Musculoskeletal disorders and the following pain were common in most people’s daily life, and the musculoskeletal pain caused by musculoskeletal disorders was the second most common cause of disability. Many established factors, such as physical, biological, cognitive, behavioral, social, and occupation, were correlated with the pain following musculoskeletal disorders
- Multi-Modal Therapies for Kinesiophobia
1. Introduction
Fear was considered to be an explanation of why pain and associated outcomes such as disability persist once the body injury had healed[1][2], and the fear-avoidance model of pain was one of the frameworks which could explain the development and persistence of the pain and disability following a musculoskeletal injury[3][4]. According to this model, people with a trait tend to have fear and catastrophic thoughts in response to pain were more at risk of developing chronic musculoskeletal pain after an injury than people who did not have this tendency[2][4]. These people over-reacted in response to actual or potential threats, developing avoidance behaviors to prevent a new injury/re-injury[2]. Fear in relation to pain had been described with various conceptual definitions, among which pain-related fear, fear-avoidance beliefs, fear of movement, and kinesiophobia were the most commonly used[5].
Kinesiophobia was one of the most commonly used conceptual definitions which could describe fear in relation to pain[6]. Kinesiophobia (also known as the fear of movement) was defined as an excessive, irrational, and debilitating fear to carry out a physical movement due to a feeling of vulnerability to a painful injury or re-injury[6]. It could be acquired through a direct aversive experience such as pain and trauma or through social learning such as observation and instruction [7]. Kinesiophobia had been associated with pain, disability, and quality of daily life to some extent[8]. The prevalence of kinesiophobia in chronic pain was from 50% to 70%[9][10].
The objective of rehabilitation is to recover physical exercises’ performance, regain the capacity of daily activities, and restore social functions. In recent years, studies on the rehabilitation of musculoskeletal disorders had begun to focus on the fear in relation to pain[11][12]. The fear in relation to pain would cause people to produce fear-avoidance and had a negative effect on their quality of life. Therefore, not only the rehabilitation at the physical level but also the rehabilitation at the psychological level should be paid attention to[13][14][15][16]. At the same time, as mentioned above, kinesiophobia could be acquired through many different ways (e.g., personal experience, social learning)[7], therapies combined multi-modal from both psychological and physical perspectives had become increasingly popular[11][17][18]. However, at present, only a few studies focus on the advantage of multi-modal therapies over uni-modal therapies, and most of the studies on the rehabilitation of musculoskeletal disorders were limited to specific musculoskeletal disorders. There was a lack of high-quality evidence from the macro-perspective. To answer this question, the terms “physical therapy” and “psychological therapy” should be defined in this review at first.
Moreover, a quantitative indicator was required to assess the fear of movement, and there was not a specific tool to assess fear of movement directly[5]. The term “kinesiophobia” would be used. People with kinesiophobia would change their movements to avoid pain and adjust their motor behaviors[8]. The processing of pain and pain-related information in people with musculoskeletal disorders could be related to how kinesiophobia was perceived[19]. Therefore, a greater degree of kinesiophobia predicted greater levels of fear of pain and a great inclination to avoid physical movements[20].
Kinesiophobia could be measured by the Tampa Scale of Kinesiophobia (TSK) [21]. Since the Tampa Scale of Kinesiophobia had good validity in the quantization of kinesiophobia, the change of TSK scores would reflect the effect of therapy and be taken as a comparative indicator of therapy effect to some extent[22][23]. In the original version of the Tampa Scale of Kinesiophobia, participants would be asked to respond to how much they agreed with each of the 17 items, and the ratings available were: (1) disagree; (2) partially disagree; (3) partially agree; (4) strongly agree. The score of each item varies from 1–4 or 0–3. The responses were summed, and the generated score, which ranges from 17 to 68 or from 0 to 51[9][21]. However, the TSK scores were usually reported as a secondary outcome, and that there was a limited number of studies that focus on the treatments for kinesiophobia. It made that a special study search strategy, information extraction, and data processing methods need to be applied.
2. Systematic Review of Related Studies
2.1. Study Selection, Information, and Original Data
After deduplication and applying the exclusion criteria, 12 studies[24][25][26][27][28][29][30][31][32][33][34][35] of the total 1042 studies were included for analysis. The flow diagram could be seen in
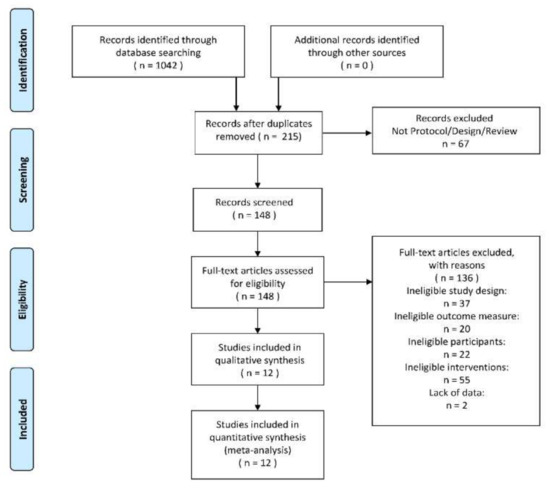
Figure 1.
Table 1.
| Study Design | Characteristics of Participants | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Version of TSK | Multi-Modal Therapy Group | Uni-Modal Therapy Group | Mean Age | Type of Pain | |||||

| Study | Group | Baseline (T0) | Follow-Up Times (T1) | Follow-Up Times (T2) | Follow-Up Times (T3) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| TSK + | N0 | TSK + | Duration | N1 | TSK + | Duration | N2 | TSK | ||||
2
2
2
Table 4.
| Statistics of Heterogeneity Test | 95% CI of T2 | 95% CI of I2 | Prediction Intervals | ||||||
|---|---|---|---|---|---|---|---|---|---|
Table 5.
| Outcome Subdivision | Subgroups | Statistics of Heterogeneity Test | 95% CI of T2 | 95% CI of I2 | Prediction Intervals | + | Duration | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| df | N | 3 | Q | I2 | Tau2 | LL | UL | LL | UL | LL | UL | ||
| Language | R | Intervention | Duration of Intervention (Weeks) | N | Intervention | ||||||||
| Index | Duration of Treatments | Mean Age of Participants | Follow-Up Times (Week) | ||||||||||
| Duration of Intervention (Weeks) | N | ||||||||||||
| Gardner 2019 [26] | English | 0.820 | Education + Patient-led goal setting intervention | 8 | 37 | Standardised advice to exercise with a plan | 8 | 38 | 44.51 | Chronic Low-back Pian |
| Gardner 2019[26] | OG | 36.60 (7.50) | 37 | 29.30 (6.90) | |||||
| df | Q | I2 | Tau2 | LL | UL | LL | UL | LL | UL |
| Types of Pain | CLBP | 10 | 323.8 | 97% | 8 | 37 | 30.00 (5.30) | 16 | 29.62 | 37 | 3.63 | 5.37 | 79% | 85% | 31.20 (7.90) | 48 | 37 | 0.00 * | 21.29 |
| Nambi 2020-Arm1 |
| Number of obs | N | 24 | 24 | 24 | |||||||
| [35] | English | 0.820 | Virtual reality training | 4 | 20 | Isokinetic training with a plan | 4 | 20 | 23.00 | Chronic Low-back Pian | |
| CG | 39.90 (9.30) | 38 | 39.40 (8.30) | ||||||||
| 23 | |||||||||||
| 8 | |||||||||||
| 1549.94 | 99% | 34.21 | 3.37 | ||||||||
| 38 | |||||||||||
| REML estimate of between-study variance | Tau2 | 4.09 | 0.87 | 0.89 | 0.00 * | 24.39 | 19.08 | 29.86 | |||
| Nambi 2020-Arm2 | English | 0.820 | Virtual reality training | 4 | 20 | Conventional training with a plan | 4 | 20 | 23.25 | Chronic Low-back Pian | |
| 39.30 (8.10) | |||||||||||
| 95% | 5.34 | 0.70 | |||||||||
| % residual variation due to heterogeneity | I-squared_res | 98.38% | 96.11% | 99.58% | |||||||
| Saracoglu 2020-Arm1 [32] | |||||||||||
| Proportion of between-study variance explained | |||||||||||
| Turkish | 0.806 | Manual therapy + Supervised home exercise + Pain neuroscience education | 4 | ||||||||
| Adj R-squared | 14.46% | 33.10% | |||||||||
| 20 | Manual therapy + Supervised home exercise | 4 | 19 | 40.50 | Chronic Low-back Pian | ||||||
| −4.74% | |||||||||||
| Saracoglu 2020-Arm2 | Turkish | 0.806 | Manual therapy + Supervised home exercise + Pain neuroscience education | 4 | 20 | Supervised home exercise | 4 | 18 | 39.94 | Chronic Low-back Pian | |
| 1.28 | 73% | 83% | 0.14 | 14.10 | |||||||
| Gustavsson 2006 [ | |||||||||||
| Statistical Significance | P-value | 0.052 | 0.002 | 0.963 | |||||||
| 24] | Swedish | 0.910 | |||||||||
| CG | 57.93 (4.30) | ||||||||||
| Relaxation treatment | 7 | 13 | |||||||||
| 20 | 40+ | 8 | 63.73 | 46.21 (4.10) | |||||||
| Treatment as usual | 20 | ||||||||||
| 87% | |||||||||||
| 16 | |||||||||||
| 4 | 0.61 | 20 | 0.10 | 0.24 | 53% | 73% | 1.01 | 7.05 | |||
| Monte Carlo Permutation Test | Adjusted P-value | 0.139 | 0.008 | 1.000 | |||||||
| Duration of Treatments | 0–3 weeks | 3 | 5.31 | 44% | 0.58 | 0 * | 0.98 | 0% * | 57% | 7.03 | 16.29 |
| 4–6 weeks | 11 | 1065.22 |

2residual
2
2residual
2
2.4.3. Statistical Power
Table 7.
| Study | Statistical Power of Study | Subdivisions | Subgroups | Statistical Power of Effect Combination | Statistical Power of Heterogeneity Test | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Gardner 2019 (1) [26] | 13.45% | Types of Pain | CLBP | 100.00% | 51.76% | |||||||||||||||||
| Gardner 2019 (2) | 18.34% | CNP | 48.92% | 39.09% | ||||||||||||||||||
| Gardner 2019 (3) | 8.15% | UEMD | 100.00% | 22.36% | ||||||||||||||||||
| Nambi 2020-Arm1 (1)[35] | 5.62% | Follow-up times | 0–12 weeks | 100.00% | 61.90% | |||||||||||||||||
| Nambi 2020-Arm1 (2) | 11.75% | 13–24 weeks | 99.66% | |||||||||||||||||||
| 55 | Ordinary general practitioner care | 6 | 56 | 63.64 | Knee Osteoarthritis Pain | |||||||||||||||||
| 16 | 38 | 37.30 (8.00) | 48 | 38 | ||||||||||||||||||
| 39.09% | ||||||||||||||||||||||
| 38.64 (3.90) | 24 | 19 | ||||||||||||||||||||
| 37.48 | Chronic Neck Pain | |||||||||||||||||||||
| Meijer 2006 [27] | Dutch | 0.780 | Treatment combined physical and psychological sessions | 2 | 20 | Usual care by occupational health services | 2 | 14 | 38.14 | Upper extremity musculoskeletal disorders | ||||||||||||
| Gulsen 2020 [ | ||||||||||||||||||||||
| Nambi 2020-Arm1[35] | OG | 57.52 (4.80) | 20 | 26.43 (3.50) | 4 | 20 | 20.12 (2.50) | 24 | 19 | |||||||||||||
| CG | 58.11 (4.50) | 20 | 27.54 (3.80) | 4 | 20 | 21.21 (2.40) | 24 | 20 | ||||||||||||||
| Nambi 2020-Arm2 | OG | 57.52 (4.80) | 20 | 26.43 (3.50) | 4 | 20 | 20.12 (2.50) | 24 | 19 | |||||||||||||
| Javdaneh 2020[34] | Persian | 0.920 | Cognitive functional therapy + Scapular exercise | 6 | 24 | |||||||||||||||||
| Saracoglu 2020-Arm1 | ||||||||||||||||||||||
| Scapular exercise with a plan | ||||||||||||||||||||||
| [32] | ||||||||||||||||||||||
| 6 | 24 | 29.50 | Chronic Neck Pain | |||||||||||||||||||
| OG | 44.35 (4.30) | 20 | 35.55 (5.75) | 4 | 20 | 35.19 (3.99) | 6 | |||||||||||||||
| Ris 2016 [28] | English | 0.820 | Physical training + Specific exercises + Pain education | 16 | 101 | Pain education | 16 | 99 | 45.15 | Chronic Neck Pain | ||||||||||||
| CG | 45.10 (4.45) | 19 | 41.63 (5.23) | 4 | 19 | 42.21 (5.04) | 6 | |||||||||||||||
| Nambi 2020-Arm2 (1) | 17.54% | 24+ weeks | 48.16% | 16.58% | ||||||||||||||||||
| Bahat 2015 | Dutch | 0.780 | Cervical kinematic training + Interactive Virtual Reality training | 5 | 16 | Cervical kinematic training with a plan | 5 | 16 | 40.88 | Chronic Neck Pain | ||||||||||||
| Saracoglu 2020-Arm2 | OG | 44.35 (4.30) | 20 | 35.55 (5.75) | 4 | 20 | 35.19 (3.99) | 6 | ||||||||||||||
| Tompson 2016 [29] | English | 0.820 | Cognitive-behavioural physiotherapy + Progressive neck exercise | 24 | 29 | Progressive neck exercise | 24 | 28 | 47.53 | Chronic Neck Pain | ||||||||||||
| Yilmza 2017 [33 | ||||||||||||||||||||||
| CG | 45.55 (4.10) | 18 | 44.94 (4.70) | 4 | 18 | 44.88 (5.10) | 6 | |||||||||||||||
| ] | Turkish | 0.806 | Virtual walking therapy | 2 | 22 | Traditional Physiotherapy | 2 | |||||||||||||||
| Gustavsson 2006[24] | OG | 26.00 (7.46) | 13 | 27.00 (5.22) | 7 | 13 | ||||||||||||||||
| 22 | 25.14 | Non-special Low-back Pain | ||||||||||||||||||||
| 29.00 (5.22) | 20 | 13 | ||||||||||||||||||||
| Helminen 2015[31] | Finnish | 0.890 | Cognitive-behavioral group intervention contains skill training plan | |||||||||||||||||||
| CG | 29.50 (1.67) | |||||||||||||||||||||
| 6 | ||||||||||||||||||||||
| 16 | 32.00 (0.00) | 7 | 16 | 30.00 (2.00) | 20 | 16 | ||||||||||||||||
| 30 | ||||||||||||||||||||||
| Javdaneh 2020 [34] | OG | 50.00 (5.23) | 24 | 21.00 (5.22) | 6 | 24 | ||||||||||||||||
| ] | Turkish | 0.806 | Immersive Virtual Reality + Exercise | 8 | 8 | Exercise with a plan | ||||||||||||||||
| 19.33 | ||||||||||||||||||||||
| CG | 49.00 (4.78) | 24 | 30.00 (3.55) | 6 | 24 | |||||||||||||||||
| 8 | 8 | 42.50 | Fibromyalgia | |||||||||||||||||||
| Total | 405 | 398 | ||||||||||||||||||||
| Ris 2016[28] | OG | 37.80 (0.69) | 101 | 36.57 (4.50) | 16 | 101 | Average | 0.829 | 7.1 | 8.1 | 38.7 |
| CG | ||||||||||||||
| 37.70 (0.71) | ||||||||||||||
| 99 | ||||||||||||||
| 37.49 (4.50) | ||||||||||||||
| 16 | ||||||||||||||
| 99 | ||||||||||||||
| Bahat 2015[25] | OG | 32.75 (6.80) | 16 | 30.13 (5.70) | 5 | 16 | 31.23 (6.50) | 12 | 14 | |||||
| CG | ||||||||||||||
| Nambi 2020-Arm2 (2) | 5.82% | Mean Age of Participants | 20–30 | 100.00% | 35.41% | |||||||||
| 99% | 45.64 | |||||||||||||
| Saracoglu 2020-Arm1 (1)[32] | 14.54% | |||||||||||||
| 3.73 | 4.74 | |||||||||||||
| 30–40 | 99.99% | 39.09% | ||||||||||||
| 89% | 91% | 0.00 * | 23.12 | |||||||||||
| 7–9 weeks | 5 | 54.64 | ||||||||||||
| Saracoglu 2020-Arm1 (2) | ||||||||||||||
| 91% | 13.68 | 1.95 | 4.86 | |||||||||||
| 6.13% | ||||||||||||||
| 59% | 78% | |||||||||||||
| 40+ | 99.42% | 45.79% | ||||||||||||
| 0.00 * | 14.31 | |||||||||||||
| 9+ weeks | 1 | 2.39 | 58% | 4.38 | 0 * | 6.85 | 0% | 69% | N/N | N/N | ||||
| Saracoglu 2020-Arm2 (1) | 5.61% | Physical Therapy in Control Groups | Active Exercise | 100.00% | 57.10% | |||||||||
| Follow-up Times | 0–12 weeks | 14 | 965.81 | 99% | 35.78 | 3.40 | 4.34 | 87% | 89% | 0.00* | 20.28 | |||
| Saracoglu 2020-Arm2 (2) | 21.80% | Passive Therapy | 100.00% | 39.09% | ||||||||||
| 13–24 weeks | 6 | 380.24 | 98% | 53.32 | 4.90 | 7.19 | 85% | 89% | 0.00 * | 25.90 | ||||
| Gustavsson 2006 (1)[24] | 19.81% | Duration of Treatments | 0–3 weeks | 100.00% | 27.16% | |||||||||
| 24+ weeks | 1 | 37.07 | 97% | 13.05 | 1.02 | 3.15 | 74% | 90% | N/N | N/N | ||||
| Gustavsson 2006 (2) | 11.61% | 4–6 weeks | 100.00% | 54.51% | ||||||||||
| Physical Therapy in Control Groups | Active Exercise | 12 | 327.26 | 96% | 27.47 | 3.63 | 5.34 | 78% | 84% | 0.00 * | ||||
| 34 | ||||||||||||||
| 19.82 | ||||||||||||||
| ] | 56.06% | 7–9 weeks | 55.56% | 35.41% | ||||||||||
| Passive Therapy | 6 | 546.14 | 99% | 39.00 | ||||||||||
| Ris 2016[28] | ||||||||||||||
| 3.13 | ||||||||||||||
| 64.57% | 9+ weeks | 14.78% | ||||||||||||
| 4.36 | 88% | 91% | 0.00 * | 30.38 (5.80) | 16 | 28.64 (9.90) | 5 | 14 | 30.00 (5.90) | 12 | 12 | |||
| 23.27 | Tompson 2016[29] | OG | 36.70 (7.10) | 29 | 32.00 (14.11) | 24 | 29 | |||||||
| CG | 33.60 (9.00) | 28 | 33.80 (15.04) | 24 | 28 | |||||||||
| Yilmza 2017[33] | OG | 43.72 (4.32) | 22 | 29.56 (4.04) | 2 | 22 | ||||||||
| CG | 40.36 (5.61) | 22 | 38.70 (5.44) | 2 | 22 | |||||||||
| Helminen 2015[31] | OG | 35.00 (1.25) | 55 | 33.00 (1.05) | 6 | 55 | ||||||||
| CG | 33.30 (1.35) | 56 | 32.50 (1.33) | 6 | 56 | |||||||||
| Meijer 2006[27] | OG | 38.90 (1.51) | 20 | 29.10 (1.54) | 8 | 20 | 25.80 (2.65) | 24 | 20 | 26.40 (1.90) | 48 | 20 | ||
| CG | 40.91 (1.81) | 14 | 41.00 (1.68) | 8 | 14 | 39.90 (3.16) | 24 | 14 | 40.40 (2.65) | 48 | 14 | |||
| Gulsen 2020 [30] | OG | 49.00 (4.44) | 8 | 35.00 (7.41) | 8 | 8 | ||||||||
| CG | 47.00 (7.22) | 8 | 40.00 (5.37) | 8 | 8 |
+: Mean (SD); TSK: Tampa scale of Kinesiophobia; OG: Operate group (Multi-modal therapy); CG: Control group (Uni-modal therapy).

2.2. Risk of Bias
Supplementary File (Figure S1)
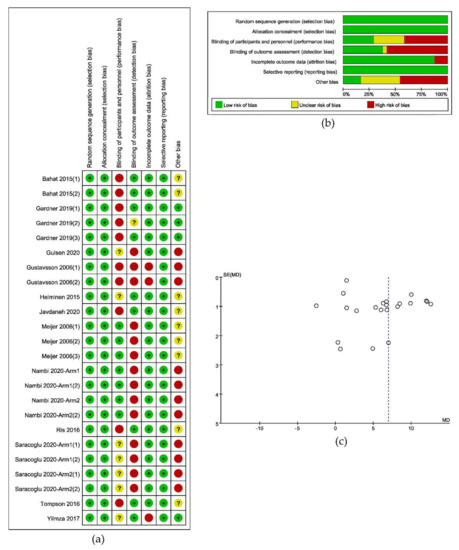

Figure 2.
a
b
c
2.3. Data Extraction and Management
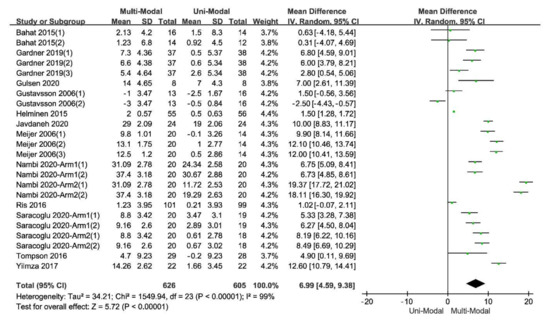
Figure 3.
Table 3.
| Study | Duration of Intervention (Weeks) | Follow-Up Times (Weeks) | Mean Age | Experiment | Control | ||||
|---|---|---|---|---|---|---|---|---|---|
| MD | SD | N | MD | SD | N | ||||
| Gardner 2019 (1) [26] | 8 | 8 | 44.51 | 7.30 | 4.36 | 37 | 0.50 | 5.37 | 38 |
| Gardner 2019 (2) | 8 | 16 | 44.51 | 6.60 | 4.38 | 37 | 0.60 | 5.34 | 38 |
| Gardner 2019 (3) | 8 | 48 | 44.51 | 5.40 | 4.64 | 37 | 2.60 | 5.34 | 38 |
| Nambi 2020-Arm1 (1) [35] | 4 | 4 | 23.00 | 31.09 | 2.78 | 20 | 24.34 | 2.58 | 20 |
| Nambi 2020-Arm1 (2) | 4 | 24 | 23.00 | 37.40 | 3.18 | 20 | 30.67 | 2.88 | 20 |
| Nambi 2020-Arm2 (1) | 4 | 4 | 23.25 | 31.09 | 2.78 | 20 | 11.72 | 2.53 | 20 |
| Nambi 2020-Arm2 (2) | 4 | 24 | 23.25 | 37.40 | 3.18 | 20 | 19.29 | 2.63 | |
df: Degree of freedom; LL: Lower limit; UL: Upper limit; *: the true value is less than 0; CNP: Chronic neck pain; CLBP: Chronic low-back pain; UEMD: Upper extremity musculoskeletal disorders; N/N: when df = 1, the t-value could not be calculated so that the prediction intervals could not be estimated as well.

2.4.2. Meta-Regression
®
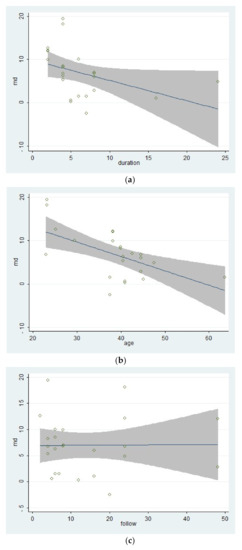
Figure 5.
a
b
c
Table 6.
| 20 |
| Saracoglu 2020-Arm1 (1) | |||||||||
| [ | |||||||||
| 32 | |||||||||
| ] | |||||||||
| 4 | 4 | 40.50 | 8.80 | 3.42 | 20 | 3.47 | 3.10 | 19 | |
| Saracoglu 2020-Arm1 (2) | 4 | 6 | 40.50 | 9.16 | 2.60 | 20 | 2.89 | 3.01 | 19 |
| Saracoglu 2020-Arm2 (1) | 4 | 4 | 39.94 | 8.80 | 3.42 | 20 | 0.61 | 2.78 | 18 |
| Saracoglu 2020-Arm2 (2) | 4 | 6 | 39.94 | 9.16 | 2.60 | 20 | 0.67 | 3.02 | 18 |
| Gustavsson 2006 (1)[28] | 7 | 7 | 37.48 | -1.00 | 3.47 | 13 | -2.50 | 1.67 | 16 |
| Gustavsson 2006 (2) | 7 | 20 | 37.48 | -3.00 | 3.47 | 13 | -0.50 | 0.84 | 16 |
| Javdaneh 2020[34] | 6 | 6 | 29.50 | 29.00 | 2.09 | 24 | 19.00 | 2.06 | 24 |
| Ris 2016 [28] | 16 | 16 | 45.15 | 1.23 | 3.95 | 101 | 0.21 | 3.93 | 99 |
| Bahat 2015 (1)[24] | 5 | 5 | 40.88 | 2.13 | 4.20 | 16 | 1.50 | 8.30 | 14 |
| Bahat 2015 (2) | 5 | 12 | 40.88 | 1.23 | 6.80 | 14 | 0.92 | 4.50 | 12 |
| Tompson 2016 [29] | 24 | 24 | 47.53 | 4.70 | 9.23 | 29 | -0.20 | 9.23 | 28 |
| Yilmza 2017[33] | 2 | 2 | 25.14 | 14.26 | 2.62 | 22 | 1.66 | 3.45 | 22 |
| Helminen 2015[31] | 6 | 6 | 63.64 | 2.00 | 0.57 | 55 | 0.50 | 0.63 | 56 |
| Meijer 2006 (1) [27] | 2 | 8 | 38.14 | 9.80 | 1.01 | 20 | -0.10 | 3.26 | 14 |
| Meijer 2006 (2) | 2 | 24 | 38.14 | 13.10 | 1.75 | 20 | 1.00 | 2.77 | 14 |
| Meijer 2006 (3) | 2 | 48 | 38.14 | 12.50 | 1.20 | 20 | 0.50 | 2.86 | 14 |
| Gulsen 2020 [30] | 8 | 8 | 42.50 | 14.00 | 4.65 | 8 | 7.00 | 4.30 | 8 |


2.4. Additional Analysis
2.4.1. Subgroup Analysis
2
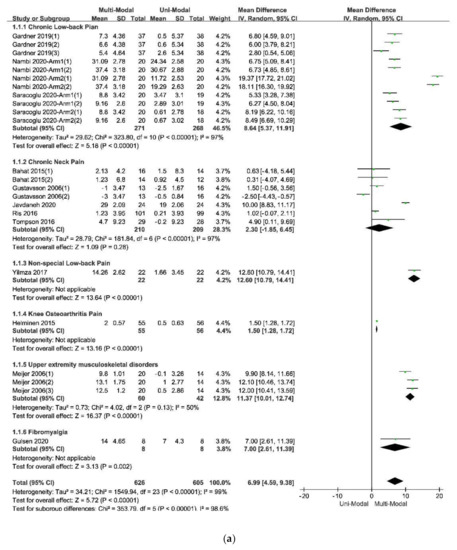
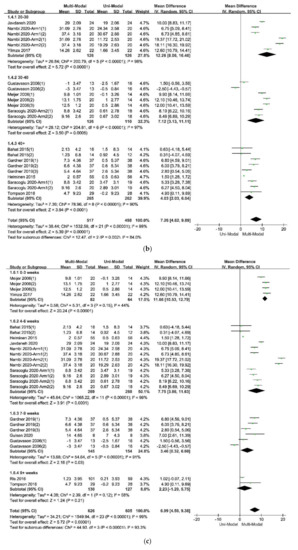
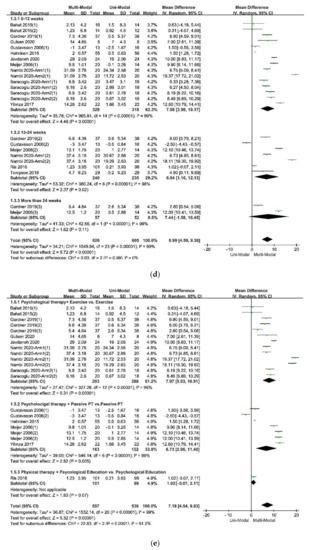
Figure 4.
a
b
c
d
e
| CNP | |||||||||||
| 6 | 181.84 | 97% | 28.79 | 3.39 | 5.70 | 78% | 85% | 0.00 * | 16.59 | ||
| UEMD | 2 | 4.02 | 50% | 0.73 | 0 * | 1.18 | 0% * | 62% | 0.00 * | 26.55 | |
| Mean Age of Participants | 20–30 | 5 | 49.24 | 90% | 2.71 | 0.39 | 1.02 | 56% | 77% | 6.14 | 18.38 |
| 30–40 | 6 | 127.78 |

3. Discussion
Although a considerable heterogeneity within the included studies, the pooled effect was positive with a statistical significance, indicating that multi-modal therapies had an advantage over uni-modal therapies. High-quality evidence reported that a long-lasting multi-modal program was superior to the exercise program in reducing disability, fear-avoidance beliefs and pain, and enhancing the quality of life of patients with different kinds of pain[11]. The effects were clinically tangible and lasted for at least one year after the intervention ended[11][16][18].
Figure 4a indicated that the multi-modal therapies were more used in the treatments for chronic pain in the people’s trunk, especially in the neck and low back. This result was consistent with the previous fear-avoidance model about the fear of pain, which was that the experience of chronic, ongoing pain tends to become fear of pain[2][4]. What’s more, multi-modal therapies combined with physical therapies and psychological therapies had an advantage over therapies from a physical perspective, no matter the physical therapy was passive or active, as was showed in
Figure 4e. Therefore, it was necessary to add psychological therapies in the treatments of chronic pain. A similar effect was found in studies that compared passive and active treatments for neck-shoulder pain and used the Visual Pain Scale (VAS) as an outcome measure[36]. Simultaneously, the age of participants, the duration of treatments, and the different follow-up times might affect the results. Within these factors, the participants’ age was more likely to be taken into consideration since the pooled effects showed a decreasing trend with the increase of age in
Figure 4b. According to the previous study results, older people were more often had a pain of longer duration, more frequently and of more complexity, felt more disabled, received more pain treatments and had more health problems, and often used passive coping for pain[37]. The influence of different durations of treatments seemed unclear, as was in
Figure 4d, indicating that the effects of multi-modal therapies might clinically tangible and lasted for a long time[11][38].
According to the meta-regression results, the covariate “follow-up times” might not be the source of the heterogeneity because that different follow-up times of included studies could hardly explain the residual variation due to between-study variance[39]. On the contrary, the differences of mean age of participants and the duration of treatments could explain part of the between-study variance, meaning that the two covariates might be part of the sources of the heterogeneity and would affect the effects of therapies. What’s more, the meta-regression of the mean age of participants had a significant statistical difference, showing that the effect of multi-modal therapies might decrease with age. This result might be related to the mental health and capacity of recovery of older adults[40][41]. Besides, the result of the meta-regression of the duration of treatments tended to be statistically significant. It indicated that there might be no additional benefit from increasing the duration of therapy for kinesiophobia. Finally, the goodness of fit of the model used in the meta-regression for these covariates was low, indicating that the results should be interpreted carefully.
A considerable heterogeneity within the included studies could be seen in the heterogeneity test in the meta-analysis and the subgroup analysis. The heterogeneity might come from the different designs of these studies. For example, the included studies had differences in the FITT characteristics (frequency, intensity, time, environments, and types) of the training plan[42][43]. Moreover, the different populations of the participants, the different blinding method, and some other factors, especially the different validities and reliability of the Tampa Scale of Kinesiophobia for participants with different educational backgrounds, culture, personalities, and types of musculoskeletal disorders[22][23][44], might lead a heterogeneity within studies.
The risk of bias was supposed to exist, and the source is various. For example, there were many musculoskeletal disorders that could lead to a fear of physical movements. Still, not all studies in the field of physical rehabilitation reported the score of the Tampa Scale of Kinesiophobia. In fact, to all kinds of musculoskeletal disorders with the following pain, the fear of physical movements was very common[1]. What’s more, different shortened versions of the Tampa Scale of Kinesiophobia, such as TSK-13 and TSK-11, were used in other studies[45][46], making these studies could not be included in the review. Lastly, other resources of publication bias could not be excluded[47][48][49][50]
The statistical power of all pooled effect analysis in this review was larger than that in any single primary study, subgroup analysis, and the heterogeneity test. This result accords with the statistical law of meta-analysis[39].
