In the context of clinical practice, situational awareness refers to conscious awareness (knowledge), which is a mental model of a given clinical situation in terms of its elements and the significance of their interrelation. Situational awareness (SA) facilitates clinical reasoning, diagnostic accuracy, and appropriate goal-directed performance, and it enables clinicians to immediately adapt treatment strategies in response to changes in clinical situational actualities and to modify the course of goal-directed activities accordingly. It also helps clinicians prepare future operational plans and procedures based on the projection of situational developments. SA, therefore, is an important prerequisite for safe clinical procedures.
- situational awareness
- clinical reasoning
- clinical judgement
- decision making
- mental models
- electronic health records
- pattern recognition
- information processing
1. Introduction
2. The Situational Awareness Construct
The framework of situational awareness (SA) refers to SA as an evolving state of knowledge about the dynamically interacting elements of a given situation [7,9][7][9]. According to this framework, all situational knowledge is generated by sequential cognitive steps that promote information processing, and it enables predictions of the immediate future state of an evolving situation (Figure 1) [7,20][7][15]. SA can be viewed as a comprehensive and coherent internal representation of any current situational actualities; it is continuously assessed and updated in accordance with the dynamic state of the situation [10,21][10][16] and is imprinted in the consciousness of the decision maker [3,20][3][15].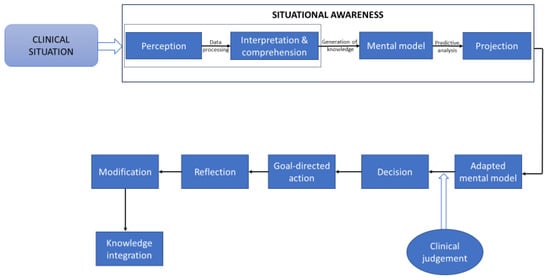
3. Information-Processing Procedures in Relation to Situational Awareness
Reasoning is a cognitive activity that uses information-processing procedures to drive rational processes in order to solve problems; the dynamic and interconnected relationships between data, information, and knowledge are a fundamental prerequisite for clinical reasoning. Data are a collection of unorganized or uncontextualized objective facts, while information is contextualized data that convey values, meanings, and purposes. There is a hierarchal bidirectional relationship among data, information, and knowledge, and this comprises a bottom-up and a top-down direction. In the bottom-up hierarchy, cognitive information-processing activities include capturing situational data and gathering basic informative elements (perception stage), processing data into usable information that is then transformed into clinical-knowledge-based rules and patterns that support clinical judgments and decision making (comprehensive or understanding stage), and predictive analysis (projection stage), all of which enable the execution of goal-directed clinical tasks (Figure 2) [28,29][21][22].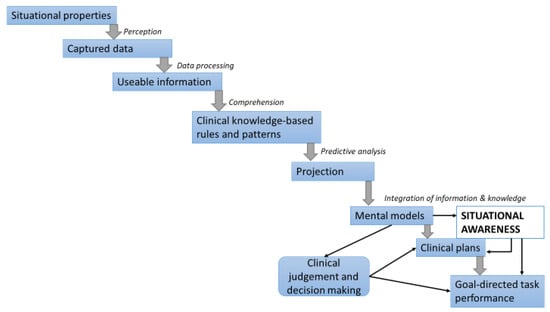
4. Clinical Judgments and Decision Making in Relation to Situational Awareness
The cognitive processes that are required to develop an accurate clinical SA force clinicians to focus their attention and to allocate resources of mental energy to the given situational elements and then to analyze and interpret the captured data and perceived information in the context of the situational constraints and of the performance of the goal-directed tasks. Goal-directed tasks may be pre-determined, and in such cases, the clinician’s role is to identify situational cues that are necessary for the efficient and effective execution of the prescribed plan (top-down); or, in the case of goal-directed activities that still need to be constructed, the clinician has to recognize situational cues that will enable the categorization and conceptualization of the current situation in accordance with previous similar mental situational models. This pattern recognition process facilitates clinical judgments, decision making, and the planning of appropriate goal-directed activities (bottom-up) [21][16] (Flach, 1995) [19][23]. The cognitive pathways involved in information processing in relation to solving clinical problems comprise a non-conscious, automatic, intuitive, and fast reasoning pathway (system 1), as well as a conscious, deliberate, analytical, effortful, and time-consuming reasoning pathway (system 2) [22,32,33][18][26][27]. In the context of clinical practice, a given clinical problem may be typical, atypical, or complex, and it may display elements of uncertainty and/or ambiguity [16,22,34][18][28][29]. Depending on the nature of the clinical situation and on the cognitive functions required for driving the decision-making process, system 1 and system 2 may either operate sequentially with system 1 being the first in action, followed by the analytical and deliberate system 2, which monitors and, if necessary, corrects the intuitive judgments and decisions constructed by system 1, or they may operate concurrently or interchangeably [16,22,32,34][18][26][28][29]. The intuitive reasoning pathway (system 1) that is used to formulate clinical judgments and decisions is based on the experience and expertise of the clinician, on heuristics, and on pre-determined mental models. The mental representations of a given current clinical situation’s elements and circumstances are matched with previous patterns and knowledge of clinical situations stored in the memory by using a pattern recognition process, and each identified match contributes to the understanding of the current clinical situation; the pre-determined mental models are revised and then adapted to accommodate the given current clinical situation. However, in the face of deficiencies in prior knowledge and mental models, as is the case with novices and inexperienced clinicians, intuitive reasoning and heuristics may be ineffective in solving clinical problems [11,34][11][29]. In such circumstances, or when a clinical problem is compound or atypical, the clinician has to employ the deliberate and analytical reasoning pathway of system 2, which is characterized by its time-consuming and complex information-processing operations that require the use of critical thinking, statistical concepts, deductive logic, scientific methods, and focused attention [33][27].5. Emotions as They Relate to Situational Awareness
Emotions may either support or hinder cognitive functioning [38[30][31],39], and it appears that the emotional state of a clinician may influence whether the gathered situational information will be processed intuitively or analytically [40][32]. While a positive affect may support information processing, clinical judgments, and decision making, a negative affect may interfere with sound reasoning, with assessments of the risks of clinical practices, and with weighting the relative clinical importance of situational elements, thus distorting the mental image in SA [16,38,40][28][30][32]. Situational uncertainties and complexities, uncertainty intolerance, worries about inflicting harm to patients, concerns about possible malpractice liability claims, worries about managing a patient’s unrealistic expectations, and a lack of confidence in one’s operational competence are some contextual stressors in clinical practice that may bring about negative emotional responses, such as frustration, anger, agitation, and fear. Fatigue, financial crisis, poor personal health, and intrinsic or substance-induced negative feelings and moods are some non-contextual stressors that may have a negative impact on SA and clinical practice, and they are not dissimilar to the effects described above with regard to contextual stressors [14,16,38][14][28][30]. Some of these non-contextual negative emotions are incidentally induced, typically persist without conscious awareness (‘carryover incidental emotions’), and may affect subsequent clinical judgments and decision-making processes [38][30]. Mental energy is an abstract construct with dynamic properties; it can be viewed as an intrapsychic resource that powers psychological mechanisms including cognition, emotions, motivation, willpower, and executive functioning, all of which are essential for performing goal-directed tasks.6. Interventions That May Boost the Development of SA
Managing SA errors in clinical practice and reducing their occurrence should not be considered the sole responsibility of clinicians. Both clinician- and organization-directed measures are required to improve clinicians’ ability to develop accurate SA and reduce the risk of SA errors [14]. Healthcare organizations should introduce, and clinicians should use, health information technology that enables easy access to relevant and up-to-date information, expert second opinions, digital images, clinical guidelines, and algorithms [16][28]. The successful integration of bioinformatics, clinical data, and information into relevant knowledge and the effective use of clinical decision support systems and electronic health records may simplify the weighing of diagnostic probabilities and their primacy, and they may bring about essential knowledge that is directly applicable to patient-specific clinical situations [44][33]. To boost SA acquisition and avoid SA errors, clinicians should have adequate domain-specific structural knowledge and clinical expertise, and they should master both intuitive and analytical cognitive operations that, in turn, support information processing and clinical reasoning, as well as the identification of common cognitive biases that have a negative impact on the development of accurate clinical SA [16][28]. In the context of SA, meditation, mindfulness, and metacognition may enable clinicians to increase their critical awareness and understanding of the complexities of a given clinical situation and to monitor and evaluate their clinical judgments and rational reasoning so that decision making and goal-directed activities can be modified according to the situational dynamics.7. Conclusions
Situational awareness plays an essential role in the complex and dynamic process of decision making and operational activities in clinical practice. It facilitates the dynamic adaptation of goal-directed plans in response to changing eventualities, and it enables the anticipation of future situational dynamics. Domain-specific experience and expertise and cognitive acuity are essential for developing high-level clinical SA. Situational awareness is susceptible to information overload, cognitive bias, and rapidly changing situational actualities; adequate resources of mental energy are required for its effective development [5]. In order to acquire the skills necessary to develop accurate SA, clinician trainees have to be repeatedly exposed to simulations of complex and dynamic high-fidelity real-life clinical situations.References
- O’Dea, A.; Morris, M.; O’Keeffe, D. Experiential Training for Situation Awareness in the Operating Room. JAMA Surg. 2022, 157, 66–67.
- Endsley, M.R. Situation awareness: Operationally necessary and scientifically grounded. Cogn. Technol. Work. 2015, 17, 163–167.
- Smith, K.; Hancock, P.A. Situation awareness is adaptive, externally directed consciousness. Hum. Factors 1995, 37, 137–148.
- Walshe, N.; Ryng, S.; Drennan, J.; O’Connor, P.; O’Brien, S.; Crowley, C.; Hegarty, J. Situation awareness and the mitigation of risk associated with patient deterioration: A meta-narrative review of theories and models and their relevance to nursing practice. Int. J. Nurs. Stud. 2021, 124, 104086.
- Gaba, D.M.; Howard, S.K.; Small, S.D. Situation awareness in anesthesiology. Hum. Factors 1995, 37, 20–31.
- Fischer, M.A.; Kennedy, K.M.; Durning, S.; Schijven, M.P.; Ker, J.; O’Connor, P.; Doherty, E.; Kropmans, T.J. Situational awareness within objective structured clinical examination stations in undergraduate medical training—A literature search. BMC Med. Educ. 2017, 17, 262.
- Endsley, M.R. Measurement of situation awareness in dynamic systems. Hum. Factors 1995, 37, 65–84.
- Kovacic, Z.; Di Felice, L.J. Complexity, uncertainty and ambiguity: Implications for European Union energy governance. Energy Res. Soc. Sci. 2019, 53, 159–169.
- Harper, A.; Mustafee, N.; Pitt, M. Increasing situation awareness in healthcare through real-time simulation. J. Oper. Res. Soc. 2022, 74, 2339–2349.
- Sarter, N.B.; Woods, D.D. Situation awareness: A critical but ill-defined phenomenon. Int. J. Aviat. Psychol. 1991, 1, 45–57.
- Fithri, Z.N.Z.; Orth, M.; Ibrahim, N. Overview of situational awareness in healthcare and the need for early exposure. Med. J. Malays. 2022, 77, 751.
- Pollack, A.H.; Mishra, S.R.; Apodaca, C.; Khelifi, M.; Haldar, S.; Pratt, W. Different roles with different goals: Designing to support shared situational awareness between patients and clinicians in the hospital. J. Am. Med. Inform. Assoc. 2021, 28, 222–231.
- Khammissa, R.A.G.; Nemutandani, S.; Feller, G.; Lemmer, J.; Feller, L. Burnout phenomenon: Neurophysiological factors, clinical features, and aspects of management. J. Int. Med. Res. 2022, 50, 3000605221106428.
- Khammissa, R.A.; Nemutandani, S.; Shangase, S.L.; Feller, G.; Lemmer, J.; Feller, L. The burnout construct with reference to healthcare providers: A narrative review. SAGE Open Med. 2022, 10, 20503121221083080.
- Gundersen, O.E.; Kucs, R.; Sheehy, T.; de Holden, M.S. Transferring Knowledge Through Decision Support: A Case Study in Drilling. In Proceedings of the IADC/SPE Drilling Conference and Exhibition 2014, Fort Worth, TX, USA, 4–6 March 2014; OnePetro: Richardson, TX, USA, 2014.
- Flach, J.M. Situation awareness: Proceed with caution. Hum. Factors 1995, 37, 149–157.
- Ardito, C.; Di Noia, T.; Fasciano, C.; Lofú, D.; Macchiarulo, N.; Mallardi, G.; Pazienza, A.; Vitulano, F. Towards a Situation Awareness for eHealth in Ageing Society. In Proceedings of the Italian Workshop on Artificial Intelligence for an Ageing Society 2020, Co-Located with 19th International Conference of the Italian Association for Artificial Intelligence (AIxIA 2020), Virtual, 25–27 November 2020; pp. 40–55.
- Laurila-Pant, M.; Pihlajamäki, M.; Lanki, A.; Lehikoinen, A. A protocol for analysing the role of shared situational awareness and decision-making in cooperative disaster simulations. Int. J. Disaster Risk Reduct. 2023, 86, 103544.
- Flach, J.; Mulder, M.; Van Paassen, M. The concept of the situation in psychology. In A Cognitive Approach to Situation Awareness: Theory and Application; Ashgate Publishing: Oxon, UK, 2004; pp. 42–60.
- Dekker, S.; Hollnagel, E. Human factors and folk models. Cogn. Technol. Work. 2004, 6, 79–86.
- Michaels, S.; Goucher, N.P.; McCarthy, D. Considering knowledge uptake within a cycle of transforming data, information, and knowledge. Rev. Policy Res. 2006, 23, 267–279.
- Cato, K.D.; McGrow, K.; Rossetti, S.C. Transforming clinical data into wisdom. Nurs. Manag. 2020, 51, 24.
- Rasmussen, J.; Lind, M. A model of human decision making in complex systems and its use for design of system control strategies. In Proceedings of the 1982 American Control Conference, Arlington, VA, USA, 14–16 June 1982; IEEE: Piscataway, NJ, USA, 1982; pp. 270–276.
- Cummings, M. Informing autonomous system design through the lens of skill-, rule-, and knowledge-based behaviors. J. Cogn. Eng. Decis. Mak. 2018, 12, 58–61.
- Embrey, D. Understanding human behaviour and error. Hum. Reliab. Assoc. 2005, 1, 1–10.
- Croskerry, P. A universal model of diagnostic reasoning. Acad. Med. 2009, 84, 1022–1028.
- Feller, L.; Lemmer, J.; Nemutandani, M.S.; Ballyram, R.; Khammissa, R.A.G. Judgment and decision-making in clinical dentistry. J. Int. Med. Res. 2020, 48, 300060520972877.
- Vally, Z.I.; Khammissa, R.A.G.; Feller, G.; Ballyram, R.; Beetge, M.; Feller, L. Errors in clinical diagnosis: A narrative review. J. Int. Med. Res. 2023, 51, 3000605231162798.
- Feller, L.; Feller, G.; Ballyram, T.; Chandran, R.; Lemmer, J.; Khammissa, R.A.G. Interrelations between pain, stress and executive functioning. Br. J. Pain 2020, 14, 188–194.
- Lerner, J.S.; Li, Y.; Valdesolo, P.; Kassam, K.S. Emotion and decision making. Annu. Rev. Psychol. 2015, 66, 799–823.
- Mirabella, G. The weight of emotions in decision-making: How fearful and happy facial stimuli modulate action readiness of goal-directed actions. Front. Psychol. 2018, 9, 1334.
- Ferrer, R.; Klein, W.; Lerner, J.; Reyna, V.; Keltner, D. Emotions and health decision making. In Behavioral Economics and Public Health; Harvard University Press: Cambridge, MA, USA, 2016; pp. 101–132.
- Castaneda, C.; Nalley, K.; Mannion, C.; Bhattacharyya, P.; Blake, P.; Pecora, A.; Goy, A.; Suh, K.S. Clinical decision support systems for improving diagnostic accuracy and achieving precision medicine. J. Clin. Bioinform. 2015, 5, 4.
