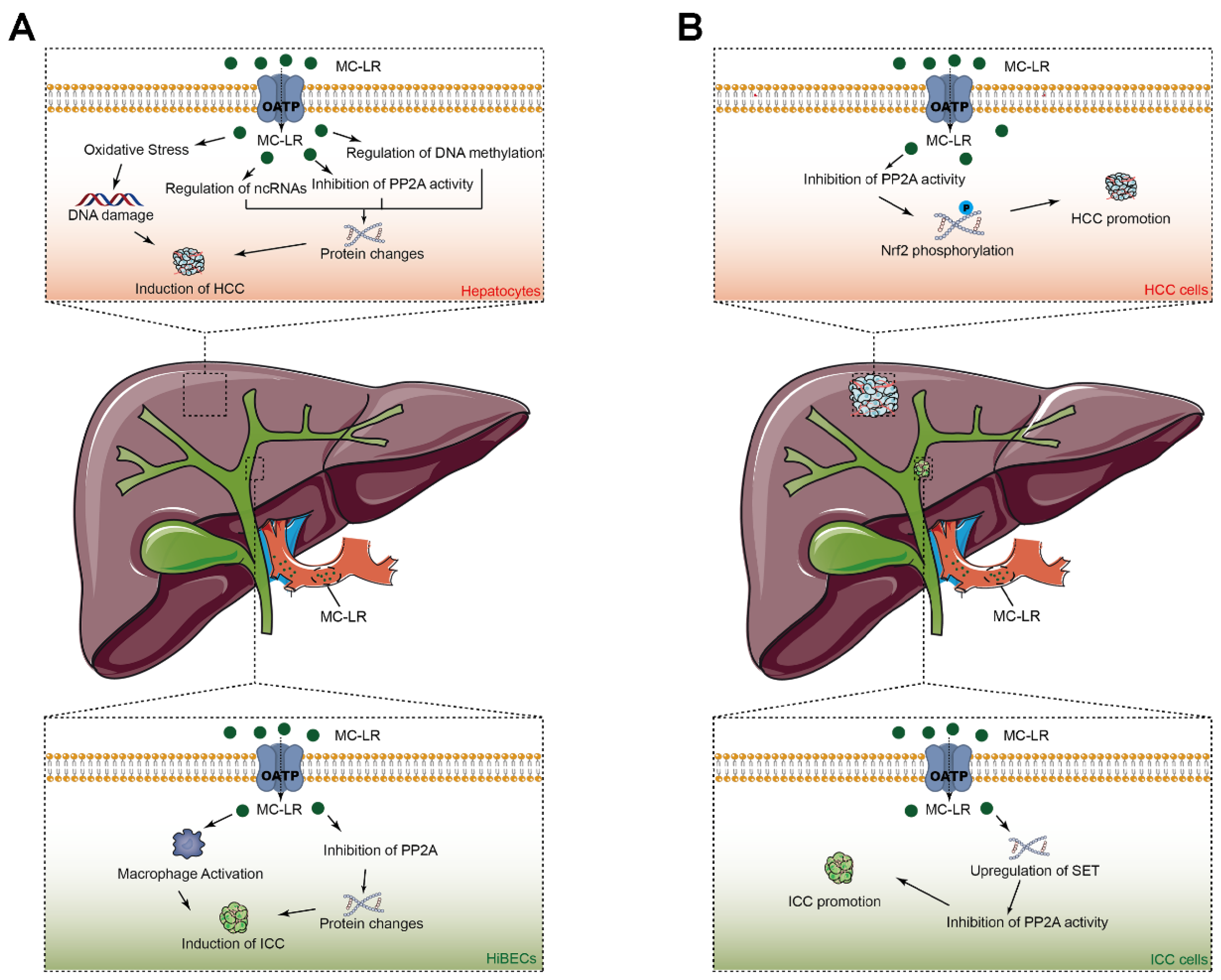
Among all of the variants of MCs, MC-LR has been widely studied due to its severe hepatotoxicity. Since 1992, various studies have discovered the important role of MC-LR in the origin and progression of primary liver cancers (PLCs), while few reviews have focused on it. Based on the available literature, the mechanisms of how MC-LR induces or promotes PLCs are elucidated in this review. This review aims to enhance our understanding of the role that MC-LR plays in PCLs and provides a rational approach for future applications.
- microcystin-LR
- primary liver cancers
- tumor origin
1. Introduction
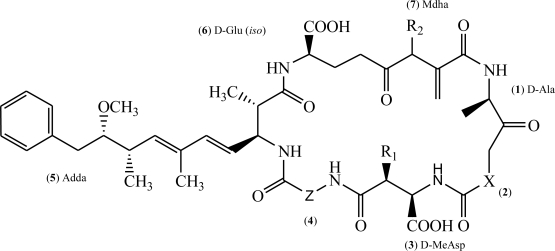
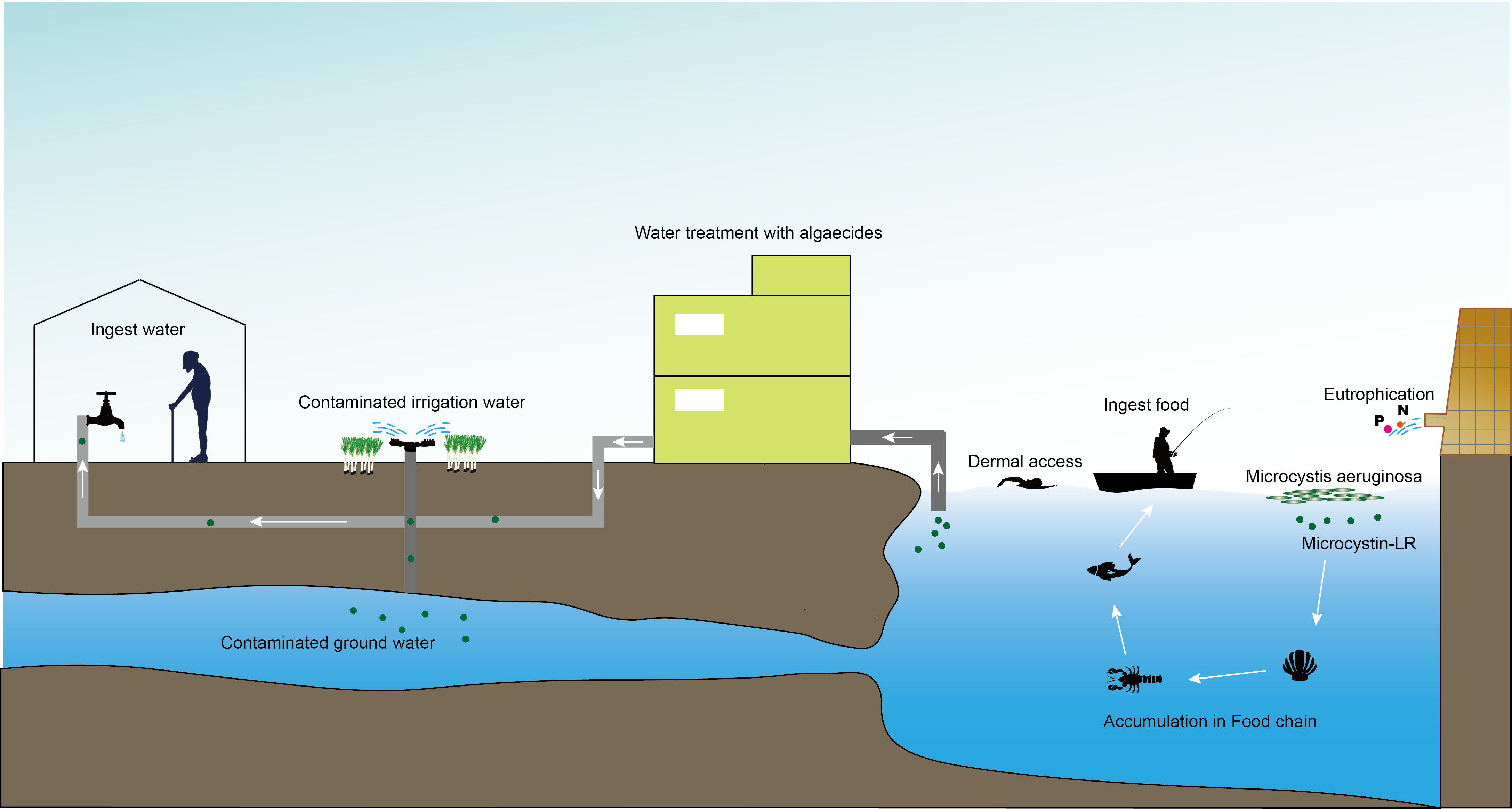
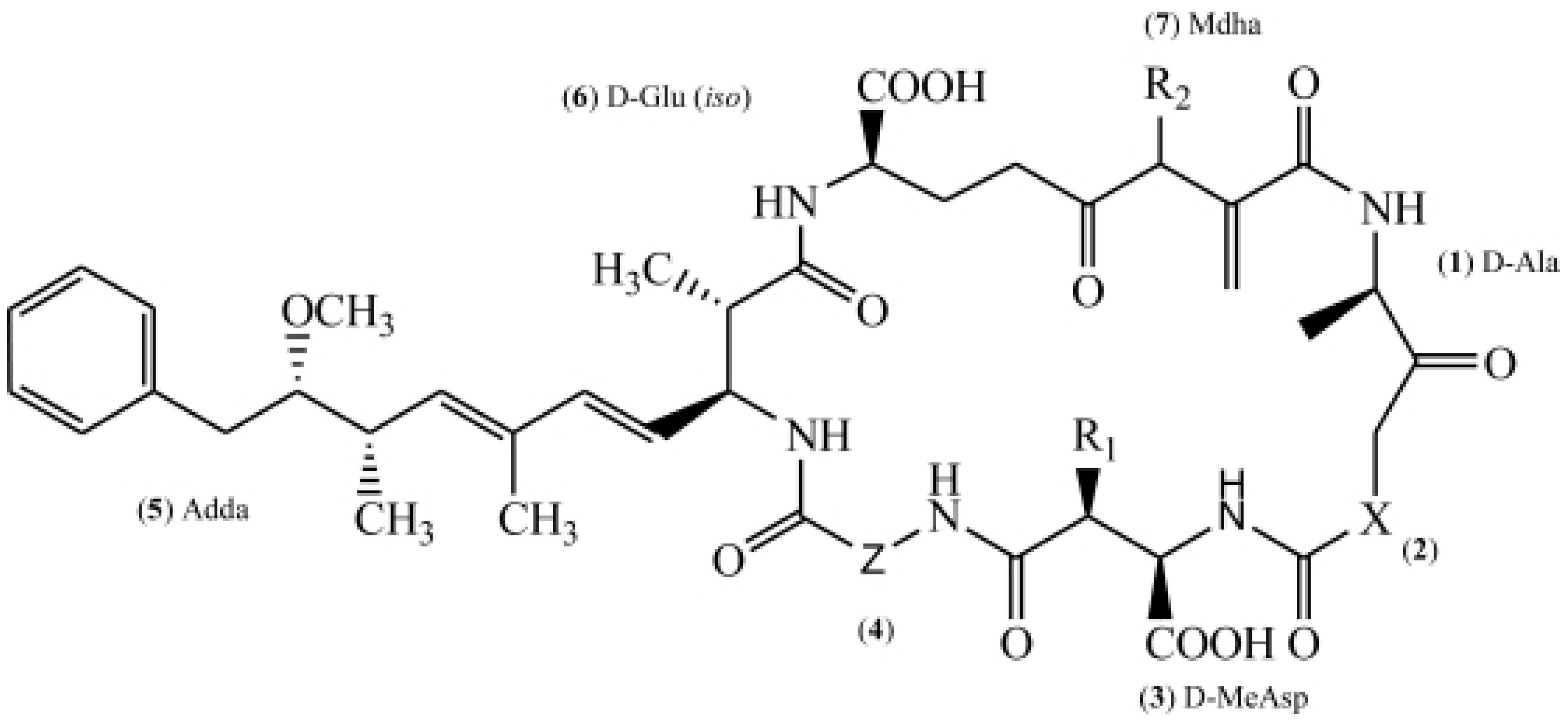
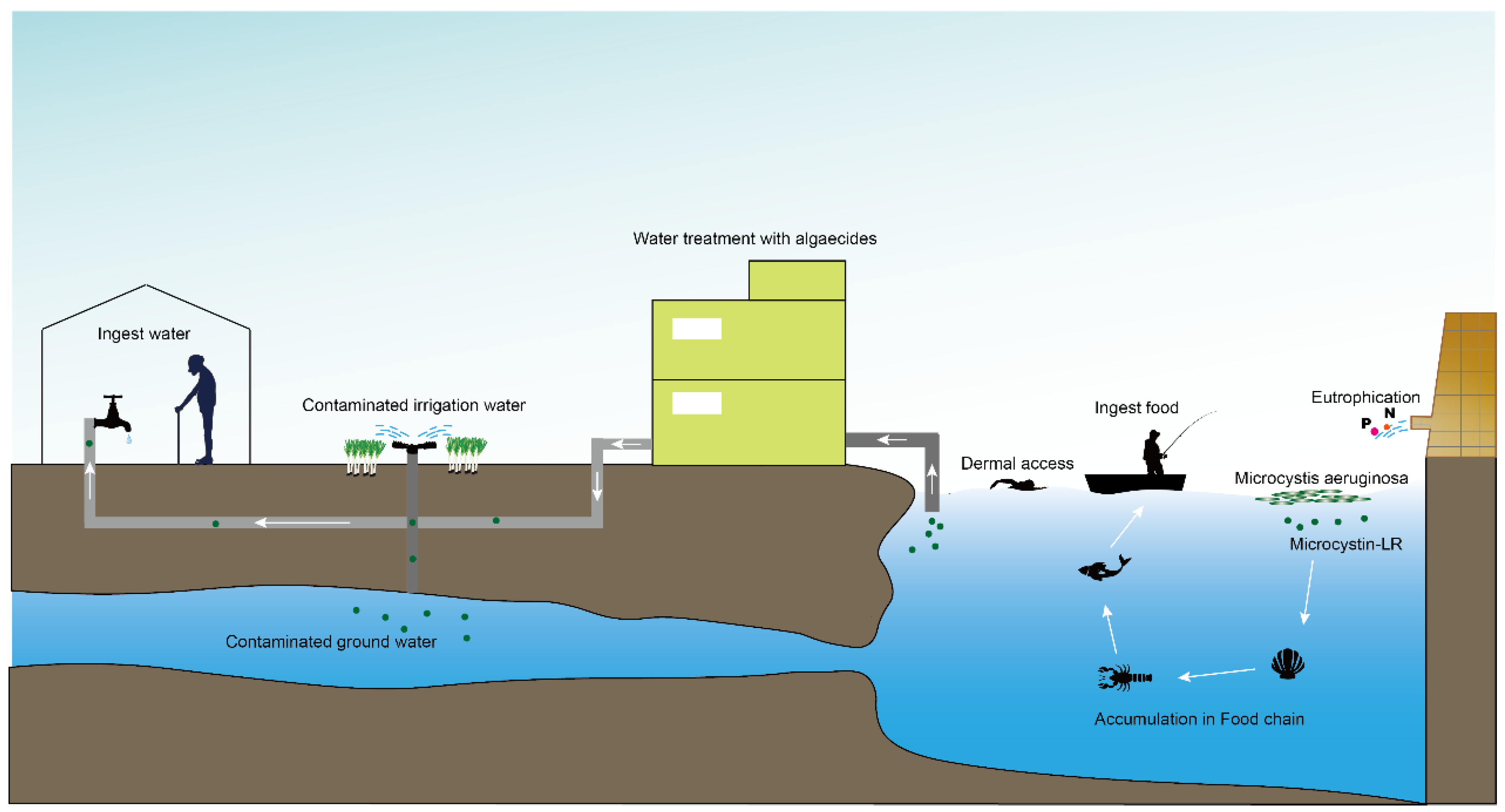
Contamination with harmful cyanobacterial blooms has become a serious environmental issue around the world. Cyantoxins are essentially endotoxins that are released in water following cellular lysing or treatment with algaecides. All major orders of Cyanobacteria can produce a family of hepatotoxins called microcystins (MCs), which are the most frequently encountered cyanotoxins in fresh water. More than 279 congeners of MCs have been identified with molecular weights in the range of 882–1101 Da. MC-LR – MCs combined with leucine (L) and arginine (R) at positions 2 and 4 (Figure 1) – is the most studied congener due to its ubiquity and toxicity. The unique cyclic structure of MC-LR protects it from oxidation, heat, and hydrolysis, enhancing its stability in the environment and its resistance to biodegradation. MC-LR can pose a threat to animals and humans through drinking contaminated water or through the food chain (Figure 2).
MC-LR can easily enter cells via organic anion-transporting polypeptides (OATPs) and accumulate in the target organs through blood circulation. As such, MC-LR can damage almost every system in the body, including the digestive system, nervous system, respiratory system, circulatory system, dermal system, genital system, etc. In addition, experimental studies have indicated that MC-LR exposure may play an important role in the origin and progression of various cancers. Thus, MC-LR was classified as a Group 2B carcinogen by the International Agency for Research on Cancer in 2010.
Primary liver cancer (PLC) ranks as the sixth most common cancer and the third leading cause of cancer-related death in the world, accounting for more than 800 thousand deaths in 2020. The main types of PLC include hepatocellular carcinoma (HCC), intrahepatic cholangiocarcinoma (ICC), and other rare types. HCC and ICC are both malignant tumors originating from hepatocytes and the biliary epithelium, respectively. The biological behaviors of HCC and ICC are completely different. MC-LR was first reported as a potent liver cancer promoter in 1992, and a range of related studies have been published in last 30 years. However, there are few reviews focusing on the role of MC-LR in PLC. Previous studies mainly focused on the relationship between HCC and MC-LR, while recent research has discussed the role of MC-LR in ICC. For the deeper understanding of the effects of MC-LR in PLCs, data on the function and mechanism of MC-LR in PLC was collected in this paper to review these findings.
2. Microcystin-LR in Hepatocellular Carcinoma
Hepatocellular carcinoma (HCC) is the most common type of primary liver cancer, comprising 75%-85% of cases, with China being one of the most high-risk areas for HCC in the world. Early research reported that microcystin-LR (MC-LR) dose-dependently increased the number of neoplastic foci in rat liver, which was initiated with diethyl nitrosamine. Additionally, more and more research has proven that MC-LR is closely related to the origin and progression of HCC through in vitro and vivo studies.
2.1. MC-LR in the Origin of HCC
Clinical and experimental studies both show that MC-LR plays a significant role in the incidence of HCC. This section summarizes the role of MC-LR in the origin of HCC in experimental and clinical studies. Experimental studies have revealed the effects of MC-LR on hepatocytes and the liver. Clinical and epidemiological studies include research on the association between freshwater/serum MC-LR content and the incidence of HCC.
2.2. MC-LR in the Prognosis of HCC
Though early research from 1992 discovered that MC-LR participated in diethyl-nitrosamine-induced HCC, few studies focused on the poorer prognosis of HCC induced by MC-LR. Gan et al. found that MC-LR could promote liver cancer cell growth via the activation of the nuclear factor erythroid 2-related factor 2 in HCC cell lines (HepG2 and Hep3B Cells). Lei et al. also confirmed the correlation between MC-LR and the prognosis of HCC patients in a clinical study. After the detection of MC-LR in the serum of patients with HCC, multifactorial COX regression analysis was conducted, and the results showed that serum MC-LR ≥ 0.97 ng·mL-1 was related to an increased risk of tumor relapse. Thus, serum MC-LR could worsen prognosis in patients with HCC.
3. Microcystin-LR in Intrahepatic Cholangiocarcinoma
Intrahepatic cholangiocarcinoma (ICC) is a rare, highly aggressive, and often fatal primary epithelial cancer arising from the intrahepatic bile duct. Most ICCs develop in non-cirrhotic livers, and mass-forming ICCs are typically characterized by a hypo-vascularized tumor stroma and prominent desmoplastic, making it different from conventional HCCs. Recently, several investigations have discussed the function of MC-LR in the origin and progression of ICCs, and these results are discussed below.
3.1. MC-LR in the Origin of ICC
In the past few years, the special effects of MC-LR on ICC have been demonstrated, and all these results have indicated that MC-LR might participate in the onset of ICC. Yan et al. conducted a study to investigate the toxic effects of MC-LR on intrahepatic biliary epithelial cells in vivo and in vitro. After chronic exposure, MC-LR-treated mice exhibited an obviously thickened bile duct morphology and bile duct hyperplasia. MC-LR can activate the ERK-RSK signaling in human primary intrahepatic biliary epithelial cells (HiBECs) and promote cell proliferation via inhibiting PP2A activity.
In addition to the direct effects on HiBECs induced by MC-LR, Yan et al. also focused on the interaction between HiBECs and surrounding cells after exposure to MC-LR in vivo and in vitro studies. A growing number of macrophages were evaluated as being in the portal area after exposure to MC-LR. To explore the molecular mechanism involved in this progression, a co-culture system including THP-1 cells and HiBECs was implemented in the presence of MC-LR. During exposure to MC-LR, the HiBECs had a giant chemotactic effect on THP-1 cells and induced M2-type polarization. In turn, inflammatory factors in the medium of polarized THP-1 cells can induce the abnormal proliferation and migration of HiBECs via the activation of related pathways in HiBECs. These results indicate that the interaction between HiBECs and the surrounding macrophages after exposure to MC-LR might promote the formation of ICC in humans.
3.2. MC-LR in the Prognosis of ICC
The prognosis for ICC remains dismal despite the development of advanced therapeutic tools. Previous studies have confirmed that the desmoplastic reaction in ICC plays an active and crucial role in promoting progressive and invasive ICC growth and metastasis. Gu et al. conducted a retrospective study to evaluate the prognostic value of MC-LR in ICC after resection, and multivariate analysis showed that a high-MC-LR level in tumor issue was the independent prognostic factor for over-survival and recurrence-free survival after hepatectomy. In addition, MC-LR was proven to promote the survival of human ICC cell lines, and SET was identified to play an important role in this progression.
4. Summary
Microcystin-LR (MC-LR) has been shown to participate in the origin and progression of hepatocellular carcinoma (HCC) and intrahepatic cholangiocarcinoma (ICC). MC-LR was found to be able to inhibit the activity of phosphatase 2A (PP2A) activity and to be able to activate the Akt and MAPK signaling pathways, resulting in abnormal cell proliferation in hepatocytes. The inhibition of PP2A in hepatic stellate cells induced by MC-LR was also found to promote liver fibrosis and to result in the development of HCC. MC-LR can induce the accumulation of reactive oxygen species and damage the DNA in hepatocytes, which have been confirmed to be related to the formation of HCC. In addition, MC-LR can regulate expression of the proteins associated with hepatocarcinogenesis by influencing non-coding RNAs, including microRNAs, circular RNAs, long ncRNAs, as well as by influencing DNA methylation. Furthermore, some studies have demonstrated persistent carcinogenic changes and impaired hepatic recovery after MC-LR toxicity in nonalcoholic steatohepatitis-a risk factor for liver cirrhosis and HCC. Moreover, serum MC-LR levels have been confirmed to be involved in the onset and prognosis of HCC. Moreover, we have also proposed for the first time that MC-LR can induce abnormal cell proliferation in human intrahepatic biliary epithelial cells in vivo and in vitro via the direct inhibition of PP2A in biliary epithelial cells and that it has an indirect influence on the surrounding macrophages. Clinical studies have also been conducted to investigate the role of MC-LR in the poor prognosis of ICC patients, and MC-LR was identified as the independent prognostic factor for over-survival and recurrence-free survival.