Oral candidosis is the most common fungal infection that frequently occurs in patients debilitated by other diseases or conditions. No candidosis happens without a cause; hence oral candidosis has been branded as a disease of the diseased. Prior research has identified oral candidosis as a mark of systemic diseases, such as hematinic deficiency, diabetes mellitus, leukopenia, HIV/AIDS, malignancies, and carbohydrate-rich diet, drugs, or immunosuppressive conditions. An array of interaction between Candida and the host is dynamic and complex. Candida exhibits multifaceted strategies for growth, proliferation, evasion of host defenses, and survival within the host to induce fungal infection.
1. Overview
Oral candidosis is the most common fungal infection that frequently occurs in patients debilitated by other diseases or conditions. No candidosis happens without a cause; hence oral candidosis has been branded as a disease of the diseased. Prior research has identified oral candidosis as a mark of systemic diseases, such as hematinic deficiency, diabetes mellitus, leukopenia, HIV/AIDS, malignancies, and carbohydrate-rich diet, drugs, or immunosuppressive conditions. An array of interaction between Candida and the host is dynamic and complex. Candida exhibits multifaceted strategies for growth, proliferation, evasion of host defenses, and survival within the host to induce fungal infection. Oral candidosis presents a variety of clinical forms, including pseudomembranous candidosis, erythematous candidosis, angular cheilitis, median rhomboid glossitis, cheilocandidosis, juxtavermillion candidosis, mucocutaneous candidosis, hyperplastic candidosis, oropharyngeal candidosis, and rare suppurative candidosis. The prognosis is usually favorable, but treatment failure or recurrence is common due to either incorrect diagnosis, missing other pathology, inability to address underlying risk factors, or inaccurate prescription of antifungal agents. In immunocompromised patients, oropharyngeal candidosis can spread to the bloodstream or upper gastrointestinal tract, leading to potentially lethal systemic candidosis. This review therefore describes oral candidosis with regard to its pathophysiology and best practice for diagnosis, practical classification, and successful management.
2. Candida Species
Candida species can be both commensals and opportunistic pathogens of the oral cavity
[1]. The genus
Candida includes more than 150 species of asporogenous yeast that are widespread in the environment
[2]. Most species cannot live at the temperature of the human body
[2][3], so only a limited number of
Candida species harmlessly live in the healthy mouth, eyes, gastrointestinal tract, vagina, and skin
[2][3][4][5][6][7][8][9]. The prevalence of
Candida albicans (
C. albicans) isolated from the oral cavity are reported to be around 30% to 50% of the healthy general population, 50–65% of people who wear dentures, 65–88% of people who reside in long term care facilities, and 90–95% of individuals with human immunodeficiency virus (HIV) infection and also in patients who receive corticosteroid, chemotherapy, immunosuppressant, or radiation for head and neck cancers
[1][2][4][10][11][12][13]. When an imbalance in the normal oral flora or inadequate immune defense occurs,
Candida can overgrow to induce a fungal infection called oral candidosis or thrush. The terms oral candidosis and candidiasis are synonymous. In this study, the term candidosis is used in preference to candidiasis because the suffix “-osis” is consistent with the ending used for the vast majority of fungal infections, whereas the ending “-iasis” is used for parasitic diseases
[5].
Over 17
Candida species can cause oral mucosa and deep tissue infection. Although
C. albicans remains the most frequent pathogen of candidosis, increased incidence of isolation of non-albicans
Candida (NAC) species from oral lesions and the bloodstream has subsequently developed
[4][5][6][7][14][15][16][17]. The most prominent have been
C. glabrata and
C. parapsilosis, followed by
C. tropicalis and C. Krusei. The four
Candida species plus
C. albicans account for more than 90% of cases of oral or disseminated candidosis and candidemia
[5][6][7][8][9][10]. This shift in species with a higher incidence of candidosis caused by NAC species has emerged as a major bearing on the morbidity and management of patients who are cared for in intensive care units (ICUs) or have important risk factors, such as hematologic malignancies, transplants, major abdominal surgery, and/or prolonged treatment with corticosteroid, as the increasing antifungal resistance along with a wide range of minimum inhibitory concentrations (MICs) to fluconazole between
Candida species exists
[16][17][18][19][20][21]. All
C. krusei are intrinsically fluconazole resistant, and infections caused by this species are strongly associated with prior fluconazole prophylaxis and neutropenia
[15][16][17][18][19][20][21]. An increasing proportion of
C.
glabrata is fluconazole resistant.
C. tropicalis and
C. parapsilosis are generally susceptible to azoles; however,
C. tropicalis is less susceptible to fluconazole than is
C. albicans. In addition, species distribution and echinocandin resistance show considerable differences between medical centers and countries
[16][17][21]. Patient characteristics and prior antifungal therapy also have a considerable influence on the distribution and frequency of
Candida species regardless of geographical area.
Oral candidosis has received considerable attention since the advent of HIV infection and the increasing prevalence of compromised individuals due to modern therapeutic advances. Oral candidosis is actually a mixed
Candida species infection. The three major species of
C. albicans (the commonest; over 50%),
C. tropicalis, and
C. glabrata account for more than 80% of oral candidosis because they can evade antimicrobial activity of lysozyme of saliva and easily adhere to denture acrylic surfaces
[5][6][7][22]. Tobgi and Samaranayake and MacFarlane reported a significant dose-response relationship between lysozyme concentration and fungicidal activity. When different species of
Candida were tested,
C. krusei and
C. parapsilosis were found to be most sensitive to lysozyme compared with
C. albicans and
C. glabrata, which were least sensitive
[22]. The relatively high resistance of
C. albicans and
C. glabrata to lysozyme may partly explain their high oral prevalence both among carriers and in patients with oral candidosis
[22][23][24]. The mixed colonization of
C. albicans and
C. glabrata can enhance fungal invasion and damage of oral epithelial tissues
[25]. Other risk factors are also needed in addition to colonization. In immunocompromised patients, failure to properly treat oral candidosis may lead to chronic persistent infection or invasive candidosis, which may result in necrotizing ulcerative mucositis, suppurative candidosis, inflammatory papillary hyperplasia of hard palate, oropharyngeal and esophageal candidosis, or potentially lethal systemic candidosis, such as
Candida endocarditis
[2][7][26][27]. Patients with candidemia or invasive candidosis may show fever, dysphagia, poor nutrition, slow recovery, or prolonged hospital stay, with a high mortality rate up to 79%
[2][4][17]. Although most patients do not become candidemic, over half of all cases of disseminated candidosis or candidemia are undiagnosed at the time of death
[2][5][7][16][17]. Therefore,
Candida in a blood culture should never be viewed as a contaminant and should always prompt searching for the source of fungemia. The incidence of candidemia clearly exceeds that of invasive aspergillosis and mucormycosis and has become an important nosocomial infection in the hospitals
[15][16][17].
Oral candidosis is usually easy to treat with good prognosis, but the eradication of fungus to achieve a mycological cure is difficult
[2][4][5]. This raises the question whether the recurrence is a second infection or due to persistent
Candida cells. Clinically, unsuccessful management or recurrence of oral candidosis is not uncommon due to either incorrect diagnosis, missing other pathology, failure to correct the underlying predisposing factors, or improper prescription of antifungal agents, such as recurring use of nystatin oral suspension, inadequate treatment duration, and decrease in drug susceptibility or increase of azole-resistant strains with time
[2][7][16][20]. Among these pit falls, the elimination of identifiable predisposing factors is considered the top priority in preventing the recurrence or treatment failure of oral candidosis.
Historically, the aphorism “disease of the diseased” has been given to oral candidosis, and suspicion should therefore be raised when patients have oral candidosis
[1][2][5]. It can be a mirror of underlying systemic disease, such as HIV/AIDS, nutritional deficiency, anemia, diabetes mellitus, Cushing’s syndrome, leukopenia, hypothyroidism, end stage of renal or liver diseases, and hematologic malignancies of leukemia, multiple myeloma, or lymphoma (
Figure 1). Other oral white lesions, including lichen planus, lichenoid reaction, chronic graft-versus-host disease, leukoplakia, and squamous cell carcinoma, may affect the efficiency of the mucosa barrier and then become superinfected with oral candidosis
[4][5][6][7]. These underlying risk factors are usually more important than oral candidosis itself.
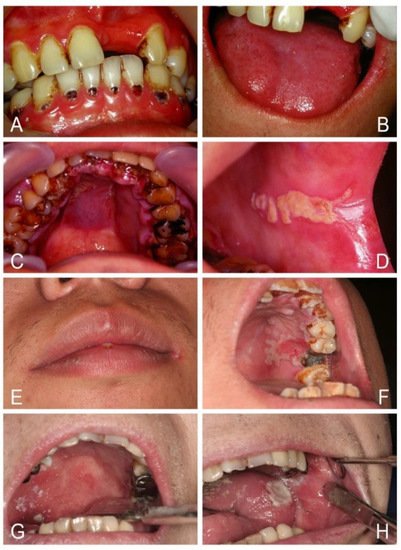
Figure 1. Oral candidosis can be a mark of systemic disease. (A,B) Erythematous candidosis, angular cheilitis, and rampant cervical caries led to the diagnosis of diabetes mellitus and iron deficiency anemia in a 30-year-old male who drank soda daily instead of water. (C,D) Pseudomembranous candidosis and diffuse gum hyperplasia with cyanotic change led to the diagnosis of acute myeloid leukemia in a 32-year-old man. (E,F) Cheilocandidosis and pseudomembranous candidosis around a necrotic ulcer over the palate led to the diagnosis of HIV infection in a 28-year-old man. (G,H) Pseudomembranous and erythematous candidosis with a necrotic tongue ulcer led to the diagnosis of severe leukopenia in a 33-year-old woman.
3. Conclusions
- (1)
-
Maintenance of good oral and denture hygiene is crucial. It is important to remove dentures overnight, use denture cleanser, or make a new denture if an ill-fitting denture with stomatitis exists.
- (2)
-
Rinsing the mouth after use of an inhaled steroid is helpful to prevent oral candidosis.
- (3)
-
Glucose promotes yeast growth, and a high-carbohydrate diet enhances its adherence to oral epithelial cells. Limiting their consumption is helpful in the control of oral Candida colonization and infection.
- (4)
-
Removal of heavy candidal plaques or biofilm from oral lesions by mechanical means can improve antifungal action and speed healing.
- (5)
-
Nystatin tablets are significantly superior to nystatin oral suspension in treating oral candidosis. Swallowing nystatin tablets rather than sucking or dissolving them in the mouth is ineffective to treat oral candidosis.
- (6)
-
The duration of antifungal treatment should be sufficient or prolonged for at least four weeks to achieve a more permanent mycological cure.
- (7)
-
Early fluconazole monotherapy or fluconazole combined with nystatin is helpful to treat oropharyngeal candidosis, suppurative candodosis, or Candida-related chronic oral ulcers.
- (8)
-
Attempts to increase CD4 count in patients with HIV/AIDS or thymoma are helpful to treat oral candidosis. HAART can reduce recurrent oropharyngeal candidosis.
- (9)
-
Underlying predisposing factors should be identified and treated simultaneously as well as monitored regularly.
- (10)
-
The final eradication of oral candidosis is by host defense system.