicity: Alternatives to in Vivo Animal Testing. Int. J. Mol. Sci. 2021, 22, 4216.
- Savage, D.T.; Hilt, J.Z.; Dziubla, T.D. In Vitro Methods for Assessing Nanoparticle Toxicity. In Methods in Molecular Biology; Humana Press Inc.: Totowa, NJ, USA, 2019; Volume 1894, pp. 1–29.
- Chenthamara, D.; Subramaniam, S.; Ramakrishnan, S.G.; Krishnaswamy, S.; Essa, M.M.; Lin, F.H.; Qoronfleh, M.W. Therapeutic Efficacy of Nanoparticles and Routes of Administration. Biomater. Res. 2019, 23, 20.
- Gupta, R.; Xie, H. Nanoparticles in Daily Life: Applications, Toxicity and Regulations. J. Environ. Pathol. Toxicol. Oncol. 2018, 37, 209–230.
- Elsaesser, A.; Howard, C.V. Toxicology of Nanoparticles. Adv. Drug Deliv. Rev. 2012, 64, 129–137.
- Sung, Y.K.; Kim, S.W. Recent Advances in the Development of Gene Delivery Systems. Biomater. Res. 2019, 23, 8.
- Eshka, S.F.A.; Bahador, M.; Gordan, M.M.; Karbasi, S.; Tabar, Z.M.; Basiri, M. A Systematic Review of Gene Editing Clinical Trials. medRxiv 2022.
- Kontogiannis, O.; Karalis, V. On the in Vivo Kinetics of Gene Delivery Vectors. medRxiv 2022.
- Nayerossadat, N.; Ali, P.; Maedeh, T. Viral and Nonviral Delivery Systems for Gene Delivery. Adv. Biomed. Res. 2012, 1, 27.
- Wang, D.; Tai, P.W.L.; Gao, G. Adeno-Associated Virus Vector as a Platform for Gene Therapy Delivery. Nat. Rev. Drug Discov. 2019, 18, 358–378.
- Abinaya, R.V.; Viswanathan, P. Biotechnology-Based Therapeutics. In Translational Biotechnology; Elsevier: Amsterdam, The Netherlands, 2021; pp. 27–52.
- Trobridge, G.D. Foamy Virus Vectors for Gene Transfer. Expert. Opin. Biol. Ther. 2009, 9, 1427–1436.
- Deregowski, V.; Canalis, E. Gene Delivery by Retroviruses. In Osteoporosis. Methods in Molecular Biology; Humana Press: Totowa, NJ, USA, 2008; Volume 455.
- Cavalieri, V.; Baiamonte, E.; Lo Iacono, M. Non-Primate Lentiviral Vectors and Their Applications in Gene Therapy for Ocular Disorders. Viruses 2018, 10, 316.
- Worgall, S.; Crystal, R.G. Gene Therapy. In Principles of Tissue Engineerin, 4th ed.; Elsevier Inc.: Amsterdam, The Netherlands, 2013; pp. 657–686. ISBN 9780123983589.
- Wong, L.-F.; Goodhead, L.; Kyriacos, C.P.; Mitrophanous, K.A.; Kingsman, S.M.; Mazarakis, N.D. Lentivirus-Mediated Gene Transfer to the Central Nervous: Therapeutic and Research Applications. Hum. Gene Ther. 2006, 17, 1–9.
- Lee, C.S.; Bishop, E.S.; Zhang, R.; Yu, X.; Farina, E.M.; Yan, S.; Zhao, C.; Zeng, Z.; Shu, Y.; Wu, X.; et al. Adenovirus-Mediated Gene Delivery: Potential Applications for Gene and Cell-Based Therapies in the New Era of Personalized Medicine. Genes. Dis. 2017, 4, 43–63.
- Kasala, D.; Yoon, A.R.; Hong, J.; Kim, S.W.; Yun, C.O. Evolving Lessons on Nanomaterial-Coated Viral Vectors for Local and Systemic Gene Therapy. Nanomedicine 2016, 11, 1689–1713.
- Ahmadi, S.E.; Soleymani, M.; Shahriyary, F.; Amirzargar, M.R.; Ofoghi, M.; Fattahi, M.D.; Safa, M. Viral Vectors and Extracellular Vesicles: Innate Delivery Systems Utilized in CRISPR/Cas-Mediated Cancer Therapy. Cancer Gene Ther. 2023, 30, 936–954.
- Zhang, H.; Wang, H.; An, Y.; Chen, Z. Construction and Application of Adenoviral Vectors. Mol. Ther. Nucleic Acids 2023, 34, 102027.
- Vargas, J.E.; Chicaybam, L.; Stein, R.T.; Tanuri, A.; Delgado-Cañedo, A.; Bonamino, M.H. Retroviral Vectors and Transposons for Stable Gene Therapy: Advances, Current Challenges and Perspectives. J. Transl. Med. 2016, 14, 288.
- Capasso, C.; Garofalo, M.; Hirvinen, M.; Cerullo, V. The Evolution of Adenoviral Vectors through Genetic and Chemical Surface Modifications. Viruses 2014, 6, 832–855.
- Vandendriessche, T.; Naldini, L.; Collen, D.; Chuah, M.K.L. Oncoretroviral and Lentiviral Vector-Mediated Gene Therapy. Methods Enzym. 2002, 346, 573–589.
- Cevher, E.; Demir, A.; Sefik, E. Gene Delivery Systems: Recent Progress in Viral and Non-Viral Therapy. In Recent Advances in Novel Drug Carrier Systems; InTech: London, UK, 2012.
- Travieso, T.; Li, J.; Mahesh, S.; Mello, J.D.F.R.E.; Blasi, M. The Use of Viral Vectors in Vaccine Development. NPJ Vaccines 2022, 7, 75.
- Minnaert, A.K.; Vanluchene, H.; Verbeke, R.; Lentacker, I.; De Smedt, S.C.; Raemdonck, K.; Sanders, N.N.; Remaut, K. Strategies for Controlling the Innate Immune Activity of Conventional and Self-Amplifying MRNA Therapeutics: Getting the Message Across. Adv. Drug Deliv. Rev. 2021, 176, 113900.
- Maruggi, G.; Zhang, C.; Li, J.; Ulmer, J.B.; Yu, D. MRNA as a Transformative Technology for Vaccine Development to Control Infectious Diseases. Mol. Ther. 2019, 27, 757–772.
- Ballesteros-Briones, M.C.; Silva-Pilipich, N.; Herrador-Cañete, G.; Vanrell, L.; Smerdou, C. A New Generation of Vaccines Based on Alphavirus Self-Amplifying RNA. Curr. Opin. Virol. 2020, 44, 145–153.
- Blom, D.J.; Marais, A.D.; Moodley, R.; van der Merwe, N.; van Tonder, A.; Raal, F.J. RNA-Based Therapy in the Management of Lipid Disorders: A Review. Lipids Health Dis. 2022, 21, 41.
- Magadum, A.; Kaur, K.; Zangi, L. MRNA-Based Protein Replacement Therapy for the Heart. Mol. Ther. 2019, 27, 785–793.
- Erasmus, J.H.; Khandhar, A.P.; O’Connor, M.A.; Walls, A.C.; Hemann, E.A.; Murapa, P.; Archer, J.; Leventhal, S.; Fuller, J.T.; Lewis, T.B.; et al. An Alphavirus-Derived Replicon RNA Vaccine Induces SARS-CoV-2 Neutralizing Antibody and T Cell Responses in Mice and Nonhuman Primates. Sci. Transl. Med. 2020, 12, eabc9396.
- McCullough, K.C.; Bassi, I.; Milona, P.; Suter, R.; Thomann-Harwood, L.; Englezou, P.; Démoulins, T.; Ruggli, N. Self-Replicating Replicon-Rna Delivery to Dendritic Cells by Chitosan-Nanoparticles for Translation in Vitro and in Vivo. Mol. Ther. Nucleic Acids 2014, 3, e173.
- Blakney, A.K.; McKay, P.F.; Yus, B.I.; Aldon, Y.; Shattock, R.J. Inside out: Optimization of Lipid Nanoparticle Formulations for Exterior Complexation and in Vivo Delivery of SaRNA. Gene Ther. 2019, 26, 363–372.
- Feng, X.; Xu, W.; Li, Z.; Song, W.; Ding, J.; Chen, X. Immunomodulatory Nanosystems. Adv. Sci. 2019, 6, 1900101.
- Machado, B.A.S.; Hodel, K.V.S.; Fonseca, L.M.D.S.; Mascarenhas, L.A.B.; Andrade, L.P.C.d.S.; Rocha, V.P.C.; Soares, M.B.P.; Berglund, P.; Duthie, M.S.; Reed, S.G.; et al. The Importance of Rna-Based Vaccines in the Fight against COVID-19: An Overview. Vaccines 2021, 9, 1345.
- Wadhwa, A.; Aljabbari, A.; Lokras, A.; Foged, C.; Thakur, A. Opportunities and Challenges in the Delivery of Mrna-Based Vaccines. Pharmaceutics 2020, 12, 102.
- Cullis, P.R.; Hope, M.J. Lipid Nanoparticle Systems for Enabling Gene Therapies. Mol. Ther. 2017, 25, 1467–1475.
- Kowalski, P.S.; Rudra, A.; Miao, L.; Anderson, D.G. Delivering the Messenger: Advances in Technologies for Therapeutic MRNA Delivery. Mol. Ther. 2019, 27, 710–728.
- Garcia, A.B.; Siu, E.; Sun, T.; Exler, V.; Brito, L.; Hekele, A.; Otten, G.; Augustijn, K.; Janse, C.J.; Ulmer, J.B.; et al. Neutralization of the Plasmodium-Encoded MIF Ortholog Confers Protective Immunity against Malaria Infection. Nat. Commun. 2018, 9, 2714.
- Erasmus, J.H.; Archer, J.; Fuerte-Stone, J.; Khandhar, A.P.; Voigt, E.; Granger, B.; Bombardi, R.G.; Govero, J.; Tan, Q.; Durnell, L.A.; et al. Intramuscular Delivery of Replicon RNA Encoding ZIKV-117 Human Monoclonal Antibody Protects against Zika Virus Infection. Mol. Ther. Methods Clin. Dev. 2020, 18, 402–414.
- Leventhal, S.S.; Meade-White, K.; Rao, D.; Haddock, E.; Leung, J.; Scott, D.; Archer, J.; Randall, S.; Erasmus, J.H.; Feldmann, H.; et al. Replicating RNA Vaccination Elicits an Unexpected Immune Response That Efficiently Protects Mice against Lethal Crimean-Congo Hemorrhagic Fever Virus Challenge. Lancet 2022, 82, 104188.
- Fotoran, W.L.; da Silva, J.R.; Glitz, C.; Ferreira, L.C.d.S.; Wunderlich, G. Establishment of an Antiplasmodial Vaccine Based on PfRH5-Encoding RNA Replicons Stabilized by Cationic Liposomes. Pharmaceutics 2023, 15, 1223.
- Goswami, R.; O’hagan, D.T.; Adamo, R.; Baudner, B.C. Conjugation of Mannans to Enhance the Potency of Liposome Nanoparticles for the Delivery of Rna Vaccines. Pharmaceutics 2021, 13, 240.
- Chahal, J.S.; Khan, O.F.; Cooper, C.L.; McPartlan, J.S.; Tsosie, J.K.; Tilley, L.D.; Sidik, S.M.; Lourido, S.; Langer, R.; Bavari, S.; et al. Dendrimer-RNA Nanoparticles Generate Protective Immunity against Lethal Ebola, H1N1 Influenza, and Toxoplasma Gondii Challenges with a Single Dose. Proc. Natl. Acad. Sci. USA 2016, 113, E4133–E4142.
- McCullough, K.C.; Milona, P.; Thomann-Harwood, L.; Démoulins, T.; Englezou, P.; Suter, R.; Ruggli, N. Self-Amplifying Replicon RNA Vaccine Delivery to Dendritic Cells by Synthetic Nanoparticles. Vaccines 2014, 2, 735–754.
- Brito, L.A.; Chan, M.; Shaw, C.A.; Hekele, A.; Carsillo, T.; Schaefer, M.; Archer, J.; Seubert, A.; Otten, G.R.; Beard, C.W.; et al. A Cationic Nanoemulsion for the Delivery of Next-Generation RNA Vaccines. Mol. Ther. 2014, 22, 2118–2129.
- Erasmus, J.H.; Khandhar, A.P.; Guderian, J.; Granger, B.; Archer, J.; Archer, M.; Gage, E.; Fuerte-Stone, J.; Larson, E.; Lin, S.; et al. A Nanostructured Lipid Carrier for Delivery of a Replicating Viral RNA Provides Single, Low-Dose Protection against Zika. Mol. Ther. 2018, 26, 2507–2522.
