Looking at the published research in ASD, there is plenty of information about neurological
[41], psychiatric
[42] and biological (outside the brain) CMPD of ASD
[3]. These are almost always called comorbidities. However, comorbidities mean that medical conditions present are not related to a main diagnosis, in this case ASD. The design of the research studies in ASD is performed considering OFAT (one factor at a time) instead of the context of multimorbidity. ASD is a model psychiatric disorder following the DSM-5 for the analysis of multimorbidity and personalized medicine.
In this case, multimorbidity is present in the brain (psychiatric and neurological issues) and outside the brain (biological problems in body systems outside the brain) with behavioral, emotional, motor, sensorial and communicational symptoms. The physicians related to these areas are from Psychiatry, Neurology and Pediatrics. The Pediatrician detects ASD and refers to other areas. However, in the Advanced Integrative Model the Pediatrician (or General Practitioner) by training, experience, and competence, is of paramount importance in the Advanced Integrative Approach.
2.1. The Response to Treatment of CMPD in ASD
When a family receives a diagnosis, CMPD are considered comorbid, not related to ASD and of little or no impact on core symptoms or trajectory of ASD. The recommended practice, if it includes exploration of CMPD, is only the limited exploration of gastrointestinal issues, beyond the neurological or psychiatric co-occurring medical problems. In a recent manuscript the recommendations were educational practices, developmental therapies, and behavioral interventions, but CMPD (in particular the out-of-the-brain biological issues) were not properly considered in the state-of-the art knowledge
[43]. It has not been considered, historically, that the results of all the behavioral, relational, developmental or psychoeducative methods to approach ASD are strongly related to the biological status of the person with the ASD diagnosis.
The question is how could the treatment(s) of CMPD affect the ASD symptoms?
There are several possible outcomes to the treatments of CMPD of ASD outside the brain.
There are people diagnosed with ASD (mainly children) whose core ASD symptoms disappear after the adequate treatment of CMPD outside the brain. ASD symptoms seem to be only symptoms of a few CMPD outside the brain with a causal relation
[44].
There are people diagnosed with ASD (all ages) whose core ASD symptoms ameliorate after the adequate treatment of CMPD outside the brain. Many times, several CMPD need to be considered and properly treated to show an impact in the core symptoms. ASD symptoms appear to be related to CMPD in ASD
[45].
There are people diagnosed with ASD (all ages) whose core ASD symptoms do not change after the adequate treatment of CMPD outside the brain, even when several CMPD are considered and properly treated. ASD symptoms are not related to CMPD in ASD. In this case, they could be called “comorbid”.
The individual response to the most rigorous, controlled, and serious allopathic treatments of CMPD in ASD, taking into account multimorbidity and complexity, gives clues to their roles. Therefore, the role of CMPD in ASD would be shown or concluded after and not before the treatment of them.
As Dr. Frye’s group has reported, in ASD many neurological issues have links to biological problems not related to the brain
[46]. Dr. Frye has published several important manuscripts about CMPD in ASD and from the design the work is presented differently than other manuscripts. The titles of these manuscripts generally are “XXX as treatment of YYY in ASD”. This kind of approach to the problem takes into account, since the design, the multiple CMPD in ASD. Historically the presentation of the treatment of CMPD was “XXX as treatment of ASD”. Many recent manuscripts detect, count, and report the so called “comorbidities” instead of considering new models for the role of these CMPD
[4][47][48]. Not all children with gut dysbiosis have ASD, not all children with mitochondrial dysfunction or with some immune deficiency have ASD. There should be another component to take into account and address this complexity and this other component is the brain status in ASD.
2.2. The Controversy about Whether a Static or Dynamic Encephalopathy Contributes to ASD
Encephalopathy is a term used here for a diffuse disorder (or disease) that alters brain function or structure. An encephalopathy is dynamic when it responds to treatments of CMPD outside the brain. An encephalopathy is static when it does not change; it does not respond to treatments of CMPD. A central point is if the encephalopathy in ASD is static or dynamic and how. The dynamic encephalopathy in ASD is considered at first to be chronic and difficult to change, once present. The dynamism of the encephalopathy would also be related to the plastic nature of the brain and the number, combination, and severity of the CMPD. The development of the encephalopathy and the path to chronicity of it is then considered a process, not a genes-mediated fact for all people diagnosed with ASD. This process may begin prenatally (as vulnerability and/or through a genetic mutation/s or polymorphism/s and combinations of them with environmental impact) and/or postnatally. The mechanisms for the encephalopathy to develop involve the genetic susceptibility to CMPD in the brain and outside the brain and the individual response to in-series and in-parallel exposures in the second decade of the XXI century. From processed food to antibiotics, from contaminated water and air to mitochondrial impact, from dysbiosis to whole-body dysfunction and more the many pathways to gut barrier permeability and brain–blood barrier permeability in vulnerable people are explained looking at the model of ASD as symptoms of a dynamic (but chronic) encephalopathy.
Since the presentation of the genetic model (GM) with the manuscript of Folstein and Rutter
[49], 44 years has shown the exploration of the genetic basis of ASD. Meanwhile, the prevalence has grown up to 1 in 54 from the CDC data
[50], that is more related to 1 in 36
[51] and near 1 in 20 males in children up to 17 years or even higher
[52]. The main point of the GM is the consideration of the root of ASD as a static encephalopathy of prenatal origin
[53]. In the neurodiversity model, ASD is a way of being
[54]. These two points of view do not explain many findings, do not give tools or resources to professionals, non-professionals and families to address the individual complex medical, non-medical, and educational needs of many children, teens and adults diagnosed with ASD. There are several recent reports about these unmet needs
[55][56][57].
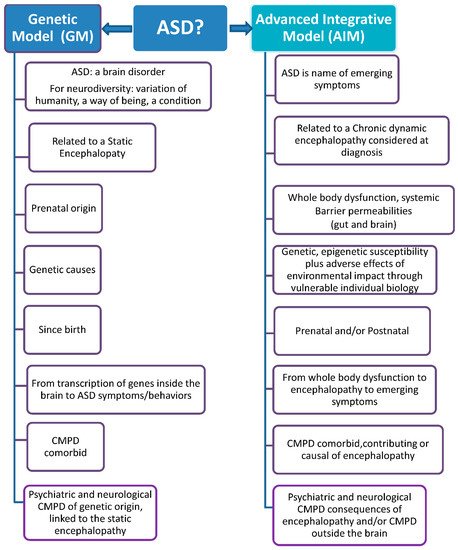
The Advanced Integrative Model (AIM) is a new model of ASD. In this model the CMPD outside the brain should be properly diagnosed and treated. These CMPD may be related to a chronic encephalopathy through the barrier’s permeability. Gut and brain blood barrier permeabilities are important to understand in this proposal. The gut dysbiosis involves pathogenic bacteria, parasites, and fungus that may translocate and/or produce metabolites and correlates with inflammation in the presence of a permeable gut barrier. This abnormal situation produces an immune response. The immune system components and metabolites from gut dysbiosis reach the bloodstream due to the permeable gut barrier and finally the brain due to brain blood barrier permeability
[15]. The idea of a chronic, dynamic encephalopathy as a model of ASD was presented by Dr. Herbert in 2005
[58] but unfortunately was not explored adequately up until the last 10 years and much more in the last 5 years.
In the framework of a model based on the explanation of ASD as a static encephalopathy of prenatal origin, the plausibility of a role of postnatal development disturbance is not taken into account and dismissed. CMPD have been labeled as “comorbid”: medical issues that have no link to ASD. Coincidence or simply better health has been the explanation for the reported improvements after treatments of CMPD, which are sometimes very dramatic. Regression (loss of speech and/or abilities and/or skills) continues to happen today without explanation in these models. No other proposals have been presented, even when no genetic link in brain to regression can be clearly shown in ASD
[59]. Today, regression has been reported to be present in prospective studies in up to 88% of people with ASD
[60], although the consensus in retrospective studies is lower and nearer 30%
[61]. Regression is understood in AIM as the final point of a pre-encephalopathy process. The pathway to chronicity is considered to be an individual process and not a single event
[62] and the final point could be considered to be the regression. The chronic status of the encephalopathy would be related to chronic pathophysiological processes in the brain in ASD (see reference
[51] for further explanation).