Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is a comparison between Version 1 by Loai A. Elfawy and Version 2 by Conner Chen.
Burns are a widespread global public health traumatic injury affecting many people worldwide. Non-fatal burn injuries are a leading cause of morbidity, resulting in prolonged hospitalization, disfigurement, and disability, often with resulting stigma and rejection. The treatment of burns is aimed at controlling pain, removing dead tissue, preventing infection, reducing scarring risk, and tissue regeneration.
- skin burn
- sustainable biomaterials
- multifunctional bioscaffolds
- c
1. Introduction
Burn, a traumatic injury that leads to a huge disruption in skin structure and function, is a widespread public health problem. Through energy transfer from the causative agent to tissues, heat, cold, friction, electricity, radiation, and chemicals could induce a serious burn injury [1]. Many causative agents are associated with other physiological and pathophysiological responses. A superficial level-up to deep burn might happen after direct exposure to hot grease and liquids, fire, and steam. Another thermal burn type that can damage deep tissue is frostbite burn. Colliquative and coagulation necrosis might happen upon contacting with alkaline or acidic chemicals [2]. The deep tissues affected directly after exposure to electrical shock are greater than the superficial skin injury, which is correlated with the strength of the electric field [3]. According to WHO, there are approximately 180,000 deaths per year due to burns. The highest percentage goes to low- and middle-income countries. In India, over one million moderate to severe burns cases are admitted to hospitals annually. In addition, 17% to 18% of children have temporary and permanent disabilities after burning in Egypt, Colombia, Pakistan, and Bangladesh. The second cause of common injury in Nepal, with 5% of disabilities, is burning. In 2008, around 40,000 patients were hospitalized with different degrees of burn injuries in the United States of America (2018).
Tissue engineering and regenerative medicine (TERM) is one of the most rapidly evolving multidisciplinary fields, which develops several principles for repairing, regrowing, or even replacing diseased or damaged tissues and organs [4]. It combines basic sciences such as material science, biochemistry, biomechanics, polymer chemistry, cell biology, and nanotechnology with applied medical and engineering sciences [5]. In the last few decades, human beings have been dreaming of repairing and restoring the functions of damaged tissues and organs, but now, huge progress has been accomplished. Despite the tremendous progress, TERM is still in its infancy. Bioengineers are trying to extract and innovate new biomaterials that could be a base of engineered replacement tissues to facilitate burn healing. These biomaterials are designed to interact with the biological system of the skin to be used as an alternative extracellular matrix for replacing or augmenting natural skin tissue and to provide support structures or scaffolds for regenerative medicine applications such as implants, drug delivery devices, and tissue engineering scaffolds. Biomaterials must be biocompatible to minimize the risk of adverse effects and immune reactions toward the fabricated scaffolds [6]. They include natural and synthetic polymers such as collagen and silicones, metals and ceramics such as titanium alloys and zirconia, and nanomaterials such as carbon nanotubes.
Non-ecological biomaterials have been replaced by green biomaterials or, in other words, “sustainable biomaterials” that open new opportunities in their therapeutic applications in 3D bioprinting, tissue engineering, drug delivery, and the fabrication of different types of scaffolds. The interaction and coexistence of these natural biomaterials inside human bodies could be safe if they achieved the minimum requirements needed. They must be non-toxic, biodegradable, and biocompatible, especially for these green biomaterials that are used to be a scaffold for cells to grow on it. Many aspects have been used to describe the responsiveness of green biomaterials [7]. Most the sustainable biomaterials are saccharide repeat units in nature [8]. However, some of them are body-like components due to the presence of amino acid repeat units that enhance biodegradability and biocompatibility for biomedical uses [9].
Naturally extracted biomaterials are commonly obtained from algae, plant, and animal sources [10] either by enzymatic processes or the fermentation of microorganisms [11]. Animal waste, mainly produced by the meat, leather, and poultry industries, is abundant and includes non-edible parts such as bones, feathers, tendons, and skins. These wastes contain pathogens and require proper treatment. Common treatments include burning them or composting them with manure, although both methods have drawbacks, including high energy consumption, carbon dioxide emissions, an unpleasant H2S smell during composting, and others. Current research has focused on finding sustainable applications for animal waste, including the extraction of biomaterials (collagen, gelatine, chitosan, and elastin), the generation of biogas, and the production of commercial crops and biodiesel [12]. In addition to animal waste, human skin also contains abundant bio-materials that can be used for sustainable applications such as the extraction of human collagen. For instance, the human skin has a redundant property, which means that it can be removed during surgery or cosmetic procedures and still be functional. This redundant skin can be repurposed as a valuable bioscaffold material for tissue engineering and wound healing applications. Researchers are exploring various methods for treating and processing redundant human skin to create bioscaffolds that mimic the natural extracellular matrix, providing a supportive environment for cell growth and tissue regeneration. This sustainable reuse of human skin can not only reduce waste but also offer an alternative to traditional synthetic materials, ultimately improving patient outcomes.
Sustainable biomaterials are classified chemically into two main groups: polysaccharides in nature such as chitosan, alginate, carrageenan, cellulose, pectin, agarose, and hyaluronic acid [13] and protein such as collagen, gelatin, silk, keratin, and fibrin. Several synthetic biomaterials have also been used in skin burn treatment for several purposes. Researchers are developing synthetic biodegradable polymers that can be used as scaffolds for skin tissue repair. These attempts include using antimicrobial agents, antioxidants, growth factors, cytokines, and other supplements incorporated inside these biomaterials to be fabricated as multifunctional scaffolds to accelerate burn healing by promoting endogenous cell migration and proliferation. It opens a new era for exploiting the treasures of mother nature to adapt them in the innovation of new green biomaterials to be used not only in tissue engineering but also in drug delivery systems, drug targeting approaches, allo- or auto-transplantation, and molecular medicine.
2. Burn Pathophysiology
Burn injury involves both local and systemic responses. Regarding local reaction, a burn can be described by Jackson’s (1953) three concentric zones on the first day of injury: central coagulation, intermediate stasis, and outer hyperthermia zones (Figure 1) [14]. There are three zones of injury in a burn: the central zone of coagulation, the intermediate zone of stasis, and the outer zone. The central zone appears white due to irreversible tissue damage, while the intermediate zone has compromised blood supply and reversible tissue injury with possible petechial hemorrhages. Prompt treatment to increase tissue perfusion is necessary to prevent progression to the central zone [15]. The outer zone sustains the least damage and can heal within a week, but the healing time varies depending on the depth of the wound, the site of burning, and the patient [15].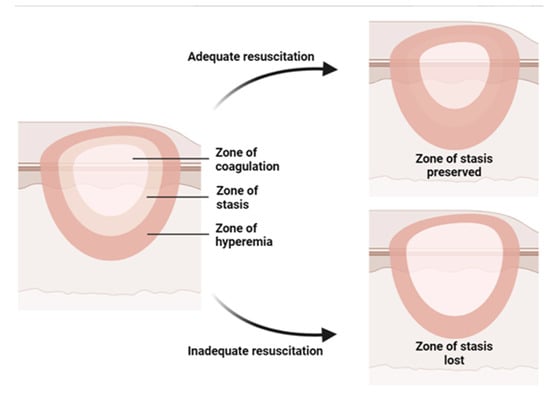
Figure 1. Illustration of the three concentric zones of thermal burn that can be recognized in and around the burned skin: the zone of coagulation is in the center, which is the area closest to the source of the burn and experiences the most intense damage; the zone of stasis, which is the area surrounding the zone of coagulation, where the damage is less severe but still significant; the zone of hyperemia, which is the outermost area surrounding the burn injury, where the tissues are minimally affected.
2.1. Wound Healing Mechanism
Wound healing is a systematic process that involves multiple cell types, the extracellular matrix, and mediators. There are four overlapping and time-dependent phases of natural wound healing: (i) hemostasis; (ii) inflammation; (iii) proliferation; and (iv) remodeling. Due to the specific nature of burns, burn healing differs from natural wound healing. When it comes to thermal burns, the initial inflammatory response may be more pronounced due to the extent of tissue damage and the release of cytokines and other inflammatory mediators. However, the subsequent phases of wound healing, including proliferation and remodeling, may also be impacted by the extent of the injury and other factors such as infection and underlying medical conditions. The burn wound healing depends on the depth and severity of the burns, according to the involvement of the epidermis, dermis, or deeper tissues. The repair process of extensive burn injuries (involving skin and deeper tissues) is more complex and slower, leading to increased scar formation (Figure 2) [27].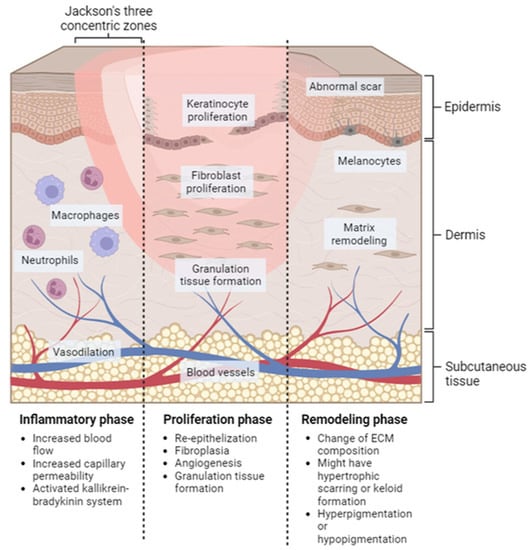
Figure 2. Localized natural phases of the wound healing process for burn injury. Inflammatory phase: this stage starts immediately after the injury occurs and lasts for approximately 3–5 days. Proliferation phase: this stage typically lasts from days 5 to 21 after the injury. Remodeling phase: this can last for several months or even years after the injury.
