1000/1000
Hot
Most Recent

Tissue engineering is an emerging field of research that initially aimed to produce 3D tissues to bypass the lack of adequate tissues for the repair or replacement of deficient organs.
| Type of Scaffold | Biomaterials | Ref Example | Advantages | Drawbacks |
|---|---|---|---|---|
| Synthetic | PLCL | [46] | - biocompatible - mechanical properties |
- Degradation products |
| PLCL/Collagen | [47] | - low cost | - Poor differentiation of epithelial cells (except for cellularised collagen matrices; improved by functionalisation) | |
| PLA | [48] | - highly reproducible | -degradation rate (too low or too high) | |
| PU/mesh in PGA | [49] | - quickly available | -mechanical properties during or after degradation | |
| PLGA | [37] | - functionalisation | - poor angiogenesis | |
| PLLA | [50] | |||
| Natural | Cellulose | [51] | ||
| Silk Fibroin | [26][52][53][54] | |||
| Collagen | [18][28][55][56][57][58][59] | |||
| Acellular matrix | SIS | [21][60][61][62][63][64][65] | - Adequate microenvironment for cell proliferation and differentiation | - Immune risk (including DNA, prions) |
| Placental membrane | [66] | - Significant angiogenesis | - Unfavourable clinical experience | |
| BAMG | [67][68][69] | - Quality of the matrix | ||
| Urethra | [70] | |||
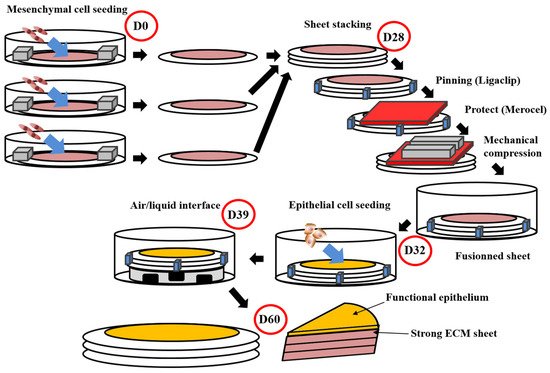
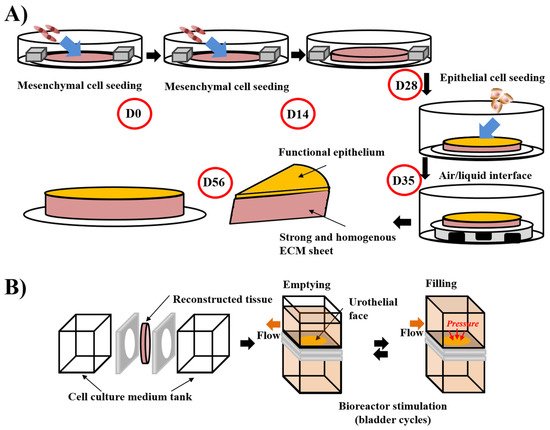
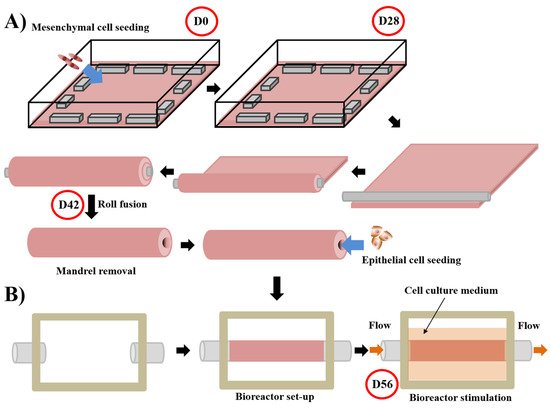
| Self-Assembly | None | [13][71][72] | - Excellent microenvironment with organ-specific cells - Mechanical properties |
- time and cost to produce tissues |
| Type of Scaffolds | Biomaterials | Patients # | References |
|---|---|---|---|
| Synthetic | PGA | 4 | [88] |
| PLA (©PACIENA) | 9 | [89] | |
| 7 | [90] | ||
| Natural | Collagen IV and hyaluronic acid | 1 | [85] |
| 23 | [85] | ||
| Acellular matrix | Amnion | 50 | [91] |
| SIS | 65 (vs Interceed) | [92] | |
| Monkey | [93] | ||
| Acellular vaginal matrix | Rat | [94] | |
| Rat | [87] | ||
| Artificial dermis | 35 | [95] | |
| Self-Assembly | Mouse | [96][97] |