Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is a comparison between Version 1 by Soejima Hidenobu and Version 2 by Rita Xu.
Placental mesenchymal dysplasia (PMD) is a morphological abnormality resembling partial hydatidiform moles without abnormal trophoblastic proliferation. In PMD, approximately 20% of fetuses have Beckwith–Wiedemann syndrome (BWS), and approximately 20% of BWS fetuses are associated with PMD. In addition, PMD is a cardinal feature of BWS, and paternal uniparental diploidy/biparental diploidy mosaicism (also called androgenetic/biparental mosaicism) has been found in both BWS and PMD.
- placental mesenchymal dysplasia
- genomic imprinting
- androgenetic/biparental mosaicism (paternal uniparental diploidy/biparental diploidy mosaicism)
1. Introduction
Placental mesenchymal dysplasia (PMD) was first reported by Moscoso [1] as diffuse mesenchymal hyperplasia of the placental stem villi, leading to increased placental volume (placentomegaly) and elevated levels of alpha fetoprotein (AFP). It is now known to be characterized by varying levels of placentomegaly, aneurysmally dilated chorionic plate vessels, thrombosis of the dilated vessels, and large grapelike vesicles within the placenta [2]. Since these features may mimic a molar pregnancy on ultrasound, it is often mistaken for partial hydatidiform mole (PHM) or complete hydatidiform mole (CHM) with a coexisting normal fetus [3]. Unlike molar pregnancies, PMD usually features a normal fetus and the pregnancy often extends into the third trimester [4]. However, PMD pregnancies are high-risk because they carry fixed probabilities of several complications. These include fetal growth restriction (FGR); preterm delivery; fetal demise; preeclampsia; eclampsia; hemolysis, elevated liver enzymes, and low platelets (HELLP) syndrome; and hypertensive disorders of pregnancy (HDP) [2][3][5][6][2,3,5,6]. In addition, approximately 20% of fetuses in PMD pregnancies have Beckwith–Wiedemann syndrome (BWS) [4]. Since androgenetic/biparental mosaicism (ABM) and androgenetic/biparental chimera (ABC) have been found in PMD specimens, the presence of androgenetic cells resulting in abnormal genomic imprinting has been suggested as a cause of PMD [7][8][9][10][7,8,9,10].
BWS (OMIM #130650) was originally reported by Beckwith and Wiedemann [11][12][11,12] as a syndrome involving exomphalos, macroglossia, and gigantism. It is now known to be an imprinting disorder with complex and diverse phenotypes. Macroglossia, exomphalos, and lateralized overgrowth are the cardinal features, and there is also an increased risk of developing embryonal tumors such as Wilms tumor, hepatoblastoma, neuroblastoma, rhabdomyosarcoma, adrenocortical carcinoma, or phaeochromocytoma [13][14][13,14]. Because of the range of phenotypes, it is recommended that the Beckwith–Wiedemann spectrum (BWSp) is used and that diagnoses are made based on a scoring system. This system assigns two points to each cardinal feature and one point to each suggestive feature. Patients with a total score of ≥4 are diagnosed as classical BWS, irrespective of their molecular test results, as are patients with a score of ≥2 with positive genetic test results [13]. Placentomegaly and PMD are included as the suggestive or cardinal feature, respectively, in the BWSp scoring system [13]. There are five major causative alterations: loss of methylation of imprinting control region 2 (KCNQ1OT1:TSS-differentially methylated region (DMR)) (ICR2-LOM), gain of methylation at ICR1 (H19/IGF2:IG-DMR) (ICR1-GOM), paternal uniparental disomy of 11 (pUPD11), loss-of-function variants of the CDKN1C gene, and paternal duplication of 11p15 [13]. The genetic testing aims to detect these major alterations. Several minor alterations have also been discovered thus far: genetic variants within ICR1, paternal uniparental diploidy/biparental diploidy mosaicism (PUDM, also called ABM), and genetic variants of the KCNQ1 gene [15][16][17][18][19][15,16,17,18,19].
2. Incidence and Pathology of PMD
2.1. Incidence
In 2001, Paradinas et al. reported the incidence of PMD as 0.2% (15 out of 7560 placentas examined) [20][21]. The following year, Arizawa et al. reported an incidence of only 0.02% (7/30,758) [21][22], and in 2012, Zeng et al. reported an incidence of 0.002% (2/95,265) [22][23]. Although the intermediate figure (0.02%) is widely used in the literature, calculation of the true incidence may be difficult, since only a small fraction of placentas are subjected to pathologic examination [3]. In any case, PMD is certainly a rare placental condition, and so far only just over 100 cases have been reported [3][23][3,24]. More than 80% of the fetuses from PMD pregnancies identified thus far have been female with the normal karyotype (46,XX) [3][4][6][3,4,6]. However, a karyotype of 46,XX/46,XY has been observed in some fetuses. Cohen et al. reported a normal karyotype in 32 of 36 cases (89%) and an abnormal karyotype in the remaining four (11%) [24][20]. The abnormal karyotypes in that study included trisomy 13, 47,XXY (Klinefelter syndrome), and 69,XXX (triploidy), and these karyotypes were confirmed in the placental specimens. In addition, 13q12.11 deletion in a neonate and another case of trisomy 13 in a fetus have been reported, but these were not confirmed in PMD specimens [25][26][25,26].2.2. Pathology
Macroscopically, PMD is usually characterized by placentomegaly, meaning that the weight of the placenta is greater than the 95th percentile of placenta weights [27], and is often associated with dilatation and congestion of the vessels in the chorionic plate. In some cases, grape-like cysts formed by dilatation of the hydropic stem villi are present (Figure 1A) [5]. Most placentas with PMD have two distinct areas: one with a macroscopically normal appearance and one exhibiting macroscopic PMD characteristics (a cystic lesion) (Figure 1A) [3][28][3,28]. In a small proportion of cases the macroscopic PMD lesion occupies the entire placenta.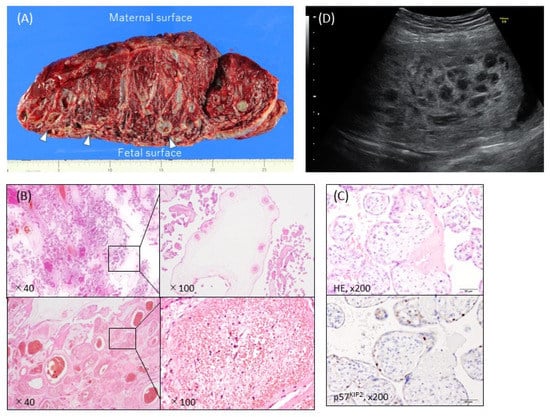
Figure 1. Typical ultrasonographic and macroscopic views and histopathological findings of placental mesenchymal dysplasia (PMD). (A) Macroscopic view of the incised plane. The placental weight was 1530 g at 38 weeks and 0 days of pregnancy. There were heterogeneous areas, with numerous cysts containing gelatinous liquid (arrows) and normal red-brown or spongy villous tissue. The cystic areas were predominantly on the fetal placental surface. (B) Hematoxylin-eosin stain. The PMD featured enlarged edematous stem villi with cisterns. Dilated, thick-walled, and thrombosed blood vessels with fibromuscular hyperplasia were also apparent. No trophoblastic proliferation was observed. (C) Immunohistochemistry against p57KIP2, which was not expressed in the stroma cells of dysplastic villi in the PMD placenta. (D) Ultrasonography revealed a thickened chorionic plate with a multicystic lesion and the living fetus (19 weeks and 2 days of pregnancy).
