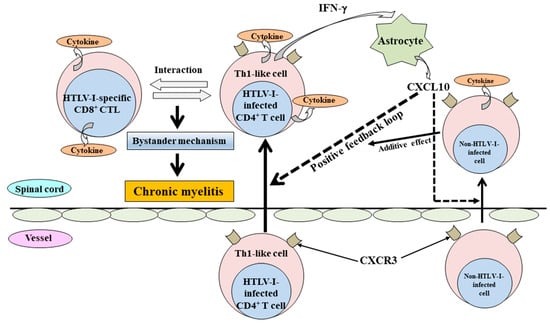
In the process leading to the transmigration of T cells into the tissues, the rolling process of T cells on vascular endothelial cells (ECs) functions as the first step
[23]. Selectin and its ligands, which are expressed on ECs and T cells, respectively, play an important role in this step
[24][25][24,25]. Of these, sialyl Lewis
x antigen (sLe
x) is a ligand for both E- and P-selectin
[26]. Therefore, T cells expressing sLe
x (sLe
x+ cell) might have the potential to transmigrate into tissues. The scholars previously compared the frequency of sLe
x+ cells together with IFN-γ production in peripheral blood CD4
+ T cells between 8 HAM/TSP patients and 14 controls, including four anti-HTLV-1-seropositive carriers
[27]. As shown in the results, the frequency of sLe
x+ cells in peripheral blood CD4
+ T cells of HAM/TSP patients was significantly higher than in controls. In addition, the activity of IFN-γ production in the sLe
x+ cell population in the peripheral blood CD4
+ T cells of HAM/TSP patients had significantly increased compared to controls.
3. The Role of Small GTPase Activation Leading to the Heightened Transmigration Activity of HTLV-1-Infected CD4+ T Cells into Tissues in HAM/TSP Patients
Small GTPases function as the propulsion for the transmigration of the cells through ECs. That is, small GTPase activation can induce the upregulation of transmigration activity of the cells into tissues through the rearrangement of the cytoskeleton involved in the adhesion and migration of cells
[30][42]. The finding that HTLV-1 tax regulates cell adhesion and migration by the interaction with small GTPases, such as Cdc42, Rac, and Rho, was previously demonstrated
[31][43]. A report indicated that Gem, which is one of the small GTP-binding proteins belonging to the Ras superfamily, is involved in the increase of the cellular migration of HTLV-1-infected cells through cytoskeleton remodeling
[32][44].
It previously reported the significantly increased adherence to ECs and subsequent transmigration through ECs of activated CD4
+ T cells with heightened LFA-1 expression in the peripheral blood T cells of HAM/TSP patients as mentioned above
[33][34][30,31], suggesting the upregulation of signaling based on integrin/ligand interaction in the peripheral blood CD4
+ T cells of HAM/TSP patients. Subsequently, the upregulation of integrin/ligand signaling induces the activation of small GTPases, which are the downstream targets, followed by the rearrangement of cytoskeletal components
[35][36][45,46]. Therefore, small GTPases might be activated in the HTLV-1-infected cells of HAM/TSP patients. To confirm this, scholars analyzed the activity of small GTPases, such as Cdc42, Rac, and Rho, in HTLV-1-infected T cell lines derived from HAM/TSP patients in comparison with those in HTLV-1-infected T cell lines derived from other origins
[37][47]. As a result, it was revealed that all small GTPases were strongly activated in all cell lines derived from HAM/TSP patients. Of these small GTPases, the difference in the degree of activation between both kinds of cell lines was the most obvious in Cdc42. Cdc42 plays an important role in the polarization of the cytoskeleton following integrin-mediated activation
[38][48] with the involvement in cell migration
[39][40][49,50]. Therefore, the activation of Cdc42 in the HTLV-1-infected cells of HAM/TSP patients suggests that these cells have upregulated transmigrating activity into the tissues. Thus, activation of the outside-in signaling from integrin signaling in HTLV-1-infected cells of HAM/TSP patients suggests that this activity functions as one of the first triggers in the development of HAM/TSP.
4. The Mediators Involved in the Heightened Tissue Transmigration of HTLV-1-Infected CD4+ T Cells in HAM/TSP Patients
When considering the transmigration of T cells into the tissues after passing through the endothelium barrier, the extracellular matrix, including the vascular basement membrane, functions as the next barrier. Although collagens, gelatine, fibronectin, and laminin are the main components of the vascular basement membrane, matrix metalloproteinases (MMPs), such as MMP-2 and MMP-9, can cleave these components followed by the disruption of the basement membrane of the endothelium
[41][55]. Indeed, the immunopathological analysis of spinal cord lesions in HAM/TSP patients revealed that MMP-2 and MMP-9 are expressed in infiltrating mononuclear cells with disruption of the vascular endothelium in chronic active lesions with the findings that higher levels of MMP-2 and/or MMP-9 were detected in the CSF of HAM/TSP patients
[42][43][56,57]. In addition, the importance of MMPs in the tissue transmigration of T cells by the degradation of the extracellular matrix is also supported by the finding that the transmigration of CD4
+ T cells of HAM/TSP patients was significantly inhibited by selective MMP inhibitor
[44][58].
Recent proteomic analysis of CSF revealed an increased level of soluble VCAM-1 (sVCAM-1) in HAM/TSP patients
[45][46][60,61]. It is reported that the production of MMPs under the inflammatory status induces the shedding of sVCAM-1 from the surface of ECs
[47][48][62,63]. Therefore, the up-regulated expression of MMPs in CSF, as mentioned above, might account for the increase of sVCAM-1 in CSF of HAM/TSP patients.
5. The Polysulfate Treatment for HAM/TSP Patients Focusing on the Inhibition of the Transmigration of HTLV-1-Infected Cells into the Spinal Cord
The ideal treatment for HAM/TSP patients is the complete elimination of HTLV-1-infected cells. However, the therapeutic strategy against HAM/TSP is yet to be established. Therefore, a regimen with an inhibitory activity against the transmigration of HTLV-1-infected cells as the first responder into the spinal cord might be recommended as one of the therapeutic strategies. The main regions in which pathological changes occur in HAM/TSP are in the lower thoracic spinal cord
[11]. These regions are anatomical watershed zones
[19][20][19,20], where lymphocytes stagnate because of the decreased blood flow, can easily transmigrate to the tissues and evoke immune reactions. Therefore, manipulation of the microcirculation and interaction between lymphocyte and vascular ECs might be one of the therapeutic strategies against HAM/TSP.
Pentosan polysulfate sodium (PPS), which was developed as a heparin-like agent and has been used in Europe for thrombosis prophylaxis and treatment of phlebitis, is a semisynthetic drug manufactured from European beech-wood hemicellulose by sulfate esterification
[49][79]. Therefore, PPS is safe and has also been approved by the US Food and Drug Administration as an oral medication for treating interstitial cystitis. In addition to the activity of improving microcirculation, polysulfates, such as heparin and PPS, have the potential to inhibit the intercellular spread of HTLV-1 by blocking the binding of the virus to heparan sulfate proteoglycans
[50][51][80,81]. Indeed, the multiple activities of PPS experimentally verified included (i) the inhibition of the adhesion to and transmigration of HTLV-1-infected cells through ECs; (ii) inhibition of HTLV-1 cell to cell transmission; (iii) suppression of HTLV-1 production; and (iv) blockage of interaction of HTLV-1 infection and ECs with the inhibition of subsequent induction of inflammatory cytokines
[52][82].
6. Conclusions and Perspectives
Considering the mechanism of chronic inflammation induced in the spinal cord of HAM/TSP patients, HTLV-1-infected CD4
+ T cells might play a crucial role as the first responder. Therefore, the activities of HTLV-1-infected CD4
+ T cells in HAM/TSP patients were evaluated based on the transmigration activity into the tissues. Consequently, it was demonstrated that HTLV-1-infected CD4
+ T cells in HAM/TSP were supposed to have enough heightened transmigrating activity into the tissues based on the activation of integrin signaling followed by small GTPase activation with the up-regulated expression of MMPs. This activity appears sufficient to allow HTLV-1-infected CD4
+ T cells to function as the first responders in the development of HAM/TSP. In addition, the HTLV-1-infected CD4
+ T cells in HAM/TSP patients might also have the potential to induce the trigger for the development of another systemic inflammatory status, including Sjögren’s syndrome, myositis, and uveitis, etc., which occasionally occur in conjunction with HAM/TSP, as the first responder.
Although the exact reasons why HTLV-1 induces HAM/TSP in a very small population of HTLV-1-infected individuals are still unsolved, a very important task in future HAM/TSP research is to clarify the molecular mechanisms leading to the establishment of HTLV-1-infected CD4
+ T cells as the first responder in HAM/TSP patients. At this point, the acquisition of heightened transmigrating activity of HTLV-1-infected CD4
+ T cells into the tissues among HTLV-1-infected individuals seems to be the key event leading to the development of HAM/TSP.