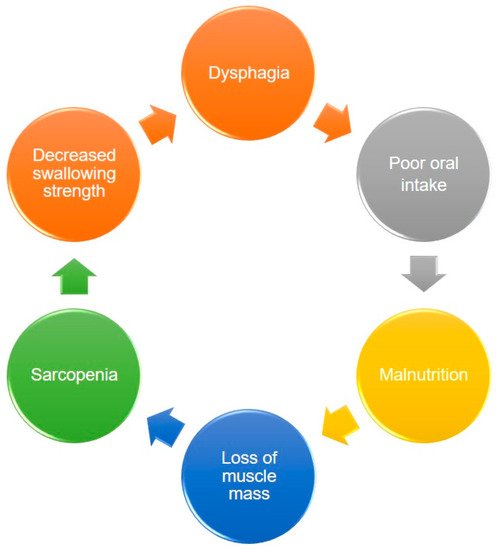
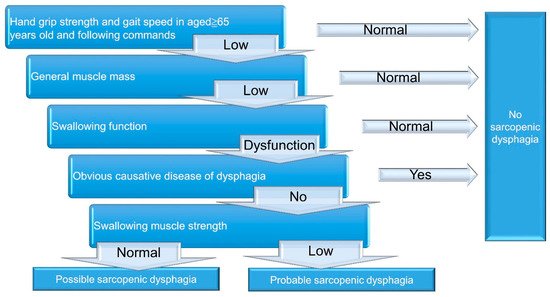
Sarcopenia is a clinical syndrome that refers to a gradual and generalized loss of skeletal muscle mass and strength
[1]. The decline of muscle mass is about 3–8% per decade after the age of 30 years and rises to 15% after 70 years of age
[2][3]. Recently, the concept of the gut-muscle axis has been proposed to play a crucial role in the development of sarcopenia. The gut microbiota has been found to impact muscle volume and performance through mediating inflammatory reactions, immunity, endocrine function, and energy metabolism
[4][5]. According to the European Working Group on Sarcopenia in Older People (EWGSOP)
[6] and Asian Working Group for Sarcopenia (AWGS)
[7] diagnostic criteria, sarcopenia is defined as low muscle mass, strength, and/or physical performance. The cut-point value of sarcopenia revised by the European Working Group on Sarcopenia in Older People (EWGSOP) in 2018 is (1) <7.0 kg/m
2 in men and <5.5 kg/m
2 in women for low muscle quantity; (2) handgrip strength < 27 kg for men and < 16 kg for women for low muscle strength; (3) 6-m walk < 0.8 m/s, Short Physical Performance Battery score ≤ 8, 5-time chair stand test ≥ 15 s, timed up-and-go test ≥ 20 s, or 400-m walk ≥ 6 min for low physical performance
[8]. Moreover, the cut-point value suggested by Asian Working Group for Sarcopenia (AWGS) 2019 consensus is: (1) <7.0 kg/m
2 in men and <5.4 kg/m
2 in women on dual-energy X-ray absorptiometry; and <7.0 kg/m
2 in men and <5.7 kg/m
2 in women on bioimpedance analysis; (2) handgrip strength < 28 kg for men and < 18 kg for women for low muscle strength; (3) 6-m walk < 1.0 m/s, Short Physical Performance Battery score ≤ 9, or 5-time chair stand test ≥ 12 s for low physical performance
[9]. Due to the variations of its diagnostic criteria, the prevalence of sarcopenia ranges between 1% and 29% in the elderly
[10]. Of note, sarcopenia may also reduce the strength of swallowing muscles, leading to dysphagia
[11][12].