From a population health perspective, during disease outbreaks and pandemics, including the COVID-19 pandemic, along with the general population, it is important for governments to include people with disability in their pandemic planning and response.
1. Introduction
According to the International Classification of Functioning, Disability and Health, disability is defined as an “umbrella term for impairments, activity limitations, and participation restrictions; it denotes the negative aspects of the interaction between an individual (with a health condition) and that individual’s contextual factors (environmental and personal)” [1]. More than a billion people (15% of the world’s population) live with some form of disability worldwide and around 785 million (15.6%) people with disability are 15 years and older [2]. Over 4.4 million (1 in 5) people in Australia live with some form of disability [3]. Furthermore, people with disability experience significant inequalities in health [4].
Epidemics and pandemics pose a serious threat to the health of children and adults with disability, their families, carers and all those that work (both directly and/or indirectly) with people with disability. The recent global pandemic, COVID-19 has shown itself to have profound impacts on all groups of society worldwide, and specifically places people with disability at an increased risk of harm. This is because people with disability are especially vulnerable to the physical, mental and social effects of the pandemic. People with disability are at an increased risk of exposure to SARS-CoV-2 (e.g., through contact with multiple support workers or potentially poor hygiene practices) and many have high risks of complications and death if infected because of underlying health problems [4][5][6].
Evidence from the aftermath of previous emergencies, such as storms and hurricanes, shows that people with disability are often disproportionately harmed, as emergency preparedness plans are often not tailored to their needs [7]. Despite the potential risks to people with disability in pandemics and evidence that they fare poorly in emergencies, people with disability were not prioritised by governments around the world in responding to COVID-19.
The first aimed to collate evidence on the risk of infection for people with disability during infectious disease outbreaks and/or pandemics. This was done to understand previous evidence on the extent to which people with disability were infected, the settings in which the infection was acquired (exposure site, e.g., private home, residential care setting or health facility) and which sub-groups within the population of people with disability were at greater risk of infection and poor health outcomes. The second rapid review aimed to gather government responses to previous infectious disease outbreaks and pandemic plans for people with disability. This will contribute to the pandemic preparedness and public health response aimed at reducing the risks of COVID-19 posed to populations with disability.
2. Aim 1
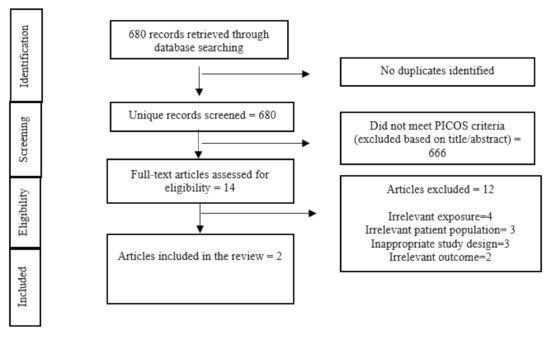
Of the 680 studies identified through our systematic search (Figure 1 Flow diagram of included studies), fourteen studies underwent a full-text screening. Of these, only two studies
[8][9] fulfilled the eligibility criteria and were included in the review. No relevant grey literature met the eligibility criteria for inclusion in this review.
Figure 1. Flow diagram of included studies.
Overview of Included Studies
The two studies included in the review were conducted in France
[8] and Israel
[9]. The study by Chevance et al.
[8] is a literature review that summarises the gaps in the mental healthcare system gathered from experiences of a previous famine in psychiatric hospitals during the Second World War in France. To help the mental healthcare system cope with the current SARS-CoV-2 epidemic in France, the review proposed the need for a reorganisation of the system. The authors’ argued that pre-existing medical comorbidities, cognitive and behavioural disorders, psychosocial vulnerability (including socio-economic living conditions) and older age made people with diagnoses of mental disorders at risk of being infected during a pandemic. Recommendations for a reorganisation of the mental healthcare system in response to the SARS-CoV-2 epidemic included establishing a COVID unit within the psychiatry ward, creation of an integrated COVID and medical/psychiatric system within the medical units, launching a telephone hotline. No information on the review methodology was provided by the authors.
The other study by Ghanaiem et al.
[9], published a decade earlier, was a case study, that described the risk of developing severe and life-threatening respiratory tract infection due to adenovirus type 7 outbreak in a paediatric residential facility. The paediatric residential facility accommodated 62 children with severe physical and/or cognitive disabilities. Eight children (median age of 22.5 months (age range: 9 months to 5 years)), that shared rooms (particularly playroom) at the paediatric residential facility reported respiratory distress with hypoxemia. No children had any prior immunodeficiency or chronic lung disease, and none were ventilator dependent. The spread of infection was through droplets of one of the twelve staff members who were in close contact with the children while showing early symptoms of fever, conjunctivitis and sore throat.
3. Aim 2
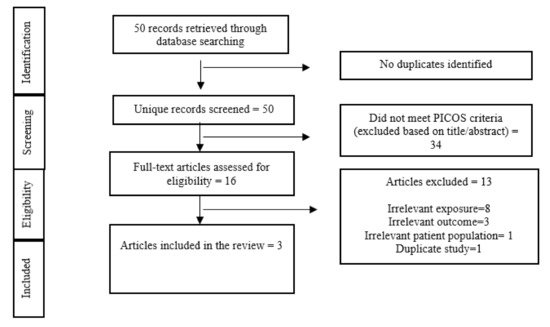
Of the 50 studies identified through our systematic search process (Figure 2 Flow diagram of included studies), 16 studies underwent a full-text screening. Of these only three studies (a commentary
[10], an open letter
[11] and an essay
[12]) met the criteria for inclusion and were included in the review. Furthermore, a grey literature search was conducted that led to the identification of 20 relevant reports. Of these four reports met the eligibility criteria and were included in the review.
Figure 2. Flow diagram of included studies.
Overview of Included Studies
Two
[10][11] (a commentary and an open letter) of the three peer-reviewed articles discussed the need to include people with disability in the government’s public health response to the COVID-19 pandemic. The third peer-reviewed article was an essay
[12] that identified the potential needs of people with disability and discussed strategies to plan a more inclusive response to pandemic influenza. Of the four grey literature documents included in this review, three documents
[13][14][15] discussed the government’s preparedness plans to assist people with disability and one document was a guide
[16] to assist people with disability to manage their own emergency preparedness plan, all for the ongoing COVID-19 pandemic. Two of the four grey literature documents were published in Australia
[13][16] and one each by United Kingdom aid (UKaid)
[14] and the WHO
[15].
These grey literature documents largely illustrated examples of current programs in place to facilitate community preparedness and maximise the prevention of transmission of COVID-19 for the general population, with only a few programs including some information for people with disability. For example, one document mentioned that King’s College London launched a population-wide C-19 COVID Symptom Study app (developed by the health science company ZOE) to identify high-risk areas and population groups that need immediate attention
[17]. This app is used by people living in the United Kingdom (UK) to regularly report on their health, their need for regular help and having a health problem that requires staying at home and regularly using a stick, walking frame or wheelchair to get about. It is endorsed by the Welsh Government, NHS Wales, the Scottish Government and NHS Scotland. The U.K. has also established British Sign Language resources for people with hearing loss or in easy English for those with intellectual disability. These groups may lack necessary public health information about the virus due to public restrictions, such as physical isolation, stay-at-home orders and reduced social contacts. The Alzheimer’s Association, also in U.K., has developed guidance for caregivers of people with dementia to explain hygienic behaviours, such as handwashing, and suggests how to keep the person healthy and safe
[18]. Furthermore, in the U.K., the National Health Services (NHS) has developed guidelines on how to include people with mental health conditions, learning disabilities and autism within the COVID-19 response
[19]. The documents published in Australia stated that the Australian Government is in regular consultation with state and territory governments and health organisations to update their emergency preparedness plans to support the disability community
[20].
4. Conclusions
Overall, due to limited evidence and in light of the limitations of the review, there is an evidence gap regarding whether people with disability are at risk of infection, the extent and the settings in which the infection can be acquired (exposure site), and whether or not there are any sub-groups within the population of people with disability that are at greater risk of infection and poor health outcomes during infectious disease outbreaks and/or pandemics. Further, there is limited consideration of the needs of people with disability in government preparedness and planning for disease outbreaks and/or pandemics. There is a need for better data collection, such that it should include variables relevant for monitoring groups at high risk such as the people with disabilities. This type of inclusive data collection will help with better disaggregation of data on the pandemic situation and the response for these groups. Beyond the threat presented to the general population, it is evident that a pandemic, such as the COVID-19 pandemic, poses a substantial risk to people with disability. It is imperative to have contingency plans for people living in long-term care (including people with disability) and their support staff or carers in the event of a pandemic. Including disability stakeholders (including people with disability) in all stages of planning, implementation and monitoring for managing infectious disease outbreaks and/or pandemics is essential to ensure that policies adequately address the needs of these groups to minimise the risk of harm.