Zearalenone (ZEA) is an estrogenic fusariotoxin, being classified as a phytoestrogen, or as a mycoestrogen. ZEA and its metabolites are able to bind to estrogen receptors, 17β-estradiol specific receptors, leading to reproductive disorders which include low fertility, abnormal fetal development, reduced litter size and modification at the level of reproductive hormones especially in female pigs. ZEA has also significant effects on immune response with immunostimulatory or immunosuppressive results. This review presents the effects of ZEA and its derivatives on all levels of the immune response such as innate immunity with its principal component inflammatory response as well as the acquired immunity with two components, humoral and cellular immune response. The mechanisms involved by ZEA in triggering its effects are addressed.
- zearalenone
- cell immunity
- humoral immunity
1. Zearalenone
Fusarium
Gibberella species which represent the largest group of mycotoxins (more than 140). Of these the most widespread and also of primary concern are the trichothecenes, fumonisins, and zearalenone [1][2]. Despite the mitigation efforts, exposure of crops to mycotoxins is indeed inevitable and decontamination is very difficult [3][4]. Even though numerous studies concerning the effect of mycotoxins are reported in the specific literature, the contamination of cereals with fusariotoxins, the impact on animal health and the economic losses they imply [5][6][7], the transmission of fusariotoxins into the target organism and the potential existence of toxic components in meat and dairy products remain unknown and need further investigations [8].
Fusarium graminearum, Fusarium cerealis, Fusarium semitectum, Fusarium culmorum and Fusarium equiseti
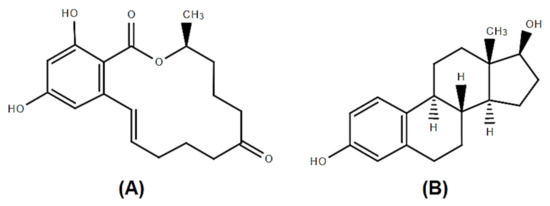
Figure 1.
A
B
After oral contamination, zearalenone is rapidly absorbed in mammals (rabbits, rats, humans and pigs, 80–85%) [16][17]. As mentioned above, structurally, ZEA has a strong similarity with 17 β-estradiol, and is able to bind to estrogen receptors, being also classified as a phytoestrogen, or as a mycoestrogen [18]. From this reason ZEA intoxication most often leads to disorders of the reproductive system. The changes involve low fertility, abnormal fetal development, reduce litter size and modification in the level of specific reproductive hormones: Estradiol and progesterone [19]. But, ZEA manifests its toxicity on many other systems besides the reproductive one. Studies show that the liver and spleen are also affected when exposed to this mycotoxin. It has been demonstrated in an experiment on female piglets that excessive amounts of ZEA raises the key liver enzymes level such as glutathione peroxidase and decreases spleen weight [20]. ZEA exerts significant effects on immune response, the major defense mechanism against pathogens, toxins and other antigens in all mammals with immunostimulatory or immunosuppressive results [21]. The cellular mechanisms activated by zearalenone in triggering its different effects are not yet well understood.
2. Effect of ZEA on Gut Immunity
The gut represents a physical barrier that ensure the body’s protection against environmental agents, mycotoxins included [22]. This barrier involves intestinal epithelial cells (IECs), but also components of both innate and adaptive immunity, as IgA and pro-inflammatory cytokines or molecules involved in the inhibition of bacterial colonization (mucins and antimicrobial peptides) [23].
A recent study of Lahjouji et al. [24] reported that the intestine is a target of ZEA which cause pathological intestinal changes. Depending on different factors as specie, sex, dose or time of exposure, ZEA can affect or not the normal anatomic structure of the intestine. For example, ZEA (40 μg/kg b.w.) did not change the mucosa thickness, the height of villi or the number of goblet cells in swine [25][26], but the ingestion of ZEA (0.3–146 mg/kg feed) in pregnant rats modified the structure of villi and decrease the junction proteins expression [27]. Also, in the first week of a chronic exposure of pigs to ZEA (40 µg/kg b.w.) produced transitory morphological modifications of small intestine and an increase in Paneth cell numbers in the crypt [24].
Exposure to ZEA was associated with the impairment of cell viability, apoptosis and necrosis in different organs including gut [28][29]. For example, recent studies have shown that treatment with ZEA at 10–100 µM for 24h decreased viability of porcine intestinal epithelial cells IPEC-J2 [30] and IPEC-1 [31][32] and increase LDH activity [30]. Apoptosis is one of the main mechanisms involved by ZEA induced toxicity in the gut and it was shown that ZEA can cause apoptosis in various intestinal epithelial cells as IPEC-J2 [33], MODE-K [34] and HCT116 [35]. Sub-chronic exposure of female Polish Large White pigs to low doses of ZEA increased apoptosis and decreased the ileal Peyer’s patches lymphocytes proliferation [36].
Some recent studies have shown that ZEA exposure alters or not the T- and B-cell subtype populations in small intestine. The administration of ZEA (5 or 20 mg/kg b.w.) to female BALB/C mice increased the percentages of CD8+ and decreased the percentages of CD4+ cells in the lamina propria and intra-epithelium lymphocytes, while no effect on CD8+ and CD19+ lymphocytes was observed in the Peyer’ patches [37]. Also, the exposure of prepubertal gilts to 100mg ZEA/kg feed decreased the percentage of CD21+ lymphocytes in pig ileum [36].
Endoplasmic reticulum stress (ERS) pathway seems to be the main signaling pathway involved in ZEA induced apoptosis. In MODE-K mouse cells exposed to zearalenone, the toxin increased the gene expression and protein synthesis of molecules involved in ERS-induced apoptosis pathway as: c-Jun N-terminal kinase, C/EBP homologous protein, GRP78, caspase-1 and the anti-apoptotic protein Bax, while decreasing the levels of the pro-apoptotic related protein Bcl-2 [34]. Similarly, an increased number of apoptotic cells were observed in the Peyer’ patches of the 20 mg/kg ZEA-treated mice associated with a significantly increase of Bax gene expression and of the ratio of Bax:Bcl-2 [37].
Mucosal IgA protects the intestinal epithelium from xenobiotics, viruses and bacteria and maintains also the homeostasis of the intestinal environment [38]. Indeed, previous studies have linked the increase of IgAs to repeated exposure to environmental toxins or to chronic infections [39]. The effect of ZEA on IgAs synthesis is controversial. ZEA administered by oral gavage to female BALB/c mice for two weeks at a dose of 5 or 20 mg/kg b.w. provokes a significantly decrease of the mucosal IgA antibody level in mice duodenum [37]. On the other side, the administration of 20 mg of ZEA/kg b.w. for only one week to male BALB/c mice significantly increased fecal IgA levels in the jejunum (1.5-fold higher that in the control group) [40]. Because the same concentration of ZEA (20 mg/kg b.w.) and the same way of administration (oral gavage) were used in both experiments, the different results could be related to the experiment duration (one week vs. two weeks) or could be influenced by the sex of the animals (male vs. female) and the intestinal segment.
Mucin glycoproteins are produced by epithelial or submucosal mucus-producing cells and represents the principal constituent of mucus [41]. The mucus structure is permanently renewed and could be rapidly adjusted to respond to the changes of the environment, as for example in response to microbial infection or to exposure to contaminants [29]. Recent studies have shown that ZEA (20 mg/kg b.w.) is responsible for intestinal mucosa abnormalities [40] as mice exposure for a short period (one week) to ZEA significantly increased the expression of mucin 1 and mucin 2 genes in the gut. Results on in vitro cell cultures also indicates that ZEA interferes with the mucin synthesis since the toxin increased the concentration of these molecules in Caco-2/HT29-MTX cells [42]. In vitro exposure of swine IPEC-J2 cells to 40 µM ZEA [43], and in vivo exposure of mice to 20 mg ZEA/kg b.w. [40] resulted in the upregulation of β-defensin, an important antimicrobial peptide, with important consequences for the defense against intestinal infection.
IL-1β, TNF-α, IL-6, IL-8, IL-12p40 in IPEC-1 [44] and of
IL-1β
TNF-α in IPEC-J2 cells [43]. The increase in the expression of pro-inflammatory cytokines (IL-1β and TNF-α) was also registered in the in vivo studies, in jejunum of mice intoxicated with 20 mg ZEA/kg b.w. Also, prepubertal gilts exposed to 100 mg ZEA/kg feed for 42 days had elevated ileum concentrations of IL-12/23 40p and IL-1β [36]. By contrast, other researchers found that ZEA had no effect on proinflammatory IL-8 cytokine synthesis by IPEC-1 cells [31] or decreased the gene expression of
IL-1β
TNF-α
IL-8 in the jejunum of rats when administered in different doses (0.3–146.0 mg/kg feed) [27]. As well, a microarray study performed on IPEC-1 cells exposed to ZEA (25 μM) found a decrease of the expression of pro-inflammatory cytokines
IL-8
TNF-α
IL-6
3. Effect of ZEA on Innate Immune Response
Innate or nonspecific immunity is the first form of defense for multicellular organisms. The innate immune response is triggered by receptors that recognize the pathogen and activate a series of signaling pathways that control the immune response [47]. Neutrophils, NK and NKT cells, monocytes/macrophages and dendritic cells that mediate interactions with pathogens are the innate immune system components able to form networks with key role in the initial immune response to infection and tissue damages [48]. They are phagocytic cells that when stimulated can produce reactive oxygen species (ROS), important in cell signaling and homeostasis [49][50]. An imbalance between ROS production and its inefficient elimination drives to a dramatic increase in ROS levels leading to cells damage, known as oxidative stress [49]. Recently, Wang et al., reported that ZEA (5, 10, 20 µM) increased ROS production in bovine neutrophils and decreased antioxidant enzymes (SOD and CAT) activity by involving NADPH, ERK and p38 activation followed by the formation of neutrophil extracellular traps (NETs), a network of DNA extracellular fibbers which help neutrophil cells to kill extracellular pathogens [51]. This could have significant cytotoxic and pro-inflammatory consequences.
Fusarium
In vitro studies highlight an increase or a decline of inflammatory response induced or not by ZEA depending on the immune cell type. Thus, the in vitro study of Marin et al., in which swine PBMCs were exposed to ZEA and its metabolites for 48h showed that ZEA decreased significantly at 5 and 10 µM the TNF-α response of these cells and had no significantly effect on IL-1β and IL-8, while zearalanone decreased also the production of IL-8 at 10 µM [19]. Interleukin 8 (IL-8) is a common inflammatory cytokine important in the recruitment of the immune cells, a key parameter in localized inflammation which induced after that an increase of oxidative stress mediators [60]. The same authors reported later [31] that ZEA derivatives, alpha-zearalenol (α-ZOL), beta-zearalenol (β-ZOL), and zearalanone (ZAN) decreased in a dose dependent manner the IL-8 synthesis in polymorphonuclear cells (PMN), significantly at 10 µM (−49.2% for α-ZOL; −45.6% for β-ZOL and −45.1% for ZAN respectively) after 3 h of exposure. No effect of ZEA on IL-8 concentration registered. Similarly, ZEA metabolites were more potent than ZEA itself in decreasing the IL-8 synthesis in porcine epithelial cells (IPEC-1) [31]. By contrast, Ding e al. [61] found that the level of IL-1β and IL-18 increased significantly in peritoneal mouse macrophages isolated from mice receiving ZEA by gavage (4.5 mg/kg b.w.) once a day for 9 days and treated in vitro with 8 µg/mL for 24h. In a model monocytic cell line, hER + IL-1β-CAT+, the exposure of the cells to low level 50 ng/mL of zearalenone and α-zearalenol resulted in a pro-inflammatory effect as 17β-estradiol by modulating and promoting IL-1β synthesis. The toxins manifested full agonist activity with 17β-estradiol but at lower potency [62] exposure of human placental choriocarcinoma (BeWo) cells to different concentrations of ZEA (2–16µM) increased the IL-6 production [63].
TNF-α, IL-6, IL-8
IL-1β, while in liver the toxin decreased dramatically the expression of these cytokine which might have consequences on immune homeostasis taking into account that liver is considered a key organ for immune homeostasis [64]. It seems that the pro- or anti-inflammatory effect of ZEA depend on the organ involved. The earlier results of Salah-Abbes [65][66] showed a significant reduction of TNF-α, IL-1β and IL-12 in plasma of mice treated with 40 mg ZEA /kg b.w. as well as an increase of the cytokines (TNF-α, IL-6, IL-10) in kidney of mice fed the same concentration of toxin [67]. The inflammatory reaction in kidney is produced through the activation of macrophages which, once activated, will further produce inflammatory cytokines and chemokines subsequently responsible for different reactions and effects such as apoptosis and necrosis, the up- or down regulation of pro- and anti- apoptotic genes [67]. In testicular tissue of mice exposed for 48h to ZEA (40mg/kg b.w.) the toxin increased the level of TNF-α, IL-1β, IL-6 and decreased the level of anti-inflammatory IL-10 cytokine [68].
4. Effect of Zearalenone on Adaptive Immune Response
4.1. Effect of Zearalenone on Humoral Immune Response
Table 1. Literature studies show that ZEA leads to a decrease in serum IgG levels regardless the animal species (mice, rat or swine), toxin concentration or the duration of the exposure. Similarly, most studies have shown that the level of IgM in serum decreases no matter the species (mice or rats), time of exposure (12–36 days) and mycotoxin concentration (5–30 mg/kg b.w.). However, sub-chronic exposure (3–4 weeks) of rats to lower concentrations of ZEA (2–4 mg/kg b.w.) was associated with an increase in serum IgM concentration [69][70]. It seems that the effect of ZEA on IgM concentration is correlated with the sex of animal, since male piglets exposed to low concentration of toxin (0.8 mg/kg feed) resulted in a decreased in IgM level, while no significant changes were observed in serum IgM concentration of gilts receiving ZEA higher concentrations (1.1–3.2 mg/kg feed). Serum IgA concentration was not affected in mice, rats or swine after the exposure to low and medium concentration of the toxin (0.08–30 mg/kg feed) as resulted from most studies (
Table 1.
| Effect (s) | Species/Cell Type | Dose/Time of ZEA Administration |
References |
|---|
| ↑ IgE, ↓ IgM no changes of IgG and IgA |
BALB/c mice female | 20 mg/kg b.w. |
| [ | ||
| 72 | ] | |
| ↓ Ig A, Ig G |
Table 2.
| Effect (s) | Species/Cell Type | Dose/Time of ZEA Administration | References |
|---|
| ↓ B cells producing IgM to SRBC 1 | 14 days | Wistar rats female[37][38] |
|||||
| 3 mg/kg b.w. | 28 days | [57] | ↓ IgG, IgA ↑ IgM |
Pregnant rats | 100,150 mg/kg feed 7 days |
[70 | |
| BALB/c mice, female | |||||||
| No differences in humoral immune response against SRBC 1 | prepubertal gilts | ] | |||||
| 0.75 mg/kg feed | 21 days | [80][81] | ↓ IgG, IgM, IgE no changes of IgA |
Wistar rats female |
0, 1, 5, 30 mg/kg b.w. 36 days |
40 mg/kg b.w. | |
| ↓ Ab titer to porcine parvovirus | Wistar rats | 5 mg/kg b.w. 36 days |
[72]48h | [71] | |||
| ↓ Ab titer to swine plague | post-weaning female piglets | 1.1–3.2 mg/kg feed 18 days |
[76] | ↓ IgG ↑ Ig M |
83]. These authors reported that ZEA (0.2–1800 ng/mL) produced a reduction of peripheral lymphocytes and this was a consequence of apoptosis and cell death triggered by ZEA at the spleen level knowing that spleen is one of the most important organs for maturing lymphocytes [66][71]. The death of spleen lymphocytes leads to the decrease of the peripheral lymphocytes. Zearalenone metabolites also reduced the lymphocytes proliferation. EFSA Scientific Opinion (2011) [84] cited the work of Forsell [85] in which the proliferation of human lymphocytes stimulated with different mitogens was reduced with 50% by 3.5 μg/mL zearalenone, 6.3 μg/mL α-zearalenol, 36 μg/mL β-zearalenol, 3.8 μg/mL α-zearalanol and 33 μg/mL β-zearalanol. The inhibition of proliferation was not related to the estrogenic potential of ZEA and its derivatives, but to their structure and the presence of a single or double bond. The presence in C-6’ of a keto parent molecule (ZEA) or alpha-hydroxyl substituents (alpha-ZEL and alpha-ZAL) led to a 10-fold higher toxicity [86]. Comparing the in vitro effect of zearalenone and is derivatives α-zearalenol and β-zearalenol with that of trichothecenes on proliferation of human peripheral mononuclear cells (PBMC) [83] observed that only the high concentration of these toxins had significant immunosuppressive effect. Indeed, in vitro investigation of Vlata et al. [87] on freshly human PBMC using increased concentration of zearalenone (0.1, 1, 5, 10, 30 µg/mL) showed that the highest concentration of ZEA (30 µg/mL) inhibited the proliferation of B and T lymphocytes and induced also a necrotic effect. A clear necrotic effect was also found irrespective of cells stimulation. The study of Zhang et al. [88] demonstrated that ZEA at 10–50 μg/mL had a time and dose dependent inhibitory action on mouse thymic epithelial cells proliferation and arrested thymic cells in G2/M phase of cellular cycle. Studies performed on TM3 cells shows that low doses of ZEA increases cell proliferation [89].
Fusarium
CDs (Clusters of Differentiation) are glycoproteins expressed on the surface of the immune cells. T cells are characterized by the expression of CD3, CD4 and CD8 markers [91][92] which are involved in in the transduction of signals from T cell surfaces (CD4 and CD8), while CD3 markers activate both the cytotoxic and helper T cells. As can be seen also in
Table 3, there are conflicting data concerning the effect of ZEA on T cells subpopulations. While, most studies indicate a decrease in CD4+, CD8+ and CD3+ expression under the influence of ZEA, regardless of the animal species, other studies suggest an increase in CD4+ and CD8+ expression. However, any change in the CD4/CD8 ratio may indicate an immune dysfunction [91][92].
Table 3.
| Effect (s) | Species/Cell Type | Dose/Time of ZEA Administration | References |
|---|
| ↓ CD4+, CD8+, CD11c+ in spleen ↓ CD4+, CD8+, F4/80+ and ↑ CD19+ and CD11c+ in the mesenteric lymph nodes ↑TNFα and apoptosis, ↓ IL-6 |
BALB/c mice (female, 7-week-old) |
5,20 mg/kg b.w.2 weeks |
[37][38] | ||||
| ZEA 100 and 150 mg/kg: ↓ viability of splenocytes ↓ T-cell proliferation Induce histopathological damage in spleen ZEA 150mg/kg: ↑ interleukin IL-6, IL-18 and IL-1β ↓ interferon-γ, TNFα and IL-10 in spleen |
Sprague Dawley Pregnant Rats | 50, 100, 150 mg/kg b.w. 7 days |
[70] | ||||
| disrupt the proliferation of CD4+8+ in peripheral blood cells | Polish Landrace x Polish Large White crossbreeds |
0.5 mg/kg 6 weeks |
[93][105] | ||||
| ↓ IL-1 in thymus and spleen ↓ IFN-γ in serum ↓ IL-2, IL-6, IL-10 in thymus ↓ IL-10 and IFN-γ in the spleen |
Wistar rat | 1, 5, 30 mg/kg b.w. 36 days |
[72] | ||||
| No effect on the splenic PFC 2 response to SRBC 1 Delayed hypersensitivity response to keyhole limpet hemocyanin | |||||||
| ↓ CD3+, CD4+, CD8+ | Wistar rats male |
, CD56+ cells | B6C3F1 female mice2 mg/kg b.w./week 3 weeks |
10 mg/kg b.w.[69] | |||
| 2–8 weeks | BALB/c mice | 40 mg/kg b.w. 48h[79] |
[71] | ↓ Ig G no changes of IgA, IgM |
Prepubertal gilts | ||
| ↓ CD4+, CD8+ cells in peripheral blood | 200, 800, 1600 μg/kg feed | 14 days |
BPC and SPC Sheep | 3.07– 14.49 μg/kg feed winter time[73] |
|||
| [ | 94 | ] | [106] | ↓ IgG, IgM no changes of IgA |
|||
| ZEA 40 µM: Inhibit T cell-chemotaxis by CCL19 ↑ CD4+ T cells induced by CCL19 chemotaxis ZEA 20 µM: ↑ CD8+ T cells induced by CCL21 chemotaxis | Piglets male |
↓ expression of chemokine receptor CCR7 and CCR2 | BALB/cmouse splenic lymphocytes0.8 mg/kg feed 4 weeks |
[ | 10, 20, 40 µM 48h74] |
||
| [ | 95 | ] | [107] | ↓ IgG, IgM in serum ↑ IgA in serum |
Kunming mice, female |
||
| ↓ CD3+CD4+ T cells ↑ CD3+CD8 | 30 mg/kg b.w. | 12 days |
[ | 20, 30 mg/kg b.w. 12 days75] |
|||
| + T cells | [ | 96 | ][108] | ↓ IgG in serum no changes on IgA, IgM |
post-weaning female piglets |
1.1-3.2 mg/kg feed 18 days |
[76] |
| Female Kunming Mice | no effect of serum IgG, IgM, IgA | B6C3F1 mice | 10 mg/kg feed 6 weeks |
[77] | |||
| ↓ IgG, IgA, IgM in cell SN | Swine PBMC | 10 mM 7 days |
[19] | ||||
| ↓ IgG ↓ IgM |
BALB/c mice | 5, 10, 15 mg/kg b.w./day 2 weeks |
[66] |
1 SRBC (sheep red blood cell); 2 PFC (plaque forming cells).
Fusarium mycotoxins on human and animal host susceptibility to infectious diseases, it was shown that in contrast to other fusariotoxins, the interaction between zearalenone and infectious disease was less studied [81]. Pestka and collaborators showed that mice fed 10 mg ZEA/kg feed for 2 weeks and infected with
Listeria monocytogenes
4.2. Effect of Zearalenone on Cellular Immune Response
Beside its effect on humoral immune response, ZEA cause negative effects on cellular immune response (e.g., cell viability and proliferation, apoptosis and necrosis, and cytokine production) due to the fact that most of the cells involved in the immune response have estrogenic receptors on their surface [82]. A disturbance of cell proliferation and apoptosis was reported in a number of studies investigating ZEA toxicity. As proved by many studies zearalenone is an inductor of apoptosis and necrosis in different type of immune cells. B and T lymphocytes are among the immune cells affected by the action of ZEA. It seems in fact that the immunosuppression produced by ZEA is caused by the decrease in B and T lymphocytes viability and proliferation [66][
| ↓ CD21 | |||
| + | |||
| B, CD2 | |||
| + | |||
| T, CD4 | |||
| + | |||
| CD8 | |||
| −T ↑ CD8+CD4− and TCRγδ+ T |
Polish Large White female | 0.1 mg/kg 42 days |
[97][109] |
| ↓ CD4+CD8+, CD4+, CD4+/CD8+(2 mg/kg) ↑ CD8+ (3.2 mg/kg) |
Landrace × Yorkshire × Duroc Piglets |
1.1, 2, 3.2 mg/kg feed 18 days |
[76] |
| ↑ IL-1β and IL-6, ↓ IFN-γ cytoplasmic edema chromatin deformation splenic damages |
Yorkshire × Landrace × Duroc Piglets |
1.1, 2.0, 3.2 mg/kg feed 18 days |
[98][110] |
| ↓ IFN-γ, IL-10↓ proliferation |
kidneys of piglets | 0.8 mg/kg 4 weeks |
[99][111] |
| ↑ IL-2, ↓ IL-6 | Isa Brown chicken splenic lymphocytes |
0.1–25 μg/mL 48 h |
[82] |
Induction of cellular death and proliferation inhibition was also found on other type of immune cells than lymphocytes. Viability of polymorphonuclear cells was decreased after 24h by 50 µM of ZEA and its metabolites α-ZOL, β-ZOL and ZAN action [52] and the exposure of RAW 264.7 macrophages to 10 to 100 μM ZEA for 24h diminished the cell viability in a dose dependent manner through apoptosis and necrosis [56][100].
In weaned piglets, ZEA (0.5, 1.0 and 1.5 mg/kg) induces ovarian development by accelerating ovarian follicles proliferation through the activation of ERs/GSK-3β-dependent Wnt-1/β-catenin signaling pathway [101]. Also, ZEA (0.5–1.5 mg/kg) determined an abnormal uterine proliferation through TGF signaling pathway [102]. Investigating other regulatory pathways involved by ZEA in uterine hypertrophy, these authors exposed porcine endometrial epithelial cells to ZEA 0, 5, 20 and 80 μmol/L for 24 h and cell cycle was analyzed. A significant lower proportion of cells in S and G2 phases and an increase in the phase of G1 was found at ZEA 80 μmol/L [102]. The related mechanism involved also the activation of Wnt/β-catenin signaling pathway.
In mouse ovarian granulosa cells Chen et al. [103] and Zhang et al. [104] demonstrated by MTT, EdU and flow cytometry that ZEA suppressed in vitro cell viability at 30–150 μM and increased apoptosis at 15–60 μM after 24 or 72h of exposure. Close to the results recorded by Song et al. [102] in pig (a decreased of cell proportion in the S and G2 phase at ZEA 80 µmol/L), Zhang et al. [104], found that mouse granulosa cells were arrested in G1 phase of cell cycle and the cells proportion decreased in phase S and G2 after 30 μM ZEA treatment. However, in another study this author [105] found species specific ZEA effect, pig being more sensitive than mouse. Thus, ZEA 10 μM significantly increased the percentage of TUNEL porcine positive cells while the TUNEL percentage of granulosa mouse cells increased only at 30 μM.
Also, it has been observed that the metabolite of ZEA, α-ZOL at 9.4 µM concentration induces an increase in porcine granulosa cell proliferation and in progesterone levels [106].
In rats, ZEA perturb cell proliferation in both female and males. In Sprague Dawley males receiving by gavage 10 or 20 mg ZEA/kg b.w., the toxin significantly decreased the numbers of Leydig cells (adjacent cells to the testicle seminiferous tubules) which could produce anomalies of the male reproductive tract [107]. Similar results on Leydig cells were found by Wang et al. [108], with ZEA 50 μM. By contrast, Zheng et al. [89], found that low doses of zearalenone (0.01, 0.02, 0.03, 0.04, and 0.05 μmol/L) stimulated cell viability of TM3 cells (Leydig cells) measured by using the xCELLigence real-time cell analysis. Also, under the action of ZEA (20μM), cell viability of Sertoli cells derived from Male Wistar, which are important for male reproductive system, increased over control [109].
In human, study of Marton et al. [110], on ovarian epithelial cells investigating the effect of several compounds, ZEA among them on miRNA expression in correlation with cells estrogenic sensitivity observed that ZEA (1, 10, 100, 1000 nM) increased the rate of cell proliferation in direct proportion to ZEA concentration and depending on the presence of ER-α. By contrast, 30 µM of ZEA in prostate cancer cells induced G2/M cell cycle arrest and decreased cell viability compared to control [111].
5. Effect of Zearalenone on Immune Organs
Table 4), but the toxin has been responsible for immune organs atrophy and depletion as well as for other histopathological modifications in immune organs. ZEA caused also a decrease of B cell percentage in the spleen or swelling of red pulp [57][96][99].
Table 4.
| Effect (s) | Species/Cell Type | Dose/Time of ZEA Administration |
References |
|---|
| Thymic atrophy with histological and thymocyte phenotype changes and decrease in the B cell percentage in the spleen |
Wistar rats | 3.0 mg/kg b.w. 28 days |
[57] |
| Atrophy of white pulp and swelling of red pulp | post-weanling gilts | 2.0, 3.2 mg/kg feed 18 days |
[98][110] |
| No effect on spleen and bursa of Fabricius weights | one-day-old broiler chicks | 10–800 mg/kg feed 21 days |
[113] |
| No effect on spleen and bursa of Fabricius weights | one-day -old broiler chicks | 50–800 mg/kg feed 3 weeks |
[114] |
| Enlargement of the spleen in males | Sprague Dawley rats | 1.25, 3.75 mg/kg b.w. 8 weeks |
[115] |
| No effect on spleen weight | Sprague Dawley rats | 0.5, 0.9, 1.8, 3.6 mg/kg b.w. 4 weeks |
[116] |
| No effect on spleen weight | BALB/c mice female, 7-weeks-old |
5, 20 mg/kg b.w. 14 days |
[37][38] |
| No effect on spleen weight | White Leghorn female chickens, 2-weeks-old |
50, 200, 400, 800 mg/kg b.w. 7 days |
[117] |
| No macroscopic changes and no histopathologic effect on lymph nodes | 32-day-old gilts | 0.75 mg/kg feed 21 days |
[80][81] |
| No effect on thymus and spleen weights No histopathologic changes |
B6C3F1 weanling female mice | 10 mg/kg feed 56 days |
[77] |
| Decreased immune organ weight and lymphocyte counts, lymphoid atrophy and depletion in the spleen | BALB/c female mice |
40, 80 mg ZEN/kg b.w. 28 days |
[118] |
