Merkel cell carcinoma (MCC) is an uncommon type of skin cancer with poor prognosis. It is seen predominantly in old age in sun-exposed body areas. Racial and geographical differences are seen in its occurrence. Viral infection and radiation exposure are the two leading factors implicated in its causation. Small, firm to hard nodule (usually in sun-exposed areas), red with a history of a rapid increase in size is a common personation of the disease. Other body parts such as upper limbs, trunk, and even lower limbs may be also involved. The disease is diagnosed by taking a tissue sample (biopsy) for examination, and other radiological investigations are needed to reach a proper diagnosis with the staging of the disease. There are various treatment options including surgery, radiotherapy, and chemotherapy. Surgery is the primary treatment option though some patients may not be the candidates for operation where other treatment options come into play.
- Merkel cell carcinoma
- polyomavirus
- sentinel lymph node
- UV-radiation
1. Introduction
2. Epidemiology
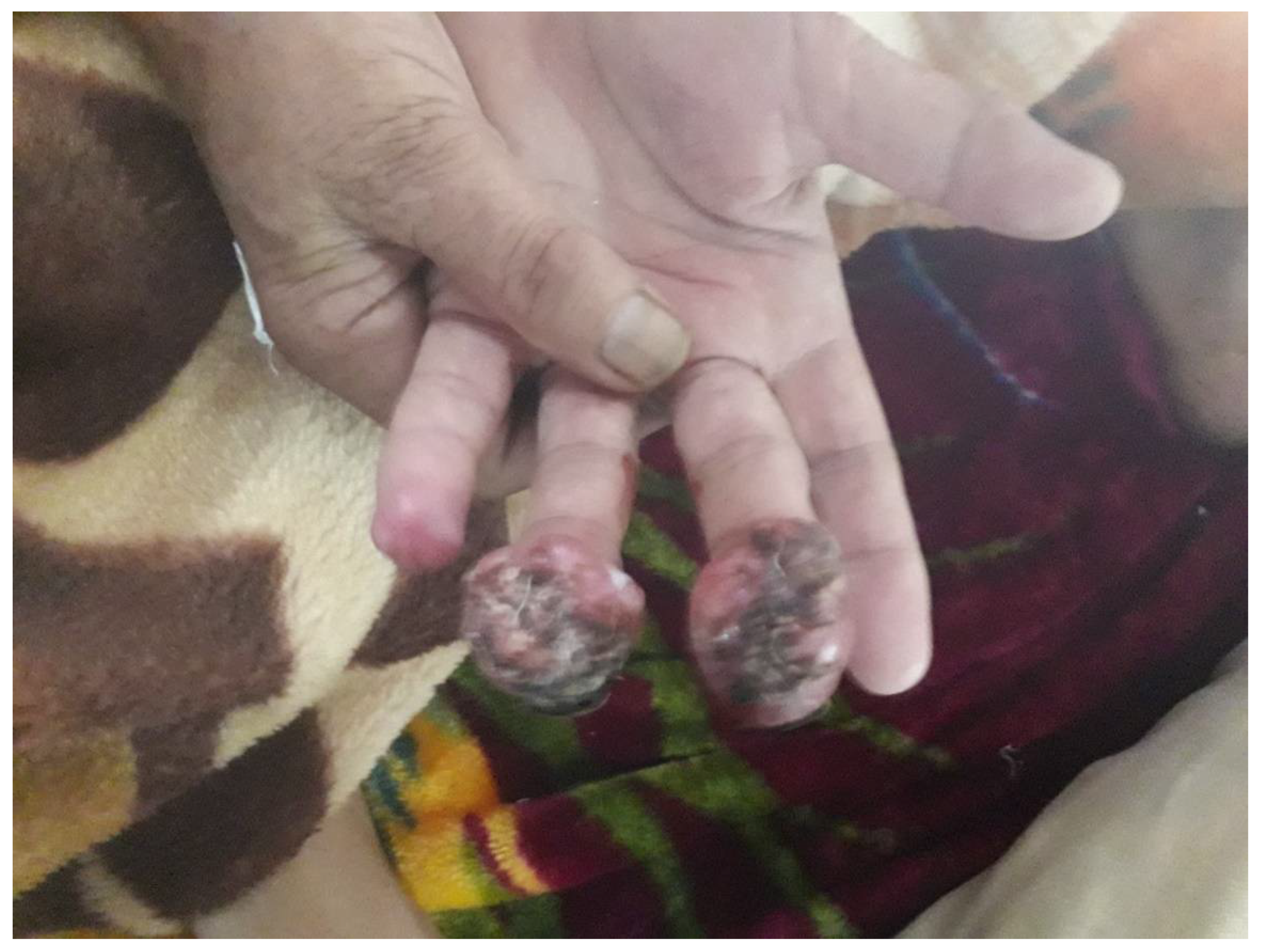
3. Treatment Options
Depending upon the clinical stage, comorbidities, and performance status of the patient, multimodality management protocols consisting of extirpation of the primary lesion, regional lymphadenectomy with radiotherapy/chemotherapy is being employed as the optimal treatment. However, at present, there is debate on the most efficacious treatment scheme for the advanced disease; moreover, it should be distinguished from nodal only MCC, which is thought to be MCC with spontaneous resolution of the cutaneous lesion [9,10,11][9][10][11]. Operative management is the gold standard for localized or locoregional disease. Wide excision with a margin of 1–2 cm (1 cm for <2 cm tumor size and 2 cm for >2 cm ones) is usually recommended [15,20][15][20]. Surgery resulting in positive margins is a candidate for re-excision. In sites where tissue sparing is critical, Mohs microsurgery may be an option, but lack of unanimity precludes its utility. Lymph node dissection followed by radiation is the standard treatment for Stage III disease. SLNB is typically recommended at the time of the primary surgery for the cases without nodes on clinical examination. For those with positive SLNB, elective lymph node dissection (ELND) with radiation is the norm [13,20][13][20]. Radiotherapy (RT) is utilized both as an adjuvant to surgery and as a monotherapy in those in whom surgery is not conducive or suitable, e.g., an elderly patient with a plethora of comorbidities with high risk for anesthesia/surgery. Most frequently, it is employed for the locoregional control of the disease. Most literature suggests that recurrence rates are considerably reduced with adjuvant RT, which has better results than adjuvant chemotherapy [58,59,60,61][23][24][25][26]. The cumulative radiation dosage regimen for the primary site ranges between 50 and 56 Gy for margin negative surgery with dosage enhancement up to 60 Gy for positive histological margins and a maximum of 66 Gy for gross disease (standard fractions ranging from 1.8 to 2 Gy per session) (Table 31) [58][23].| Site | Clinical Scenario | Recommended Dose |
|---|---|---|
| Primary | Surgical resection with wide margins (e.g., 1–2 cm) Small tumor size (<1–2 cm) | Consider observation |
| Surgical resection with negative margins | 50–56 Gy | |
| Surgical resection with histologically positive margins | 56–60 Gy | |
| Surgical resection with gross positive margins |
| Avelumab | Pembrolizumab | Nivolumab | Ipilimumab | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mechanism of action | Anti-PD-L1 | Anti-PD-1 | Anti-PD-1 | Anti-CTLA-4 | ||||||||
| Dose and schedule of administration | 10 mg/kg IV q2 week |
2 mg/kg q3 week |
240 mg IV q2 week |
3 mg/kg IV q3 weeks × 4 doses |
||||||||
| ORR in chemotherapy naïve MCC | 69% ( | n | = 16) | 56% ( | n | = 26) | 71% ( | n | = 14) | 40% ( | n | = 5) |
| 60–66 Gy | ||||||||||||
| No resection performed; as definitive therapy | 60–66 Gy | |||||||||||
| Nodal basin | Node-negative (clinical examination); SLNB negative | Observation | ||||||||||
| Node-negative (clinical examination); SLNB/lymph node dissection not performed | 46–50 Gy | |||||||||||
| Node-negative (clinical examination) SLNB positive, lymph node dissection not performed | 50–56 Gy | |||||||||||
| Lymph node dissection with extracapsular extension; multiple positive Lymph nodes | 50–60 Gy | |||||||||||
| Node positive (clinical examination); SLNB or lymph node dissection not performed | 60–66 Gy |
| ORR in chemotherapy treated/second line MCC | ||||||||
| 33% | ( | n | = 88) | N/A | 63% ( | n | = 8) | |
| The median time of response | 6.1 weeks | 12 weeks | 2 months |
4. Conclusions
References
- Pan, D.; Narayan, D.; Ariyan, S. Merkel cell carcinoma: Five case reports using sentinel lymph node biopsy and a review of 110 new cases. Plast. Reconstr. Surg. 2002, 110, 1259–1265.
- Leech, S.N.; Kolar, A.J.O.; Barrett, P.D.; Sinclair, S.A.; Leonard, N. Merkel cell carcinoma can be distinguished from metastatic small cell carcinoma using antibodies to cytokeratin 20 and thyroid transcription factor 1. J. Clin. Pathol. 2001, 54, 727–729.
- Erovic, I.; Erovic, B.M. Merkel cell carcinoma: The past, the present, and the future. J. Ski. Cancer 2013, 2013, 929364.
- Touzé, A.; Gaitan, J.; Maruani, A.; Le Bidre, E.; Doussinaud, A.; Clavel, C.; Durlach, A.; Aubin, F.; Guyétant, S.; Lorette, G.; et al. Merkel Cell Polyoma virus Strains in Patients with Merkel Cell Carcinoma. Emerg. Infect. Dis. 2009, 15, 960.
- Wang, T.S.; Byrne, P.J.; Jacobs, L.K.; Taube, J.M. Merkel cell carcinoma: Update and review. Semin. Cutan. Med. Surg. 2011, 30, 48–56.
- Patel, P.; Hussain, K. Merkel Cell Carcinoma. Clin. Exp. Dermatol. 2021, 46, 814–819.
- Koljonen, V. Merkel cell carcinoma. World J. Surg. Oncol. 2006, 4, 7.
- Becker, J.C.; Eigentler, T.; Frerich, B.; Gambichler, T.; Grabbe, S.; Höller, U.; Klumpp, B.; Loquai, C.; Krause-Bergmann, A.; Müller-Richter, U.; et al. S2k guidelines for merkel cell carcinoma (MCC, neuroendocrine carcinoma of the skin)—Update 2018. J. Dtsch. Dermatol. Ges. 2019, 17, 562–576.
- Carneiro, C.; Juliano Carlos, S.; Balchiero, J.C.; Neto, B.R.C.; Graziosi, G.B.; de Paiva Dumaresq, F. Merkel cell carcinoma: Clinical presentation, prognostic factors, treatment and survival in 32 patients. Rev. Bras. Cir. Plástica 2013, 28, 196–200.
- Schadendorf, D.; Lebbe, C.; Hausen, A.; Avril, M.-F.; Hariharan, S.; Bharmal, M.; Becker, J.C. Merkel cell carcinoma: Epidemiology, prognosis, therapy, and unmet medical needs. Eur. J. Cancer 2017, 71, 53–69.
- Senchenkov, A.; Steven, M.D.; Moran, L. Merkel cell carcinoma: Diagnosis, management, and outcomes. Plast. Reconstr. Surg. 2013, 131, 771–778.
- Tirumani, S.H.; Shinagare, A.B.; Sakellis, C.; Saboo, S.S.; Jagannathan, J.P.; Krajewski, K.M.; Ramaiya, N.H. Merkel cell carcinoma: A primer for the radiologist. Am. J. Roentgenol. 2013, 200, 1186–1196.
- Coggshall, K.; Tello, T.L.; Jeffrey, P.; North, J.P.; Yu, S.S. Merkel cell carcinoma: An update and review: Pathogenesis, diagnosis, and staging. J. Am. Acad. Dermatol. 2018, 78, 433–442.
- Lebbe, C.; Becker, J.C.; Grob, J.J.; Malvehy, J.; del Marmol, V.; Pehamberger, H.; Peris, K.; Saiag, P.; Middleton, M.R.; Bastholt, L.; et al. Diagnosis and treatment of Merkel Cell Carcinoma. European consensus-based interdisciplinary guideline. Eur. J. Cancer 2015, 51, 2396–2403.
- Merkel Cell Carcinoma. Chapter 30. In AJCC Cancer Staging Manual; Springer: Berlin/Heidelberg, Germany, 2009.
- Bichakjian, C.K.; Lowe, L.; Lao, C.D.; Sandler, H.M.; Bradford, C.R.; Johnson, T.M.; Wong, S.L. Merkel cell carcinoma: Critical review with guidelines for multidisciplinary management. Cancer 2007, 110, 1–12.
- Panqueva, R.D.P.L.; Suarez-Zamora, D.A.; Barrera-Herrera, L.E.; Cadena, M.R. Merkel cell carcinoma and diagnostic experience in a reference hospital: A case series. Case Rep. Med. 2020, 2020, 8391510.
- Ramahi, E.; Choi, J.; Fuller, C.D.; Eng, T.Y. Merkel cell carcinoma. Am. J. Clin. Oncol. 2013, 36, 299–309.
- Becker, J.C. Merkel cell carcinoma. Ann. Oncol. 2010, 21, 81–85.
- Cassler, N.M.; Merrill, E.; Bichakjian, C.K.; Brownell, I. Merkel cell carcinoma therapeutic update. Curr. Treat. Options Oncol. 2016, 17, 36.
- Pulitzer, M. Merkel cell carcinoma. Surg. Pathol. Clin. 2017, 10, 399–408.
- Monteiro, A.; Gouveia, E.; Garcez, D.; Donato, S.; Martins-Branco, D.; Marques, J.; Nunes, H.; Passos, M.J.; Clara, A.I.; Moreira, A. Challenges of new approaches in metastatic merkel cell carcinoma. Case Rep. Oncol. 2020, 13, 501–507.
- Stetsenko, G.Y.; Malekirad, J.; Paulson, K.; Iyer, J.G.; Thibodeau, R.M.; Nagase, K.; Schmidt, M.; Storer, B.E.; Argenyi, Z.B.; Nghiem, P. P63 expression in merkel cell carcinoma predicts poorer survival yet may have limited clinical utility. Am. J. Clin. Pathol. 2013, 140, 838–844.
- Green, M.D.; Hayman, J.A. Radiotherapy in the multidisciplinary management of merkel cell carcinoma. J. Natl. Compr. Cancer Netw. 2018, 16, 776–781.
- Petrelli, F.; Ghidini, A.; Torchio, M.; Prinzi, N.; Trevisan, F.; Dallera, P.; De Stefani, A.; Russo, A.; Vitali, E.; Bruschieri, L.; et al. Adjuvant radiotherapy for merkel cell carcinoma: A systematic review and meta-analysis. Radiother. Oncol. 2019, 134, 211–219.
- Mortier, L.; Mirabel, X.; Fournier, C.; Piette, F.; Lartigau, E. Radiotherapy alone for primary merkel cell carcinoma. Arch. Dermatol. 2003, 139, 1587–1590.
- Ott, M.J.; Tanabe, K.K.; Gadd, M.A.; Stark, P.; Smith, B.L.; Finkelstein, D.M.; Souba, W.W. multimodality management of merkel cell carcinoma. Arch. Surg. 1999, 134, 388–393.
- Servy, A.; Maubec, E.; Sugier, P.; Grange, F.; Mansard, S.; Lesimple, T.; Marinho, E.; Couturaud, B.; Girod, A.; Albert, S.; et al. Merkel cell carcinoma: Value of sentinel lymph-node status and adjuvant radiation therapy. Ann. Oncol. 2016, 27, 914–919.
- American Cancer Society. Cancer.org|1.800.227.2345. Available online: https://www.cancer.org/content/dam/CRC/PDF/Public/8893.00.pdf (accessed on 16 September 2021).
- Stege, H.M.; Bradfisch, F.; Fleischer, M.I.; Mohr, P.; Ugurel, S.; Terheyden, P.; Thiem, A.; Kiecker, F.; Leiter, U.; Becker, J.C.; et al. Retrospective multicentre analysis of the outcome of a re-induction with immune checkpoint inhibitors in advanced merkel cell carcinoma. SN Compr. Clin. Med. 2020, 2, 2202–2207.
- Paulson, K.G.; Bhatia, S. Advances in immunotherapy for metastatic merkel cell carcinoma: A clinician’s guide. J. Natl. Compr. Cancer Netw. 2018, 16, 782–790.
