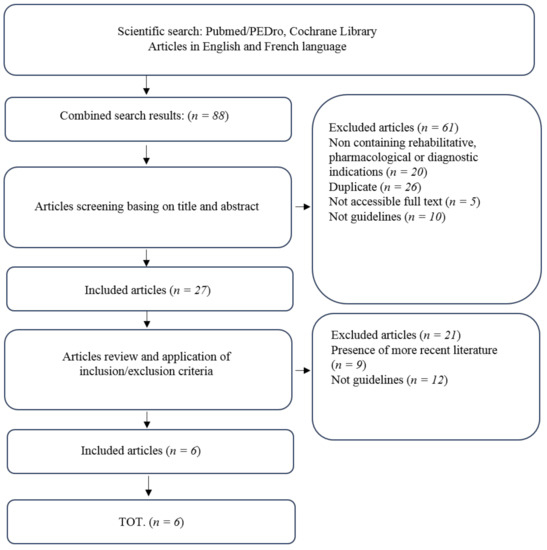
4. Discussion
In this paper, we performed a systematic review of the guidelines published over the last thirteen years regarding rehabilitative interventions in neuropathic pain in order to clarify their role. Although some interventions like TENS therapy, physiotherapy, and psychological interventions were recommended, the key stone of neuropathic pain management lays in the implementation of multidisciplinary complex interventions focusing on all the different aspects affected by this chronic and extremely disabling pathological condition. Moreover, it is important to underline the lack of papers addressing the role of rehabilitation in patients affected by neuropathic pain, focusing on single interventions only aimed at treating neuropathic pain.
Among rehabilitative interventions, physical therapies commonly play a pivotal role in reducing pain. In this systematic review, we evidenced that several studies suggest TENS for neuropathic pain
[7][24][25][26][28]. More in detail, Martinez et al. recommend TENS for localized peripheral neuropathic pain and Demarin et al.
[25] for painful diabetic neuropathy. Cruccu et al.
[24] give a level C recommendation to TENS, which may be better than placebo; they consider its employment as preliminary treatment or additional therapy. Moreover, TENS might exert is action also in association with physiotherapy and psychotherapy for neuropathic pain management
[7].
Several International Guidelines
[12][28] recommend physiotherapy, although not providing clear indications for intervention modalities, for treating neuropathic pain. In this context, Cohen et al.
[28] claim that, among complementary and alternative interventions, the strongest evidence is showed by therapeutic exercise for neck pain management. A recommendation has been detected for percutaneous nerve stimulation in painful diabetic neuropathy by Bril et al.
[27]. Furthermore, spinal cord stimulation has been recommended
[24][26] to treat chronic postoperative lumbar back pain with predominant radiculalgia; it is further suggested by Cruccu et al.
[24] for complex regional pain syndrome. In this regard, Zilliox et al.
[7] suggests spinal cord stimulation for failed back surgery syndrome, complex regional pain syndrome and for diabetic neuropathy. Moreover, it has been suggested
[28] that deep brain stimulation should be reserved for neuropathic pain unable to be treated with pharmacological and companion treatments; in addition, Cruccu et al.
[24] suggest performing this procedure only in experienced centers.
Nevertheless, there is a broad agreement in the scientific literature to give proper attention and not underestimate psychological issues. They are frequently encountered, confirming the repercussion on psychosocial sphere and quality of life by a condition, which is chronic, disabling, and difficult to manage. Several authors
[24][25] recommend psychological intervention in the management of neuropathic pain. Additionally, Acevedo et al.
[12] recommend carrying out a psychosocial assessment at the primary level of care to these patients. Even Martinez et al.
[26] and Chetty et al.
[28] support psychotherapy, suggesting cognitive behavioral therapy.
The greatest consensus is on the recommendation of a multidisciplinary intervention for neuropathic pain, involving pharmacological therapy in association with non-pharmacological one (psychotherapy, physical therapies, and physiotherapy). This is observed on Demarin et al.
[25], Chetty et al.
[28] and Acevedo et al.
[12] studies. In this regard, even recent reviews have been published, whose authors (Binder et al.
[3], Cohen et al.
[29], Deng et al.
[4] and Zilliox et al.
[7]) are strongly in favor of the multidisciplinary approach, a key element essential to target different aspects in neuropathic pain treatment.
Taken together, we showed that TENS is broadly recommended in the management of patients with neuropathic pain, both performed as a preliminary treatment or in association with other interventions, as a component of a multimodal approach. This technique presents some favorable features considering that it is a non-invasive and safe treatment, with relatively few contraindications. TENS is also inexpensive, and this aspect should be taken in consideration since neuropathic pain is a condition that commonly entails a considerable cost for both the healthcare system but especially for the patients. A broad agreement on physiotherapy (alone or as complementary treatment) in the management of neuropathic pain emerges from the recent scientific literature; it might be provided for patients with neuropathic pain. Physiotherapy is necessary to prevent or reverse changes in trophism, disuse atrophy, subsequent contractures, and deformities, preventing ankylosis and deconditioning in general. Psychological assessment, followed by an appropriated psychotherapy is also suggested considering that neuropathic pain frequently results in various psychological sequelae (i.e., anxiety, depression, and sleep disturbances), which further worsen quality of life of the patient.
A combination of an appropriated physiotherapy program alongside psychotherapy, physical therapy, and pharmacological treatment, should be provided for neuropathic pain patients, which include also physical, psychological, and social issues.
Indeed, neuropathic pain presents different severe implications not only related to pain itself, but also to the consequent impairment of function that this entails. Therefore, the intervention of a specialist focused on functional impairment management and recovery is required. This need can be addressed by the Physical Medicine and Rehabilitation specialist, which deals with functional issues responsible for the patient’s disability.
Severe neuropathic pain is difficult to treat effectively, with only a minority of people experiencing a clinically relevant benefit from any single intervention. A multidisciplinary approach is now advocated, combining pharmacological interventions with physical or cognitive interventions (or both). The evidence for interventional management is very weak or non-existent. In those patients with very severe or treatment-refractory pain, surgical options should be considered
[8][29].
Physical Medicine and Rehabilitative specialists should set-up and implement a multi-professional and inter-disciplinary intervention leveraging on a strict collaboration with various healthcare professionals involved in the patient management, in order to ensure the best management of pain. Moreover, it is mandatory to act through an integrated and holistic approach on the various dimensions influenced by neuropathic pain: physical, functional, affective, emotional, social, relational and work-related. A global and customized intervention with necessary active involvement and contribution of the patient in order to maximize the impact on his health-related quality of life
[30][31].
We are aware that this study is not free from limitations: first, the absence of assessment of the quality and reporting of practice guidelines by AGREE-II instrument and review protocol have not been pre-registered; second, the heterogenicity and the complexity of neuropathic pain, in its etiology, signs, and symptoms and thus diagnosis; third, a significant limitation is represented by the low to moderate quality of evidence on neuropathic pain intervention modalities in literature, especially regarding rehabilitative ones.
However, to the best of our knowledge, the main strength of this study is that it addresses neuropathic pain treatment from a rehabilitative point of view for the first time in literature. Although evidence on rehabilitative intervention are not conspicuous, in consequence of the serious limitation of function characterizing the majority of patients with this pathology, the present review was needed to formulate summarized indications of the recommendations included in international guidelines.