Hypothermic Oxygenated Perfusion (HOPE) is a new liver preservation technique used in clinical trials. It may mitigate ischemia/reperfusion injury and improve organ function and patient outcomes.
1. Overview
Although machine perfusion is a hot topic today, we are just at the beginning of understanding the underlying mechanisms of protection. Recently, the first randomized controlled trial reported a significant reduction of ischemic cholangiopathies after transplantation of livers donated after circulatory death, provided the grafts were treated with an endischemic hypothermic oxygenated perfusion (HOPE). This approach has been known for more than fifty years, and was initially mainly used to preserve kidneys before implantation. Today there is an increasing interest in this and other dynamic preservation technologies and various centers have tested different approaches in clinical trials and cohort studies. Based on this, there is a need for uniform perfusion settings (perfusion route and duration), and the development of general guidelines regarding the duration of cold storage in context of the overall donor risk is also required to better compare various trial results. This article will highlight how cold perfusion protects organs mechanistically, and target such technical challenges with the perfusion setting. Finally, the options for viability testing during hypothermic perfusion will be discussed.
2. Background
The field of liver transplantation has recently seen a boost in the development of machine perfusion technology with the first randomized controlled trials published and the availability of several devices on the market. To further drive this technology successfully into routine clinical practice, the community needs to first understand underlying mechanisms of protection by different perfusion approaches. Secondly, transparent reports of study results and the identification of gaps in the literature are needed. With this review article we summarize the clinical studies on hypothermic machine perfusion (HMP) in liver transplantation. Next, the protective mechanism of this cold oxygenation is described. Third, a few methodological differences of HMP performed by different groups are identified and discussed followed by the impact of HMP on organ selection through viability assessment. Finally, this review will project future trials needed to answer the here described ambiguities.
3.What Is the Real HOPE-Effect in Solid Organ Transplantation?
For a prolonged time, the cascade of ischemia-reperfusion-injury (IRI) was supposed to be initiated by the release of reactive oxygen species (ROS) from phagocytes, and here mainly macrophages
[1][2]. Recently, various mechanistic studies point, however, to an overall and ongoing inflammation, which is seen and pronounced by different cell types, resident in the donor liver and introduced with the recipient blood after normothermic reperfusion. The main instigators of IRI were identified with a high number of mitochondria in hepatocytes (>2000)
[3][4]. During warm and cold ischemia, metabolites such as succinate accumulate here. Due to the lack of oxygen, the respiratory chain is unable to maintain the normal electron flow, which leads to a loss of adenosine triphosphate (ATP) and to an accumulation of precursors, including hypoxanthine and xanthine
[5]. Another consequence is the accumulation of oxidized nicotine adenine dinucleotide (NADH) at Complex-I. When mitochondria at this stage undergo rewarming and normothermic reperfusion with oxygen, mitochondria aim for a quick reestablishment of their electron flow, however, with incongruent initial electron transfer speeds of the different complex proteins
[6][7][8][9]. The immediate result is the production and release of reactive oxygen species (ROS) predominantly from Complex-I
[9]. Of note this occurs within the first few seconds of warm reoxygenation in various cell types, not exclusively in macrophages ()
[10][11][12]. The frequently described tissue inflammation, objectified by various molecules, including cytokines, is considered as a downstream injury and depends on the initial organ quality and the previous duration of ischemia
[2][13][14].
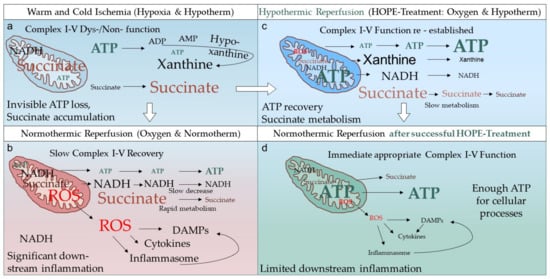
Figure 1. HOPE-Effect on mitochondria. During warm and cold ischemia, the tricarboxylic acid cycle (TCA) and the electron transfer is on hold with a subsequent succinate accumulation. Another direct consequence is the loss of ATP, which is broken down to the precursors, hypoxanthine and xanthine
[5]. The dysfunctional cellular respiration also leads to a high number of NADH molecules, stuck at Complex-1 (
a). When such tissues undergo direct normothermic reoxygenation (reperfusion), mitochondria aim to decrease the high load of succinate with the quick reestablishment of the electron flow. This, however, leads to an immediate release of reactive oxygen species (ROS) mainly from Complex-1. Such ROS molecules leak through the mitochondrial membrane and further damage other cell components, with additional release of danger associated molecular patterns (damps) and cytokines. The result of this IRI cascade is an ubiquitarian inflammation, which depends directly on the initial organ quality. Similarly, the time needed to recover cellular ATP and metabolize succinate and NADH after normothermic reperfusion or transplantation is linked to the number of healthy mitochondria able to quickly recover from the IRI (
b). In contrast, during hypothermic oxygenated perfusion (HOPE, D-HOPE, HMP-O
2) the aerobe respiration is reestablished with a normally directed electron flow, very limited ROS release from Complex-1 and full ATP recovery (
c). Paralleled by a slow succinate and NADH metabolism, such cold pre-treatment of solid organs provides enough cellular energy (ATP) and prevents later ROS release at rewarming and reperfusion under normothermic conditions (
d).
What is the role of machine perfusion in this cascade? Most dynamic perfusion techniques reintroduce oxygen at different temperatures, thereby inducing an aerobe metabolism. However, at normothermic temperatures this process is accompanied with ROS release and downstream inflammation, because the accumulated succinate is still present when the respiratory chain restarts the electron transfer
[5][15][16][17][18]. Therefore, the most protective machine perfusion technique should lead to a slow metabolism of accumulated succinate before rewarming to reprogram the respiratory chain with subsequent ATP-reloading before the cellular energy needs increase to levels required for a normal metabolism at 37 degrees ()
[19]. A similar metabolic situation was also found in mitochondria of the Siberian wood frog, who is naturally protected to live in cold water without oxygen
[20]. Another interesting example occurs with hibernators, who are naturally protected from IRI and the related inflammatory injury at rewarming
[3][20].
Hypothermic oxygenated perfusion (HOPE) has been identified as the best perfusion technique to achieve the above-described mitochondrial protection
[5][18][21]. Reoxygenation in the cold induces a slow succinate metabolism and recovery of Complex-1 to 5 function with efficient ATP recharging. Additionally, a slow metabolism of NADH at Complex-1 has been identified and is used as viability marker for mitochondrial function
[5][22]. When mammalian tissue undergoes rewarming at this “prepared” stage, the normothermic reperfusion appears with significantly less ROS release, better organ function, and reduced downstream inflammation
[18][23]. Of note, this mechanism is the same in all solid organs, including livers, kidney, and hearts
[5][13][24][25].
Another goal of machine perfusion technology is to provide more confidence when accepting an organ through viability assessment. Liver reperfusion at normothermic temperatures is frequently suggested as advantageous for viability testing due to the “near physiologic” behavior during perfusion with a blood-based perfusate at 37°
[26][27][28][29]. Dynamic parameters, including lactate clearance, bile flow, and composition are considered helpful in this context
[29][30][31][32]. However, despite a few case series with normothermic machine perfusion (NMP), none of the markers have been linked to biliary complications and graft survival in a large population yet, and various thresholds for viability parameters exist. One example is perfusate lactate, where four different approaches and cut-offs are found in the literature
[29][31][33], and in a good number of studies the considered viability parameters were not tested in a transplant model, lacking clinical confirmation
[26][29].
Clinically relevant markers to explore liver quality and predict function should ideally be linked to the subcellular structure, which triggers the IRI cascade in mitochondria. Next to the ROS pocket in Complex-1, another molecule, flavin-mononucleotide (FMN), has been identified
[34]. At reaction with oxygen, FMNH
2 is released into perfusate and plasma and has been found to predict liver function and outcomes after transplantation during HOPE treatment of high-risk livers
[5][34][35]. Of particular interest are the autofluorescence characteristics of this FMN molecule, which enable real-time quantification from perfusates through fluorescence spectroscopy during machine perfusion within a few minutes
[5][36].
4. Conclusions
Hypothermic oxygenated liver perfusion was successfully introduced in clinical practice. In addition to the recently published RCT, the results of another five randomized trials are currently awaited. In addition, underlying mechanisms of protection were established through reprogramming of mitochondria during HOPE prior to normothermic reperfusion at transplantation. Despite this success, further questions remain with a few technical differences, where the best possible approach with the easiest and most cost-effective device needs to be determined through further clinical and experimental studies. Here the main questions include, first, the duration of cold storage before or after a minimum of two hours of HMP. Next, the best possible perfusion route could for example be clarified with a comparative randomized controlled trial in high-risk DCD livers, where the HOPE treatment is performed with or without perfusion through the hepatic artery (HOPE vs. dual-HOPE). In addition to the two ongoing comparative RCTs between HOPE and NMP, the cold technique should also be compared to NRP in the donor. Although most warm perfusion techniques are frequently discussed as beneficial to administering genes or stem cells, there is also experimental evidence of gene therapy during HMP. This approach should also be explored further to understand potential treatment options to improve mitochondrial function in livers with an FMN release that is currently too high
[37].